UNITED STATES
SECURITIES AND EXCHANGE COMMISSION
Washington, D.C. 20549
FORM
(Mark One)
Annual report pursuant to Section 13 or 15(d) of the Securities Exchange Act of 1934
for the fiscal year ended
or
Transition report pursuant to Section 13 or 15(d) of the Securities Exchange Act of 1934.
for the transition period from to .
Commission File Number
(Exact name of registrant as specified in its charter)
(State or other jurisdiction of incorporation or organization)
(IRS Employer Identification No.)
.,
,
(Address of principal executive offices, including zip code)
Registrant’s telephone number, including area code:
(
)
Securities registered pursuant to Section 12(b) of the Act:
Title of each class
Trading Symbol
Name of exchange on which registered
The
Nasdaq
Securities registered pursuant to Section 12(g) of the Act: None
Indicate by check mark if the registrant is a well-known seasoned issuer, as defined in Rule 405 of the Securities Act. Yes
☐
☒
Indicate by check mark if the registrant is not required to file reports pursuant to Section 13 or Section 15(d) of the Act. Yes
☐
☒
Indicate by check mark whether the registrant (1) has filed all reports required to be filed by Section 13 or 15(d) of the Securities Exchange Act of
1934 during the preceding 12 months (or for such shorter period that the registrant was required to file such reports), and (2) has been subject to such
filing requirements for the past 90 days.
☒
☐
Indicate by check mark whether the registrant has submitted electronically every Interactive Data File required to be submitted pursuant to Rule 405
of Regulation S-T (§ 232.405 of this chapter) during the preceding 12 months (or for such shorter period that the registrant was required to submit such
files).
☒
☐
Indicate by check mark whether the registrant is a large accelerated filer, an accelerated filer, a non-accelerated filer, a smaller reporting company or
an emerging growth company. See the definitions of “large accelerated filer,” “accelerated filer,” “smaller reporting company” and "emerging growth
company" in Rule 12b-2 of the Exchange Act.
Large Accelerated Filer
☐
Accelerated Filer
☐
☒
Smaller Reporting Company
Emerging Growth Company
If an emerging growth company, indicate by check mark if the registrant has elected not to use the extended transition period for complying with any
new or revised financial accounting standards provided pursuant to Section 13(a) of the Exchange Act.
Indicate by check mark whether the registrant has filed a report on and attestation to its management’s assessment of the effectiveness of its internal
control over financial reporting under Section 404(b) of the Sarbanes-Oxley Act (15 U.S.C. 7262(b)) by the registered public accounting firm that
prepared or issued its audit report.
Indicate by check mark whether the registrant is a shell company (as defined in Rule 12b-2 of the Exchange Act). Yes
☐
No
☒
The registrant was not a public company as of June 30, 2021, the last business day of its most recently completed second fiscal quarter, and therefore,
cannot calculate the aggregate market value of its voting and non-voting common equity held by non-affiliates as of such date. The registrant’s Class
A common stock began trading on the Nasdaq Global Market on November 11, 2021. As of March 24, 2022, the registrant had
$0.0001 par value Class A common stock outstanding and
DOCUMENTS INCORPORATED BY REFERENCE
Portions of the following document are incorporated by reference in Part III of this Report: the registrant’s definitive proxy statement relating to its
2022 Annual Meeting of Shareholders. We currently anticipate that our definitive proxy statement will be filed with the SEC not later than 120 days
after December 31, 2021, pursuant to Regulation 14A of the Securities Exchange Act of 1934, as amended.
1
TABLE OF CONTENTS
3
46
91
91
91
91
92
92
92
104
105
138
138
139
139
PART III
139
139
139
139
139
Item 15.
139
141
142
2
PART I
Unless otherwise indicated in this report, “Vaxxinity ,” “we,” “us,” “our,” and similar terms refer to Vaxxinity, Inc. and our consolidated
subsidiaries.
SPECIAL NOTE REGARDING FORWARD -LOOKING STATEMENTS
This Annual Report on Form 10-K for the year ended December 31, 2021 (“Report”) contains forward-looking statements. Forward-
looking statements are neither historical facts nor assurances of future performance. Instead, they are based on our current beliefs,
expectations and assumptions regarding the future of our business, future plans and strategies and other future conditions. In some cases,
you can identify forward-looking statements because they contain words such as “anticipate,” “believe,” “estimate,” “expect,” “intend,”
“may,” “predict,” “project,” “target,” “potential,” “seek,” “will,” “would,” “could,” “should,” “continue,” “contemplate,” “plan,” other
words and terms of similar meaning and the negative of these words or similar terms.
Forward-looking statements are subject to known and unknown risks and uncertainties, many of which may be beyond our control. We
caution you that forward-looking statements are not guarantees of future performance or outcomes and that actual performance and
outcomes may differ materially from those made in or suggested by the forward-looking statements contained in this Report. In addition,
even if our results of operations, financial condition and cash flows, and the development of the markets in which we operate, are
consistent with the forward-looking statements contained in this Report, those results or developments may not be indicative of results
or developments in subsequent periods. New factors emerge from time to time that may cause our business not to develop as we expect,
and it is not possible for us to predict all of them. Factors that could cause actual results and outcomes to differ from those reflected in
forward-looking statements include, among others, the following:
• the prospects of UB-612 and other product candidates, including the timing of data from our clinical trials for UB-612
and other product candidates and our ability to obtain and maintain regulatory approval for our product candidates;
• our ability to develop and commercialize new products and product candidates;
• our ability to leverage our Vaxxine Platform;
• the rate and degree of market acceptance of our products and product candidates;
• our status as a clinical-stage company and estimates of our addressable market, market growth, future revenue,
expenses, capital requirements and our needs for additional financing;
• our ability to comply with multiple legal and regulatory systems relating to privacy, tax, anti-corruption and other
applicable laws;
• our ability to hire and retain key personnel and to manage our future growth effectively;
• competitive companies and technologies and our industry and our ability to compete;
• our and our collaborators’, including United Biomedical’s (“UBI”), ability and willingness to obtain, maintain, defend
and enforce our intellectual property protection for our proprietary and collaborative product candidates, and the scope
of such protection;
• the performance of third party suppliers and manufacturers and our ability to find additional suppliers and
manufacturers;
• our ability and the potential to successfully manufacture our product candidates for pre-clinical use, for clinical trials
and on a larger scale for commercial use, if approved;
• the ability and willingness of our third-party collaborators, including UBI, to continue research and development
activities relating to our product candidates;
• general economic, political, demographic and business conditions in the United States, Taiwan and other jurisdictions;
• the potential effects of government regulation, including regulatory developments in the United States and other
jurisdictions;
• ability to obtain additional financing in future offerings;
3
• expectations about market trends; and
• the effects of the Russia-Ukraine conflict and the COVID-19 pandemic on business operations, the initiation,
development and operation of our clinical trials and patient enrollment of our clinical trials.
We discuss many of these factors in greater detail under Item 1A. “Risk Factors.” These risk factors are not exhaustive and other sections
of this report may include additional factors which could adversely impact our business and financial performance. Given these
uncertainties, you should not place undue reliance on these forward-looking statements.
You should read this Report and the documents that we reference in this Report and have filed as exhibits completely and with the
understanding that our actual future results may be materially different from what we expect. We qualify all of the forward- looking
statements in this Report by these cautionary statements. Except as required by law, we undertake no obligation to publicly update any
forward-looking statements, whether as a result of new information, future events or otherwise.
Item 1. Business.
Overview
We are a purpose-driven biotechnology company committed to democratizing healthcare across the globe. Our vision is to disrupt the
existing treatment paradigm for chronic diseases, increasingly dominated by drugs, particularly monoclonal antibodies (“mAbs”), which
suffer from prohibitive costs and cumbersome administration. We believe our synthetic peptide vaccine platform (“Vaxxine
Platform”) has the potential to enable a new class of therapeutics that will improve the quality and convenience of care, reduce costs
and increase access to treatments for a wide range of indications. Our Vaxxine Platform is designed to harness the immune system to
convert the body into its own “drug factory,” stimulating the production of antibodies with a therapeutic or protective effect. While
traditional vaccines have been able to leverage this approach against infectious diseases, they have historically been unable to resolve
key challenges in the fight against chronic diseases. We believe our Vaxxine Platform has the potential to overcome these challenges,
and has the potential to bring the efficiency of vaccines to a whole new class of medical conditions. Specifically, our technology uses
synthetic peptides to mimic and optimally combine biological epitopes in order to selectively activate the immune system, producing
antibodies against only the desired targets, including self- antigens, making possible the safe and effective treatment of chronic diseases
by vaccines. The modular and synthetic nature of our Vaxxine Platform generally provides significant speed and efficiency in candidate
development and has generated multiple product candidates that we are designing to have safety and efficacy equal to or greater than
the standard-of-care treatments for many chronic diseases, with more convenient administration and meaningfully lower costs. Our
current pipeline consists of five chronic disease product candidates from early to late-stage development across multiple therapeutic
areas, including Alzheimer’s Disease (“AD”), Parkinson’s Disease (“PD”), migraine and hypercholesterolemia. Additionally, we believe
our Vaxxine Platform may be used to disrupt the treatment paradigm for a wide range of other chronic diseases, including any that are
or could potentially be successfully treated by mAbs. We also will opportunistically pursue infectious disease treatments. When the
COVID-19 pandemic struck the world in March 2020, we quickly reallocated our resources to develop vaccine candidates for the
condition. We have assembled an industry-leading team with extensive experience developing and commercializing successful drugs
that is committed to realizing our mission of democratizing healthcare. Our website address is www.vaxxinity.com. The information
contained on, or that can be accessed through, our website is not part of, and is not incorporated into, this Report.
Limitations of the Current Healthcare Paradigm
The current healthcare paradigm favors the development of drugs that are primarily intended for the U.S. market, for niche indications
and for treatment of disease rather than prevention. Furthermore, these drugs are expected to be sold at price points that are only
accessible to healthcare systems in developed countries. One class of drugs in particular exemplifies the current environment: biologics,
particularly mAbs. In 2019, biologics represented eight of the ten top selling drugs in the United States, of which seven were mAbs. The
global market for mAbs totaled approximately $163 billion in 2019, representing approximately 70% of the total sales for all
biopharmaceutical products.
While mAbs can provide life-altering care with generally favorable safety characteristics and significant health benefits for the patients
who receive them, regular in-office transfusions and annual treatment costs, which can exceed hundreds of thousands of dollars, present
challenges to both patients and payors. These price and administration hurdles cause mAb treatments to be available to only a fraction
of the population who could benefit from them. Furthermore, mAbs are often restricted to moderate to severe disease and to later lines
of treatment due to their high cost. Based on internal estimates, less than 1% of the worldwide population is on mAbs. Meanwhile, the
alternative to mAbs treatments tends to be small molecules, which are accessible to most patients, but are often comparatively less
effective with more significant side effects. Collectively, this perpetuates a profound inequity in healthcare access, domestically but
even more so globally, that we believe represents a tremendous social and market opportunity.
4
Our Solution
Monoclonal antibodies are developed, produced and purified outside the body and then transfused into the patient on a regular basis, as
frequently as bi-weekly. Therefore, mAbs are inherently less efficient than vaccines, which instead stimulate antibody production within
the patient’s immune system, requiring both less active material and less frequent treatments. However, while traditional vaccines have
historically been successful addressing infectious diseases, previous attempts to utilize vaccines to address chronic disease have not
achieved both acceptable safety and efficacy. This limitation is driven by a traditional vaccine’s inability to either stimulate the requisite
antibody response against harmful self-antigens, that is, break immune tolerance, or produce acceptable levels of reactogenicity, the
physical manifestation of the immune response to vaccination. Our Vaxxin e Platform technology contains modular components custom-
designed to mimic select biology and activate the immune system, enabling our product candidates to break immune tolerance when
targeting self- antigens, a property observed across multiple clinical and pre-clinical studies. Our Vaxxine Platform depends heavily on
intellectual property licensed from UBI and its affiliates, a related party and a commercial partner for us, who first developed the peptide
vaccine technology utilized by our Vaxxine Platform. The formulation of peptide-based medicines is also complex, requiring significant
expertise from UBI, its affiliates and our other contract manufacturers to produce our product candidates.
We believe our Vaxxine Platform has the potential to generate product candidates with attributes that collectively offer significant
advantages over both mAbs and small molecule therapeutics:
•
Cost
: Monoclonal antibodies require costly and complex biological manufacturing processes. Our
manufacturing process is chemically based and highly scalable and requires lower capital expenditures. In addition, we designed our
product candidates to generate antibody production in the body, thus requiring meaningfully less drug substance relative to mAbs,
leading to commensurately lower costs.
•
Administration
: Our product candidates are designed to be injected in quarterly or longer intervals via
intramuscular injection similar to a flu shot. We believe this offers considerable convenience compared to mAbs, which can require up
to bi-weekly dosing via intravenous infusion or subcutaneous injections, and small molecules, which often require daily dosing.
•
Efficacy
: In our clinical trials conducted to date, our product candidates have yielded high response rates
(95% or above at target dose levels) for UB-311, UB-312 and UB-612, high target-specific antibodies against self-antigens (as seen in
UB-311 and UB-312 clinical trials) and long durations of action for UB-311 (based on titer levels remaining elevated between doses)
and UB-612 (based on half-life). See our descriptions of these clinical trials under “—Our Product Candidates.” We also believe that
the improved convenience of our product candidates as compared to mAbs has the potential to lead to increased adherence by patients.
Furthermore, our Vaxxine Platform enables the combining of target antigens into a single formulation. For indications that could be
treated more effectively with a multivalent approach, we believe our Vaxxine Platform would have an advantage over other modalities.
Finally, because our Vaxxine Platform is designed to elicit endogenous antibodies, we believe our product candidates may lessen or
avoid altogether the phenomenon of anti-drug antibodies which has limited the efficacy of certain mAbs over time.
•
Safety
: Based on our clinical trials to date, our product candidates have been well tolerated, with safety
profiles comparable to placebo. We aim to offer product candidates with safety profiles at least comparable to the competing mAb or
small molecule alternative for the relevant disease.
5
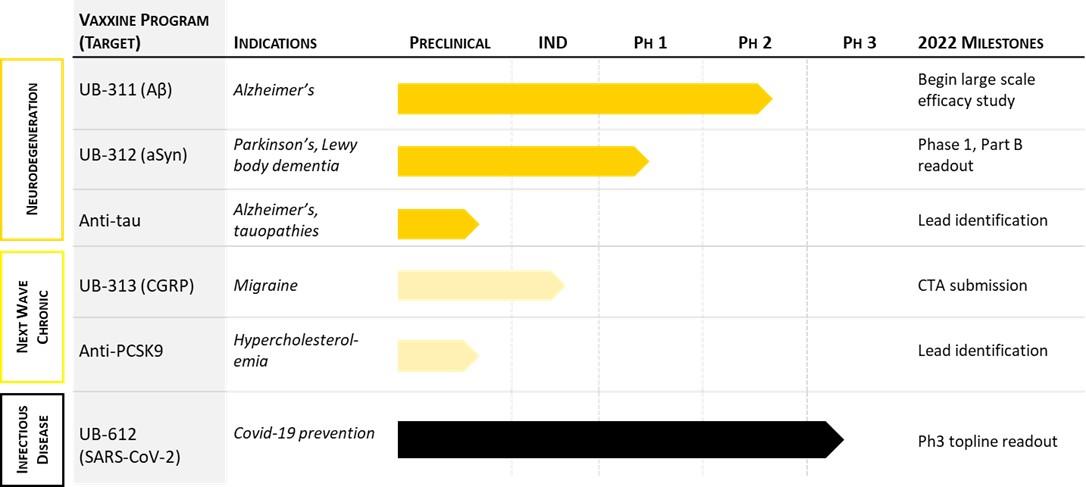
Our Pipeline
The following chart reflects our current product candidate pipeline:
As used in the chart above, “IND” signifies a program has begun investigational new drug (“IND”)-enabling studies.
Our pipeline consists of five lead programs focused on chronic disease, particularly neurodegenerative disorders, in addition to other
neurology and cardiovascular indications.
Neurodegenerative Disease Programs:
•
UB-311
: Targets toxic forms of aggregated amyloid-b (“Ab”) in the brain to fight AD. Phase 1, Phase 2a and
Phase 2a Long Term Extension (“LTE”) trials have shown UB-311 to be well tolerated in mild-to-moderate AD subjects over three
years of repeat dosing, with a safety profile comparable to placebo, with no cases of amyloid- related imaging abnormalities-edema
(“ARIA-E”) observed in the Phase 2a trial, and immunogenic, with a high responder rate and antibodies that bind to the desired target.
We expect to initiate a Phase 2b early AD efficacy trial in the second half of 2022.
•
UB-312
: Targets toxic forms of aggregated α-synuclein in the brain to fight PD and other synucleinopathies,
such as Lewy body dementia (“LBD”) and multiple system atrophy (“MSA”). The first part of a Phase 1 trial in healthy volunteers has
shown UB-312 to be well tolerated, with no significant safety findings, and immunogenic, with a high responder rate and antibodies
that cross the blood-brain barrier (“BBB”). No serious adverse events were observed in Part A of the Phase 1 trial. We have initiated
the second part of this Phase 1 trial in PD subjects, and anticipate the completion of an end-of-treatment analysis in the second half of
2022.
•
Anti-tau
: We are developing an anti-tau product candidate that has the potential to address multiple
neurodegenerative conditions, including AD, by targeting abnormal tau proteins alone and in potential combination with other
pathological proteins such as Aβ to combat multiple pathological processes at once. We expect to identify a lead product candidate in
the next two years.
Next Wave Chronic Disease Programs:
•
UB-313
: Targets Calcitonin Gene-Related Peptide (“CGRP”) to fight migraines. We have initiated IND-
enabling studies and expect to begin a first-in-human Phase 1 clinical trial in 2022.
•
Anti-PCSK9
: Targets proprotein convertase subtilisin/kexin type 9 serine protease (“PCSK9”) to lower low-
density lipoprotein (“LDL”) cholesterol and reduce the risk of cardiac events. We expect to initiate IND-enabling studies for this
program in 2022.
Given the global COVID-19 pandemic and our Vaxxine Platform’s applicability to infectious disease, we also have advanced product
candidates that address SARS-CoV-2.
6
COVID-19
•
UB-612
: Employs a “multitope” approach to neutralizing the SARS-CoV-2 virus, meaning the product
candidate is designed to activate both antibody and cellular immunity against multiple viral epitopes. Phase 1 and Phase 2 trials of UB-
612 have shown UB-612 to be well tolerated, with no significant safety findings to date (over 7,500 doses have been administered to
over 3,750 subjects). No serious adverse events were observed in the Phase 1 trial. In the Phase 2 trial, twenty serious adverse events
were observed through interim analysis. Only one led to discontinuation of the study, and none were considered UB-612-related. In
these trials we observed that UB-612 generated antibodies that can bind to the S1-RBD protein and neutralize SARS-CoV-2, in addition
to driving T-lymphocytes (“T-cell”) response. An emergency use authorization (“EUA”) application for UB-612 was denied by the
Taiwan Food and Drug Administration (“TFDA”) in August 2021, but, in collaboration with our partner United Biomedical, Inc., Asia
(“UBIA”), we are appealing that decision. At the same time, we are still pursuing approval of UB-612 elsewhere, including as a
heterologous boost (boosting the immunity of a subject who has already received a different vaccine). In collaboration with University
College London and VisMederi , we analyzed sera from subjects immunized with a booster dose of UB-612. Data demonstrated that
UB-612 elicited a broad IgG antibody response against multiple SARS-CoV-2 variants of concern, including Alpha, Beta, Delta,
Gamma, and Omicron, and higher levels of neutralizing antibodies against Omicron than reported with three doses of an approved
mRNA vaccine.
We believe our Vaxxine Platform has application across a multitude of chronic and infectious disease indications beyond our existing
pipeline. We also are developing additional product candidates that we believe may address significant unmet needs both within and
beyond our current pipeline’s therapeutic areas.
Our Team
We have assembled an experienced group of executives with deep scientific, business and leadership expertise in pharmaceutical and
vaccine discovery and development, manufacturing, regulatory and commercialization. Mei Mei Hu, our co-founder and Chief
Executive Officer, has been a member of the executive committee of UBI since 2010. Our board of directors is chaired by our co-founder
Louis Reese, who has been a member of the executive committee of UBI since 2014. Our research efforts are guided by highly
experienced scientists and physicians on our leadership team including Dr. Ulo Palm, our Chief Medical Officer, and Dr. Farshad
Guirakhoo, our Chief Scientific Officer. Our leadership team contributes a diverse range of experiences from leading companies
including Acambis, Allergan, Amgen, Dendreon, Eli Lilly, Merck, Novavax, Novartis, Sanofi, and Schering-Plough, and were
executives in multiple successful mAb and vaccine launches, including Dupixent, Kevzara, Provenge, PreveNile, Ervebo, Imojev and
Dengvaxia. As of December 31, 2021, we have assembled an exceptional team of approximately 86 employees, the majority of whom
hold Ph.D., M.D., J.D. or Master’s degrees, and we are regularly hiring additional personnel. We also have a highly experienced
scientific advisory board consisting of 13 doctors and scientists.
Our Strategy
Our mission is to develop product candidates that improve the quality of care for chronic diseases and are accessible to all patients across
the globe. In order to achieve this mission, we seek to:
•
Advance our chronic disease pipeline through clinical stage development
: We plan to advance UB-311 and
UB-312 through clinical stage development for the treatment of neurodegenerative disorders. In addition, we are conducting IND-
enabling studies on multiple pre-clinical product candidates that are focused on the treatment of chronic migraines, hypercholesterolemia
and additional neurodegenerative disorders. We believe that our differentiated Vaxxine Platform will enable our product candidates, if
successful, to potentially disrupt the treatment paradigm for their respective indications. However, there can be no guarantee that we
will achieve commercialization of any such product candidates.
•
Expand our pipeline of product candidates
: Chronic diseases are prevalent globally and expected to worsen
over the next several decades. In furtherance of our mission, we plan to expand our pipeline by developing new product candidates that
address additional indications. In expanding our pipeline, we rely on our proprietary filtering methodology, which evaluates potential
product candidates across five principal criteria – (i) probability of technical and regulatory success, (ii) addressable market, (iii)
development cost, (iv) competitive dynamics and (v) disruptive potential.
•
Opportunistically develop treatments for infectious diseases
: While our core mission focuses on the treatment
of chronic diseases, we are committed to bringing accessible medicines to people around the world and will address infectious diseases
opportunistically. For example, when the COVID-19 pandemic struck the world, we rapidly deployed resources in pursuit of a product
candidate currently embodied in UB-612.
•
Expand and scale our existing capabilities
: We are investing in our operational processes, facilities and
human capital to accelerate the speed with which we can bring product candidates through the development pipeline, and to expand the
capacity for developing more product candidates simultaneously.
7
•
Continue to improve our Vaxxine Platform
: In addition to, and in conjunction with, our product candidate
development efforts, we are continuously working to improve and enhance the richness, breadth and effectiveness of our Vaxxine
Platform. As our Vaxxine Platform further develops, we believe that we can both increase the number of product candidates in concurrent
development and accelerate the process of advancing product candidates through pre-clinical and clinical development.
•
Maximize the value of our product candidates through potential partnerships
: We currently retain worldwide
rights for the majority of our product candidates and will consider entering into development and commercialization partnerships with
third parties that align with our mission on an opportunistic basis.
Background and Limitations of Traditional Vaccines and Monoclonal Antibodies
The immune system, the body’s mechanism for fighting off potential threats, is comprised of cells that form the innate and adaptive
immune responses. The main purpose of the innate immune system is to immediately prevent the spread and movement of foreign
pathogens throughout the body. The adaptive immune response is specific to the pathogen presented to T-cells and B lymphocytes (“B-
cells”) and leads to an enhanced response upon future encounters with those antigens. Antibodies represent an important tool within the
adaptive immune system’s arsenal. Upon detection of a potential threat, B-cells produce antibodies that recognize, bind to and eliminate
the threatening pathogen. Over time, the immune system develops the ability to produce countless types of antibodies, each finely tuned
against a specific threat.
Generally, the immune system is able to function effectively by neutralizing viruses, bacteria and even self-generated cells and proteins
from within our own bodies that could cause harm if unchecked. However, as powerful as the immune system is, there are threats that
it cannot overcome on its own, generating the need for medicine. Conventional forms of medicine include small molecules (e.g.,
antibiotics), which can inhibit or promote action within the body by, for instance, binding to a receptor on the surface of a cell, or directly
inducing toxic effects upon bacteria. These medicines do not necessarily modulate the immune system directly in order to work. Instead,
they work alongside it. While small molecules have provided substantial benefits to human health, they are not designed to interact with
the immune system. They may also have limited efficacy in cases where an immune response to a target can be used against a chronic
condition.
Vaccines
In the first part of the twentieth century, vaccines revolutionized healthcare by directly interacting with, and modulating, the immune
system — training it to recognize a dangerous pathogen by introducing the immune system to a relatively harmless form of the pathogen,
its toxins or one of its surface proteins, thereby promoting the body’s own production of binding antibodies. Once immunized to a
specific pathogen, the immune system can recognize it and generate the antibodies to fight it more quickly and robustly.
Traditional vaccine technologies have generally focused on the prevention of bacterial and viral infections and not on chronic disease.
In chronic disease settings, the disease-causing agents frequently come from within the body. These self-antigens are proteins that
become too abundant, misfolded or aggregated such that they can no longer perform their healthy function and even may induce toxic
effects. The body can sometimes produce antibodies against such proteins, but this often falls short of providing the right types of
antibodies in the right concentrations to ward off disease. Historically, vaccine technologies developed to target these proteins have been
unable to break immune tolerance — that is, the immune system’s general avoidance of reactivity towards self-antigens — with an
acceptable level of reactogenicity. The challenges faced by prior efforts to advance vaccine technologies for chronic diseases included
low response rates, low titer levels, off- target responses and other safety concerns such as T-cell mediated inflammation.
Monoclonal Antibodies
The first mAbs were developed in the later part of the twentieth century. In contrast to vaccines, which prompt the body to produce
antibodies, mAbs are antibodies manufactured outside of the patient’s body and then injected or infused into the body to recognize and
eliminate harmful targets. Monoclonal antibodies have revolutionized the standard-of-care treatment for many chronic diseases.
However, manufacturing mAbs is often an expensive and complex process and administering mAbs is cumbersome, sometimes requiring
infusions as frequently as bi-weekly. These factors have generally limited mAbs’ availability to moderate-to-severe disease, to later
lines of therapy and to wealthier geographies, thus denying access to a substantial portion of the patients who could benefit from them.
Finally, patients on mAbs often experience a loss of effectiveness over time due to a phenomenon known as anti-drug antibodies,
whereby the immune system begins to recognize therapeutic mAbs as foreign, and mounts a response against them, eventually mitigating
their efficacy.
Our Vaxxine Platform
Our Vaxxine Platform is designed to stimulate the patient’s own immune system to generate antibodies and overcome the limitation of
traditional vaccines to effectively and safely target self-antigens in chronic diseases. Our product candidates have broken immune
tolerance against self-antigens consistently. As described in the section titled “Our Product Candidates” below, across six clinical trials,
we have consistently observed that our product candidates have stimulated the development of antibodies against the desired target at

8
relevant doses in clinical trial subjects, including the elderly. We have observed favorable tolerability and reactogenicity of our product
candidates across studies of UB-311, UB-312 and UB-612, with no significant safety findings to date. We aim to develop product
candidates that possess clinical advantages against, and safety profiles at least comparable to, relevant mAbs and small molecule
treatments. We believe our product candidates have the potential to eventually capture meaningful market share from mAbs and small
molecules, and to provide therapeutic benefit to large patient populations who currently receive neither form of treatment. This would
represent an unprecedented shift in the treatment paradigm, potentially providing better global access to treatments that have been
previously limited to the wealthiest nations. In particular, we believe our treatments for chronic disease could reflect the following
benefits as compared with the relevant mAbs and small molecule alternatives:
Characteristics of our Product Candidates versus Monoclonal Antibodies and Small Molecules
History and Design
Our Vaxxine Platform utilizes a peptide vaccine technology first developed by UBI and subsequently refined over the last two decades,
with more than three billion doses of animal vaccines sold to date. UBI initiated the development of this technology for human use; the
business focused on human use was then separated from UBI through two separate transactions: a spin-out from UBI in 2014 of
operations focused on developing chronic disease product candidates that resulted in United Neuroscience, a Cayman Islands exempted
company (“UNS”), and a second spin-out from UBI in 2020 of operations focused on the development of a COVID-19 vaccine that
resulted in C19 Corp., a Delaware corporation (“COVAXX”) . Our current company, Vaxxinity, Inc., was incorporated under the laws
of the State of Delaware on February 2, 2021 for the purpose of acquiring UNS and COVAXX in March of 2021.
On March 2, 2021, in accordance with a contribution and exchange agreement among Vaxxinity, UNS, COVAXX and the UNS and
COVAXX stockholders party thereto (the “Contribution and Exchange Agreement”), the existing equity holders of UNS and COVAXX
contributed their equity interests in each of UNS and COVAXX in exchange for equity interests in Vaxxinity (the “Reorganization”).
In connection with the Reorganization, (i) all outstanding shares of UNS and COVAXX preferred stock and common stock were
contributed to Vaxxinity and exchanged for like shares of stock in Vaxxinity, (ii) the outstanding options to purchase shares of UNS
and COVAXX common stock were terminated and substituted with options to purchase shares of Class A common stock in Vaxxinity,
(iii) the outstanding warrant to purchase shares of COVAXX common stock was cancelled and exchanged for a warrant to acquire
Class A common stock in Vaxxinity, and (iv) the outstanding convertible notes and a related party not payable were contributed to
Vaxxinity and the former holders of such notes received Series A preferred stock in Vaxxinity.
UBI has used its capabilities in peptide technology for innovations across an array of business endeavors: antibody testing for human
diagnostics, animal health vaccines and the manufacture of medical products. Its innovative products include one of the first approved
peptide-based blood antibody tests in the world (for HIV), one of the first approved peptide vaccines against an infectious disease in the
world in animal health (for a food-and-mouth disease virus) and one of the first approved peptide vaccines against a self-antigen in the
world in animal health (an anti-luteinizing hormone-releasing hormone (“LHRH”) vaccine used for the immunocastration of swine).
Grant funding from the National Institutes of Health supported some of UBI’s work in the fields of vaccines and antibody testing. To
commercialize its animal health vaccine business, UBI and its affiliates scaled up GMP vaccine manufacturing to over 500 million doses
per year and partnered with a top-ten animal health company for commercialization of its anti-LHRH vaccine; all together, UBI’s
technology platform is utilized for the vaccination of approximately 25% of the global swine population annually.
We are advancing our peptide-based Vaxxine Platform to develop product candidates that target chronic diseases and COVID-19. Our
Vaxxine Platform comprises a custom, rationally designed antigen capable of evoking an immune response (an “immunogen”)
formulated with a proprietary CpG oligonucleotide. The immunogen contains several advanced synthetic peptides, including B-cell
epitopes, T-helper (“Th”) antigen carrier constructs and epitope linker configurations. This composition enables us to achieve a highly
9
specific immune response to the target antigen, with limited inflammation and off-target effects that could cause reactogenicity. This
design process has evolved into a repeatable series of well-defined steps, which has enabled the development of our current pipeline of
product candidates.
Key Elements of our Vaxxine Platform Constructs and Formulations
When developing a product candidate, we use publicly available information and sophisticated bioinformatics tools to investigate the
entire protein structure of a target in a comprehensive manner to identify functional B-cell epitopes that may provide optimal antigens.
We then synthesize custom peptides that mimic these identified antigens to elicit highly specific antibodies against these B-cell epitopes.
To yield favorable tolerability profiles, we design our product candidates such that they lack T-cell epitopes and screen them for lack of
T-cell mediated inflammation and toxicity, as well as reactogenicity. Such screening tests include the measuring of immunogenicity of
each B-cell antigen with and without conjugation to a Th carrier peptide (a response only when conjugated to a Th carrier peptide is
desired), epitope mapping assays and in vivo and ex vivo tests of lymphocyte proliferation, pro-inflammatory cytokine release and T-
cell infiltration. To enhance effectiveness, we seek to optimize the size and sequence of our custom peptides to elicit a robust, specific
antibody response when linked to a carrier molecule.
We then attach a proprietary carrier molecule, an artificial Th carrier peptide that delivers the synthetic peptide into cells. Carrier
molecules used in traditional vaccines often elicit a strong T-cell mediated immune response, resulting in significant off-target activity.
In our pre-clinical trials and clinical trials to date, our product candidates have displayed specific immunogenicity, or the ability to
stimulate an immune response, thereby greatly reducing potential off-target effects and increasing the potential for our product
candidates to be well tolerated and efficacious. We have observed that our carrier molecules have produced consistent results across
multiple species and against multiple targets in our six human clinical trials to date. Traditional vaccines have faced challenges in
achieving specific responses because they rely on conjugating the antigen to a large toxoid molecule carrier protein, to which most of
the antibody response is directed, causing off-target effects such as inflammation.

10
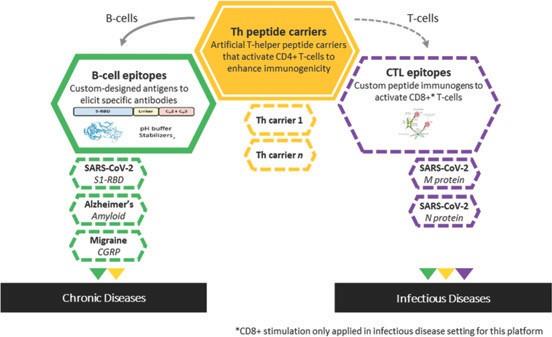
Our Product Candidate Does not Induce an Antibody Response against its Carrier Molecule
The graph above illustrates that our peptide carriers induce a strong immune response against the target antigen, and a minimal immune
response against themselves, as compared to traditional vaccines formulated with other types of carrier molecules.
Our peptide carriers have short sequence lengths, which contribute to their immunosilence and ability to avoid a direct response by
cytotoxic T-cells. However, the carriers’ sequences mirror those found in naturally ubiquitous pathogens, so they are easily recognized
by T-helper cells. This encourages robust T-helper cell exposure to the carrier peptide and promotes activation of other immune cells.
In turn, B-cells are exposed to the B-cell antigen and begin antibody production against the antigen, while avoiding exposure to the
carrier peptide, which avoids antibody response to the carrier. We believe that B-cell exposure to the carrier peptide is avoided because
of its relatively small size and its high affinity to T-helper cells, such that T-helper cells are exposed to the carrier peptide rapidly and
robustly, more so than other cell types. UBI first developed a library of such peptide carriers, which contain various Th cell epitopes
and are of critical importance to our vaccine configuration. Our library of peptide carriers enables the use of different carrier molecules
or different combinations of carrier molecules, which allows us to potentially regulate the speed of immune response onset as well as
the magnitude and duration of that response. For example, a longer duration of response would allow for less frequent dosing. Other
variables that can be adjusted to modulate the immune response include dosing and formulation optimization. In the case of vaccines
targeting infectious diseases, T-cell mediated activity is desirable, while in the case of chronic diseases, it is not. Our Vaxxine Platform
affords the flexibility to design immunogen constructs that specifically promote cytotoxic T-cell activity when warranted (e.g., for
infectious diseases).
We utilize our linker construct to attach our peptide carriers with our custom antigens. In addition to their binding function, these linkers
also enhance the immune system response further by enabling conformational changes to optimize presentation of the B-cell epitope to
antigen-presenting cells (“APCs”), such as B-cells and dendritic cells (“DC”).
Our Vaxxine Platform also enables the construction of multitope configurations, whereby we can attach multiple immunogens targeting
multiple B-cell epitopes simultaneously, each with different targets, within a single product candidate. Combinations of therapies
targeting different molecular mechanisms are common in treating neurologic, cardiovascular, psychiatric, metabolic, respiratory,
infectious and oncologic disease. Our Vaxxine Platform’s favorable cost of goods and efficient manufacturing process could allow for
viable combinations of targeted therapies in a single formulation. This concept could be applied in an array of potential therapeutic
areas. Our current pipeline has candidates against amyloid-β, α-synuclein and tau; combinations of two or more of these might prove
more effective than any single therapy in some patients. Pre-clinical data to date suggests that we can elicit antibody titers against all
three targets in a single formulation. For mAb-based treatments, such combinations might require the individual dosing of multiple
separate mAb therapies, thereby compounding cost and administration burdens.
11
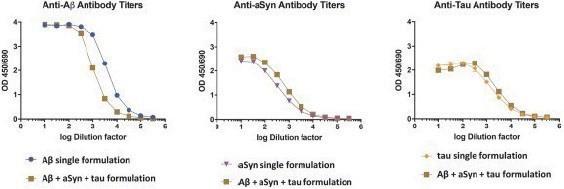
Immunogenicity of Single- Versus Combination-Target Formulations in Guinea Pigs
Guinea pigs (three per dose) were tested with either single-target or combination-target formulations, then serum was drawn and
antibody titers compared via enzyme immunoassays (“EIA”). Combination-target formulations elicited similar titer levels against each
target as corresponding single-target formulations. This suggests we can create product candidates with multiple neurodegenerative
targets in a single formulation and achieve sustainable titer levels.
Product Candidate Formulations
In addition to our immunogen construct, each product candidate formulation includes custom CpG oligonucleotides and adjuvant
selection. CpG oligonucleotides are negatively charged, and we utilize proprietary CpG configurations to stabilize the positively charged
peptides. This stabilization acts to optimize display of the B-cell epitope to APCs. In this way, the primary function of CpG
oligonucleotides in our formulations is that of an excipient, even though it has the secondary function of an adjuvant.
A potential secondary function of CpG is that of an adjuvant. Certain CpG configurations are known to act as immunostimulants and
promote direct cytotoxic T-cell activity, while others do not. Accordingly, our selection of the specific CpG modality is highly dependent
on the target indication. For infectious disease indications, the T-cell response generated by the CpG configuration is independent and
in addition to that of the T-cell response generated by the peptide carrier.
The final formulation includes the addition of an adjuvant, such as a well-recognized, alum-derived Adju-Phos or Alhydrogel to further
enhance the immunogenicity of our product candidate. Alum-derived adjuvants are commonly used in vaccines to enhance the
stimulation of an immune response. This is not the same adjuvant used in other companies’ failed neurodegenerative vaccine candidates.
How our Product Candidates Function
Our immunogens stimulate the body’s adaptive immune system to produce antibodies against a variety of antigen targets, including
secreted peptides or proteins, degenerative or dysfunctional proteins and membrane proteins, as well as infectious pathogens. The
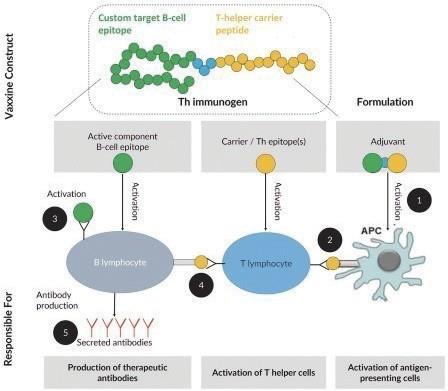
mechanism of action involves the following sequence of steps:
1. The immunogen is taken up by an APC, such as a DC. Antigen uptake leads to DC maturation and migration
to the draining lymph nodes where the DCs interact with CD4+ T-helper cells.
2. DCs engulf and process the antigen internally and present the T-helper epitope on major histocompatibility
complex (“MHC”) Class II molecules. The presentation activates immunogen-specific CD4+ T-helper cells causing them to mature,
proliferate and promote B-cell stimulatory activity.
3. B-cells with receptors that recognize the target B-cell epitope bind, internalize and process the immunogen.
The binding of the B-cell receptor to the immunogen provides the first activation signal to the B-cells.
4. When B-cells function as APCs and present the T-helper epitope on MHC Class II molecules, interaction
with immunogen-specific CD4+ T-helper cells provides a second activation signal to B-cells, which causes them to differentiate into
plasma cells.
5. B-cell epitope-specific plasma cells produce high affinity antibodies against the target B-cell epitope. Of
particular importance for neurodegeneration targets, these antibodies are produced in sufficient concentrations to cross the BBB.
12
Overview of How our Product Candidates Function
Importantly, from both clinical trials and pre-clinical studies, we have observed the rapid expansion of antibodies upon administration
of a booster of our product candidates. Based on the available data to date, we can infer that while antibody titers decline with time after
administration, a small number of memory B-cells and antibody secreting cells are maintained in the lymphoid organs, spleen or bone
marrow. We believe this is important because if a patient misses a dose of our product candidate, they may be able to recall the antibody
response, and therefore the therapeutic effect of the antibodies, with a single booster, even after a long period of time has passed.
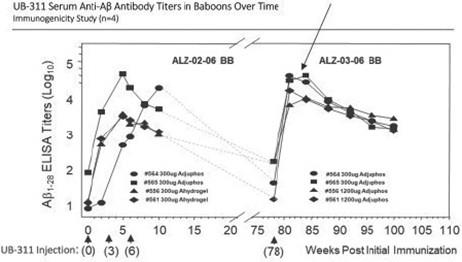
Vaxxine Platform Immunogenicity upon Re-dosing
As shown in the above graph, a repeatable immune response elicited from our product candidates has been observed with a booster
dose over one year after the priming regimen.
Furthermore, the antibodies elicited by our product candidates have different properties than those of mAbs targeting similar pathology.
In general, we aim to achieve binding affinity, specificity and functionality similar or improved compared to mAbs targeting similar
pathology. We use Bio-Layer Interferometry (ForteBio®) to compare kon, koff and kD values of antibodies elicited by our product
candidates versus mAbs. We also use Western blot or slot blot to evaluate the binding specificity of antibodies elicited by our product
13
candidates against the toxic, misfolded or aggregated forms of the target protein, and avoidance of monomers or healthy forms. We use
immunohistochemical analyses to observe the binding of antibodies to pathological inclusions on brain sections of patients. Moreover,
we use cell-based models and animal models to measure the induced antibodies’ functionality. Additionally, a major challenge in mAb
drug discovery is that mAbs are prone to induce an immune response against themselves, resulting in a potential
inactivation/neutralization of the mAb by the host (i.e., the patient). This is not a concern with our vaccine approach as each patient will
produce its own antibodies against the target. Finally, mAbs have a potential for off-target binding, which could result in non- specific
safety and toxicity issues. We believe that this is unlikely to happen using our vaccine approach since antibodies elicited by our product
candidates come from the body’s own B-cells and are therefore unlikely to induce antibodies against other self-proteins as a foreign
antibody may.
Product Candidate Selection Process
Because our Vaxxine Platform may have applicability across a range of chronic diseases, we employ a proprietary filtering methodology
to best identify new product candidates for development. We evaluate potential product candidates across five principal criteria:
•
Probability of technical and regulatory success
: We examine the probability of success for a product
candidate based on stage of development and therapeutic area, and then make target- specific adjustments for design difficulty, industry
knowledge and clarity of biological mechanism, general safety risk and estimated titer level required for therapeutic effect. This criterion
accounts for the known validity of a given target in the relevant disease context.
•
Market opportunity
: We account for the prevalence, unmet need and drug market size for each likely
indication associated with a given target, as well as the number of potential indications.
•
Development cost
: We estimate the cost of development through BLA submission, the time to submission
and the number of patient-years to proof-of-concept.
•
Competitive advantages
: We evaluate the extent to which the advantages of our Vaxxine Platform compare
to the current and potential future standard of care, including convenience, dosing, safety, efficacy and cost.
•
Disruptive opportunities
: We evaluate the extent to which the potential disruptive properties of our Vaxxine
Platform may play a role in treatment paradigms, including the ability to “leap-frog” mAbs and treat patients in earlier lines of treatment,
to be used as a prophylactic, to combine multiple targets into a single formulation and to be used as an adjuvant therapy.
After assigning values to each criterion for a given product candidate, we weight each criterion according to a confidential algorithm,
and thereby prioritize product candidates for development. We update these values on a regular basis based on new scientific literature,
trial results and our Vaxxine Platform advancements.
As an example, in light of these criteria, AD and other neurodegenerative diseases that involve misfolded proteins are an attractive area
for development. First, as the field has gained knowledge and clinical experience around the biology of targeting aberrant proteins with
antibodies, the relative technical, safety and regulatory risk has decreased. AD and PD have high prevalence worldwide, and large unmet
need with no disease-modifying products readily available to patients. Moreover, the underlying pathologies often begin years or decades
before symptoms may appear and as a result, early intervention in the disease state, as well as prevention or delay of onset strategies,
may be optimal and more practically achievable with a vaccine approach. While mAbs can target the pathology, they face the limitations
of high cost, cumbersome and inefficient administration and limited access, and are not suited for early treatment or prevention, which
we believe provides a disruptive opportunity for our Vaxxine Platform.
We do not currently evaluate oncology and infectious diseases through the above framework. We generally do not pursue oncology
targets given the hyper-segmentation of subjects common in clinical development efforts in oncology that leads to relatively narrow
labels, and due to the strengths of other new modalities such as cell-based therapy in this area. We only consider infectious disease
opportunistically. However, our approach with respect to oncology and infection diseases could change in the future.
We believe that our Vaxxine Platform, and our strategy more generally, will create a significant opportunity for drug development well
beyond our current pipeline of clinical and pre-clinical indications, in therapeutic areas including allergy (e.g., chronic rhinosinusitis,
atopic dermatitis, food allergy), autoimmune disease (e.g., psoriasis, psoriatic arthritis, Crohn’s disease), pain (e.g., peripheral
neuropathy, diabetic neuropathy) and bone and muscle atrophy (e.g., sarcopenia of aging, osteopenia).
Underlying Drivers of Our Platform Advantages
Our Vaxxine Platform’s properties drive the unique combination of attributes that we believe will be reflected in our product candidates:
14
•
Cost
: Our reliance on chemically linked, custom peptide sequences fuels cost efficiencies that we expect to
enable broad accessibility to our product candidates. Foremost among these relates to dosing. Monoclonal antibodies require more
physical material for annual dosing because the patient needs to be delivered the externally manufactured therapeutic antibodies, which
have high molecular weight. In contrast, our product candidates are designed to stimulate the body’s immune system to produce its own
antibodies and have relatively low molecular weight. While an annual supply of mAbs doses may include grams or tens of grams of
drug substance, our current product candidates only require 1 to 2 milligrams each, or even less, leading to a relatively low annual cost
of goods. In our development programs to date, we have achieved a cost of goods amounting to a small fraction of the typical cost of
mAbs (as low as <1%).
•
Administration
: Administration of our product candidates generally requires three priming doses, each in the
range of several hundred micrograms, followed by booster doses of a similar magnitude 2 to 4 times per year. As described in the section
titled “Our Product Candidates” below, in clinical trials we have observed that our product candidates elicited a sustained antibody
response, with elevated antibody levels lasting six months or longer. We believe this presents a meaningful advantage over many mAbs,
which commonly require either bi-weekly or monthly injections, or monthly or quarterly infusions, and many small molecules, which
commonly require a daily pill.
•
Safety
: The antibodies generated by our product candidates are designed to be highly specific to the target
antigen and to avoid an off-target immune response to the peptide carrier, thereby limiting inflammation and other off-target activity.
We believe these characteristics have yielded the high tolerability observed in the clinical studies of our product candidates to date.
Furthermore, the titer response to our product candidates is naturally titrated, which may reduce the likelihood of an antibody Cmax
safety side effect, and is naturally reversible, thus avoiding an uncontrolled or permanent immune response.
•
Efficacy
: In our clinical trials conducted to date, our product candidates have yielded comparatively high
response rates (95% or above at target dose levels) for UB-311, UB-312 and UB-612, high target- specific antibodies against self-
antigens (as seen in UB-311 and UB-312 clinical trials) and long durations of action for UB-311 (based on titer levels remaining elevated
between doses) and UB-612 (based on half-life). Furthermore, our Vaxxine Platform enables the combining of target antigens into a
single formulation. For indications that could be treated more effectively with a multivalent approach, we believe our Vaxxine Platform
would have an advantage over other modalities. Finally, because our Vaxxine Platform is designed to elicit endogenous antibodies, we
believe our product candidates may lessen or avoid altogether the phenomenon of anti-drug antibodies which has limited the efficacy of
certain mAbs over time.
Additionally, our Vaxxine Platform possesses important benefits reflected at the platform level, as opposed to the product candidate
level:
•
Product Candidate Discovery
: Our Vaxxine Platform enables the efficient iteration of product candidates in
the discovery phase through rapid, rational design and formulation. We are able to screen in high throughput rapidly and at low cost.
Upon nominating a target for drug discovery, we can formulate several dozen product candidate compounds for preliminary in vivo
immunogenicity and cross-reactivity screening within 2 to 3 months. This process allows nonviable product candidates to “fail fast” and
allows us to carry top product candidates forward through subsequent pre-clinical development to lead identification. In contrast,
biologics require the maintenance and adjustment of living cultures to design, formulate and iterate, and therefore discovery and early
development is inherently less efficient.
•
Process Development
: Scaling the formulation of a drug product from research grade to clinical grade, then
to commercial grade, typically consumes a great deal of resources. This, together with the development of assays for quality control and
quality assurance, comprise process development. Through our manufacturing partnership with UBI and certain of its affiliates, we
leverage their experience scaling the manufacture of both clinical and commercial compounds that use our Vaxxine Platform technology.
Unlike process development for mAbs, which has inherent challenges such as risk of contamination in cell culture or bioreactors and
time-consuming adjustments to cell lines for any formulation adjustment, our peptide platform relies on chemical synthesis which is
more reproducible and scalable, and relatively quick to manipulate for any modifications.
Our Product Candidates
Neurodegenerative Disease Programs
Neurodegenerative diseases are a collection of conditions defined by progressive nervous system dysfunction, degeneration or death of
neurons, which can cause cognitive decline, functional impairment and eventually death. Neurodegeneration represents one of the most
significant unmet medical needs of our time due to an aging population and lack of effective therapeutic options.
Two of the most common neurodegenerative diseases are AD and PD. In the United States, currently more than six million people suffer
from AD, and approximately one million people suffer from PD according to estimates from the Alzheimer’s Association and the
Parkinson’s Disease Foundation, respectively. As a result, AD and PD bring a heavy burden on our society’s cost of care. The direct
costs of caring for individuals with AD and other dementias in the United States were estimated at $305 billion in 2020 according to a
15
study published by the American Journal of Managed Care, and are projected to increase to $1.1 trillion by 2050 according to the
Alzheimer’s Association. The financial burden of PD exceeded $50 billion in the United States in 2019. Many more people around the
world suffer from these two diseases and their related social and economic implications.
UB-311
An Overview of Alzheimer’s Disease
Alzheimer’s disease is a progressive neurodegenerative disorder that slowly destroys memory and cognitive skills and eventually the
ability to carry out simple tasks. Its symptoms include cognitive dysfunction, memory abnormalities, progressive impairment in activities
of daily living and a host of other behavioral and neuropsychiatric symptoms. The exact cause of AD is unknown, but genetic and
environmental factors are established contributors. AD affects more than six million people in the United States and 44 million
worldwide. The economic burden of AD is expected to surpass $2.8 trillion by 2030.
Many molecular and cellular changes take place in the brain of a person with AD. Aβ plaques and neurofibrillary tangles of tau protein
in the brain are the pathological hallmarks of the disease. These abnormal depositions lead to loss of neurons and neuronal connectivity
and the signs and symptoms of AD.
The Aβ protein involved in AD comes in several different molecular forms that accumulate between neurons. One form, Aβ 42, is
thought to be especially toxic. In the brains of patients with AD, abnormal levels of this naturally occurring protein clump together to
form plaques that collect between neurons and disrupt cell function. Research is ongoing to better understand how, and at what stage of
the disease, the various forms of Aβ influence AD.
Neurofibrillary tangles are abnormal accumulations of a protein called tau that collect inside neurons. Healthy neurons are supported
internally, in part, by structures called microtubules, which help to guide nutrients and molecules from the cell body to the axon and
dendrites. In healthy neurons, tau normally binds to and stabilizes microtubules. In AD, abnormal chemical changes cause tau to detach
from microtubules and to stick to other tau molecules, forming threads that eventually join to form tangles inside neurons. These tangles
block the neuron’s transport system, which harms the synaptic communication between neurons.
Converging lines of evidence suggest that AD-related brain changes may result from a complex interplay among abnormal tau, Aβ
proteins and several other factors. It appears that abnormal tau accumulates in specific brain regions involved in memory. Concurrently,
Aβ clumps into plaques between neurons. As the level of Aβ reaches a tipping point, tau rapidly spreads throughout the brain. In addition
to the spread of Aβ and tau, chronic inflammation and its effect on the cellular functions of microglia and astrocytes, as well as changes
to the vasculature, are thought to be involved in AD’s pathology and progression.
Limitations of Current Therapies
Two classes of small molecules approved for the treatment of AD’s symptoms are acetylcholinesterase inhibitors (“AChEIs”) and
glutamatergic modulators. AChEIs are designed to slow the degradation of the neurotransmitter acetylcholine, helping to preserve
neuronal communication and function temporarily. Glutamatergic modulators are designed to block sustained, low-level activation of
the N-methyl-D-aspartate (“NMDA”) receptor, without inhibiting the normal function of the receptor in memory and cognition.
However, these therapeutic products only address the symptoms of AD and do not modify or alter the progression of the underlying
disease.
Aducanumab, marketed under the trade name Aduhelm, is a mAb developed by Biogen, Inc. (“Biogen”) that targets aggregated forms
of Aß. The FDA approved aducanumab in June 2021, making it the first approved immunotherapy for AD, the first new FDA-approved
treatment since 2003 and, importantly, the first to receive accelerated approval based on a biomarker. By approving aducanumab on the
basis of biomarker evidence, we believe the FDA set a precedent for developers of anti-Aβ immunotherapies. Soon after the FDA’s
decision, Eli Lilly and Company (“Lilly”) announced that it would file for approval of its anti-Aβ mAb, donanemab, in 2022 on the
basis of Phase 2 data. Despite the milestone in the treatment of AD that aducanumab’s approval represents, the drug has several
limitations. Approximately one-third of patients experience ARIA-E related adverse events, which can manifest as symptoms ranging
from headaches to confusion to coma. In addition, the drug must be administered monthly via intravenous infusion in locations with
healthcare professionals trained to administer infusion therapies in facilities specifically configured to support an hours-long infusion
process, creating a burden for patients and additional costs resulting from the complex administration process. Because of the risk of
developing ARIA-E, physicians who prescribe aducanumab must titrate dosing and carefully monitor each patient using magnetic
resonance imaging (“MRI”). This process is costly and burdensome, and thus expected to limit the prescribing of and regular access to
aducanumab. In addition, aducanumab launched at a price of $56,000 annually for the drug product only, not including administration
and ongoing monitoring costs such as positron emission topography (“PET”) and MRI scans. Since that time, Biogen has reduced the
price of Aduhelm. The combination of price, side effects, extra costs and extra administration burden highlight the challenges of, and
have limited access to, this mAb.
16
Our Product Candidate: UB-311
We are developing a novel product candidate, UB-311, as a potential disease-modifying therapy for the treatment of AD. We completed
a Phase 1 open label trial (V118-AD) and a Phase 2a randomized, double-blinded, placebo-controlled trial (the “Phase 2a Main Trial”)
in 2021 and believe that UB-311 may offer several differentiators versus aducanumab, including the preferential targeting of aggregated
Aβ oligomers over monomers with modest clearance of Aβ plaques, and a tolerability profile comparable to placebo. No signs of ARIA-
E related adverse events were reported in the Phase 2a Main Trial despite more than two-thirds of the study participants being APOE4
carriers.
Post hoc
cognitive decline in some subjects by up to 50% when compared to placebo, as measured by Clinical Dementia Rating Sum of Boxes
(“CDR-SB”), Alzheimer’s Disease Assessment Scale – Cognitive Subscale (“ADAS-Cog”), Alzheimer’s Disease Cooperative Study –
Activities of Daily Living (“ADCS-ADL”) and Mini-Mental State Examination (“MMSE”) scores, all clinically validated measures of
cognition or function in AD. In this small Phase 2a study, these were secondary measures, as the study was not designed to assess
cognitive decline. Although our Phase 2a trial was a proof-of-concept study, not powered to demonstrate significant changes in any
endpoint, we believe the data are suggestive of potential therapeutic efficacy and may lead to clinical benefit.
UB-311 is formulated for intramuscular administration on a dosing schedule of every three or six months. In addition, lower
manufacturing costs may support meaningfully lower pricing. We believe such advantages of UB-311, if ever approved for use, could
position it not only to disrupt the emerging mAb-based treatment for early AD as both a monotherapy and adjuvant therapy to existing
mAbs, but also to open up a new paradigm (i.e., for potential prophylactic use to delay or interrupt early disease onset).
Clinical Development
We completed a randomized, double-blind, placebo-controlled Phase 2a trial of two dosing regimens of UB-311 in subjects with mild
AD. The primary objective of this trial was to assess safety and immunogenicity. Secondary measures for exploratory analyses included
assessment of changes in the ADAS-Cog, CDR-SB, ADCS-ADL and MMSE ratings, along with amyloid PET imaging evaluations.
This study was intended for proof-of-concept, so no statistical hypothesis testing was planned, and exploratory analyses were performed
to evaluate trends as described below.
A total of 43 patients diagnosed with mild AD were randomized (1:1:1) to one of three treatment groups: UB-311 high- frequency
(quarterly dosing, or “Q3M”) receiving a total of seven doses, UB-311 low-frequency (every six month dosing, or “Q6M”) receiving a
total of five doses, and placebo. The high-frequency cohort, which included 14 subjects, received an initial regimen of three 300μg
injections, one injection at the trial start, one at week 4 and the final at week 12, followed by four single 300μg booster doses administered
in three-month intervals over the subsequent 12 months. The low-frequency cohort, which included 15 subjects, involved the same
initial schedule of three 300μg injections administered over the first 12-week period, followed by the administration of two 300μg
booster doses given at six-month intervals. The placebo group comprised 14 subjects.
In the Phase 2a Main Trial, UB-311 generated an immune response as measured by ELISA in 28 out of 29 subjects. Across this trial
and the Phase 1 trial, 47 of the 48 subjects (98%) that received UB-311 registered an immune response (which we define as a 95%
confidence interval separation from placebo) as measured by ELISA. The intramuscular injection produced appreciable antibody titers
against Aβ. The antibody titers remained elevated through the trial’s duration. Moreover, in vitro studies demonstrate that UB-311
generated serum anti-Aβ antibody titers against oligomers, the components that form Aβ, comparable or greater than those measured
after maximum therapeutic dosing with aducanumab. We believe these results underscore the significant promise of our therapeutic
approach.
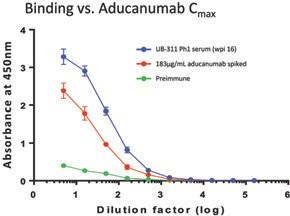
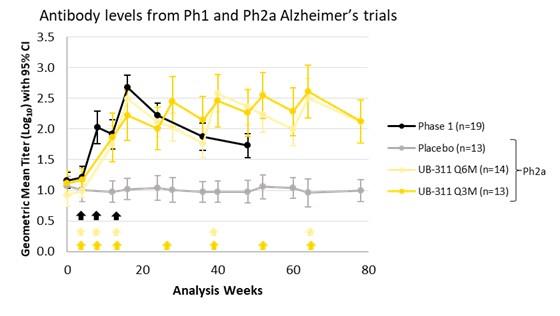
Generation of Antibodies Repeatable Across Clinical Studies, and Antibodies Bind Target with High
Specificity as Compared to Monoclonal Antibody

17
Across Phase 1 and Phase 2a trials, UB-311 generated an over 95% response rates in subjects. In a comparative in vitro study with
aducanumab, we observed that UB-311 elicited titer levels comparable to mAbs.
Our Phase 1 and Phase 2a trials demonstrated a repeatable anti-Aβ titer response. In an in vitro comparison of titers in serum from
subjects dosed with UB-311 versus pre-immune serum spiked with aducanumab at the published Cmax concentration following 10mg/kg
administration (183μg/mL), antibodies generated by UB-311 bond to Aβ oligomers similarly to or greater than aducanumab as measured
by EIA.
Exploratory analyses of clinical and imaging measures were conducted. Trends of changes in disease assessment scores suggest showing
of cognitive decline. Changes in the CDR-SB assessment at week 78 of the Phase 2a Main Trial showed a 48% slowing in cognitive
decline from baseline relative to the placebo group; changes in ADAS-Cog measurements showed a 50% slowing in decline relative to
placebo and showed a 54% slowing in decline in ADCS-ADL relative to placebo.
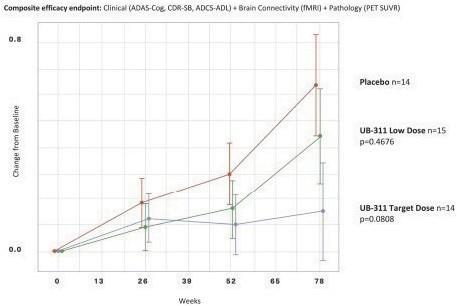
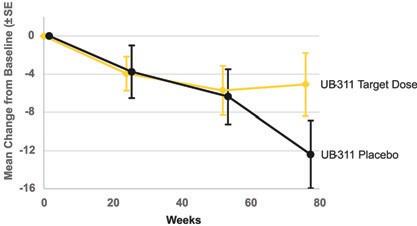
UB-311 Phase 2a Suggests Slowing of Cognitive Decline in Mild Alzheimer’s Subjects (mITT)
UB-311 Phase 2a secondary endpoint data suggested possible slowing of clinical decline by up to 50% in subjects with mild AD. These
are exploratory analyses and no statistical inference was performed.
In addition, functional MRI suggested marginal increases in connectivity in some brain regions and PET imaging showed a modest
reduction in amyloid plaque burden as measured by standard uptake value ratio. We believe these clinical and biomarker endpoints
suggest a causal effect of UB-311 impacting the underlying molecular pathology of the disease and slowing of clinical decline. Together,
these findings offer some evidence that UB-311 may exhibit disease-modifying effects.
UB-311 Phase 2a Analysis of Clinical and Biomarker Endpoints Suggests Overall Disease-Modifying Effect
Compared to placebo, UB-311 low-frequency dosing and high-frequency dosing demonstrated slowing of overall disease progression
in an independent analysis conducted by Pentara Corporation.
In addition to the composite above, Pentara Corporation performed a post hoc analysis to estimate the performance of UB-311 on the
integrated Alzheimer’s Disease Rating Scale (“iADRS”) versus placebo in the Phase 2a trial. The results of this analysis suggested that
the UB-311 target dosing regimen (quarterly dosing) on average slowed decline versus placebo by approximately 59% over 78 weeks.
18
iADRS Change from Baseline over Time vs. Placebo (Exploratory Analysis)
Compared to placebo, UB-311 (quarterly dosing) declined less on an iADRS-like clinical endpoint over 78 weeks in mild-moderate AD
subjects in the Phase 2a Main Trial. This analysis was performed by Pentara Corporation. The UB-311 Q6M group showed 26% decline
versus placebo which is not shown on the plot.
We have provided a side-by-side summary table of subject baseline characteristics below, with anti-Aβ mAbs using data from the
exploratory endpoints of the Phase 2a Main Trial, in particular CDR-SB, as well as using the post hoc iADRS-like endpoint (no head-
to-head clinical trials of UB-311 against mAbs have been performed). We believe the performance of aducanumab and donanemab on
CDR-SB and iADRS change from baseline over time, the respective primary endpoints from the pivotal trials of those mAbs, represent
meaningful references.
Post hoc
on CDR-SB change from baseline over time, and comparably to donanemab on iADRS change from baseline over time, in an
appropriately powered study, noting that the UB-311 Phase 2a Main Trial was a proof-of-concept study not powered to detect statistically
significant changes, and these are indirect comparisons with aducanumab and donanemab trials. We have provided an overview of the
sample sizes and baseline characteristics of the UB-311 Main Trial and various anti-Aβ mAb trials below.
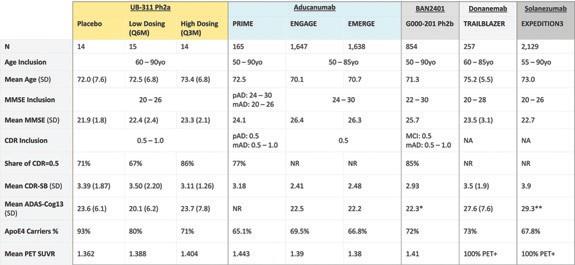
Baseline Characteristics of Various Anti-Aβ Immunotherapy Clinical Trials
The Phase 2a Main Trial recapitulated the safety and tolerability profile of UB-311 that was observed in an earlier Phase 1 trial. No
subjects discontinued trial participation due to a treatment emergent adverse effect (“TEAE”). No ARIA-E was observed in quarterly
MRI scans. Aβ-related imaging abnormalities related to microhemorrhages or hemosiderosis seemed similar between the UB-311
treatment groups and placebo group. In the Phase 2a Main Trial, six serious adverse events were observed, including three in the Q6M
dosing arm and one in the Q3M dosing arm. None was deemed related or likely related to UB-311.
Titers generated by UB-311 ramped up gradually over the course of several months, as opposed to titers following the administration of
anti-Aβ mAbs, which immediately reach Cmax. We believe this lead to the relatively low rates of ARIA-E observed in our clinical
studies of UB-311 as compared to those observed in clinical studies of mAbs. No meningoencephalitis was observed.
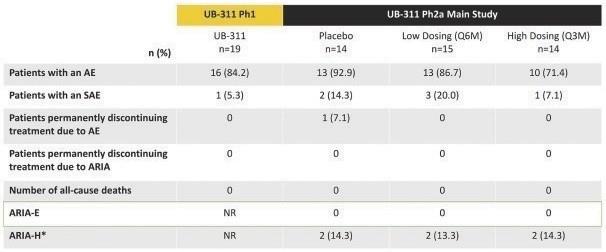
19
Summary of Safety Data from UB-311 Phase 1 and Phase 2a Trials
As depicted in the table above, UB-311 was well tolerated across Phase 1 and Phase 2a trials. The most common TEAE was site injection
reactivity, and there were no discontinuations or withdrawals due to TEAEs
An extension of the Phase 2a Main Trial, the Phase 2a LTE trial, involved the continued participation by 34 of the subjects who
participated in the Phase 2a Main Tri al for an additional 78 weeks. The objectives of the Phase 2a LTE trial were to assess the longer-
term tolerability of extended treatment with UB-311. Following a non-treatment period of up to 26 weeks, participants in the LTE trial
were segmented into two groups: those previously on drug in the Phase 2a Main Trial would receive two placebo doses and a single
300μg priming dose at the start of the LTE treatment period and those previously on placebo would receive three 300μg priming doses
over an initial 12-week period. Due to an error by the CRO responsible for administering blinded placebo and active doses to trial
subjects, which reduced the confidence of subsequently collected data, we decided to discontinue the LTE trial, having determined that
we had collected sufficient data on UB-311’s tolerability and immunogenicity. Analysis of the data collected before trial discontinuation
indicated that UB-311 was well tolerated, with return of anti-Aβ antibody titers to peak levels achieved after a gap of as much as 12
months between doses and a continued trend toward evidence of disease modification. In the Phase 2a LTE trial, six serious adverse
events were observed. One case of ARIA-E was observed in the Phase 2a LTE trial. None was deemed related or likely related to UB-
311, and all such events were recovered/resolved by the end of the study. Exploratory analyses of the clinical data generated in this
portion of the trial suggested that subjects in the treatment cohorts showed sustained improvement, as measured by the change in CDR-
SB from baseline.
We completed an open-label Phase 1 trial of UB-311 in 19 subjects with mild-to-moderate AD between the ages of 51 to 78 years. The
primary objective of the trial was to assess safety and tolerability. Secondary measures included UB-311 antibody titers along with
changes in the ADAS-Cog, MMSE and the Alzheimer’s Disease Cooperative Study-Clinician’s Global Impression of Change disease
assessment ratings. The 24-week, open label trial was designed as three intramuscular injections of 300μg, the first dose administered
at the start of the trial, a second at week four and a third at week 12. An observation study included additional follow-up visits up to 48
weeks after the first injection to assess the long-term immunogenicity and safety of UB-311. In this trial, UB-311 was well tolerated,
with the most common TEAE being injection site redness and swelling. No TEAE resulted in the discontinuation or withdrawal of any
study participant in the trial. In the Phase 1 trial, one serious adverse event was observed: a case of herpes zoster deemed unlikely related
to UB-311.
Anti-Aβ antibody titers, recorded among all study participants, approached a 100-fold increase during weeks 16 to 48 after
administration of the third 300μg injection at week 12, demonstrating the ability of UB-311 to elicit a strong immune response. Durability
of the response was reflected in elevated anti-Aβ antibody titers measurable well beyond the 24-week duration of the trial.
In a Western blot assay, we observed that UB-311 elicited antibody titers specific to toxic forms of Aβ with minimal binding to normal,
non-plaque-causing, forms of Aβ.
Pre-Clinical Data
Pre-clinical trials of UB-311 included multiple antibody titer studies involving mice, guinea pigs, macaques and baboons. Application
of specific transgenic animal models was intended to emulate both therapeutic and preventive treatment paradigms. These trials
demonstrated that UB-311 generated high antibody titers across multiple species that selectively target aggregated Aβ and both slow the
accumulation of and reduce existing Aβ pathology.
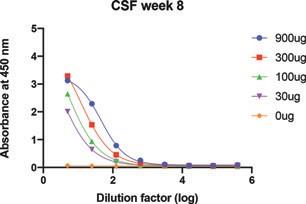
20
We also observed the ability of UB-311 induced antibodies to penetrate the BBB, as well as preferentially bind to toxic Aβ aggregates.
In our study of UB-311 in cynomolgus monkeys, we tested five escalating dose levels of UB-311: 0μg, 30μg, 100μg, 300μg and 900μg.
Each dose level was administered on weeks zero, three and six by intramuscular injection and the cerebrospinal fluid (“CSF”): serum
ratio of UB-311 calculated on week eight (two weeks after the last dose). This analysis concluded that UB-311 antibody titers were
detectable in the CSF in a dose-dependent manner with CSF: serum antibody ratios of 0.1% to 0.2%, ratios similar to published data for
mAbs in development for neurodegenerative diseases.
UB-311 Shows Dependent Response in CSF in Pre-Clinical Study
The above graphs demonstrates that UB-311 achieved CSF: serum ratios in the 0.1% to 0.2% range across five doses in a pre -clinical
study involving cynomolgus monkeys.
Development Plans for UB-311
We have completed a pre-Phase 3 meeting with the FDA and obtained guidance on the further development of UB-311.
Subject to the FDA’s review, we expect to conduct a randomized, double-blinded, placebo-controlled Phase 2b efficacy trial of UB-311
in approximately 670 subjects with early AD. The Phase 2b trial will include subjects diagnosed with early AD with MMSE scores
between 22 and 30. We will also screen to enrich for positive amyloid PET, positive tau PET and positive plasma p-tau181, in quantities
consistent with an early AD population. Subjects in the active arm will receive UB-311 as three 300μg priming doses at weeks 0, 4 and
12, followed by four 300μg booster doses every three months thereafter. The primary objective of this trial will be to assess the effect
of UB-311 on the decline of cognitive and functional performance as measured by the iADRS over the 78-week treatment period.
Secondary endpoints will include the changes from baseline measurements of other validated clinical outcomes scores. The effect of
UB-311 on specific AD biomarkers will also be evaluated, including neurofilament light arm (“NfL”), p-tau, total-tau, brain amyloid as
measured by PET, Aβ-40 and Aβ-42, hippocampal volume and whole brain volume as measured by MRI, and an assessment of certain
CSF biomarkers. We expect to initiate this trial in the second half of 2022.
Assuming positive results in the Phase 2b trial, we expect to initiate a Phase 3 trial in subjects with early AD. The Phase 3 program may
involve one, but more likely two, clinical trials, conducted at multiple international sites. Assuming positive results in the Phase 2b trial,
we may also seek FDA approval under the accelerated approval pathway, which allows for earlier approval of drugs that treat serious
conditions, and that fill an unmet medical need based on a surrogate endpoint. We expect that together, the Phase 2b trial and the Phase
3 program, if successful, will provide sufficient data to enable BLA filing with the FDA, but there can be no guarantee that we will not
need to conduct additional trials or studies prior to a BLA filing with the FDA.
We believe UB-311 could also have a potential therapeutic benefit in a prophylactic setting for the prevention of AD in high-risk patients.
We may seek to further develop UB-311 for the prevention of AD.
UB-312
An Overview of Parkinson’s Disease
Parkinson’s disease currently affects approximately one million people in the United States and more than 10 million people worldwide.
The economic burden of PD is estimated at $52 billion in the United States alone. PD is a chronic and progressive neurodegenerative
disorder that affects predominately dopamine-producing (“dopaminergic”) neurons in the substantia nigra area of the brain. Although
the mechanisms responsible for the dopaminergic cell loss in PD are not fully elucidated, several lines of evidence suggest that α-
synuclein plays a central role in the neurodegenerative process.
21
Alpha-synuclein is a protein highly expressed in neurons, mostly at presynaptic terminals, suggesting a role in synaptic vesicle
trafficking, synaptic functions and in regulation of neurotransmitter release at the synapse. Duplications, point mutations or single
nucleotide polymorphisms in the gene encoding α-synuclein are known to cause or increase the risk of developing PD or LBD. Mutations
have been shown to primarily alter the secondary structure of α-synuclein, resulting in misfolded and aggregated forms of α-synuclein
(i.e., pathological forms). While mutations in the α-synuclein gene are rare, aggregates of α-synuclein in the form of Lewy bodies (“LB”)
and Lewy neurites are common neuropathological hallmarks of both familial and sporadic PD, suggesting a key role of α-synuclein in
PD neuropathogenesis. Moreover, preformed fibrils of α-synuclein can induce the formation of LB-like inclusions and cellular
dysfunction in cell-based assays as well as in pre-clinical animal models. Together, these data strongly suggest that targeting pathological
forms of α-synuclein has therapeutic potential.
Limitations of Current Therapies
Most approved therapeutic products are aimed at compensating for the dopaminergic deficits and only provide symptomatic relief. While
existing products can indeed provide meaningful symptomatic relief, they often produce significant side effects and lose their beneficial
effects overtime. On the other hand, there are no currently approved disease-modifying therapeutics for PD.
Immunotherapy approaches targeting α-synuclein have been shown to ameliorate α-synuclein pathology as well as functional deficits
in mouse models of PD and are now being investigated in the clinic. These include passive immunization therapy using humanized or
human anti-α-synuclein mAbs or active immunization therapy aimed at inducing a humoral response against pathological α-synuclein.
These approaches have thus far demonstrated good tolerability profiles in Phase 1 clinical trials. A Phase 2 clinical trial in PD subjects
with prasinezumab, a mAb that preferentially recognizes oligomeric and fibrillar forms of α-synuclein significantly reduced subjects’
motor function decline and delayed clinically meaningful worsening or motor symptoms, compared with placebo. Despite encouraging
preliminary data observed with this mAb, we expect that mAbs, even if approved as therapeutic for PD, would be burdened by the
general challenges of cost and administration.
Our Product Candidate: UB-312
We are developing UB-312, an anti-α-synuclein product candidate, as a treatment for PD and other synucleinopathies. We believe that
UB-312 has the potential to be established as a disease-modifying treatment modality for PD, and possibly for LBD and MSA. Pre-
clinical data indicated that UB-312 elicits antibodies that preferentially recognize pathological forms of a-synuclein and improves motor
performance in mouse models of α-synucleinopathies. Preliminary clinical data from our ongoing Phase 1 trial indicate that UB-312
elicits antibody levels sufficient to cross the BBB (i.e., detectable in CSF). In 2018, the European Medical Agency (“EMA”) granted
UB-312 orphan designation for MSA.
Clinical Development
We have conducted Part A of a randomized, placebo-controlled, double-blind, dose-escalating, single- center Phase 1 clinical trial of
UB-312 in which 50 healthy volunteers between the ages of 40 and 85 years received three intramuscular doses of either UB-312 or
placebo. During this 44-week Part A trial, subjects received three doses (on weeks 1, 5 and 13) with escalating doses ranging from
40μg to 2,000μg. Immunogenicity was evaluated by measuring changes in serum anti-α-synuclein antibody concentrations during the
course of the study. Data from Part A indicated that UB-312 is generally well tolerated, with no significant safety findings. Data from
Part A also suggested that UB-312 is highly immunogenic, with all individuals in the 300μg/dose group showing detectable anti-α-
synuclein antibodies in both serum and CSF samples. CSF: serum ratios appeared similar to those observed in UB-311 non-human
primate studies (approximately 0.2%), and to those observed in clinical trials of mAbs. Based on these results, we are now evaluating
two dosing regimens of UB-312 in Part B of the Phase 1 trial: three doses of 300μg, and one dose of 300μg followed by two doses of
100μg. Part B will evaluate UB-312 and placebo in 20 PD subjects and began enrollment in January 2022. In addition to the endpoints
evaluated in Part A, an exploratory endpoint involving a clinical assessment using the Movement Disorder Society – Unified
Parkinson’s Disease Response Score will be used.
The Michael J. Fox Foundation (“MJFF”) is funding a 2-year collaborative project between Vaxxinity, Mayo Clinic, and University of
Texas Houston using CSF collected from individuals enrolled in Part B of the Phase 1 trial of UB-312. This work will evaluate the
potential of protein misfolding cyclic amplification (“PMCA”) to assess target engagement and will also aim to characterize the anti-
α-synuclein antibodies produced after immunization with UB-312. Demonstrating whether pathological forms of α-synuclein are
detectable in the CSF of PD subjects, and whether UB-312-derived antibodies prevent the formation of α-synuclein seeds measured by
PMCA, might provide a meaningful surrogate marker of target engagement.
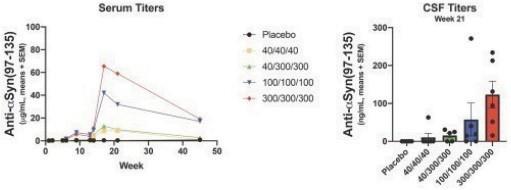
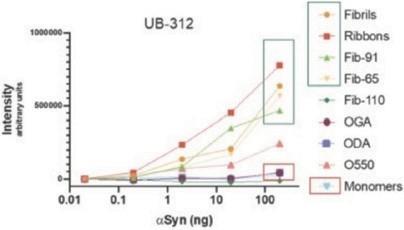
22
UB-312 Demonstrated Dose-Dependent Response in Phase 1 Part A Trial Including Penetration of Titers into CSF
Across four cohorts, UB-312 demonstrated a dose-dependent immunogenic response. Antibodies generated by UB-312 were readily
detectable in CSF, indicating BBB penetration with a CSF: serum ratio of approximately 0.2%.
We paused dosing in high dose cohorts in Part A of the trial after one subject developed an adverse effect (“AE”) of special interest (i.e.,
Grade 3 flu-like symptoms) shortly after receiving the second 1000μg dose of UB-312. Although this AE was transient and not a serious
adverse event (“SAE”), data collected until that point suggested that the 100μg and 300μg dose levels were well tolerated and yielded
relatively high anti-α- synuclein titers. During the evaluation of the AE, the COVID-19 pandemic was becoming increasingly pervasive
throughout Europe, increasing the risk to healthy volunteers participating in the trial. We therefore did not resume dose escalation and
selected 100μg and 300μg doses for Part B in PD subjects.
Pre-Clinical Data
We have conducted pre-clinical studies of UB-312 across multiple animal species, including mice and guinea pigs. These trials
demonstrated that our product candidates, including UB-312, generated high antibody titers to α-synuclein across animal species. In
addition, in vitro studies provided evidence that anti-α-synuclein antibodies produced after UB-312 immunization are highly selective
to pathological α-synuclein, and do not bind to normal α-synuclein.
UB-312 Demonstrates Selective Binding Towards α-Synuclein Fibrils and Ribbons
This in vitro slot blot analysis of sera from guinea pigs dosed with UB-312 demonstrates that antibodies induced by UB-312 bind to α-
synuclein fibrils and ribbons, the toxic forms of α-synuclein believed to underlie PD, more strongly than they bind to monomers, the
normal form of α-synuclein in the body. We believe this preference will allow UB-312 antibodies to avoid target-mediated clearance by
monomers and bind selectively to the toxic species
(Nimmo et al., Alzheimers Res Ther. 2020;12:159).
Anti-α-synuclein antibodies produced by UB-312 immunization specifically bind pathogenic species of α-synuclein, including
aggregated fibrils, oligomers and ribbons, while demonstrating low affinity for the monomer. This species selectivity contrasted with
Syn-1, a commercial research mAb used as a control, which failed to differentiate the toxic variants.
In an in vivo study of UB-312 using a transgenic mouse model of PD, we demonstrated prevention of motor deficits in treated animals,
which was associated with significant reduction of brain oligomeric forms of α- synuclein. We believe this data supports the potential
of UB-312 to prevent behavioral motor deficits and reduce toxic forms of α-synuclein.
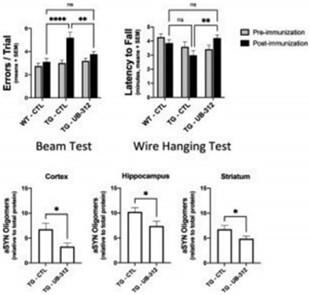
23
UB-312 Demonstrates Improvement in Motor Symptoms in Pre-Clinical Study
UB-312 immunization in a transgenic mouse model (α-synuclein overexpression) demonstrates improvement in beam test and wire
hanging test, and reductions in α-synuclein oligomers in various brain regions (Nimmo et al., Acta Neuropathol. 2022;143:55-73).
We have also observed by immunohistochemistry that serum antibodies from guinea pigs dosed with UB-312 can bind to aberrant α-
synuclein in PD, LBD and MSA brain sections.
Finally, antibodies derived from UB-312 showed no off-target binding on human tissue sections. UB-312-treated transgenic mice
showed no signs of neuroinflammation, and GLP toxicity studies in rats indicated a good non-clinical safety and tolerability profile. We
believe our preclinical data suggest that UB-312 may potentially induce a well-tolerated, strong and specific IgG response against
pathological forms of
a-synuclein
in PD subjects.
Development Strategy
While certain portions of this Phase 1 trial were interrupted by the COVID-19 pandemic, Part A in 50 healthy volunteers was completed
in 2020, and we began dosing PD subjects in Part B in early 2022. In Part B we expect to include exploratory endpoints potentially
relevant to PD, such as total and free α-synuclein in serum and CSF, in addition to T-cell ELISpot analyses and antibody characterization.
Upon the completion of the Phase 1 trial, we expect to advance UB-312 into further clinical development, which may comprise trials
for various synucleinopathies.
Other Neurodegeneration Programs
We are actively engaged in additional initiatives related to neurodegenerative disorders. One of these programs focuses specifically on
tau-protein pathology and its involvement in diseases such as AD and related tauopathies. We believe that targeting different pathological
tau variants simultaneously may enhance treatment efficacy, which will most likely require targeting multiple epitopes concomitantly.
Using our Vaxxine Platform, we have constructed combination product candidates that target these multiple epitopes and have
successfully demonstrated their utility to raise therapeutic antibody titers in in vitro studies as well as early in vivo animal models.
We are also investigating the use of a combination of product candidates targeting Aβ, α-synuclein, tau and C9ORF79 dipeptide repeat
proteins, as multiple proteins could be implicated in neurodegenerative diseases.
Next Wave Chronic Disease Treatments
Pathological endogenous proteins (“self-proteins”) drive a wide range of chronic diseases. While mAbs and small molecules have
provided therapeutic benefits in the treatment of these diseases, inherent limitations of these drug classes have restricted access and
adherence to these treatment modalities globally.
Our next wave chronic disease program is initially focused on migraine and hypercholesterolemia. Monoclonal antibodies have been
approved in both therapeutic areas; however, their high costs have limited access and generally limited use to relatively severe disease.
We aim to develop product candidates in these therapeutic areas that could offer similar efficacy as mAbs at a meaningfully lower cost
24
and improved administrative convenience to patients, thereby potentially allowing for access to broader patient populations versus
mAbs, and greater efficacy than small molecules.
UB-313
An Overview of Migraine
Migraine is a chronic and debilitating disorder characterized by recurrent attacks lasting four to 72 hours with multiple symptoms,
including typically one-sided, pulsating headaches of moderate to severe pain intensity that are associated with nausea or vomiting,
sensitivity to sound and sensitivity to light. Over 90% of the patients are unable to function normally during a migraine attack. Many
experience comorbid conditions such as depression, anxiety and insomnia.
The Migraine Research Foundation ranks migraine as the world’s third most prevalent illness. The disease affects 39 million individuals
in the United States and approximately one billion individuals globally. Patients generally suffer from chronic or episodic migraines.
Chronic migraine is defined as 15 headache days or more per month, while episodic migraine is defined as fewer than 15 headache days
per month. Both acute and prophylactic treatments are used to address chronic and episodic migraines.
CGRP’s Role in Migraine
CGRP is a neuropeptide found throughout the body, including in the spinal cord. CGRP activates CGRP receptor in the
trigeminovascular system, which is located within pain-signaling pathways, intracranial arteries and mast cells. Activation of the CGRP
receptor has been demonstrated to induce migraine in migraineurs. Multiple anti-CGRP therapies have been approved for the treatment
of migraine.
Limitations of Current Therapies
Since the early 1990s, there has been minimal improvement in the standard treatment for migraine. Treatments are characterized as elite
acute or prophylactic. Triptans are the current first-line prescription therapy for the acute treatment of migraine, with over 15 million
annual prescriptions written in the United States.
Prophylactic medications approved for migraine include beta blockers, such as propranolol, topiramate, sodium valproate and botulinum
toxin, branded as Botox. However, many of these medications provide limited clinical benefit. In addition, they are often not well
tolerated, with AEs such as cognitive impairment, nausea, fatigue and sleep disturbance.
Therapeutics targeting the CGRP pathway represent an emerging treatment paradigm. Three anti-CGRP mAbs were approved by the
FDA in 2018 for the prophylactic treatment of migraine in adults. These mAbs, erenumab-aooe (Aimovig), fremanezumab-vfrm (Ajovy)
and galcanezumab-gnlm (Emgality), are all administered subcutaneously. Their side effects are generally mild, including pain and
redness at the site of injection, nasal congestion and constipation. Studies show that these mAbs reduce the number of headache days
by 50% or more in approximately 50% of patients. Sales for marketed and clinical-stage anti-CGRP therapeutics are projected to reach
approximately $7.4 billion by 2026. Despite the commercial success that this class represents, many of these treatments require frequent
administration, creating inconvenience for patients.
Our Product Candidate: UB-313
We are developing UB-313 as a prophylactic treatment initially for chronic migraine. We believe UB-313 has the potential to improve
upon the current treatments for chronic migraine in multiple aspects: we expect UB-313 will require administration quarterly to annually
in contrast to monthly to quarterly for currently marketed mAbs and frequent administration for small molecules. Furthermore, a
potential long durability of response may offer physicians and patients the option to administer UB-313 in an office setting, which can
potentially improve adherence. We expect the cost of UB-313 treatment, if approved, to be lower than that of mAbs for migraine.
Pre-Clinical Studies
We have completed both in vitro and in vivo pre-clinical studies of UB-313. We used an in vivo proof-of-concept capsaicin-induced
dermal blood flow model in mice to demonstrate target engagement of the marketed CGRP-targeting mAbs. In this model, we observed
similar rates in reduction of dermal blood flow as fremanezumab in a head-to-head comparison against fremanezumab.
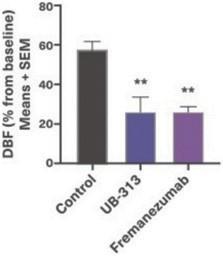
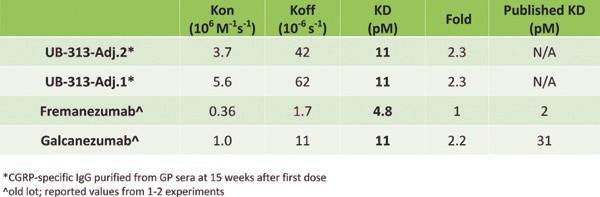
25
UB-313 Reduces Capsaicin-Induced Dermal Blood Flow in Mice
**Dunnett’s: Ctl vs Vac 1p < 0.05; Ctl vs Vac 2 p < 0.05
In this preliminary study, dermal blood flow measurements were taken 17 weeks following the first dose of UB-313. There were 3 to 11
animals per treatment group. Reduced dermal blood flow indicates target engagement with CGRP. UB-313 reduced dermal blood flow
versus the control with an approximately similar magnitude to fremanezumab, which was administered 24 hours prior to the capsaicin
test.
We observed similar results in a capsaicin / dermal blood flow model in rats, comparing a rat version of UB-313 head-to-head against
galcanezumab.
Our
in vivo
tested. Characterization of the antibodies produced after immunization with UB-313 indicated that they have limited, if any, off-target
potential, are primarily IgG1 and IgG2, potently bind to CGRP and potently block CGRP activity
in vitro
. We refer to potency as the
amount of drug required to produce a pharmacological effect of given intensity and is not a measure of therapeutic efficacy. In a
comparison of binding affinities with fremanezumab and galcanezumab, UB-313-induced IgG antibodies demonstrated comparable
binding affinities.
UB-313 Demonstrated Induced Antibodies Comparable to Approved CGRP mAbs
We evaluated UB-313 formulations with two different adjuvants in comparison to fremanezumab and galcanezumab; both formulations
demonstrated comparable IgG to these two approved CGRP mAbs.
Additional
in vitro
in vitro
activity to CGRP-targeted mAbs.
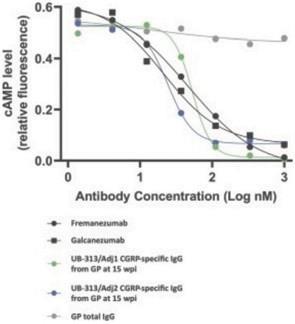
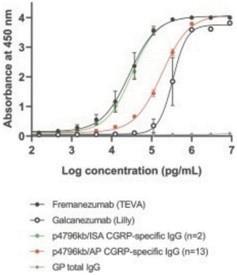
26
UB-313 Induced IgGs Have Comparable In Vitro Activities to Marketed CGRP mAbs
In a cyclic AMP (“cAMP”) production assay conducted in human SK-N-MC cells, antibodies taken from the serum of guinea pigs 15
weeks following the first injection of UB-313 demonstrated similar properties to two approved CGRP mAbs.
Moreover, the binding potency of UB-313 was determined to be comparable to these mAbs.
UB-313 Induced IgGs Demonstrate Comparable Binding Potencies to Marketed CGRP mAbs
Antibodies taken from the serum of guinea pigs 15 weeks following the first injection of UB-313 demonstrated similar binding potencies
to two approved CGRP mAbs as measured by ELISA.
Development Strategy
We have identified a lead candidate and anticipate submitting a clinical trial application (“CTA”) or an IND in 2022. While we are
currently developing UB-313 as a potential treatment of chronic migraine, depending on successful clinical results, we may seek to
address episodic migraine and cluster headaches as well.
27
PCSK9
An Overview of Hypercholesterolemia
Hypercholesterolemia is the presence of high levels of cholesterol in the blood and typically results from a combination of environmental
and genetic factors. Cholesterol is transported in the blood plasma within particles called lipoproteins. Lipoproteins are classified by
their density: very low-density lipoprotein, intermediate density lipoprotein, LDL and high density lipoprotein (“HDL”). All lipoproteins
carry cholesterol, but elevated levels of lipoproteins other than HDL, particularly LDL, are associated with the development of
cardiovascular disease. Approximately 2 billion people worldwide have elevated levels of LDL, potentially putting them at risk for
cardiovascular disease.
Although hypercholesterolemia itself is asymptomatic, elevation of serum cholesterol can over time lead to atherosclerosis. Over many
years, elevated serum cholesterol contributes to formation of atheromatous plaques in the arteries. These plaque deposits can in turn
lead to progressive narrowing of the involved arteries. Smaller plaques may rupture and cause a clot to form and obstruct blood flow. A
sudden blockage of a coronary artery may result in a heart attack. A blockage of an artery supplying the brain can cause a stroke. If the
development of the stenosis or occlusion is gradual, blood supply to the tissues and organs slowly diminishes until organ function
becomes impaired.
PCSK9 is mainly expressed in the liver and, to a lesser extent, in the small intestine, kidney, pancreas and the central nervous system.
The LDL receptors (“LDLR”) at the cell surface bind and initiate ingestion of LDL particles from extracellular fluid into cells, leading
to a reduction in serum LDL levels. PCSK9 protein plays a major regulatory role in cholesterol homeostasis, mainly by reducing LDLR
levels on the plasma membrane, which leads to decreased metabolism of LDL by the cells. Inhibition of PCSK9 prevents this reduction
in LDLR levels on the plasma membrane, and in consequence the cellular process of internalizing LDL particles, resulting in a reduction
of LDL.
Limitations of Current Therapies
Statins are the most commonly used drugs to treat hypercholesterolemia and result in a pronounced reduction in LDL. The unambiguous
benefits of statins, together with the prevalence of coronary heart disease, have made statins the most highly prescribed drug class in
developed countries. However, many patients are unable to achieve targeted lipid levels despite intensive statins therapy. In addition,
continued patient adherence to statin therapy, which is necessary to maintain a lower risk for cardiac events, is variable but considered
to be low – as low as 30% to 40% after two years in persons following a myocardial infarction. Importantly, at the transcriptional level,
statins up-regulate not only LDLR, but also PCSK9, causing the so-called paradox of statin treatment. Although statins induce a
beneficial increase in LDLR, they also increase PCSK9, thus leading to LDLR degradation, which indirectly increases LDL, mitigating
the overall LDL reduction that statins otherwise cause. Given the limitations in efficacy and adherence, targeting PCSK9 in combination
with statins treatment is an emerging treatment paradigm for hypercholesterolemia.
Two mAbs that inhibit activity have received FDA approval, alirocumab (Praluent) and evolocumab (Repatha). These drugs were
initially approved to treat the genetic condition heterozygous familial hypercholesterolemia, although the approved indications were
expanded after the publication of studies demonstrating that the use of a PCSK9 inhibitor in conjunction with a statin significantly
reduced the risk for major cardiovascular events, including heart attack, stroke, unstable angina requiring hospitalization or death from
coronary heart disease. In addition, inclisiran (Leqvio), an siRNA inhibitor of PCSK9 synthesis, was approved by the EMA in late 2020
for the treatment of heterozygous familial hypercholesterolemia in addition to other dyslipidemia.
While alirocumab and evolucumab have demonstrated clinical benefit, their commercial potential has been limited by their pricing. Both
launched with a wholesale acquisition price exceeding $14,000 annually, but prices for both were subsequently reduced in 2018.
Nevertheless, this drug class generated sales of approximately $1.3 billion in 2020 and is expected to grow to approximately $5.2 billion
by 2026, including the addition of inclisiran to the market. In addition, both must be administered bi-weekly, which represents what we
believe to be a frequent and inconvenient administration schedule for patients. While inclisiran represents an improved administration
schedule compared to alirocumab and evolucumab, as it must be administered only twice annually, we believe that it may encounter
similar pricing challenges due to the published cost effectiveness price.
Our Hypercholesterolemia Program
We are developing an anti-PCSK9 product candidate to treat hypercholesterolemia. Our program is dedicated to developing a product
candidate that has long-acting treatment duration, which we believe will offer a more convenient treatment regimen of every six to 12
months compared to the up to bi-weekly dosing required by some mAbs. We believe that lower manufacturing costs commensurate with
the requirement of meaningfully less drug substance relative to mAbs, coupled with our ability to achieve commercial scale production
rapidly may promote expanded use of this drug class as a first-line therapy treating a greater number of hypercholesterolemia patients
than currently treated with mAbs.
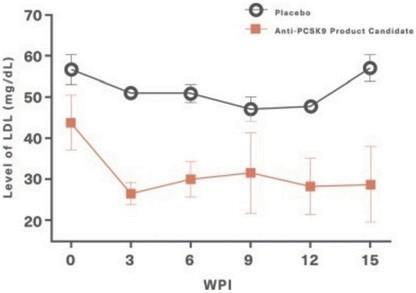
28
Pre-Clinical Studies
Pre-clinical studies of our anti-PCSK9 vaccine indicate that our product candidate generates therapeutic titer levels of anti-PCSK9
antibodies. These studies also indicate that it produces a high response rate among dosed animals. We achieved proof-of-concept in a
guinea pig model, reducing LDL cholesterol by more than 30% over the 15-week treatment duration, comparable to the reductions
observed with the use of anti-PCSK9 mAbs.
Anti-PCSK9 Product Candidate Reduces LDL by 30 to 50% Over 15 Weeks in Guinea Pigs (n=6)
Development Strategy
We plan to initiate IND-enabling studies of a lead anti-PCSK9 candidate in 2022.
Next Stage Development Candidates
In addition to our initial focus on migraines and hypercholesterolemia, we believe our Vaxxine Platform can generate product candidates
for a range of chronic diseases. We are evaluating opportunities across multiple disease areas, including allergy (e.g., chronic
rhinosinusitis, atopic dermatitis, food allergy), autoimmune (e.g., psoriasis, psoriatic arthritis), pain (e.g., peripheral neuropathy, diabetic
neuropathy) and bone and muscle deterioration (e.g., osteopenia, sarcopenia of aging) indications as they may apply to geriatrics and
space travel health.
COVID-19 Program
An Overview of COVID-19
COVID-19, caused by SARS-CoV-2, has rapidly swept throughout the world. The WHO declared COVID-19 a public health emergency
of international concern. As of February 22, 2022, there have been more than 420 million laboratory-confirmed COVID-19 patients and
more than 5.8 million deaths worldwide. Common symptoms of COVID-19 are fever, cough, lymphocytopenia and chest radiographic
abnormality. A proportion of patients recovering from COVID-19 continue shedding virus for days, and asymptomatic carriers may also
transmit SARS-CoV-2, indicating a risk of a continuous and long-term pandemic. According to Our World in Data (ourworldindata.org),
as of March 2, 2022, approximately 87% of people in low-income countries have not received a single dose of a COVID-19 vaccine.
SARS-CoV-2 is an enveloped, single-stranded, positive-sense RNA virus belonging to the family
Coronavidae
coronavirus. The genome of SARS-CoV-2 encodes one large Spike (“S”) protein that plays a pivotal role during viral attachment to the
host receptor, angiotensin converting enzyme 2 (“ACE2”), and entry into host cells. The S protein is the major principal antigen target
for vaccines against human coronavirus, including SARS-Co-V-2. Neutralizing antibodies targeting the receptor binding domain
(“RBD”) subunit of the S protein block the virus from binding to host cells. Over 90% of all neutralizing antibodies produced in response
to infection are directed to the RBD subunit, and mAbs that have shown therapeutic activity target epitopes on the RBD.
More than twenty vaccines are authorized for use in one or more countries around the world, including three in the United States. These
vaccines are based on the S protein of the SARS-CoV-2, but rely on different mechanisms for presentation or expression of the S antigen,
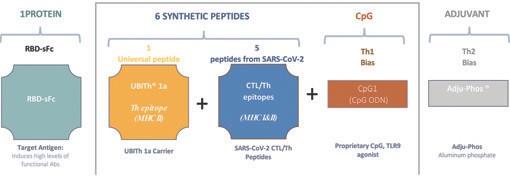
29
including whole inactivated virus, defective adenovirus vectors (three different types) or mRNA. All have been shown to be safe and
effective in placebo- controlled clinical trials. Antiviral drugs and mAbs have limited availability and effectiveness.
COVID-19 Vaccine Market
Disparities in COVID-19 vaccine availability and distribution continue to grow despite the myriad of procurement efforts underway.
There exists a shortfall in the supply of COVID-19 vaccines globally for primary immunization, driven by supply constraints along with
substantial challenges around distribution, delivery and poor logistical capacity to administer doses. This primary immunization shortfall
is disproportionately pronounced in low- and middle-income countries (“LMICs”). We estimate that in order for these countries to
approach herd immunity (modeled at 70% vaccinated), there remains a shortfall of hundreds of millions of doses (excluding India and
China).
Furthermore, as knowledge of SARS-CoV-2 and its circulating variants (e.g., Omicron) and vaccination efforts grow, the need for
booster immunizations has become more apparent. We estimate that the size of the COVID-19 vaccine booster dose market globally in
2022 will exceed 1.5 billion doses. We expect the need for heterologous booster vaccines with low reactogenic profiles, broad variant
coverage, durable immunity and mechanisms of action different from presently authorized vaccines to continue through 2022.
UB-612: Our COVID-19 Vaccine Initiative
We are developing UB-612 as a product candidate for the prevention of COVID-19. UB-612 is designed to activate both antibody and
cellular immunity against multiple viral targets. The vaccine is composed of a recombinant S1-RBD-sFc fusion protein combined with
rationally designed synthetic Th and CTL epitope peptides selected from the S2 domain of the spike, membrane (“M”), and nucleocapsid
(“N”) proteins. These peptides bind to MHC I and II without significant genetic restriction, so that they may be recognized by the entire
human population. Our mixture of peptides is designed to elicit T-cell activation, memory recall and effector functions similar to those
of natural COVID-19. The S1-RBD-sFc fusion protein incorporates essential B-cell epitopes that promote the generation of neutralizing
antibodies to the RBD of SARS-CoV-2. UB-612 is formulated with Adju-Phos, an adjuvant widely used in many approved vaccines
globally. For added safety, synthetic peptides in UB-612 are adsorbed by our propriety CpG1 excipient, a Toll-like receptor 9 agonist
molecule, known to help to stimulate balanced T-cell immunity in humans. UB-612 can be stored and shipped at 2° to 8°C (conventional
cold chain refrigerated temperatures). An EUA application for UB-612 was denied by the TFDA in August 2021 because the neutralizing
antibody response generated by UB-612, as compared to a designated adenovirus vectored vaccine, did not meet the TFDA’s specified
evaluation criteria but, in collaboration with UBIA, we are appealing the decision. We are now also pursuing paths to authorization for
UB-612 as a heterologous boost and have agreement with a high income regulator about our development approach.
Components of the UB-612 Multitope Vaccine Product Candidate
UB-612’s construct contains an S1-RBD-sFc fusion protein for the B-cell epitopes, plus five synthetic Th/CTL peptides for class I and
II MHC molecules derived from SARS-CoV-2 S2, M and N proteins, and the UBITh1a peptide. These components are formulated with
CpG1, which binds the positively charged (by design) peptides by dipolar interactions and also serves as an adjuvant, which is then
bound to Adju-Phos adjuvant to constitute the UB-612 product candidate.
Clinical Development
In March 2022, Vaxxinity initiated a Phase 3 pivotal study to compare the immune responses stimulated by mRNA (BNT162b2),
adenovirus (ChAdOx1-S), inactivated virus (Sinopharm BIBP) COVID-19 vaccines, and UB-612, when delivered as third dose boosters.
This is an active-controlled, randomized, multicenter study being conducted in several countries under a platform protocol which enrolls
subjects 16 years and older who completed a two-dose primary immunization with one or more of the vaccines mentioned above. Eligible
subjects will be randomized into one of two treatment arms to receive a single dose of UB-612 or an active comparator. The primary
objective of the study is to determine non-inferiority of UB-612-stimulated neutralizing antibodies against the comparator vaccines.
Additionally, Omicron neutralizing antibodies, non-neutralizing antibodies and T cell responses will be analyzed as part of secondary
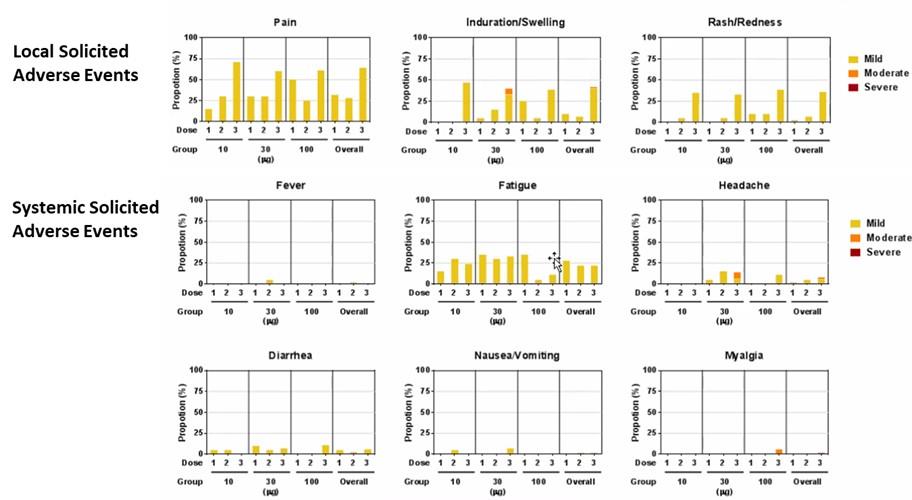
30
and exploratory objectives. We expect that, if successful, this study may enable conditional approval of UB-612 in multiple high income
countries and LMICs.
3-Dose Data: Phase 1 Extension Trial
In early 2021, we completed an open-label dose escalation Phase 1 clinical trial to evaluate the safety, tolerability and
immunogenicity of UB-612 in healthy adults in Taiwan. This trial consisted of three cohorts of 20 subjects each. The first cohort
received two intramuscular injections of 10μg doses of UB-612, the second cohort received two 30μg doses and the third cohort
received two 100μg doses. The first dose in each cohort was administered at the start of the trial, with the second dose administered
on day 28.
In a Phase 1 extension trial, 50 subjects from Phase 1 received a third booster dose of UB-612 approximately 7-9 months after their
second dose (100µg).
After one and two doses in the Phase 1 trial, UB-612 was considered to be generally safe and well tolerated, with a low frequency of
solicited and unsolicited AEs, which were all Grade 1 (mild) in severity. We selected the highest dose (100μg) to take into the Phase
2 trial.
Similarly, in the Phase 1 extension trial, UB-612 was generally well tolerated after a third dose, with no vaccine-related SAEs
reported.
Local and Systemic Solicited Adverse Events Following 1, 2, and 3 Doses of UB-612 at Varying Dose Levels
Solicited adverse event data from Phase 1 and Phase 1 extension (n=50) suggests UB-612 is well tolerated after each of three doses
across varying dose levels.
Immunogenicity and safety data from the Phase 1 extension suggests that UB-612 elicits a multi-fold increase in neutralizing
antibody titers upon third dose, significantly exceeding those observed in human convalescent sera, and that the third dose is well
tolerated with no vaccine-related SAEs reported. Published studies have shown a correlation between efficacy in randomized
controlled trials and the ratio of neutralizing titers in sera from vaccinated subjects to titers in human
convalescent sera.

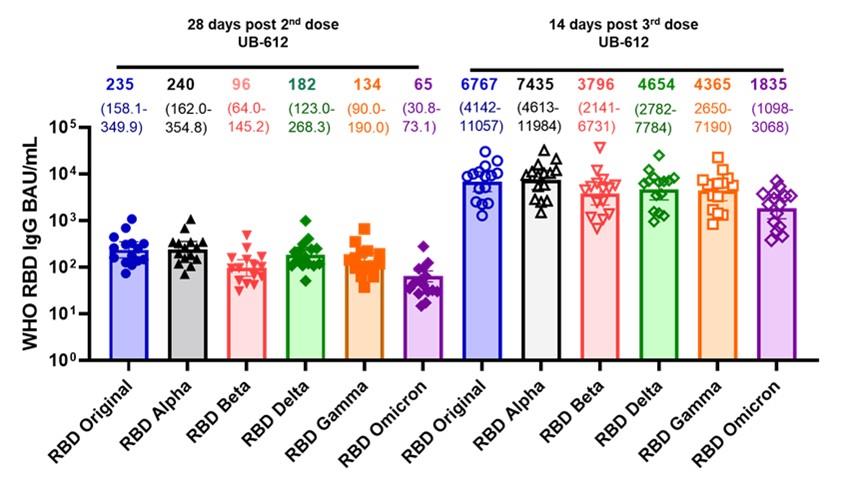
31
UB-612 Neutralizing Antibodies Against Wuhan Strain of SARS-CoV-2
(GMT, WHO International Units)
UB-612 Phase 1 extension (n=50) demonstrated that a dose of 100μg UB-612 following three doses of various sizes of UB-612 elicits
a multi-fold increase in neutralizing antibody titers.
In collaboration with University College London and VisMederi, we analyzed sera from subjects immunized with three doses of UB-
612. Data demonstrated that UB-612 elicited a broad IgG antibody response against multiple SARS-CoV-2 variants of concern,
including, Alpha, Beta, Delta, and Gamma, and Omicron, and higher levels of neutralizing antibodies against Omicron than three
doses of an approved mRNA vaccine.
IgG Binding to RBD by Variant of Concern after 2 and 3 Doses of UB-612
IgG binding titers against SARS-CoV-2 major variants of concern in sera collected 28 days after 2 doses and 14 days after 3 doses of
UB-612 (100µg) from Phase 1 trial participants (n=15). The loss of antibody bindings to RBD of variants compared with the original
RBD (Wuhan) remains stable between 2 doses and 3 doses of UB-612 vaccine, along with a high overall increase in levels of binding
antibodies to RBD.
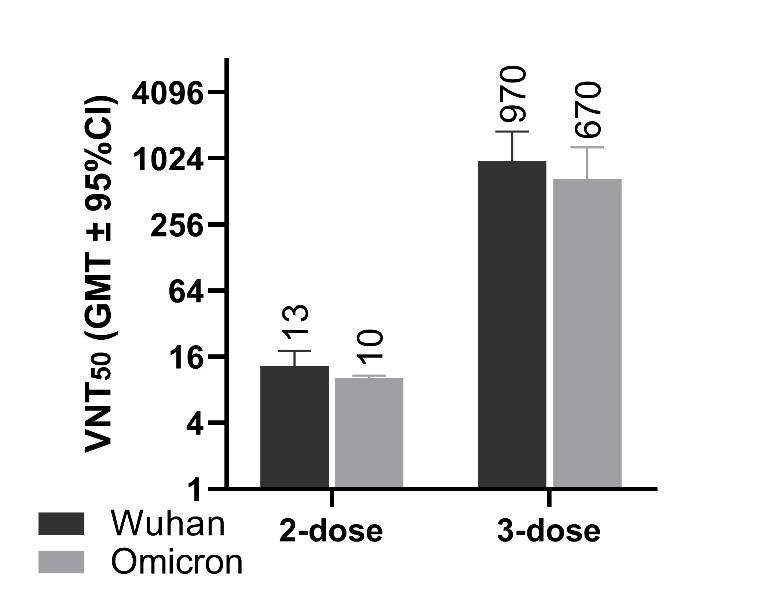
32
Third immunization with UB-612 Produces Neutralizing Antibodies Against Omicron
Phase 1 extension subjects (n=15) received primary series with UB-612 100µg. Serum is taken 28 days after the second dose and 14
days after the third booster immunization administered 7-9 months after the primary series. Live virus neutralization test against
Wuhan and Omicron are performed at VisMederi; results are expressed as virus neutralization antibody GMT ± 95% CI.
2-Dose Data: Phase 2 Trial
A randomized, placebo-controlled, multi-center Phase 2 trial of UB-612 in 3,850 healthy volunteers aged 12 to 85 is ongoing in Taiwan.
Subjects in this trial receive two doses of 100μg UB-612, or placebo, 28 days apart. The objectives of this trial include the analysis of
safety and immunogenicity of UB-612, in particular, antigen-specific antibodies to UB-612, the seroconversion rate and lot-to-lot
consistency of antibody responses. An interim analysis of data from this Phase 2 trial in healthy volunteers 18 years and older based on
the data cut-off date of June 27, 2021 was submitted to the TFDA as part of a filing for an EUA in Taiwan. The EUA was denied in
August 2021 by the TFDA, but, in collaboration with UBIA, we are appealing that decision.
In data from over 3,750 subjects, UB-612 appears well tolerated, with no significant safety findings to date. AEs were generally
mild, and no related SAEs were observed. Local injection site AEs occurred in half of the subjects, the most frequent being injection
site pain. Systemic AEs occurred in less than half of the subjects, and the incidence was similar in the active and placebo groups,
except for muscle pain which was more frequent in the active group. Aside from muscle pain, systemic reactions were comparable
across the active and placebo groups, with less than 10% of subjects in either group experiencing fever or chills. Systemic AEs were
similar after the first and second doses. The vast majority of AEs were mild (Grade 1), and all were self-limited. No subject had a
severe (Grade 3) local reaction. The incidence of severe (Grade 3) systemic reactions was <0.1%.
The Phase 2 interim analysis suggests that Phase 1 observations on immunogenicity, neutralizing titers and tolerability are repeatable,
with an overall seroconversion rate of 94.7% one month after the second dose. In a live virus (Wuhan) neutralization test, sera collected
from UB-612 vaccinated younger adults (19-64 years, n=322), 28 days after the second dose (day 57) were estimated to reach geometric
mean titers (“GMT”) of 102 of 50% virus-neutralizing antibodies (VNT
50
).
Sera collected from a subset of subjects (n=48) 28 days after
the second immunization was shown to neutralize several SARS-CoV-2 variants, with the loss of neutralization activity against Delta
estimated at 1.39-fold when compared to the neutralizing antibodies against the parental Wuhan virus.
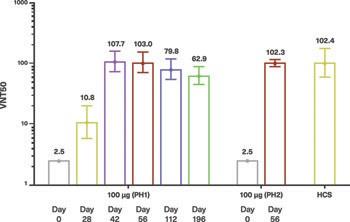
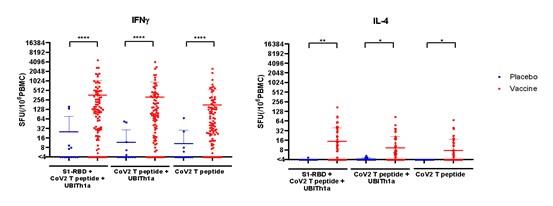
33
Immunogenicity Results from Phase 2 & Phase 1 were Consistent:
Live Virus Neutralization Versus Convalescent Sera
Phase 1 (n=20 in 100μg dose group) and Phase 2 (n=322) sera (taken 28 days after the second dose) titer neutralizing activity, versus
a panel of human convalescent serum titers taken from patients hospitalized with COVID-19, as measured by a live virus neutralization
test, VNT50, shows that two doses of UB-612 may yield neutralizing antibodies comparable to those found in convalescent patients.
Immunization with UB-612 in both Phase 2 and Phase 1 studies led to detectable T-cell responses observed in a subset of subjects. In
Phase 2, a total of 88 subjects receiving UB-612 and 12 receiving placebo were tested for T cell responses at baseline and on Day 57.
Preliminary results of ELISpot (Interferon-γ and IL-4) and intracellular cytokine staining indicate robust responses to UB-612, with a
strong Th1 orientation. Intracellular cytokine staining (ICS) confirmed the Th1 orientation of T cell responses. UB-612 induced
measurable CD8+ T cell responses and CD107a+/Granzyme secreting cells, which are putative cytotoxic T cells.
UB-612 stimulates T-cell responses with predominately Th1 polarity

34
Top panel: ELISPOT analysis of PBMCs collected on day 57 Phase 2 study. Bottom panels (A, B and C): ICS analysis of PBMCs
collected on day 57 Phase 2 study. Placebo (n=14) subjects without IgG ELISA, ACE2 and neutralizing antibody responses. UB-
612 n=86 subjects. Statistical analysis was performed using Mann-Whitney t test. (* p<0.05; ** p<0.01; ***p<0.001; ****
p<0.0001).
2-Dose Data: Phase 1 Trial
In early 2021, we completed an open-label dose escalation Phase 1 clinical trial to evaluate the safety, tolerability and immunogenicity
of UB-612 in healthy volunteers between the ages of 20 and 55 in Taiwan. This six-month trial consisted of three cohorts of 20 subjects
each. The first cohort received two intramuscular injections of 10μg doses of UB-612, the second cohort received two 30μg doses and
the third cohort received two 100μg doses. The first dose in each cohort was administered at the start of the trial, with the second dose
administered on day 28. The mean titer of antigen-specific antibodies to UB-612 and the seroconversion rate was be evaluated
throughout the six-month duration of the study to determine the humoral immune response and persistence of immunogenicity. In
addition, T-cell responses were evaluated by interferon-γ ELISpot assay and intracellular cytokine staining by flow cytometry.
The Phase 1 clinical trial was sponsored by UBIA. UBIA conducted the trial on our behalf in accordance with one of our related party
master services agreements.
After one and two doses, UB-612 was considered to be generally safe and well tolerated, with a low frequency of solicited and unsolicited
AEs, which were all Grade 1 (mild) in severity. After each vaccination, the most common AE was injection site pain, with no clear
difference in reactogenicity between dose levels. In all dose groups, there was a trend towards increased reactogenicity with increase in
dose. Three cases of mild allergic reactions were reported (e.g., itching at vaccine site), which were all resolved within 1-3 days.
Importantly, and in distinction to certain vaccines authorized for emergency use, no other increase in AEs was seen at second dose as
compared to first injection. We selected the highest dose (100μg) to take into the Phase 2 trial.
In an anti-S1-RBD ELISA assay, we observed that all three dose levels of UB-612 induced titer levels comparable to or greater than
those in sera from patients hospitalized with COVID-19. Furthermore, in a cytopathic effect viral neutralization assay (CPE VNT50),
we observed neutralizing titers comparable to those in sera from patients hospitalized with COVID-19.

35
Since September 2020, a number of genotypic variants of SARS-CoV-2 have emerged and contributed to epidemic spread in multiple
countries. Notable among these are the Alpha or B.1.1.7 (United Kingdom), Beta or B.1.351 (South Africa), Gamma or P.1 (Brazil) and
the Delta or B.1.617.2 variant (India) and Omicron (B.1.1.529). Some SARS-CoV-2 variants containing mutations in the S protein,
especially the N-terminal domain and the RBD, show reduced neutralization by antibody against the Wuhan strain, evidenced both in
persons naturally infected and in vaccinated individuals. The Beta (South Africa) and Omicron variants show the highest level of
resistance, with 13-fold to over 30-fold reduction in neutralization, respectively, and vaccines have shown reduced protection against
these variants.
Neutralizing activities of sample sera from the Phase 1 trial were assessed against live virus variants at the Viral and Rickettsial Disease
Laboratory of the California State Department of Public Health. The results indicate that UB-612 induces viral neutralizing antibody
titers against the Alpha, Gamma and Delta variants of SARS-CoV-2, close to the neutralizing titer level against the original (wild-type,
WT) Wuhan strain, while the titer level against the Beta variant is lower in comparison. The latter finding is anticipated by results
published for other COVID-19 vaccines, as pointed out above. These data align with observations taken from a cynomolgus macaque
study of UB-612 as well.
We measured viral-neutralizing antibody titers up to 154 days after the second dose (day 196) in the Phase 1 trial of UB-612; the level
of VNT50 antibodies remained at 52% of the maximum level observed following the second dose, on average. Based on the interim six-
month cutoff, the UB-612-specific neutralizing antibody half-life was estimated to be 195 days using an exponential model.
Time Course of SARS-CoV-2 Antibody Neutralization Responses after Vaccination
Data from a micro-neutralization assay of sera from subjects who received two 100μg doses of UB-612 yielded an estimated neutralizing
titer half-life of 195 days (CI: 136, 349) using an exponential model.
Pre-Clinical Study Results for UB-612
Initial work to select the S1-RBD-sFc antigen was performed in guinea pig immunogenicity studies, which demonstrated the superiority
of S1-RBD-sFc over other protein designs tested. Product candidate dose and formulation were explored in rat immunogenicity studies,
which allowed the selection of the current formulation of UB-612. Efficacy studies were carried out in mouse and nonhuman primate
models, in which UB-612 showed protective efficacy against live viral challenge. In a nonhuman primate model challenge study, we
observed full protection against SARS-CoV-2.
A GLP toxicology study in rats demonstrated an acceptable safety profile and enabled clinical testing of UB-612. In addition to these
studies, a Developmental and Reproductive Toxicity study yielded no significant findings.
Development Strategy
Based on UB-612 three-dose titer data from the Phase 1 extension, and our belief in UB-612’s potential utility as a heterologous booster
dose (boosting the immunity of a subject who has already received a different vaccine), we are pursuing accelerated pathways to
authorization with regulators in multiple jurisdictions,
including high income countries and LMICs based on a heterologous booster trial
of UB-612 beginning in the first half of 2022, with the first dose administered in the U.S. in the first quarter of 2022 under
FDA IND
clearance.
36
COVID-19 Diagnostics Program
We have developed an ELISA test that can quickly detect antibodies in human sera or plasma to determine if a patient has had a SARS-
CoV-2 infection post fourteen days of onset. It employs synthetic peptides derived from the M, S and N proteins of SARS-CoV2 for the
detection of IgG antibodies to SARS-CoV2 in human sera or plasma. These synthetic peptides bind antibodies specific to highly
antigenic segments of SARS- CoV2 structural M, N and S proteins and constitute the solid phase antigenic immunosorbant. The FDA
issued an EUA for our ELISA test in January 2021. We are not actively pursuing commercialization of our ELISA tests at this time.
Competition
The pharmaceutical industry is characterized by rapidly advancing technologies, intense competition and a strong emphasis on
proprietary products. While we believe that our technology, the expertise of our executive and scientific teams, research, clinical
capabilities, development experience and scientific knowledge provide us with competitive advantages, we face increasing competition
from multiple sources, including pharmaceutical and biotechnology companies, academic institutions, governmental agencies and public
and private research institutions.
Vaccines
The global vaccine market is highly concentrated among a small number of multinational pharmaceutical companies: Pfizer, Merck,
GlaxoSmithKline and Sanofi together control most of the global vaccine market. Other pharmaceutical and biotechnology companies,
academic institutions, governmental agencies and public and private research institutions are also working toward new solutions given
the continuing global unmet need.
More than twenty COVID-19 vaccines are currently authorized for use in one or more countries around the world, including three in the
United States. All have been shown to be safe and effective in placebo-controlled clinical trials. All these vaccines are based on the S
protein of the SARS-CoV-2 virus, but rely on different mechanisms for presentation or expression of the S antigen, including whole,
inactivated virus, defective adenovirus vectors (three different types) or mRNA.
Neurodegenerative Disorders
We expect that, if approved, our product candidates will compete with the currently approved therapies for management of
neurodegenerative diseases, such as AD and PD. In AD, four drugs are currently approved by the FDA for the treatment of symptoms
of AD, based on acetylcholinesterase (“AChE”) inhibition and NMDA receptor antagonism. In addition to the marketed therapies, we
are aware of several companies currently developing therapies for AD, including Eisai, Eli Lilly, Hoffman-LaRoche, Otsuka
Pharmaceuticals, Novartis and Biohaven Pharmaceuticals. Biogen’s aducanumab was approved by the FDA in June 2021 under the
accelerated approval pathway, which allows for earlier approval of drugs that treat serious conditions, and that fill an unmet medical
need based on a surrogate endpoint. Regulatory approval of aducanumab is pending in Europe and Japan.
Pharmaceutical treatments for PD address its symptoms only and do not treat the underlying causes of PD. The majority of prescription
drugs are dopaminergic medications and act by increasing dopamine, a neurotransmitter. We are aware of several companies with
product candidates at various stages of clinical development, including Sanofi, Kyowa Kirin, Cerevel Therapeutics and Hoffman
LaRoche. Hoffman LaRoche is developing prasinezumab, a mAb, as a potential treatment for PD.
CGRP-Directed Migraine Treatments
Six migraine treatments have been approved by the FDA that target CGRP. Four of these therapeutics are mAbs and were approved to
prevent or reduce the number of migraine episodes. These medications are galcanezumab (Emgality), which was developed by Lilly;
erenumabb (Aimovig), which was developed by Amgen in collaboration with Novartis; fremanezumab (Ajovy), which was developed
by Teva; and eptinezumab (Vyepti), which was developed by Alder, acquired by Lundbeck. Ubrogepant (Ubvelvy), developed by
Allergan, was approved for the treatment of acute migraine episodes; rimegepant (Nurtec), also approved for the treatment of acute
migraine, is sold by Biohaven.
PCSK-9 Inhibitors
Two companies currently have PCSK-9 inhibitors approved by the FDA to treat hypercholesterolemia. Both are mAbs. Regeneron
Pharmaceuticals developed alirocumab (Praluent), in collaboration with Sanofi, and Amgen developed evolocumab (Repatha). The
Medicines Company, a subsidiary of Novartis, is developing inclisiran, an RNAi construct, to down-regulate synthesis of PCSK-9.
Inclisiran was approved by the EMA in December 2020.
37
Collaborations
From time to time, we may enter into licensing and commercialization agreements when they align with our mission, including the
Platform License Agreement described under “—Intellectual Property—Platform License Agreement” and the agreement with our
partner Aurobindo.
Aurobindo License Agreement
In December 2020, we entered into an exclusive license agreement with Aurobindo (as amended, the “Aurobindo Agreement”) to
develop and commercialize UB-612 to India and other territories. Pursuant to the Aurobindo Agreement, we granted Aurobindo an
exclusive license (with certain rights reserved to us) to develop, manufacture and commercialize UB-612 in India and other countries
through UNICEF and a non-exclusive license to develop, manufacture and commercialize UB-612 in other selected emerging and
developing markets.
The Aurobindo Agreement may be terminated (i) by Aurobindo, without cause at any time after three years following the effective date
or prior to such time if UB-612 fails to meet clinical end-points or fails in development, (ii) by us, (a) if Aurobindo disputes the
patentability, enforceability or validity of our patent rights related to the UB-612 technology, (b) in case of a suit alleging Aurobindo’s
use of the licensed intellectual property infringes a third party’s intellectual property rights if we reasonably believe the license is no
longer commercially reasonable in light of such claim or (c) without cause at any time after four years following the effective date, (iii)
by either party in the event of the other party’s material breach of its obligations under the Aurobindo Agreement (subject to a cure
period) or (iv) by either party in the event of the other party’s insolvency.
Manufacturing
The manufacture of our product candidates encompasses both the manufacture of custom components and the formulation, fill and finish
of the final product. We do not currently own or operate manufacturing facilities for these processes. We currently rely upon contract
manufacturing organizations, including those mentioned below, to produce our product candidates for both pre-clinical and clinical use
and will continue to rely upon these relationships for commercial manufacturing if any of our product candidates obtain regulatory
approval. Although we rely upon contract manufacturers, we also have personnel with extensive manufacturing experience that can
oversee the relationships with our manufacturing partners.
Historically, we have depended heavily on UBI and its affiliates for our business operations, including the provision of research,
development and manufacturing services. Currently, UBIA provides testing services for UB-312 and UB-612, UBI Pharma Inc.
(“UBIP”) provides testing relating to formulation-fill-finish services for UB-312, and United BioPharma, Inc. (“UBP”) is the sole
manufacturer of protein for UB-612. Our commercial arrangements with UBI and its affiliates are described in more detail below.
Formulation-fill-finish services for UB-612 are provided by multiple contract manufacturers to ensure adequate capacity and minimize
supply chain risks. For supply of our other custom components, in addition to protein manufacturing conducted by UBP, we have
engaged third party CMOs, including C S Bio Co. (“CSBio”) as our primary peptide supplier for UB-612 peptides and Wuxi STA for
process development and manufacturing services of oligonucleotides.
UBI Group Manufacturing Partnership
We primarily rely on our relationships with third-party contract manufacturing organizations to produce product candidates for our
clinical trials. Historically, we have heavily depended on UBI as a manufacturing partner for these efforts. In support of our COVID-19
program (UB-612), we have entered into a master services agreement with UBP and an additional master services agreement with UBI,
UBIA and UBP. Pursuant to these agreements, UBI and its affiliates have provided research, development, testing and manufacturing
services to us and continue to provide manufacturing services for our protein. Payment terms are mutually agreed in connection with
each work order relating to services rendered. Our agreement with UBP will expire on the later of March 2024 and the completion of
all services under the last work order executed prior to such scheduled expiration and our agreement with UBI, UBIA and UBP will
expire on the later of September 2023 and the completion of all services under the last work order executed prior to such scheduled
expiration. We also have a management services agreement with UBI pursuant to which UBI has provided research and prior back office
administrative services to us and acts as our agent with respect to certain matters relating our COVID-19 program. UBI is compensated
for its services on a cost-plus basis. The agreement terminates upon mutual agreement between the parties.
In support of our chronic disease pipeline, we have entered into master service agreements with each of UBI, UBIA and UBIP. Pursuant
to these agreements, UBI currently provides limited research services to us on a cost-plus basis, UBIA provides testing services related
to UB-312 clinical trial material already manufactured and UBIP has provided manufacturing, quality control, testing, validation, GMP
warehousing and supply services to us for UB-312 on payment terms agreed in connection with work orders relating to the services
rendered. UBI and its affiliates no longer provide clinical or manufacturing services for other programs. These agreements may all be
terminated for convenience upon 180 days’ notice or less.
38
We have also entered into a research and development services agreement with UBI. Pursuant to this agreement, UBI and its affiliates
provide research and development services to us. Service fees payable by us to UBI for research and development projects undertaken
in accordance with the research and development plan will be determined by a joint steering committee and set forth in a research and
development plan. The aggregate services fees payable by us under the research and development services agreement are subject to a
quarterly cap throughout the term of the agreement. The research and development services agreement expires in August 2026.
Intellectual Property
Our ability to obtain and maintain intellectual property protection for our product candidates and core technologies is fundamental to
the long-term success of our business. We rely on a combination of intellectual property protection strategies, including patents,
trademarks, trade secrets, license agreements, confidentiality policies and procedures, nondisclosure agreements, invention assignment
agreements and technical measures designed to protect the intellectual property and commercially valuable confidential information and
data used in our business.
In summary, our patent estate includes issued patents and patent applications which claims cover our Vaxxine Platform and each of our
product candidates. As of December 31, 2021, our patent estate included ten U.S. issued patents, twelve U.S. patent applications, three
U.S. provisional patent applications, four pending Patent Cooperation Treaty (“PCT”) patent applications, 98 issued non-U.S. patents
and 194 pending non-U.S. patent applications.
For our product candidates targeting the prevention and treatment of neurodegenerative disease, including claims covering UB-311,
UB-312, patent rights are provided by patents and patent applications, the majority of which are being prosecuted in the United States,
Australia, Brazil, Canada, China, the EPO, Hong Kong, Indonesia, India, Israel, Japan, the Republic of Korea, Mexico, Russia,
Singapore, South Africa, Taiwan and the United Arab Emirates directed to peptide vaccines for the prevention and treatment of
neurodegenerative diseases. These issued patents and patent applications, if issued, are expected to expire between 2022 and 2039,
excluding any patent term adjustments or patent term extensions.
For our product candidates directed to peptide immunogens targeting CGRP and formulations thereof for the prevention and treatment
of migraine, including UB-313, patent rights may be provided by a patent family being prosecuted in the United States, Australia, Brazil,
Canada, China, India, Indonesia, Japan, Mexico, Russia, the Republic of Korea, Singapore, Taiwan and the United Arab Emirates. These
patent applications, if issued, are expected to expire in 2039, excluding any patent term adjustments or patent term extensions.
For our product candidates targeting cholesterol and cardiovascular disease, including our anti-PCSK9 product candidate targeting
PCSK9 and formulations thereof for prevention and treatment of PCSK9-mediated disorders, we are in the process of acquiring a
pending patent application in Taiwan and a pending PCT patent application. This Taiwanese patent application, if issued, and any U.S.
or non-U.S. patent issuing from this PCT patent application, if such patent is issued, is expected to expire in 2041, excluding any patent
term adjustment or patent term extension.
For our product candidates targeting SARS-CoV-2, including UB-612 for COVID-19, we have pending patent applications in Brazil,
Pakistan and Taiwan, one pending PCT patent application and three provisional patent applications in the United States. These patent
applications, if issued, and any U.S. or non-U.S. patent issuing from this PCT or provisional patent application, are expected to expire
between 2041 and 2042, excluding any patent term adjustments or patent term extensions.
For each product candidate utilizing the Vaxxine platform, additional patent rights directed to artificial T helper cell epitopes and to a
CpG delivery system are provided by patents and patent applications, the majority of which are being prosecuted in the United States,
Australia, Austria, Belgium, Brazil, Canada, Chile, China, Colombia, Denmark, the EPO, France, Germany, Hong Kong, Indonesia,
India, Ireland, Israel, Italy, Japan, Mexico, the Netherlands, New Zealand, Peru, Philippines, the Republic of Korea, Russia, Singapore,
South Africa, Spain, Sweden, Switzerland/Liechtenstein, Taiwan, Thailand, the United Arab Emirates, the United Kingdom and
Vietnam. These issued patents and patent applications, if issued, are expected to expire between 2023 and 2039, excluding any patent
term adjustments or patent term extensions.
The term of individual patents depends on the countries in which they are obtained. The patent term is 20 years from the earliest effective
filing date of a non-provisional patent application in most of the countries in which we file, including the United States. In the United
States, a patent’s term may be lengthened by patent term adjustment, which compensates a patentee for administrative delays by the
USPTO in examining and granting a patent, or may be shortened if a patent is terminally disclaimed over an earlier filed patent. The
term of a patent that covers a drug or biological product may also be eligible for patent term extension when FDA approval is granted
for a portion of the term effectively lost as a result of the FDA regulatory review period, subject to certain limitations and provided
statutory and regulatory requirements are met.
In addition to our reliance on patent protection for our inventions, products and technologies, we also seek to protect our brand through
the procurement of trademark rights. We own registered trademarks and pending trademark applications for our brands, including our
“Vaxxinity”, “United Neuroscience” and “COVAXX” brands and other related names and logos, in the United States and certain foreign
jurisdictions.
39
Furthermore, we rely upon trade secrets and know-how and continuing technological innovation to develop and maintain our competitive
position. However, trade secrets and know-how can be difficult to protect. We generally control access to and use of our trade secrets
and know-how, through the use of internal and external controls, including by entering into nondisclosure and confidentiality agreements
with our employees and third parties. We cannot guarantee, however, that we have executed such agreements with all applicable
counterparties, that such agreements will not be breached or that these agreements will afford us adequate protection of our intellectual
property and proprietary rights. Furthermore, although we take steps to protect our proprietary information and trade secrets, third parties
may independently develop substantially equivalent proprietary information and techniques or otherwise gain access to our trade secrets
or disclose our technology. As a result, we may not be able to meaningfully protect our trade secrets. For further discussion of the risks
relating to intellectual property, see “Risk Factors—Risks Related to Our Intellectual Property Rights.”
Platform License Agreement
In August 2021, Vaxxinity entered into a license agreement (the “Platform License Agreement”) with UBI and certain of its affiliates
(collectively, the “Licensors”) that expanded intellectual property rights previously licensed under the Original UBI Licenses (as defined
below). Pursuant to the Platform License Agreement, Vaxxinity obtained a worldwide, sublicensable (subject to certain conditions),
perpetual, fully paid-up, royalty-free (i) exclusive license (even as to the Licensors) under all patents owned or otherwise controlled by
the Licensors or their affiliates existing as of the effective date of the Platform License Agreement, (ii) exclusive license (except as to
the Licensors) under all patents owned or otherwise controlled by the Licensors or their affiliates arising after the effective date during
the term of the Platform License Agreement, and (iii) non-exclusive license under all know-how owned or otherwise controlled by the
Licensors or their affiliates existing as of the effective date or arising during the term of the Platform License Agreement, in each of the
foregoing cases, to research, develop, make, have made, utilize, import, export, market, distribute, offer for sale, sell, have sold,
commercialize or otherwise exploit peptide-based vaccines in the field of all human prophylactic and therapeutic uses, except for such
vaccines related to human immunodeficiency virus (HIV), herpes simplex virus (HSE) and Immunoglobulin E (IgE). The patents and
patent applications licensed under the Platform License Agreement inclusde claims directed to a CpG delivery system, artificial T helper
cell epitopes and certain designer peptides and proteins utilized in UB-612. As partial consideration for the rights and licenses we
received pursuant to the Platform License Agreement, we granted UBI a warrant to purchase 1,928,020 shares of our Class A common
stock (“UBI Warrant”). The UBI Warrant is exercisable at an exercise price of $12.45 per share (subject to adjustment pursuant thereto),
is not subject to vesting, and has a term of five years.
Vaxxinity has the first right to control the filing, prosecution, maintenance and enforcement of the licensed patents at Vaxxinity’s own
expense, subject to the Licensors’ right to comment on and review any patent filings. The Platform License Agreement shall continue
until the parties mutually consent in writing to terminate the agreement. Upon such termination, all licenses granted under the Platform
License Agreement shall terminate and Vaxxinity will assign any regulatory documentation previously assigned to Vaxxinity back to
the Licensors.
Coverage and Reimbursement
Sales of our product candidates in the United States will depend, in part, on the extent to which third- party payors, including government
health programs such as Medicare and Medicaid, commercial insurance and managed health care organizations provide coverage and
establish adequate reimbursement levels for such product candidates. The process for determining whether a third-party payor will
provide coverage for a pharmaceutical or biological product is typically separate from the process for setting the price of such a product
or for establishing the reimbursement rate that the payor will pay for the product once coverage is approved, and we may also need to
provide discounts to purchasers, private health plans or government healthcare programs, as increasingly, third-party payors are
requiring that drug companies provide them with predetermined discounts from list prices and are challenging the prices charged for
medical products. As a result, a third-party payor’s decision to provide coverage for a pharmaceutical or biological product does not
imply that the reimbursement rate will be adequate for commercial viability, and inadequate reimbursement rates, including significant
patient cost sharing obligations, may deter patients from selecting our product candidates. Obtaining coverage and reimbursement
approval of a product from a third-party payor is a time-consuming and costly process that could require us to provide to each payor
supporting scientific, clinical and cost-effectiveness data for the use of our product on a payor-by-payor basis, with no assurance that
coverage and adequate reimbursement will be obtained. Third-party payors may limit coverage to specific products on an approved list,
also known as a formulary, which might not include all of the approved products for a particular indication.
Further, no uniform policy for coverage and reimbursement exists in the United States, and coverage and reimbursement can differ
significantly from payor to payor. In general, factors a payor considers in determining coverage and reimbursement are based on whether
the product is a covered benefit under its health plan; safe, effective, and medically necessary, including its regulatory approval status;
medically appropriate for the specific patient; cost-effective; and neither experimental nor investigational. Third-party payors often rely
upon Medicare coverage policy and payment limitations in setting their own reimbursement rates, but also have their own methods and
approval process apart from Medicare determinations. As such, one third-party payor’s decision to cover a particular medical product
or service does not ensure that other payors will also provide coverage for the medical product or service, and the level of coverage and
reimbursement can differ significantly from payor to payor. Even if favorable coverage and reimbursement status is attained for one or
40
more products for which we receive regulatory approval, less favorable coverage policies and reimbursement rates may be implemented
in the future.
Product Approval and Government Regulation
Government authorities in the United States, at the federal, state and local level, and other countries extensively regulate, among other
things, the research, development, testing, manufacture, quality control, approval, labeling, packaging, storage, record-keeping,
promotion, advertising, distribution, post-approval monitoring and reporting, marketing and export and import of products such as those
we are developing. Any product candidate that we develop must be approved by the FDA before it may be legally marketed in the
United States and by the appropriate foreign regulatory agency before it may be legally marketed in foreign countries.
U.S. Drug Development Process
In the United States, the development, manufacturing and marketing of human drugs and vaccines are subject to extensive regulation.
The FDA regulates drugs under the Federal Food, Drug and Cosmetic Act (“FDCA”) and implementing regulations, and biological
products, including vaccines, under provisions of the FDCA and the Public Health Service Act. Drugs and vaccines are also subject to
other federal, state and local statutes and regulations. The process of obtaining regulatory approvals and the subsequent compliance with
appropriate federal, state, local and foreign statutes and regulations require the expenditure of substantial time and financial resources.
Failure to comply with the applicable U.S. requirements at any time during the product development process, approval process or after
approval, may subject an applicant to administrative or judicial sanctions. FDA sanctions could include refusal to approve pending
applications, withdrawal of an approval, clinical hold, warning letters, product recalls, product seizures, total or partial suspension of
production or distribution, injunctions, fines, refusals of government contracts, debarment, restitution, disgorgement or civil or criminal
penalties. Any agency or judicial enforcement action could have a material adverse effect on us. The process required by the FDA before
a drug or biological product may be marketed in the United States generally involves the following:
• completion of nonclinical laboratory tests, animal studies and formulation and stability studies according to GLP or other
applicable regulations;
• submission to the FDA of an application for an IND, which must become effective before human clinical trials may begin;
• performance of adequate and well-controlled human clinical trials according to the FDA’s regulations commonly referred to
as GCPs to establish the safety and efficacy of the proposed drug for its intended use;
• submission to the FDA of an NDA or BLA for a new drug;
• satisfactory completion of an FDA inspection of the manufacturing facility or facilities where the drug is produced to assess
compliance with the FDA’s cGMP, to assure that the facilities, methods and controls are adequate to preserve the drug’s
identity, strength, quality and purity;
• potential FDA audit of the nonclinical and clinical trial sites that generated the data in support of the NDA or BLA; and
• FDA review and approval of the NDA or BLA.
The lengthy process of seeking required approvals and the continuing need for compliance with applicable statutes and regulations
require the expenditure of substantial resources and approvals are inherently uncertain.
Before testing any compounds with potential therapeutic value in humans, the product candidate enters the pre-clinical study stage. Pre-
clinical tests, also referred to as nonclinical studies, include laboratory evaluations of product chemistry, toxicity and formulation, as
well as animal studies to assess the potential safety and activity of the product candidate. The conduct of the pre-clinical tests must
comply with federal regulations and requirements including GLP. The sponsor must submit the results of the pre-clinical tests, together
with manufacturing information, analytical data, any available clinical data or literature and a proposed clinical protocol, to the FDA as
part of the IND. The IND automatically becomes effective 30 days after receipt by the FDA, unless the FDA imposes a clinical hold
within that 30-day time period. In such a case, the IND sponsor and the FDA must resolve any outstanding concerns before the clinical
trial can begin. The FDA may also impose clinical holds on a product candidate at any time before or during clinical trials due to safety
concerns or non-compliance. Accordingly, we cannot be sure that submission of an IND will result in the FDA allowing clinical trials
to begin, or that, once begun, issues will not arise that suspend or terminate such trial.
Clinical trials involve the administration of the product candidate to healthy volunteers or patients under the supervision of qualified
investigators, generally physicians not employed by or under the trial sponsor’s direct control. Clinical trials are conducted under
protocols detailing, among other things, the objectives of the clinical trial, dosing procedures, subject selection and exclusion criteria,
and the parameters to be used to monitor subject safety. Each protocol must be submitted to the FDA as part of the IND. Clinical trials
must be conducted in accordance with the FDA’s regulations comprising the good clinical practices requirements. Further, each clinical
41
trial must be reviewed and approved by an independent IRB at or servicing each institution at which the clinical trial will be conducted.
An IRB is charged with protecting the welfare and rights of trial participants and considers such items as whether the risks to individuals
participating in the clinical trials are minimized and are reasonable in relation to anticipated benefits. The IRB also approves the form
and content of the informed consent that must be signed by each clinical trial subject or his or her legal representative and provide
oversight for the clinical trial until completed.
Human clinical trials are typically conducted in three sequential phases that may overlap or be combined:
•
Phase 1
. The drug is initially introduced into healthy human subjects and tested for safety, dosage
tolerance, absorption, metabolism, distribution and excretion. In the case of some products for severe or life-threatening diseases,
especially when the product may be too inherently toxic to ethically administer to healthy volunteers, the initial human testing may be
conducted in patients;
•
Phase 2
.
The
risks, to preliminarily evaluate the efficacy of the product for specific targeted diseases and to determine dosage tolerance, optimal
dosage and dosing schedule; and
•
Phase 3
. Clinical trials are undertaken to further evaluate dosage, clinical efficacy and safety in an
expanded patient population at geographically dispersed clinical trial sites. These clinical trials are intended to establish the overall
risk/benefit ratio of the product and provide an adequate basis for product labeling. Generally, a well-controlled Phase 3 clinical trial is
required by the FDA for approval of an NDA or BLA.
Post-approval clinical trials, sometimes referred to as Phase 4 clinical trials, may be conducted after initial marketing approval. These
clinical trials are used to gain additional experience from the treatment of patients in the intended therapeutic indication.
During all phases of clinical development, regulatory agencies require extensive monitoring and auditing of all clinical activities, clinical
data and clinical trial investigators. Annual progress reports detailing the results of the clinical trials must be submitted to the FDA and
written IND safety reports must be promptly submitted to the FDA and the investigators for serious and unexpected adverse events or
any finding from tests in laboratory animals that suggests a significant risk for human subjects. Phase 1, Phase 2 and Phase 3 clinical
trials may not be completed successfully within any specified period, if at all. The FDA or the sponsor or its data safety monitoring
board may suspend a clinical trial at any time on various grounds, including a finding that the research subjects or patients are being
exposed to an unacceptable health risk. Similarly, an IRB can suspend or terminate approval of a clinical trial at its institution if the
clinical trial is not being conducted in accordance with the IRB’s requirements or if the drug has been associated with unexpected serious
harm to patients.
Concurrently with clinical trials, companies usually complete additional animal studies and must also develop additional information
about the chemistry and physical characteristics of the drug as well as finalize a process for manufacturing the product in commercial
quantities in accordance with cGMP requirements. The manufacturing process must be capable of consistently producing quality batches
of the product candidate and, among other things, must develop methods for testing the identity, strength, quality and purity of the final
drug. Additionally, appropriate packaging must be selected and tested, and stability studies must be conducted to demonstrate that the
product candidate does not undergo unacceptable deterioration over its shelf life.
U.S. Review and Approval Processes
Assuming successful completion of all required testing in accordance with all applicable regulatory requirements, the results of product
development, nonclinical studies and clinical trials, along with descriptions of the manufacturing process, analytical tests conducted on
the chemistry of the drug, proposed labeling and other relevant information are submitted to the FDA as part of an NDA or BLA
requesting approval to market the product. The submission of an NDA or BLA is subject to the payment of substantial fees; a waiver of
such fees may be obtained under certain limited circumstances.
In addition, under the Pediatric Research Equity Act (“PREA”), an NDA or BLA or supplement to an NDA or BLA must contain data
to assess the safety and effectiveness of the drug for the claimed indications in all relevant pediatric subpopulations and to support
dosing and administration for each pediatric subpopulation for which the product is safe and effective. The FDA may grant deferrals for
submission of data or full or partial waivers. Unless otherwise required by regulation, PREA does not apply to any drug for an indication
for which orphan designation has been granted.
The FDA reviews all NDAs or BLAs submitted to determine if they are substantially complete before it accepts them for filing. If the
FDA determines that an NDA or BLA is incomplete or is found to be non-navigable, the filing may be refused and must be re-submitted
for consideration. Once the submission is accepted for filing, the FDA begins an in-depth review of the NDA or BLA. Under the goals
and policies agreed to by the FDA under the Prescription Drug User Fee Act (“PDUFA”), the FDA has 10 months from acceptance of
filing in which to complete its initial review of a standard NDA or BLA and respond to the applicant, and six months from acceptance
of filing for a priority NDA or BLA. The FDA does not always meet its PDUFA goal dates. The review process and the PDUFA goal
42
date may be extended by three months or longer if the FDA requests or the NDA or BLA sponsor otherwise provides additional
information or clarification regarding information already provided in the submission before the PDUFA goal date.
After the NDA or BLA submission is accepted for filing, the FDA reviews the NDA or BLA to determine, among other things, whether
the proposed product is safe and effective for its intended use, and whether the product is being manufactured in accordance with cGMP
to assure and preserve the product’s identity, strength, quality and purity. The FDA may refer applications for novel drug or biological
products or drug or biological products which present difficult questions of safety or efficacy to an advisory committee, typically a panel
that includes clinicians and other experts, for review, evaluation and a recommendation as to whether the application should be approved
and under what conditions. The FDA is not bound by the recommendations of an advisory committee, but it considers such
recommendations carefully when making decisions. During the drug approval process, the FDA also will determine whether a REMS
is necessary to assure the safe use of the drug. If the FDA concludes a REMS is needed, the sponsor of the NDA or BLA must submit a
proposed REMS; the FDA will not approve the NDA or BLA without a REMS, if required.
Before approving an NDA or BLA, the FDA will inspect the facilities at which the product is manufactured. The FDA will not approve
the product unless it determines that the manufacturing processes and facilities are in compliance with cGMP requirements and adequate
to assure consistent production of the product within required specifications. The FDA requires vaccine manufacturers to submit data
supporting the demonstration of consistency between manufacturing batches, or lots. The FDA works together with vaccine
manufacturers to develop a lot release protocol, the tests conducted on each lot of vaccine post-approval. Additionally, before approving
an NDA or BLA, the FDA will typically inspect the sponsor and one or more clinical sites to assure that the clinical trials were conducted
in compliance with IND study requirements. If the FDA determines that the application, manufacturing process or manufacturing
facilities are not acceptable it will outline the deficiencies in the submission and often will request additional testing or information.
The NDA or BLA review and approval process is lengthy and difficult and the FDA may refuse to approve an NDA or BLA if the
applicable regulatory criteria are not satisfied or may require additional clinical data or other data and information. Even if such data
and information is submitted, the FDA may ultimately decide that the NDA or BLA does not satisfy the criteria for approval. Data
obtained from clinical trials are not always conclusive and the FDA may interpret data differently than we interpret the same data. The
FDA will issue a complete response letter if the agency decides not to approve the NDA or BLA. The complete response letter usually
describes all of the specific deficiencies in the NDA or BLA identified by the FDA. The deficiencies identified may be minor, for
example, requiring labeling changes, or major, for example, requiring additional clinical trials. Additionally, the complete response
letter may include recommended actions that the applicant might take to place the application in a condition for approval. If a complete
response letter is issued, the applicant may either submit new information, addressing all of the deficiencies identified in the letter, or
withdraw the application.
If a product receives regulatory approval, the approval may be significantly limited to specific diseases and dosages or the indications
for use may otherwise be limited, which could restrict the commercial value of the product. Further, the FDA may require that certain
contraindications, warnings or precautions be included in the product labeling. In addition, the FDA may require post-marketing clinical
trials, sometimes referred to as Phase 4 clinical trials, which are designed to further assess a product’s safety and effectiveness and may
require testing and surveillance programs to monitor the safety of approved products that have been commercialized. In addition, new
government requirements, including those resulting from new legislation, may be established, or the FDA’s policies may change, which
could impact the timeline for regulatory approval or otherwise impact ongoing development programs.
Expedited Development and Review Programs
The FDA has a fast track program that is intended to expedite or facilitate the process for reviewing new drugs and biologics that meet
certain criteria. Specifically, new drugs and biologics are eligible for fast track designation if they are intended to treat a serious or life-
threatening condition and preclinical or clinical data demonstrate the potential to address unmet medical needs for the condition. Fast
track designation applies to the combination of the product and the specific indication for which it is being studied. The sponsor can
request the FDA to designate the product for fast track status any time before receiving NDA or BLA approval, but ideally no later than
the pre-NDA or pre-BLA meeting.
Additionally, a drug or biologic may be eligible for designation as a breakthrough therapy if the product is intended, alone or in
combination with one or more other drugs or biologics, to treat a serious or life-threatening condition and preliminary clinical evidence
indicates that the product may demonstrate substantial improvement over currently approved therapies on one or more clinically
significant endpoints. The benefits of breakthrough therapy designation include the same benefits as fast track designation, plus intensive
guidance from the FDA to facilitate an efficient drug development program.
Any product submitted to the FDA for marketing, including under a fast track or breakthrough therapy designation program, may be
eligible for other types of FDA programs intended to expedite development and review, such as priority review and accelerated approval.
Any product is eligible for priority review if it treats a serious or life-threatening condition and, if approved, would provide a significant
improvement in safety and effectiveness compared to available therapies. Priority review reduces the review time for an initial or
supplemental marketing application by four months.
43
A product may be eligible for accelerated approval if it treats a serious or life-threatening condition and generally provides a meaningful
advantage over available therapies based on an effect on a surrogate endpoint that is reasonably likely to predict clinical benefit or on a
clinical endpoint that can be measured earlier than irreversible morbidity or mortality ("IMM") that is reasonably likely to predict an
effect on IMM or other clinical benefit. As a condition of accelerated approval, the FDA requires that a sponsor of a drug or biologic
receiving accelerated approval subsequently provide additional data confirming the anticipated clinical benefit, for example by
performing adequate and well-controlled post-marketing clinical trials. If clinical benefit is not confirmed, accelerated approval may be
revoked. If the FDA concludes that a drug or biologic shown to be effective can be safely used only if distribution or use is restricted, it
may require such post-marketing restrictions, as it deems necessary to assure safe use of the product.
Fast track designation, breakthrough therapy designation, priority review, and accelerated approval do not change the standards for
approval but may expedite the development or approval process.
EUA Approval
The Commissioner of the FDA, under delegated authority from the Secretary of the U.S. Department of Health and Human Services
(“DHHS”) may, under certain circumstances, issue an EUA that would permit the use of an unapproved drug product or unapproved
use of an approved drug product. Before an EUA may be issued, the Secretary must declare an emergency based on one of the following
grounds:
• a determination by the Secretary of the Department of Homeland Security that there is a domestic emergency, or a
significant potential for a domestic emergency, involving a heightened risk of attack with a specified biological, chemical,
radiological or nuclear agent or agents;
• a determination by the Secretary of the Department of Defense that there is a military emergency, or a significant potential
for a military emergency, involving a heightened risk to U.S. military forces of attack with a specified biological, chemical,
radiological or nuclear agent or agents; or
• a determination by the Secretary of the DHHS that a public health emergency that affects, or has the significant potential
to affect, national security and that involves a specified biological, chemical, radiological or nuclear agent or agents, or a
specified disease or condition that may be attributable to such agent or agent.
In order to be the subject of an EUA, the FDA Commissioner must conclude that, based on the totality of scientific evidence available,
it is reasonable to believe that the product may be effective in diagnosing, treating or preventing a disease attributable to the agents
described above, that the product’s potential benefits outweigh its potential risks and that there is no adequate approved alternative to
the product.
Although an EUA cannot be issued until after an emergency has been declared by the Secretary of DHHS, the FDA strongly encourages
an entity with a possible candidate product, particularly one at an advanced stage of development, to contact the FDA center responsible
for the candidate product before a determination of actual or potential emergency. Such an entity may submit a request for consideration
that includes data to demonstrate that, based on the totality of scientific evidence available, it is reasonable to believe that the product
may be effective in diagnosing, treating or preventing the serious or life-threatening disease or condition. This is called a pre-EUA
submission and its purpose is to allow FDA review considering that during an emergency, the time available for the submission and
review of an EUA request may be severely limited.
Post-Approval Requirements
Any drug or biological products for which we or our collaborators receive FDA approvals are subject to continuing regulation by the
FDA, including, among other things, record-keeping requirements, reporting of adverse experiences with the product, providing the
FDA with updated safety and efficacy information, product sampling and distribution requirements, complying with certain electronic
records and signature requirements and complying with FDA promotion and advertising requirements, which include, among others,
standards for direct-to-consumer advertising, promoting drugs for uses or in patient populations that are not described in the drug’s
approved labeling (known as “off-label use”), industry-sponsored scientific and educational activities, and promotional activities
involving the internet.
Failure to comply with FDA requirements can have negative consequences, including adverse publicity, enforcement letters from the
FDA, mandated corrective advertising or communications with doctors, and civil or criminal penalties. Although physicians may
prescribe legally available drugs for off-label uses, manufacturers may not market or promote such off-label uses.
Manufacturers of our product candidates are required to comply with applicable FDA manufacturing requirements contained in the
FDA’s cGMP regulations. cGMP regulations require, among other things, quality control and quality assurance as well as the
corresponding maintenance of records and documentation. Following approval, the FDA continues to monitor vaccine quality through
44
real-time monitoring of lots by requiring manufacturers to submit certain information for each vaccine lot. Vaccine manufacturers may
only distribute a lot following release by the FDA. Drug manufacturers and other entities involved in the manufacture and distribution
of approved drugs are required to register their establishments with the FDA and certain state agencies, and are subject to periodic
unannounced inspections by the FDA and certain state agencies for compliance with cGMP and other laws. Accordingly, manufacturers
must continue to expend time, money and effort in the area of production and quality control to maintain cGMP compliance. Discovery
of problems with a product after approval may result in restrictions on a product, manufacturer or holder of an approved NDA or BLA,
including withdrawal of the product from the market. In addition, changes to the manufacturing process generally require prior FDA
approval before being implemented, and other types of changes to the approved product, such as adding new indications and additional
labeling claims, are also subject to further FDA review and approval.
Taiwan Drug Development Process
The regulatory processes in Taiwan are generally similar with those in the United States, and include:
• Extensive pre-clinical laboratory tests, pre-clinical animal studies and formulation studies in accordance with applicable
regulations.
• Submission to the TFDA of an IND, which must be approved by the TFDA before human clinical trials may begin. Human
clinical trials in Taiwan typically include:
• Phase I trials. The new drug product is initially introduced into healthy human subjects and tested for safety, dosage
tolerance, absorption, metabolism and side effects associated with increasing doses. If possible, early evidence of
effectiveness of the new drug product is collected as well.
• Phase II trials. The new drug product is evaluated for its efficacy and proposed indication in a limited patient population,
as well as its adverse effects and safety risks.
• Phase III trials. The new drug product is further evaluated for dosage tolerance, efficacy and safety in an expanded patient
population.
• Submission to the TFDA of an NDA, which generally requires two Phase III trials, unless the NDA otherwise qualifies for
exemptions as provided by the TFDA.
In addition to information and data collected from the pre-clinical and clinical trials of the new drug product, chemistry data and
information regarding manufacturing and controls serve as significant considerations during the course of the TFDA review and approval
process. Where a new drug product will be manufactured in facilities located in Taiwan, the TFDA has the authority to inspect and
assess compliance with the Pharmaceutical Inspection Co-operation Scheme GMP regulations to ensure that the facilities, methods and
controls are adequate to preserve the drug’s identity, strength, quality and purity. Further, the TFDA may audit the pre-clinical and/or
clinical trial sites that generated the data in support of the NDA. Finally, the TFDA must review and approve the NDA prior to any
commercial marketing or sale of the drug in Taiwan.
Regulation in Europe and Other Regions
In addition to regulations in the United States and Taiwan, we and our collaborators are subject to a variety of regulations in other
jurisdictions governing, among other things, clinical trials and any commercial sales and distribution of our products.
Whether or not we or our collaborators obtain FDA approval for a product, we must obtain the requisite approvals from regulatory
authorities in foreign countries prior to the commencement of clinical trials or marketing of the product in those countries. Certain
countries outside of the United States have a similar process that requires the submission of a clinical trial application much like the
IND prior to the commencement of human clinical trials. In the European Union, for example, a CTA must be submitted to each
country’s national health authority and an independent ethics committee, much like the FDA and IRB, respectively. Once the CTA is
approved in accordance with a country’s requirements, clinical trial development may proceed.
The requirements and process governing the conduct of clinical trials, product licensing, pricing and reimbursement vary from country
to country. In all cases, the clinical trials are conducted in accordance with GCPs and the applicable regulatory requirements and the
ethical principles that have their origin in the Declaration of Helsinki.
To obtain regulatory approval of an investigational drug or biological product under European Union regulatory systems, we or our
strategic partners must submit a marketing authorization application. The application in the European Union is similar to that required
in the United States, with the exception of, among other things, country-specific document requirements.
45
For other countries outside of the European Union, such as countries in Asia, Europe and Latin America, the requirements governing
the conduct of clinical trials, product licensing, pricing and reimbursement vary from country to country. In all cases, again, the clinical
trials are conducted in accordance with GCPs and the applicable regulatory requirements and the ethical principles that have their origin
in the Declaration of Helsinki.
Employees and Human Capital Resources
As of December 31, 2021, we employed 89 full-time employees and no part-time employees. Of these 89 full-time employees, 69 were
located in the United States, 5 were located in Taiwan and 5 were located in Ireland. None of our employees are represented by a labor
union or are party to a collective bargaining agreement, and we have had no labor-related work stoppages.
Compensation, Benefits, Recruitment and Retention Strategy
We aim to focus on attracting, motivating and retaining talented employees with relevant experience who can contribute to the sustained
performance of the Company and its day-to-day operations.
We believe our total compensation package helps recruit and retain our employees. We strive to provide compensation and benefits that
are competitive to market and create incentives to attract and retain employees. Our compensation package includes market-competitive
pay, broad-based stock grants, health care and 401(k) plan benefits, paid time off and family leave, among others. We also provide
annual incentive bonus opportunities that are tied to both company performance as well as individual performance to foster a pay-for-
performance culture.
Scientific Advisory Board
We have assembled a highly qualified scientific advisory board composed of advisors who have deep expertise in the fields of biologics
and vaccine development, as well as in the relevant therapeutic areas for our product candidates. Our scientific advisory board is
composed of George Siber, M.D.; Donna Ambrosino, M.D.; Brad Boeve; Nick Fox, M.D.; Richard Mohs, Ph.D.; Eric Reiman, M.D.;
Jeffrey Cummings, M.D., ScD.; Barney Graham, M.D., Ph.D.; Peter A. Patriarca, M.D.; Stanley A. Plotkin, M.D.; Sharon Lewin, A.O.,
FRACP., Ph.D., FAHMS, Wayne Koff, Ph.D. and Thomas P. Monath, M.D.
46
Item 1A. Risk Factors.
Investing in our Class A common stock involves a high degree of risk. The following information sets forth risk factors that could cause
our actual results to differ materially from those contained in forward-looking statements we have made in this Annual Report on Form
10-K and those we may make from time to time. You should carefully consider the risks described below, in addition to the other
information contained in this Report and our other public filings, before you decide to purchase shares of our Class A common stock.
Our business, financial condition or results of operations could be harmed by any of these risks. The risks and uncertainties described
below are not the only ones we face. Additional risks not presently known to us or other factors not perceived by us to present significant
risks to our business at this time also may impair our business operations.
Summary Risk Factors
Our business is subject to a number of risks, including risks that may prevent us from achieving our business objectives or may adversely
affect our business, financial condition, results of operations and prospects. These risks are discussed more fully under Part II, Item 1A.
“Risk Factors.” The following is a summary of some of the principal risks we face:
• clinical drug development involves a lengthy and expensive process, and if our pre-clinical development or clinical trials
are prolonged or delayed or do not achieve expected results, we may be unable to commercialize our product candidates;
• we depend on intellectual property licensed from UBI and its affiliates, the termination of which could result in the loss of
significant rights;
• even if we obtain regulatory approval of any of our product candidates in Taiwan or other jurisdictions, we may never
obtain approval for or commercialize our product candidates in other jurisdictions;
• after receipt of regulatory approval for a product candidate, our products will remain subject to regulatory scrutiny and
post-marketing requirements, which may include burdensome post-approval study or risk management requirements;
• if we are able to commercialize any product candidate, the successful commercialization of such product candidate will
depend on the extent governmental authorities, private health insurers and other third-party payors provide coverage,
adequate reimbursement levels and favorable pricing policies;
• the manufacture of peptide-based medicines is complex and manufacturers often encounter difficulties in production;
• we have no history of commercializing pharmaceutical products, which may make it difficult to evaluate the prospects for
our future viability;
• the regulatory landscape that will govern our product candidates is uncertain, and changes in regulatory requirements could
result in delays or discontinuation of development of our product candidates or unexpected costs;
• developments by competitors may render our products or technologies obsolete or non-competitive or may reduce the size
of our markets;
• our capital resources may not be sufficient to successfully complete the development and commercialization of our product
candidates, which could delay, limit, reduce or terminate our development or commercialization efforts;
• we have incurred significant losses since inception, and we expect to incur losses for the foreseeable future and may never
achieve or maintain profitability;
• conflicts of interest and disputes exist and may further arise between us and UBI and its affiliates, and these conflicts and
disputes might ultimately be resolved in a manner unfavorable to us;
• we will need to expand our organization, and we may experience difficulties in managing this growth, which could disrupt
our operations;
• the dual-class structure of our common stock and the Voting Agreement (as defined below) will have the effect of
concentrating voting power, which will significantly limit your ability to influence significant corporate decisions;
• we rely on contract manufacturers for the manufacture of raw materials for our research programs, pre-clinical studies and
clinical trials and we do not have long-term contracts with many of these parties, which could impact our ability to
commercialize our products;
47
• undetected errors or defects in our production could harm our reputation or expose us to product liability claims;
• we rely on in-licensed intellectual property and technology, and the loss of such rights, our licensors’ inability or refusal
to enforce or defend such rights, and the requirement to pay royalties, milestones and other amounts could harm our
business;
• the degree of protection afforded by our intellectual property rights is uncertain because such rights offer only limited
protection and may not adequately protect our rights or permit us to gain or keep a competitive advantage;
• we have identified significant deficiencies and material weaknesses, and have previously identified material weaknesses,
in our internal control over financial reporting and if we are unable to remediate our existing deficiencies and material
weaknesses and otherwise develop and maintain an effective system of internal control over financial reporting, we may
not be able to accurately report our financial results or prevent fraud, and as a result, shareholders could lose confidence
in our financial and other public reporting, which would harm our business and the trading price of our Class A common
stock;
• cyberattacks or other failures in our or our third-party vendors’, contractors’ or consultants’ telecommunications or
information technology systems could result in information theft, compromise, or other unauthorized access, data
corruption and significant disruption of our business operations, and could harm our reputation and subject us to liability,
lawsuits and actions from governmental authorities; and
• we are subject to privacy, tax, anti-corruption and other stringent laws, regulations, policies and contractual obligations
across multiple jurisdictions and changes in, or our failure to comply with, such laws, regulations, policies and contractual
obligations could adversely affect our business, financial condition, results of operations and prospects.
Risks Related to the Discovery and Development of Product Candidates
Clinical drug development involves a lengthy and expensive process with uncertain timelines and uncertain outcomes, and results
of earlier studies and trials may not be predictive of future results. If our pre-clinical development or clinical trials are prolonged or
delayed, or if we do not or cannot achieve the results we expect, we may be unable to obtain required regulatory approvals, and
therefore be unable to commercialize our product candidates on a timely basis or at all.
Our business is dependent on the successful development, regulatory approval and commercialization of product candidates based on
our Vaxxine Platform. If we and our collaborators are unable to obtain approval for and effectively commercialize our product
candidates, our business would be significantly harmed. Even if we complete the necessary pre-clinical studies and clinical trials, the
regulatory approval process is expensive, time- consuming and uncertain, and we may not be able to obtain approvals for the
commercialization of any product candidates we may develop. Changes in regulatory approval policies, changes in or the enactment of
additional statutes or regulations, or changes in regulatory review processes, may cause delays in the approval of a particular product
candidate or rejection of an application for a particular product candidate. We have not obtained regulatory approval for any product
candidate to date, and it is possible that none of our existing product candidates or any product candidates we may seek to develop in
the future will ever obtain regulatory approval. Any regulatory approval we ultimately obtain may be limited or subject to restrictions,
including labeling requirements, or post-approval commitments that render the approved product not commercially viable. While our
enzyme-linked immunosorbent assay (“ELISA”) test has received an EUA from the FDA, there can be no assurance that any of our
product candidates will receive an EUA or regulatory approval or that there will not be changes in formulation, whether required by any
regulatory authority or at our determination for operational or scientific reasons, affecting the use of our products. Further, some
countries may not rely on an EUA or regulatory approval issued by another jurisdiction, and we may be required to seek separate EUAs
or regulatory approval from different regulatory authorities in different jurisdictions. See “Risk Factors—Even if we obtain approval of
any of our product candidates in one jurisdiction, we may never obtain approval for or commercialize any of our products in other
jurisdictions, which would limit our ability to realize their full market potential.”
To obtain the requisite regulatory approvals to market and sell any of our product candidates, we must demonstrate through extensive
pre-clinical studies and clinical trials that our products are safe and effective in humans. Clinical testing is expensive and can take many
years to complete, and its outcome is inherently uncertain. Failure can occur at any time during the clinical trial process. The results of
pre-clinical studies and early clinical trials of our product candidates may not be predictive of the results of later-stage clinical trials and
results from post-hoc data analysis may not be predictive of final results and may not support product approval. Product candidates in
later stages of clinical trials may fail to show the desired safety and efficacy characteristics despite having progressed through pre-
clinical studies and initial clinical trials. For example, an EUA for UB-612 was denied by the TFDA in August 2021 because the
neutralizing antibody response generated by UB-612, as compared to a designated adenovirus vectored vaccine, did not meet the TFDA’s
specified evaluation criteria, but, in collaboration with UBIA, we are appealing the decision. The outcome of that appeal remains highly
uncertain. If results from our clinical trials differ from previous reports or market expectations, such as a potential development of
market expectations that COVID-19 boosters or vaccines be developed specifically to address certain variants which we fail to satisfy,
or if we fail to obtain a required regulatory approval, the price of our Class A common stock could decrease substantially. Several
48
companies in the biopharmaceutical industry have suffered significant setbacks in advanced clinical trials due to lack of efficacy or
adverse safety profiles, notwithstanding promising results in earlier trials. Our ongoing and future clinical trials may not be successful.
Further, while we have conducted limited head-to-head comparisons in pre-clinical studies of UB-313, we have not conducted a head-
to-head comparison of any competing products to any of our product candidates in any clinical trial to date. We have compared the
published data for certain of our competitors’ products to the clinical trial results of certain of our product candidates. Accordingly, the
value of comparisons of our product candidates to any alternative products in this report may be limited because they are not derived
from a head-to-head trial, rather they are from trials that were conducted under different protocols, at different sites, with different
patient populations, at different times and results were analyzed using non-standardized assays performed internally or by different
clinical research organizations (“CROs”). Without head-to-head data, we will be unable to make comparative claims for our product
candidates, if any such product candidate is approved. Future clinical trials may not confirm the comparisons or analyses we have made
to date.
Clinical trials must be conducted in accordance with applicable regulatory authorities’ legal requirements, regulations or guidelines and
are subject to oversight by these governmental agencies as well as Institutional Review Boards (“IRBs”) at the medical institutions
where the clinical trials are conducted. In addition, clinical trials must be conducted with supplies of our product candidates produced
in accordance with current good manufacturing practices (“cGMP”) and other legal and regulatory requirements. Defects in
manufacturing of a clinical trial batch or a failure of a batch to meet all quality control test specifications could result in delays to
initiation of our clinical trials. We depend on medical institutions and CROs to conduct our clinical trials in compliance with good
clinical practice (“GCP”), and other applicable laws and regulations. Failure to follow and document adherence to such laws and
regulations may lead to significant delays in the availability of product for our clinical trials, result in the termination of or a clinical
hold being placed on one or more of our clinical trials, or delay or prevent submission or approval of marketing applications for our
product candidates.
To the extent our CROs fail to enroll participants for our clinical trials, fail to conduct the trial in accordance with the trial protocol GCP
or are delayed for a significant time in the execution of trials, including achieving full enrollment, we may be affected by increased
costs, program delays or both, which may harm our business and delay our ability to seek approval for our product candidates. For
example, due to an error by the CRO responsible for administering blinded placebo and active doses to trial subjects, which reduced the
confidence of subsequently collected data, we decided to discontinue a Phase 2a LTE trial for UB-311. In that case, however, we
determined that we had collected sufficient data on UB-311’s tolerability and immunogenicity. To date, we have not completed clinical
trials sufficient for obtaining marketing approvals for any of our product candidates. Our most advanced candidates are UB-612, which
initiated a Phase 3 pivotal study in March 2022 and has an ongoing Phase 2 clinical trial, and UB-311, which is in Phase 2 of clinical
development. Our product candidate UB-312 is in Phase 1 of clinical development and UB-313 is undergoing IND-enabling studies.
All of our other research programs are in the pre-clinical development stage.
The completion of clinical trials for our clinical product candidates may be delayed, suspended or terminated because of many factors,
including but not limited to:
• the delay or refusal of regulators or IRBs to authorize us to commence a clinical trial at a prospective trial site;
• changes in regulatory requirements, policies and guidelines;
• delays or failure to reach agreement on acceptable terms with prospective CROs and clinical trial sites, the terms of which
can be subject to extensive negotiation and may vary significantly among different CROs and trial sites;
• delays in patient enrollment and variability in the number and types of patients available for clinical trials;
• negative or inconclusive results, which may require us to conduct additional pre-clinical or clinical trials or to abandon
product candidates that we expect to be promising;
• delays in manufacturing and control of clinical trial materials;
• shortages of materials required for the production of our product candidates;
• disruptions from events surrounding the Russia-Ukraine conflict
• the timing, scope and effectiveness of U.S. and international governmental, regulatory, fiscal, monetary and public health
responses to the COVID-19 pandemic;
• safety or tolerability concerns causing us to suspend or terminate a trial if it is determined that the participants are being
exposed to unacceptable health risks;
49
• lower than anticipated retention rates of patients and volunteers in clinical trials and difficulty in maintaining contact with
patients after treatment, resulting in incomplete data;
• failure of us, our CROs or clinical trial sites to comply with regulatory requirements;
• failure of our CROs or clinical trial sites to meet their contractual obligations to us in a timely manner, or at all, deviating
from the clinical trial protocol or dropping out of a trial;
• delays relating to adding new clinical trial sites;
• delays in establishing necessary pre-clinical or clinical data;
• the occurrence of unexpected severe or serious product-related adverse events in a clinical trial;
• the quality or stability of the product candidate falling below acceptable standards;
• the inability to produce or obtain sufficient quantities of the product candidate to complete clinical trials on time, or delays
in sufficiently developing, characterizing or controlling a manufacturing process suitable for clinical trials;
• supply chain constraints and inflationary pressures;
• the lack of adequate funding to continue the clinical trial;
• developments observed in trials conducted by competitors for related technology that raises general concerns from
regulatory authorities about risk to patients of similar vaccine technology;
• the determination that a product candidate will not be producible in relevant quantities at the manufacturing stage;
• the failure of regulatory authorities such as the FDA or the TFDA to approve our manufacturing processes or facilities or
those of contract manufacturers with which we contract for clinical and commercial supplies; and
• the transfer of manufacturing processes to larger-scale facilities operated by contract manufacturers or by us, and delays
or failure by our contract manufacturers or us to make any necessary changes to such manufacturing process.
In addition, pre-clinical and clinical data are often susceptible to varying interpretations and analyses and results from post-hoc data
analysis may not be predictive of final results and may not support product approval. Many companies that believed their product
candidates performed satisfactorily in pre-clinical studies and clinical trials have nonetheless failed to obtain marketing approval for
their product candidates. Regulatory authorities have substantial discretion in the approval process and in determining when or whether
regulatory approval will be obtained for any of our product candidates. Additionally, the FDA typically does not accept post-hoc data
analyses as support for regulatory approval. Even if we believe the data collected from clinical trials of our product candidates are
promising, such data may not be sufficient to support approval by regulatory authorities. Regulatory authorities may disagree with the
design or implementation of our clinical trials and may disagree with our interpretation of data from pre-clinical studies or clinical trials.
In some instances, there can be significant variability in safety and/or efficacy results between different trials of the same product
candidate due to numerous factors, including changes in trial procedures set forth in protocols, differences in the size and type of the
patient populations, adherence to the dosing regimen and other trial procedures and the rate of dropout among clinical trial participants.
Further, none of our trials to date of UB-311 and UB-312 have been large enough to determine whether their assessments of efficacy
were statistically significant. Therefore, we are able to report potential trends on such measures, but we will not be able to make more
definitive statements about the efficacy of our product candidates until we complete clinical trials that are adequately powered to
demonstrate statistical significance of clinically meaningful results.
Moreover, for AD, given the difficulties in assessing whether a product candidate is disease-modifying in terms of delaying cognition
and other symptoms of AD, we plan to include in our trial designs for UB-311 biomarker endpoints and, if our trial results warrant, may
apply for regulatory approval based on biomarker data. While the FDA recently approved aducanumab based on biomarker data, there
is no assurance that the FDA will accept biomarker data for other product candidates, including UB-311, in the future.
Even if we obtain approval of any of our product candidates in one jurisdiction, we may never obtain approval for or commercialize
any of our products in other jurisdictions, which would limit our ability to realize the full market potential of our product candidates.
To market any products, we must establish and comply with numerous and varying regulatory requirements in different countries
regarding safety and efficacy and obtain relevant approvals to market our product candidates. As discussed in another risk factor above
(“
Clinical drug development involves a lengthy and expensive process…
”) an EUA for UB-612 was denied by the TFDA in August
50
2021, which decision we have appealed in collaboration with UBIA. Approval by the TFDA or by another foreign regulatory authority
in any other jurisdiction does not ensure approval by comparable regulatory authorities in other countries or jurisdictions, including
approval by the FDA in the United States. The failure to obtain approval in one jurisdiction may delay or otherwise negatively impact
our ability to obtain approval elsewhere. In addition, clinical trials conducted in one country may not be accepted by regulatory
authorities in other countries. Approval procedures vary among countries and even if we have obtained approval in one country, approval
in other countries can involve additional product testing and validation and additional administrative review periods.
Seeking regulatory approvals in different countries could result in additional and unexpected costs for us, including as a result of
additional required pre-clinical studies or clinical trials which would be costly and time-consuming. Satisfying regulatory requirements
is costly, time-consuming, uncertain and may be subject to unanticipated delays. In addition, our failure to obtain regulatory approval
in any country may delay or have negative effects on the process for regulatory approval in other countries. Apart from our ELISA test,
which has been approved for sale by the FDA through an EUA, we do not have any product candidates approved for sale in any
jurisdiction, including international markets. We do not have experience in obtaining regulatory approval in international markets, and
we will be relying on our collaboration partners such as UBIA to assist us in this process. If we fail to comply with regulatory
requirements in international markets or to obtain and maintain required approvals, our ability to realize the full market potential of our
products will be harmed.
Interim, “top-line” and preliminary data from our clinical trials that we announce or publish from time to time may change as more
patient data become available and are also subject to audit and verification procedures that could result in material changes in the
final data.
From time to time, we may publicly disclose preliminary or top-line data from our pre-clinical studies and clinical trials, which are based
on a preliminary analysis of then-available data, and the results and related findings and conclusions are subject to change following a
more comprehensive review of the data related to the particular study or trial. We also may make assumptions, estimations, calculations
and conclusions as part of our analyses of data, and we may not have received or had the opportunity to fully and carefully evaluate all
data. As a result, the top-line or preliminary results that we report may differ from future results of the same studies, or different
conclusions or considerations may qualify such results, once additional data have been received and fully evaluated. Top-line data also
remain subject to audit and verification procedures that may result in the final data being materially different from the preliminary data
we previously published. As a result, top-line data should be viewed with caution until the final data are available.
From time to time, we may also disclose interim data from our pre-clinical studies and clinical trials. Interim data from clinical trials
that we may complete are subject to the risk that one or more of the clinical outcomes may materially change as patient enrollment
continues and more patient data become available or as patients from our clinical trials continue other treatments for their disease.
Adverse differences between preliminary or interim data and final data could significantly harm our business prospects. Further,
disclosure of interim data by us or by our competitors could result in volatility in the price of our Class A common stock.
Further, others, including regulatory authorities, may not accept or agree with our assumptions, estimates, calculations, conclusions or
analyses or may interpret or weigh the importance of data differently, which could impact the value of the particular program, the
approvability or commercialization of the particular product candidate or product and the Company in general. In addition, the
information we choose to publicly disclose regarding a particular study or clinical trial is based on what is typically extensive
information, and you or others may not agree with what we determine is material or otherwise appropriate information to include in our
disclosure.
If we encounter difficulties enrolling patients in our clinical trials, our clinical development activities could be delayed and result in
increased costs and longer development periods or otherwise be adversely affected.
We will be required to identify and enroll a sufficient number of patients for our planned clinical trials. Trial participant enrollment
could be limited in future trials given that many potential participants may be ineligible because of pre-existing conditions, medical
treatments or other reasons. For example, trial participant enrollment for UB-612 could be negatively impacted as COVID-19
vaccination rates continue to increase and the number of potential unvaccinated participants continues to decrease. Similarly, the next
phase of our UB-311 trial could be affected by worldwide effects resulting from the Russia-Ukraine conflict and other geopolitical
factors. We may not be able to initiate or continue clinical trials required by applicable regulatory authorities or any of our other product
candidates that we pursue if we are unable to locate and enroll enough eligible patients or volunteers to participate in these clinical trials.
Patient enrollment is affected by other factors, as well, including the incidence and severity of the disease under investigation; the design
of the clinical trial protocol; the size and nature of the patient population; the eligibility criteria for the trial in question; the perceived
risks and benefits of the product candidate under trial; the perceived safety and tolerability of the product candidate; the proximity and
availability of clinical trial sites for prospective patients; the availability of competing therapies and clinical trials; effects of the COVID-
19 pandemic on our clinical trial sites; our ability to monitor patients adequately during and after treatment; patient referral practices of
physicians; clinicians’ and patients’ perceptions as to the potential advantages of the drug being studied in relation to other available
therapies, including standard-of-care and any new drugs that may be approved for the indications we are investigating; and efforts to
facilitate timely enrollment in clinical trials.
51
We also may encounter difficulties in identifying and enrolling such patients with a stage of disease appropriate for our ongoing or
future clinical trials. In addition, the process of finding and diagnosing patients may prove costly. Our inability to enroll a sufficient
number of patients for any of our clinical trials would result in significant delays or may require us to abandon one or more clinical
trials.
Even if we obtain regulatory approval for a product candidate, our products will remain subject to regulatory scrutiny and post-
marketing requirements.
Any regulatory approvals that we may receive for our product candidates will require the submission of reports to regulatory authorities
and ongoing surveillance to monitor the safety and efficacy of the product candidate, may contain significant limitations related to use
restrictions for specified age groups, warnings, precautions or contraindications, and may include burdensome post-approval study or
risk management requirements. For example, the FDA may require a Risk Evaluation and Mitigation Strategy (“REMS”) to approve
our product candidates, which could entail requirements for a medication guide, physician training and communication plans or
additional elements to ensure safe use, such as restricted distribution methods, patient registries and other risk minimization tools. In
addition, if one of our product candidates is approved in the United States or abroad, it will be subject to ongoing regulatory requirements
for manufacturing, labeling, packaging, storage, advertising, promotion, sampling, record-keeping, conduct of post-marketing studies
and submission of safety, efficacy and other post- market information. Manufacturers and manufacturers’ facilities are required to
comply with extensive requirements by regulatory authorities, including ensuring that quality control and manufacturing procedures
conform to cGMP regulations. As such, we and our contract manufacturers will be subject to continual review and inspections to assess
compliance with cGMP and adherence to commitments made in any approved marketing application. Accordingly, we and others with
whom we work must continue to expend time, money and effort in all areas of regulatory compliance, including manufacturing,
production and quality control.
If a regulatory authority such as the FDA discovers previously unknown problems with a product, such as adverse events of unanticipated
severity or frequency, or problems with product quality or the facility where the product is manufactured, or disagrees with the
promotion, marketing or labeling of a product, such regulatory authorities may impose restrictions on that product or us, including
requiring withdrawal of the product from the market. If we fail to comply with applicable regulatory requirements, a regulatory authority
or enforcement authority may, among other things: issue warning letters; impose civil or criminal penalties; suspend or withdraw
regulatory approval; suspend any of our clinical trials; refuse to approve pending applications or supplements to approved applications
submitted by us; impose restrictions on our operations, including closing our contract manufacturers’ facilities; or seize or detain
products, or require a product recall.
Any government investigation of alleged violations of law could require us to expend significant time and resources in response and
could generate negative publicity. Any failure to comply with ongoing regulatory requirements may adversely affect our ability to
commercialize and generate revenue from our products. If regulatory sanctions are applied or if regulatory approval is withdrawn, our
business will be seriously harmed. Further, if a regulatory authority identifies previously unknown problems with our platform, any or
all of our product candidates may also be affected.
Furthermore, the burden of these requirements may outweigh any benefit or revenue that we could generate from product sales. Even if
we obtain regulatory approval for a product candidate, compliance with the many post-approval regulations may be so costly that it
becomes financially prudent to abandon the product or sell ownership of the underlying intellectual property at prices that are not
sufficient to recoup our investment in developing the product.
Moreover, the policies of regulatory authorities may change, and additional government regulations may be enacted that could prevent,
limit or delay regulatory approval of our product candidates. We cannot predict the likelihood, nature or extent of government regulation
that may arise from future legislation or administrative or executive action, either in the United States or abroad. If we are slow or unable
to adapt to changes in existing requirements or the adoption of new requirements or policies, or if we are not able to maintain regulatory
compliance, we may lose any marketing approval that we may have obtained and we may not achieve or sustain profitability.
We have no history of commercializing pharmaceutical products, which may make it difficult to evaluate the prospects for our future
viability.
We commenced operations through UNS and COVAXX in 2014 and 2020, respectively, and as Vaxxinity in March 2021. Our operations
to date have been limited to organizing and staffing Vaxxinity, business planning, raising capital, developing our Vaxxine Platform,
identifying and testing potential product candidates and conducting clinical trials. We have a limited track record of successfully
conducting late-stage clinical trials, obtaining marketing approvals, manufacturing a commercial-scale product, or arranging for a third-
party to do so on our behalf, or conducting sales and marketing activities necessary for successful product commercialization.
Accordingly, you should consider our prospects considering the costs, uncertainties, delays and difficulties frequently encountered by
companies in the early stages of development, especially clinical-stage biopharmaceutical companies such as ours. Any predictions you
make about our future success or viability may not be as accurate as they could be if we had a longer operating history or a history of
successfully developing and commercializing pharmaceutical products.
52
We may encounter unforeseen expenses, difficulties, complications, delays and other known or unknown factors in achieving our
business objectives. We will eventually need to transition from a company with a development focus to a company capable of supporting
commercial activities. We may not be successful in such a transition.
We expect our financial condition and operating results to continue to fluctuate significantly from quarter to quarter and year to year
due to a variety of factors, many of which are beyond our control. Accordingly, you should not rely upon the results of any quarterly or
annual periods as indications of future operating performance.
Our product candidates may cause undesirable side effects that could delay or prevent their regulatory approval, limit the commercial
profile of an approved label or result in significant negative consequences following regulatory approval, if any.
Undesirable side effects that may be caused by our product candidates could cause us, our collaboration partners or the regulatory
authorities to interrupt, delay or halt clinical trials and could result in a more restrictive label or the delay or denial of approval by
regulatory authorities. Results of our trials could reveal a high and unacceptable severity and prevalence of side effects. In such an event,
our trials could be suspended or terminated and regulatory authorities could order us to cease further development of or deny approval
of our product candidates for any or all targeted indications. The product-related side effects could affect patient recruitment or the
ability of enrolled patients to complete the trial or result in potential product liability claims. Any of these occurrences may harm our
business, financial condition, results of operations and prospects significantly.
Clinical trials assess a sample of the potential patient population. With a limited number of patients and duration of exposure, rare and
severe side effects of our product candidates may only be uncovered with a significantly larger number of patients exposed to the product
candidate. If our product candidates receive an EUA or regulatory approval and we or others identify undesirable side effects caused by
such product candidates (or any other similar products) after such approval, a number of potentially significant negative consequences
could result, including:
• regulatory authorities may withdraw or limit their approval of such product candidates and require us to take our approved
product(s) off the market;
• regulatory authorities may require the addition of labeling statements, such as a “boxed” warning or a contraindication, or
submission of field alerts to physicians and pharmacies;
• we may be required to create a medication guide outlining the risks of such side effects for distribution to patients;
• we may be required to change the way such product candidates are distributed or administered, conduct additional clinical
trials or change the labeling of the product candidates;
• actual or potential drug-related side effects could negatively affect patient recruitment or the ability of enrolled patients to
complete a trial for our products or product candidates;
• market acceptance of our products by patients and physicians may be reduced and sales of the product may decrease
significantly;
• regulatory authorities may require a REMS plan to mitigate risks, which could include medication guides, physician
communication plans, or elements to assure safe use, such as restricted distribution methods, patient registries and other
risk minimization tools;
• we may be subject to regulatory investigations and government enforcement actions;
• we may decide or be required to remove such product candidates from the marketplace;
• we could be sued and potentially held liable for injury caused to individuals exposed to or taking our product candidates;
• sales of the product(s) may decrease substantially; and
• our reputation may suffer.
Any of these events could prevent us from achieving or maintaining market acceptance of the affected product candidates and could
substantially increase the costs of commercializing our product candidates, if approved, and therefore could have a material adverse
effect on our business, financial condition, results of operations and prospects.
53
The regulatory landscape that will govern our product candidates is uncertain. Regulations that impact our product candidates are
still
developing, and changes in regulatory requirements could result in delays or discontinuation of development of our product
candidates or unexpected costs in obtaining regulatory approval.
The regulatory requirements to which our product candidates will be subject are complex and uncertainties exist. Even with respect to
more established vaccine products, the regulatory landscape is still developing, especially as it relates to novel adjuvants in vaccines,
such as CpG1, which we use at low concentration in UB-612. Although regulatory authorities decide whether individual clinical trial
protocols may proceed, the review process and determinations of other reviewing bodies can impede or delay the initiation of a clinical
trial, even if another regulatory authority has reviewed the trial and authorizes its initiation. The FDA, for example, can place an IND
on clinical hold even if other regulatory agencies have provided a favorable review. In addition, adverse developments in clinical trials
involving novel adjuvants in vaccines, such as CpG1, conducted by others may cause regulatory authorities to change the requirements
for approval of any of our product candidates.
Complex regulatory environments exist in other jurisdictions in which we might consider seeking regulatory approvals for our product
candidates, further complicating the regulatory landscape. For example, in the European Union a special committee called the Committee
for Advanced Therapies was established within the European Medicines Authority in accordance with Regulation (EC) No 1394/2007
on advanced-therapy medicinal products (“ATMPs”), to assess the quality, safety and efficacy of ATMPs, and to follow scientific
developments in the field.
These various regulatory review committees and advisory groups and new or revised guidelines that they promulgate from time to time
may lengthen the regulatory review process, require us to perform additional studies, increase our development costs, lead to changes
in regulatory positions and interpretations, delay or prevent approval and commercialization of our product candidates or lead to
significant post-approval limitations or restrictions. We may face even more cumbersome and complex regulations than those emerging
for novel adjuvants. Furthermore, even if our product candidates obtain required regulatory approvals, such approvals may later be
withdrawn because of changes in regulations or the interpretation of regulations by applicable regulatory authorities.
Even if we receive regulatory approval to market any of our product candidates, we will be subject to ongoing obligations and continued
regulatory review, which may materially adversely affect our business, financial condition, results of operations and prospects. We have
not previously submitted a biologics license application (“BLA”) to the FDA, or similar regulatory approval filings to comparable
foreign authorities, for any product candidate and never received regulatory approval for any of our product candidates. Further, other
jurisdictions may consider our product candidates to be new drugs, not biologics or medicinal products, and require different marketing
applications. Even if a regulatory authority approves any of our product candidates, the manufacturing processes, labeling, packaging,
distribution, product sampling, adverse event reporting, storage, advertising, marketing, promotion and recordkeeping for the product
will be subject to extensive and ongoing regulatory requirements. These requirements include submissions of safety and other post-
marketing information and reports and registration, as well as continued compliance with cGMPs and GCPs for any clinical trials that
we conduct post-approval, all of which may result in significant expense and limit our ability to commercialize such products. There
also are continuing, annual program user fees for any marketed products. In the United States, biologic manufacturers and their
subcontractors are required to register their establishments with the FDA and certain state agencies and are subject to periodic
unannounced inspections by the FDA and certain state agencies for compliance with cGMP, which impose certain procedural and
documentation requirements upon us and our contract manufacturers. Changes to the manufacturing process are strictly regulated, and,
depending on the significance of the change, may require prior FDA approval before being implemented. FDA regulations also require
investigation and correction of any deviations from cGMP and impose reporting requirements upon us and any contract manufacturers
that we may decide to use. Accordingly, manufacturers must continue to expend time, money and effort in production and quality control
to maintain compliance with cGMP and other aspects of regulatory compliance.
Any regulatory approvals that we receive for our product candidates may also be subject to limitations on the approved indicated uses
for which the product may be marketed or to the conditions of approval, or contain requirements for potentially costly post-marketing
testing and surveillance to monitor the safety and efficacy of the product. For example, the FDA has the authority to require a REMS as
part of a BLA or after approval, which may impose further requirements or restrictions on the distribution or use of an approved product,
such as limiting prescribing to certain physicians or medical centers that have undergone specialized training, limiting treatment to
patients who meet certain safe-use criteria and requiring treated patients to enroll in a registry. Later discovery of previously unknown
problems with a product, including adverse events of unanticipated severity or frequency, or with our contract manufacturers or
manufacturing processes, or failure to comply with regulatory requirements may result in, among other things:
• restrictions on the marketing or manufacturing of the product, withdrawal of the product from the market, or voluntary or
mandatory product recalls;
• fines, warning letters, untitled letters or holds on clinical trials;
• refusal by regulatory authorities to approve pending applications or supplements to approved applications, or suspension
or revocation of product approvals;
54
• requirements to conduct additional clinical trials, change our product labeling or submit additional applications or
application supplements;
• product seizure or detention, or refusal to permit the import or export of products;
• mandated modification of promotional materials and labeling and the issuance of corrective information;
• consent decrees, corporate integrity agreements, debarment or exclusion from federal healthcare programs;
• the issuance of safety alerts, Dear Healthcare Provider letters, press releases and other communications containing
warnings or other safety information about the product; or
• injunctions or the imposition of civil or criminal penalties.
In addition, regulatory policies may change or additional government regulations or legislation may be enacted that could prevent, limit
or delay regulatory approval of our product candidates, particularly in countries where elections may result in changes in government
administration. If we fail to comply with existing requirements, are slow or unable to adapt to changes in existing requirements or the
adoption of new requirements or policies, or if we are not able to maintain regulatory compliance, we may lose any regulatory approval
that we may have obtained or face regulatory or enforcement actions, which may materially adversely affect our business, financial
condition, results of operations and prospects.
The FDA strictly regulates the promotional claims that may be made about prescription products in the United States. In particular, a
product may not be promoted for uses that are not approved by the FDA as reflected in the product’s approved labeling. If we receive
marketing approval for a product candidate, physicians may nevertheless prescribe it to their patients in a manner that is inconsistent
with the approved label. If we are found to have promoted such off-label uses, we may become subject to significant liability. The FDA
and other agencies actively enforce the laws and regulations prohibiting the promotion of off-label uses, and a company that is found to
have improperly promoted off-label uses may be subject to significant sanctions. Federal and state government agencies have levied
large civil and criminal fines against companies for alleged improper promotion and has enjoined several companies from engaging in
off-label promotion. The FDA has also requested that companies enter into consent decrees or permanent injunctions under which
specified promotional conduct is changed or curtailed.
Any government investigation of alleged violations of law could require us to expend significant time and resources in response and
could generate negative publicity. Any failure to comply with ongoing regulatory requirements may significantly and adversely affect
our ability to commercialize our product candidates.
A breakthrough therapy designation or fast track designation by the FDA for a product candidate may not lead to a faster
development or regulatory review or approval process, and it would not increase the likelihood that the product candidate will receive
marketing approval.
We may in the future seek a breakthrough therapy designation or fast track designation for one or more product candidates eligible for
such designation. A breakthrough therapy is defined as a product candidate that is intended, alone or in combination with one or more
other drugs, to treat a serious or life-threatening disease or condition, and preliminary clinical evidence indicates that the product
candidate may demonstrate substantial improvement over existing therapies on one or more clinically significant endpoints, such as
substantial treatment effects observed early in clinical development. For product candidates that have been designated as breakthrough
therapies, interaction and communication between the FDA and the sponsor of the trial can help to identify the most efficient path for
clinical development while minimizing the number of patients placed in ineffective control regimens. Product candidates designated as
breakthrough therapies by the FDA are also eligible for priority review if supported by clinical data at the time of the submission of the
BLA.
Designation as a breakthrough therapy is within the discretion of the FDA. Accordingly, even if we believe that one of our product
candidates meets the criteria for designation as a breakthrough therapy, the FDA may disagree and instead determine not to make such
designation. In any event, the receipt of a breakthrough therapy designation for a product candidate may not result in a faster development
process, review or approval compared to product candidates considered for approval under conventional FDA procedures and it would
not assure ultimate approval by the FDA. In addition, even if one or more of our product candidates qualify as breakthrough therapies,
the FDA may later decide that the product candidate no longer meets the conditions for qualification or it may decide that the time period
for FDA review or approval will not be shortened. Further, certain of our product candidates, including UB-612, are not eligible for
breakthrough therapy designation, and we will be unable to take advantage of such designation for such product candidates.
Fast track designation is designed to facilitate the development and expedite the review of therapies to treat serious conditions and fill
an unmet medical need. Programs with fast track designation may benefit from early and frequent communications with the FDA,
potential priority review and the ability to submit a rolling application for regulatory review. Fast track designation applies to both the
product candidate and the specific indication for which it is being studied. However, even if one or more of our product candidates
55
qualify for fast track designation, we may not be able to meet the criteria of the fast track designation, or if our clinical trials are delayed,
suspended or terminated, or put on clinical hold due to unexpected adverse events or issues with clinical supply, we will not receive the
benefits associated with the fast track program. Furthermore, fast track designation does not change the standards for approval. Fast
track designation alone does not guarantee qualification for the FDA’s priority review procedures. Fast track designation also does not
guarantee our product candidate will be approved in a timely manner, if at all.
We are currently attempting to secure approval of certain product candidates through the use of an accelerated approval pathway.
If we are unable to obtain such approval, we may be required to conduct additional pre-clinical studies or clinical trials beyond those
that we contemplate, which could increase the expense of obtaining, and delay the receipt of, necessary marketing approvals. Even
if our product candidates receive accelerated approval from regulatory authorities, if our confirmatory trials do not verify clinical
benefit, or if we do not comply with rigorous post-marketing requirements, such regulatory authorities may seek to withdraw
accelerated approval.
We are developing certain product candidates for the treatment of serious or life-threatening conditions, including UB-311, and therefore
may decide to seek approval of such product candidates under the FDA’s accelerated approval pathway. A product may be eligible for
accelerated approval if it is designed to treat a serious or life-threatening disease or condition and generally provides a meaningful
advantage over available therapies upon a determination that the product candidate has an effect on a surrogate endpoint or intermediate
clinical endpoint that is reasonably likely to predict clinical benefit. The FDA considers a clinical benefit to be a positive therapeutic
effect that is clinically meaningful in the context of a given disease, such as irreversible morbidity or mortality. For the purposes of
accelerated approval, a surrogate endpoint is a marker, such as a laboratory measurement, radiographic image, physical sign or other
measure that is thought to predict clinical benefit but is not itself a measure of clinical benefit. An intermediate clinical endpoint is a
clinical endpoint that can be measured earlier than an effect on irreversible morbidity or mortality that is reasonably likely to predict an
effect on irreversible morbidity or mortality or other clinical benefit.
The accelerated approval pathway may be used in cases in which the advantage of a new drug over available therapy may not be a direct
therapeutic advantage but is a clinically important improvement from a patient and public health perspective. If granted, accelerated
approval is usually contingent on the sponsor’s agreement to conduct, in a diligent manner, additional post-approval confirmatory studies
to verify and describe the drug’s clinical benefit. If the sponsor fails to conduct such studies in a timely manner, or if such post- approval
studies fail to validate the drug’s predicted clinical benefit, the FDA may withdraw its approval of the drug on an expedited basis.
If we decide to submit a BLA seeking accelerated approval or receive an expedited regulatory designation for our product candidates,
there can be no assurance that such submission or application will be accepted or that any expedited development, review or approval
will be granted on a timely basis, or at all. Failure to obtain accelerated approval or any other form of expedited development, review or
approval for a product candidate would result in a longer time period to commercialization of such product candidate, if any, and could
increase the cost of development of such product candidate, which could harm our competitive position in the marketplace. An EUA for
UB-612 was denied by the TFDA in August 2021. If we do not receive an EUA from regulatory authorities for product candidates for
which we request such approval, we may be required to conduct further clinical trials which could increase the expense of obtaining,
and delay the receipt of, marketing approvals in any jurisdiction where we do not receive an EUA. Some regulatory authorities, including
the FDA, have ceased granting EUAs for product candidates targeting COVID-19 or otherwise, which could delay our ability to
commercialize product candidates.
Because we are developing product candidates for the treatment or prevention of diseases in which there is little clinical experience
using new technologies, there is increased risk that the FDA, the TFDA or other foreign regulatory authorities may not consider the
endpoints of our clinical trials to provide clinically meaningful results and that these results may be difficult to analyze.
As we are developing novel treatments and preventative measures for diseases in which we believe there is limited clinical experience
with new endpoints and methodologies, there is heightened risk that the applicable regulatory authorities may not consider the clinical
trial endpoints to provide clinically meaningful results, and the resulting clinical data and results may be more difficult to analyze. It is
difficult to determine how long it will take, if ever, or how much it will cost to obtain regulatory approvals for our product candidates
in the United States, Taiwan or other jurisdictions, if ever. Further, approvals by one regulatory authority may not be indicative of what
other regulatory authorities may require for approval.
During the regulatory review process, we will need to identify success criteria and endpoints such that regulatory authorities will be able
to determine the clinical efficacy and safety profile of any product candidates we may develop. Because our initial focus is to identify
and develop product candidates to treat or prevent diseases in which there is little clinical experience using new technologies, there is
heightened risk that regulatory authorities may not consider the clinical trial endpoints that we propose to provide clinically meaningful
results. In addition, the resulting clinical data and results may be difficult to analyze.
In the United States, the FDA also weighs the benefits of a product against its risks, and the FDA may view the efficacy results in the
context of safety as not being supportive of regulatory approval. The TFDA and other foreign regulatory authorities may make similar
comments with respect to these endpoints and data. Any product candidate we may develop will be based on a novel technology that
makes it difficult to predict the time and cost of development and of subsequently obtaining regulatory approval.
56
We and our collaboration partners have conducted and intend to conduct additional clinical trials for selected product candidates at
sites outside the United States, and for any of our product candidates for which we seek approval in the United States, the FDA may
not accept data from trials conducted in such locations or may require additional U.S.-based trials.
We and our collaboration partners have conducted, currently are conducting and intend in the future to conduct, clinical trials outside
the United States, particularly in Taiwan where we have reported interim results of our UB-612 Phase 2 clinical trial.
Although the FDA may accept data from clinical trials conducted outside the United States, acceptance of these data is subject to certain
conditions imposed by the FDA. For example, the clinical trial must be conducted by qualified investigators in accordance with GCPs,
and the FDA must be able to validate the trial data through an on-site inspection, if necessary. Generally, the patient population for any
clinical trial conducted outside of the United States must be representative of the population for which we intend to seek approval in the
United States. There can be no assurance that the FDA will accept data from trials conducted outside of the United States. If the FDA
does not accept the data from any clinical trials that we or our collaboration partners conduct outside the United States, it would likely
result in the need for additional clinical trials, which would be costly and time-consuming and delay or permanently halt our ability to
develop and market these or other product candidates in the United States. In other jurisdictions, for instance, in Taiwan, there is a
similar risk regarding the acceptability of clinical trial data conducted outside of that jurisdiction.
In addition, there are risks inherent in conducting clinical trials in multiple jurisdictions, inside and outside of the United States, such
as:
• regulatory and administrative requirements of the jurisdiction where the trial is conducted that could burden or limit our
ability to conduct our clinical trials;
• foreign exchange fluctuations;
• manufacturing, customs, shipment and storage requirements;
• cultural differences in medical practice and clinical research; and
• the risk that the patient populations in such trials are not considered representative as compared to the patient population
in the target markets where approval is being sought.
If any of our product candidates receive an EUA or regulatory approval, such products may not achieve broad market acceptance
among government agencies, physicians, patients, the medical community and third-party payors, in which case revenue generated
from their sales would be limited.
The commercial success of our product candidates and our ability to generate revenues from our products will depend upon their
acceptance among government agencies, physicians, patients and the medical community. The degree of market acceptance of our
product candidates will depend on a number of factors, including:
• limitations or warnings contained in the approved labeling for a product candidate and any other product insert
requirements of regulatory authorities;
• changes in the standard of care for the targeted indications for any of our product candidates;
• limitations in the approved clinical indications for our product candidates;
• demonstrated clinical safety and efficacy compared to other products;
• the impact of disease variants, such as the Delta variant of SARS-CoV-2, on the efficacy and marketability of our product
candidates targeting such diseases;
• lack of significant adverse side effects, and the prevalence and severity of any side effects;
• sales, marketing and distribution support;
• availability of coverage and extent of reimbursement from managed care plans and other third-party payors;
• timing of market introduction and perceived effectiveness of our products as well as competitive products;
• continued projected growth of the markets in which our products compete;
57
• the degree of cost-effectiveness of our product candidates;
• the impact of past product price increases and limitations on future price increases for our products;
• availability of alternative therapies;
• whether the product is designated under physician treatment guidelines as a first-line therapy or as a second or third-line
therapy for particular diseases;
• whether the product can be used effectively with other therapies to achieve higher response rates;
• adverse publicity about our product candidates or favorable publicity about competitive products;
• if and when we are able to obtain regulatory approvals for indications for our products;
• our ability to establish and maintain a continuous supply of our products for commercial sale;
• potential or perceived advantages or disadvantages of our products over alternative treatments;
• convenience and ease of administration of our products; and
• the effect of current and future healthcare laws.
If any of our product candidates are approved, but do not achieve an adequate level of acceptance by government agencies as well as
physicians, patients and the medical community, we may not generate sufficient revenue from these products, and we may not become
or remain profitable. In addition, efforts to educate the medical community and third-party payors on the benefits of our product
candidates may require significant resources and may never be successful.
We may focus on potential product candidates that may prove to be unsuccessful and such focus may require us to forego
opportunities to develop other product candidates that may prove to be more successful.
We may choose to focus our efforts and resources on a potential product candidate that ultimately proves to be unsuccessful, or to license
or purchase a marketed product that does not meet our financial expectations. Furthermore, we have limited financial and personnel
resources and are placing significant focus on the development of our lead product candidates, and as such, we may forgo or delay
pursuit of opportunities with other future product candidates that later prove to have greater commercial potential. Our spending on
current and future research and development programs and other future product candidates for specific indications may not yield any
commercially viable future product candidates and could result in spending on raw materials that cannot be repurposed. As a result of
our resource allocation decisions, we may fail to capitalize on viable commercial products or profitable market opportunities, be required
to forego or delay pursuit of opportunities with other product candidates or other diseases that may later prove to have greater commercial
potential, fail to identify novel product candidates that may be successful, or relinquish valuable rights to such product candidates
through collaboration, licensing or other arrangements in cases in which it would have been advantageous for us to retain sole
development and commercialization rights. If we are unable to identify and successfully commercialize additional suitable product
candidates, or if the additional product candidates we do identify and develop prove to be ineffective, incapable of being commercialized
on a large scale or otherwise fail to achieve market success, this would adversely impact our business strategy and our financial position.
Risks Related to Our Financial Position and Need for Additional Capital
We cannot assure you of the adequacy of our capital resources to successfully complete the development and commercialization of
our product candidates, and a failure to obtain additional capital, if needed, could force us to delay, limit, reduce or terminate one
or more of our product development programs or commercialization efforts.
As of December 31, 2021, we had cash and cash equivalents amounting to $144.9 million. We believe that we will continue to expend
substantial resources for the foreseeable future developing our proprietary product candidates. These expenditures will include costs
associated with research and development, conducting pre-clinical studies and clinical trials, seeking regulatory approvals, as well as
launching and commercializing products approved for sale and costs associated with manufacturing products. In addition, other
unanticipated costs may arise. Because the outcomes of our anticipated clinical trials are highly uncertain, we cannot reasonably estimate
the actual amounts necessary to successfully complete the development and commercialization of our proprietary product candidates.
Our future funding requirements will depend on many factors, including but not limited to:
• the numerous risks and uncertainties associated with developing product candidates and maintaining our platform;
58
• the number and characteristics of product candidates that we pursue;
• the rate of enrollment, progress, cost and outcomes of our clinical trials, which may or may not meet their primary end-
points;
• the timing of, and cost involved in, conducting non-clinical studies that are regulatory prerequisites to conducting clinical
trials of sufficient duration for successful product registration;
• the cost of manufacturing clinical supply and establishing commercial supply of our product candidates;
• the costs and timing of preparing, filing and prosecuting patent applications, maintaining and enforcing our intellectual
property rights and defending any intellectual property-related claims;
• tax and other compliance costs associated with operating in foreign jurisdictions (including any withholding requirements);
• the timing of, and the costs involved in, obtaining regulatory approvals for our product candidates if clinical trials are
successful;
• the timing of, and costs involved in, conducting post-approval studies that may be required by regulatory authorities;
• the cost of commercialization activities for our product candidates, including product manufacturing, pharmacovigilance,
marketing and distribution of product candidates generated from our platform and any other product opportunity for which
we receive marketing approval in the future;
• the terms and timing of any collaborative, licensing and other arrangements that we are currently party to or may establish,
including any required milestone and royalty payments thereunder and any non-dilutive funding that we may receive;
• the costs involved in preparing, filing, prosecuting, maintaining, defending and enforcing patent claims, including litigation
costs, if any, and the outcome of any such litigation;
• the timing, receipt and amount of sales of, or royalties or milestones on, our future products, if any, including the risk of
potential nonpayment by buyers of our future products, if any;
• the costs to recruit and build the organization including key executives needed to transform to a commercial organization;
and
• the costs of operating as a public company, including hiring additional personnel.
In addition, our operating plan may change as a result of many factors currently unknown to us. As a result of these factors, we may
need additional funds sooner than planned. We expect to finance future cash needs primarily through public or private equity offerings,
strategic collaborations and debt financing. If sufficient funds on acceptable terms are not available when needed, or at all, we could be
forced to significantly reduce operating expenses and delay, limit, reduce or terminate one or more of our product development programs
or commercialization efforts, which would have a negative impact on our business, financial condition, results of operations and
prospects.
We have incurred significant losses since our inception, and we expect to incur losses for the foreseeable future and may never
achieve or maintain profitability.
We have incurred significant losses since our inception. We had net losses of approximately $137.2 million and $40.0 million for the
years ended December 31, 2021 and 2020, respectively. As of December 31, 2021, our consolidated accumulated deficit was
$229.5 million. Our expectation is that we will continue to incur losses as we continue our research and development of, and seek
regulatory approvals for, our product candidates and maintain and develop new platforms, prepare for and begin to commercialize any
approved product candidates and add infrastructure and personnel to support our product development efforts and operations as a public
company. We have devoted substantially all of our financial resources and efforts to research and development, including pre-clinical
studies and clinical trials and we anticipate that our expenses will continue to increase over the next several years as we continue these
activities. The net losses and negative cash flows incurred to date, together with expected future losses, have had, and may continue to
have, an adverse effect on our working capital. The amount of future net losses will depend, in part, on the rate of future growth of our
expenses and our ability to generate revenue.
Because of the numerous risks and uncertainties associated with biopharmaceutical product development, we are unable to accurately
predict the timing or amount of increased expenses or when, or if, we will be able to achieve profitability. For example, our expenses
59
could increase if we are required by regulatory authorities such as the FDA to perform trials in addition to those that we currently expect
to perform, or if there are any delays in completing our currently planned clinical trials, the partnering process for our proprietary product
candidates or in the development of any of our proprietary product candidates.
Our revenue to date has been generated from the sales of our ELISA test and the sale of an option to negotiate a license with UNS
(which option has expired). Our ability to generate revenue and achieve profitability in the future depends in large part on our ability,
alone or with our collaborators, to achieve milestones and to successfully complete the development of, obtain the necessary regulatory
approvals for, and commercialize, our product candidates and Vaxxine Platform. We may never succeed in these activities and may
never generate revenue from product sales that is significant enough to achieve profitability. Even if we successfully obtain regulatory
approvals to market one or more of our product candidates, our revenues will be dependent, in part, upon the size of the markets in the
territories for which we gain regulatory approval and have commercial rights. If the markets for patient subsets that we are targeting are
not as significant as we estimate, we may not generate significant revenues from sales of such products, if approved. Even if we achieve
profitability in the future, we may not be able to sustain profitability in subsequent periods. Our failure to become or remain profitable
could depress our market value and could impair our ability to raise capital, expand our business, develop other product candidates or
continue our operations. A decline in our value could also cause you to lose all or part of your investment.
Raising additional capital may cause dilution to our shareholders, restrict our operations or require us to relinquish rights to our
technology or product candidates.
We expect our expenses to continue to increase in connection with our planned operations. To the extent that we raise additional capital
through the sale of our Class A common stock, convertible securities or other equity securities, your ownership interest will be diluted,
and the terms of these securities could restrict our operations or include liquidation or other preferences and anti-dilution protections
that could adversely affect your rights as a stockholder. The issuance of additional equity securities, or the possibility of such issuance,
may cause the market price of our Class A common stock to decline. In addition, debt financing, if available, may result in fixed payment
obligations and may involve agreements that include restrictive covenants that limit our ability to take specific actions, such as incurring
additional debt, making capital expenditures, creating liens, redeeming shares or declaring dividends, that could adversely impact our
ability to conduct our business. Securing financing could require a substantial amount of time and attention from our management and
may divert a disproportionate amount of their attention away from day-to-day activities, which may adversely affect our management’s
ability to oversee the development of our product candidates.
If we raise additional funds through collaborations or marketing, distribution or licensing arrangements with third parties, we may have
to relinquish valuable rights to our technologies, future revenue streams or product candidates or grant licenses on terms that may not
be favorable to us. If we are unable to raise additional funds when needed, we may be required to delay, limit, reduce or terminate our
product development or future commercialization efforts or grant rights to develop and market product candidates that we would
otherwise prefer to develop and market ourselves.
We cannot be certain that additional funding will be available on acceptable terms, or at all. If we are unable to raise additional capital
in sufficient amounts or on terms acceptable to us, we may have to significantly delay, scale back or discontinue the development or
commercialization of our product candidates or other research and development initiatives. Our current or future license agreements
may also be terminated if we are unable to meet the payment or other obligations under the agreements.
Changes in or reinterpretations of tax laws and regulations, including their application to us or our customers as reviewed by the
relevant tax authorities, may have a material adverse effect on our business, results of operations, financial condition and prospects.
We are subject to complex and evolving tax laws and regulations. New income, sales, use or other tax laws, statutes, rules, regulations
or ordinances could be enacted at any time, which could affect the tax treatment of any of our future domestic and foreign earnings. Any
new taxes could adversely affect our domestic and international business operations, and our business and financial performance.
Further, existing tax laws, statutes, rules, regulations or ordinances could be interpreted, changed, modified or applied adversely to us
or our customers. Future changes in applicable tax laws and regulations, or their interpretation and application, could have an adverse
effect on our business, financial conditions, results of operations and prospects.
In addition, our determination of our tax liability is subject to review by applicable tax authorities. Any adverse outcome of such a
review could harm our results of operations, cash flow and overall financial condition. The determination of our tax liabilities requires
significant judgment and, in the ordinary course of business, there are many transactions and calculations where the ultimate tax
determination is complex and uncertain.
Our ability to use our net operating loss carryforwards and other tax attributes to offset future taxable income may be subject to
certain limitations.
As of December 31, 2021, we had U.S. federal net operating loss carryforwards (“NOLs”) of $134.6 million, which may be available to
offset future taxable income, if any, and have no expiration date but are limited in their usage to an annual deduction equal to 80% of
annual taxable income. In general, under Sections 382 and 383 of the Internal Revenue Code of 1986, as amended (the “Code”), a
60
corporation that undergoes an “ownership change,” generally defined as a greater than 50% change by value in its equity ownership
over a three-year period, is subject to limitations on its ability to utilize its pre-change NOLs and its research and other tax attributes to
offset future taxable income. Our existing NOLs and tax attributes may be subject to limitations arising from previous ownership
changes, and if we undergo future ownership changes, our ability to utilize NOLs and research and tax attributes could be further limited
by Sections 382 and 383 of the Code. For these reasons, we may not be able to utilize a portion of our existing NOLs or research and
tax attributes.
Risks Related to the Manufacturing of Our Product Candidates
The formulation of peptide-based medicines is complex and manufacturers often encounter difficulties in production. If we, UBI or
any of our other contract manufacturers encounter difficulties, our ability to provide product candidates for clinical trials or
products, if approved, to patients or future customers could be delayed or halted.
The formulation of peptide-based medicines is complex and requires significant expertise and capital investment, including the
development of advanced manufacturing techniques and analytics. We are currently dependent on contract manufacturers, including
UBI, its affiliates, WuXi STA and CSBio, to conduct the manufacturing and supply activities for our product candidates and the
underlying component parts, but may choose to conduct these manufacturing activities ourselves in the future. If our contract
manufacturers are unable to manufacture our product candidates in clinical quantities or, when necessary, in commercial quantities and
at sufficient yields, then we will need to identify and reach supply arrangements with additional third parties. Further, our product
candidates may be in competition with other products for access to these facilities and may be subject to delays in manufacture if our
contract manufacturers give other products higher priority. We and our contract manufacturers must comply with cGMP, regulations
and guidelines for the manufacturing of our product candidates used in pre-clinical studies and clinical trials and, if approved, marketed
products. If we or our contract manufacturers do not receive any regulatory approvals, or lose existing approvals, required to manufacture
our product candidates, production and fulfilment of orders will be delayed, which may materially adversely affect our business.
Manufacturers of biotechnology products often encounter difficulties in production, particularly in scaling up and validating initial
production. Furthermore, if microbial, viral or other contaminations are discovered in our product candidates or in the manufacturing
facilities where our product candidates are made, such manufacturing facilities may be closed for an extended period of time to
investigate and remedy the contamination. Shortages of raw materials may also extend the period of time required to develop our product
candidates.
Manufacturing these products requires facilities specifically designed for and validated for this purpose and sophisticated quality
assurance and quality control procedures are necessary. Slight deviations anywhere in the manufacturing process, including filling,
labeling, packaging, storage and shipping and quality control and testing, may result in lot failures, product recalls or spoilage. Further,
delays in our clinical trials or in any regulatory approvals may result in the expiration of manufactured product, which could in turn lead
to further delays. When changes are made to the manufacturing process, we may be required to provide pre-clinical and clinical data
showing the comparable identity, strength, quality, purity or potency of the products before and after such changes. The use of
biologically derived ingredients can also lead to allegations of harm, including infections or allergic reactions, or closure of product
facilities due to possible contamination.
In addition, there are risks associated with large scale manufacturing for clinical trials or commercial scale including, among others,
cost overruns, potential problems with process scale-up, process reproducibility, stability issues, compliance with cGMP, lot consistency
and timely availability of raw materials. Even if we obtain marketing approval for any of our product candidates, there is no assurance
that we or our manufacturers will be able to manufacture the approved product to specifications acceptable to regulatory authorities, to
produce it in sufficient quantities to meet the requirements for the potential commercial launch of the product or to meet potential future
demand. If we or our manufacturers are unable to produce sufficient quantities for clinical trials, advance purchase commitments or
commercialization, more generally, our development and commercialization efforts would be impaired, which would have an adverse
effect on our business, financial condition, results of operations and prospects.
We cannot assure you that any disruptions or other issues relating to the manufacture of any of our product candidates will not occur in
the future. Any delay or interruption in the supply of clinical trial supplies could delay the completion of planned clinical trials, increase
the costs associated with maintaining clinical trial programs and, depending upon the period of delay, require us to commence new
clinical trials at additional expense or terminate clinical trials completely. Any adverse developments affecting clinical or commercial
manufacturing of our product candidates or products may result in shipment delays, inventory shortages, lot failures, product
withdrawals or recalls or other interruptions in the supply of our product candidates. We may also have to take inventory write-offs and
incur other charges and expenses for product candidates that fail to meet specifications, undertake costly remediation efforts or seek
more costly manufacturing alternatives. Accordingly, failures or difficulties faced at any level of our supply chain could delay or impede
the development and commercialization of any of our product candidates and could have an adverse effect on our business, financial
condition, results of operations and prospects.
61
We and our contract manufacturers and suppliers could be subject to liabilities, fines, penalties or other sanctions under federal,
state, local and foreign environmental, health and safety laws and regulations if we or they fail to comply with such laws or
regulations or otherwise incur costs that could have a material adverse effect on our business.
We currently rely on and expect to continue to rely on contract manufacturers for the manufacturing and supply of our product candidates
and custom components. We and these contract manufacturers are subject to various federal, state, local and foreign environmental,
health and safety laws and regulations, including those governing laboratory procedures and the generation, handling, labeling,
transportation, use, manufacture, storage, treatment and disposal of hazardous materials and wastes and worker health and safety. We
do not have control over a manufacturer’s or supplier’s compliance with environmental, health and safety laws and regulations.
Liabilities they incur pursuant to these laws and regulations could result in significant costs or in certain circumstances, an interruption
in operations, any of which could adversely affect our business, financial condition, results of operations and prospects.
With respect to any hazardous materials or waste which we are currently, or in the future will be, generating, handling, transporting,
using, manufacturing, storing, treating or disposing of, we cannot eliminate the risk of contamination or injury from these materials or
waste, including at third-party disposal sites. In the event of such contamination or injury, we could be held liable for any resulting
damages and liability. We also could be subject to significant civil or criminal fines and penalties, cessation of operations, investigation
or remedial costs or other sanctions for failure to comply with applicable environmental, health and safety laws. In addition, we may
incur substantial costs in order to comply with current or future environmental, health and safety laws and regulations. These current or
future laws and regulations may impair our research, development or production efforts or otherwise have a material adverse effect on
our business.
Undetected errors or defects in our production could harm our reputation or expose us to product liability claims.
Undetected errors and defects in the cGMP materials used in the production of our product candidates could result in a lower quality of
any products we produce, and could give rise to reputational harm to us and to the contract manufacturers with whom we work. If any
such errors or defects are discovered, we may incur significant costs, the attention of our key personnel could be diverted, or other
significant problems may arise. We may also be subject to warranty and liability claims for damages related to errors or defects in
products made with our cGMP materials. In addition, if we do not meet industry or quality standards, if applicable, such products may
be subject to recall. A material liability claim, recall or other occurrence that harms our reputation or decreases market acceptance of
such products could harm our business and operating results.
Risks Related to Our Reliance on UBI, Collaborators and Other Third Parties
Conflicts of interest and disputes have and may arise between us and UBI and its affiliates, and these conflicts and disputes might
ultimately be resolved in a manner unfavorable to us.
UBI is our largest stockholder, the licensor of certain of our intellectual property and is a commercial partner for the Company. In
addition, Dr. Chang Yi Wang, UBI’s founder, holds shares of our common stock. Our co-founders (Mei Mei Hu and Louis Reese), one
of their affiliates and UBI (collectively, our “principal stockholders”), are party to a voting agreement (the “Voting Agreement,”), which
provides Mei Mei Hu with the authority (and irrevocable proxies) to vote the shares of capital stock held by the stockholders party to
the Voting Agreement at her discretion on all matters to be voted upon by stockholders. Our CEO, Mei Mei Hu, and two of our other
directors, Louis Reese and James Chui, also serve on and constitute a majority of the board of directors of UBI. UBI’s equity interests
in the Company, and the overlapping directorships, could give rise to conflicts of interest, in particular when a decision could favor the
interests of UBI (or its affiliates) or us over the other. Further, we have historically depended heavily on UBI and its affiliates for our
business operations, including the provision of research, development and manufacturing services. While we have taken steps to
separate our operations from those of UBI and currently anticipate taking additional steps to lessen our dependence, we still have ongoing
commercial relationships with UBI and its affiliates. With respect to our UB-612 program, we have partnered with UBIA for the
development of UB-612 in Taiwan, UBIP for the formulation-fill-finish services, and UBP as the sole manufacturer of protein. Relating
to our chronic disease pipeline, we continue to work with UBI on certain early stage research activities, and UBIP and UBIA for the
production and testing of clinical material for our UB-312 program.
Conflicts of interest may arise with respect to existing or possible future commercial arrangements between us and UBI or any of its
affiliates in which the terms and conditions of the arrangements are subject to negotiation or dispute. For example, conflicts of interest
could arise over matters such as:
• disputes over the cost or quality of the manufacturing and testing services provided to us by UBI with respect to our product
candidates;
• the allocation of UBI’s resources as between our business objectives and UBI’s own objectives;
• a decision whether to engage UBI or its affiliates in the future to manufacture, test and supply of additional custom
components or product candidates for us;
62
• decisions as to which particular product candidates we will commit sufficient development efforts to; or
• business opportunities unrelated to our current products that may be attractive both to us and to the other company.
We also cannot guarantee conflicts of interest will not arise in connection with the negotiation or execution of any future agreement
with UBI, its affiliates or any other related party.
Further, we have been advised that there is currently an ongoing dispute within UBI between Dr. Wang and the other four members of
UBI’s board of directors relating to certain corporate governance matters, including the overall management and control of UBI, as well
as its relationship with the Company. Specifically, we have been advised that Dr. Wang attempted to replace the UBI board of directors
in July and August 2021 and is currently asserting that she is the majority shareholder of UBI, which we understand UBI’s other directors
dispute as invalid and incorrect, respectively. This dispute has created risks and uncertainties for us, and this dispute or any resolution
of it could negatively impact us, including, without limitation, by impairing our ability to work with UBI and its affiliates as a commercial
partner in the future and/or otherwise adversely affecting other existing arrangements with or involving UBI or its affiliates. Late in the
day on November 9, 2021, counsel to the Company received correspondence on behalf of Dr. Wang (the “Correspondence”). The
Correspondence outlined Dr. Wang’s concerns that the preliminary prospectus for our initial public offering, subject to completion,
dated November 5, 2021 did not accurately describe the relationship between the Company and UBI, namely the Company’s ability to
operate independently from UBI. The Correspondence also relayed Dr. Wang’s concerns that the preliminary prospectus did not fully
describe the disruption to the Company’s business that could result from the abovementioned dispute, including with respect to
intellectual property agreements among the Company and UBI and its affiliates. Various other claims have been made by Dr. Wang
regarding UBI’s corporate governance, the operations of the Company and the disclosures for our initial public offering, and the
Company cannot predict the course of this dispute. However, the Company has carefully considered Dr. Wang’s concerns and, based
on the disclosures included in the preliminary prospectus and in the final prospectus for our initial public offering and the Company’s
diligence efforts, the Company remains confident in the appropriateness and accuracy of its disclosures.
We will rely on contract manufacturers for the manufacture of raw materials for our research programs,
pre-clinical studies and clinical trials and we do not have long-term contracts with many of these parties. This reliance on contract
manufacturers increases the risk that we will not have sufficient quantities of such materials or product candidates that we may
develop and commercialize, or that such supply will not be available to us at an acceptable cost or on an acceptable timeline, which
could delay, prevent or impair our development or commercialization efforts.
We rely on contract manufacturers, including UBI and its affiliates, for the manufacture of raw materials for our clinical trials and pre-
clinical and clinical development. We do not have a long-term agreement with some of the contract manufacturers we currently use to
provide pre-clinical and clinical raw materials. Certain of these manufacturers are critical to our production, and the loss of these
manufacturers to one of our competitors or otherwise, or an inability to obtain quantities at an acceptable cost or quality, could delay,
prevent or impair our ability to timely conduct pre-clinical studies or clinical trials, and would materially adversely affect our
development and commercialization efforts.
We expect to continue to rely on contract manufacturers for the commercial supply of any of our product candidates for which we obtain
marketing approval, if any. We may be unable to maintain or establish long-term agreements with contract manufacturers or to do so on
acceptable terms. Even if we are able to establish agreements with contract manufacturers, reliance on contract manufacturers entails
additional risks, including:
• the failure of the contract manufacturer to manufacture our product candidates according to our schedule, or at all, including
if our contract manufacturers give greater priority to the supply of other products over our product candidates or otherwise
do not satisfactorily perform according to the terms of the agreements between us and them;
• the reduction or termination of production or deliveries by suppliers, or the raising of prices or renegotiation of terms;
• the termination or nonrenewal of arrangements or agreements by our contract manufacturers at a time that is costly or
inconvenient for us;
• the breach by the contract manufacturers of our agreements with them;
• the failure of contract manufacturers to comply with applicable regulatory requirements;
• the failure of the contract manufacturer to manufacture our product candidates according to our specifications;
• the mislabeling of clinical supplies, potentially resulting in the wrong dose amounts being supplied or active drug or
placebo not being properly identified;
63
• clinical supplies not being delivered to clinical sites on time, leading to clinical trial interruptions, or of drug supplies not
being distributed to commercial vendors in a timely manner, resulting in lost sales; and
• the misappropriation or unauthorized disclosure of our intellectual property or other proprietary information, including our
trade secrets and know-how.
We do not have complete control over all aspects of the manufacturing process of, and are dependent on, our contract manufacturing
partners for compliance with cGMP regulations for manufacturing both custom components and finished products. Contract
manufacturers may not be able to comply with cGMP regulations or similar regulatory requirements outside of the United States. If our
contract manufacturers cannot successfully manufacture material that conforms to our specifications and the strict regulatory
requirements of applicable regulatory authorities, they will not be able to secure and/or maintain authorization for their manufacturing
facilities. In addition, we do not have full control over the ability of our contract manufacturers to maintain adequate quality control,
quality assurance and qualified personnel. Further, our manufacturing partners may be unable to successfully increase the manufacturing
capacity for any of our product candidates in a timely or cost-effective manner, or at all, and quality issues may arise during any such
scale-up activities. If regulatory authorities do not authorize these facilities for the manufacture of our product candidates or if they
withdraw any such authorization in the future, we may need to find alternative manufacturing facilities, which would significantly
impact our ability to develop, obtain marketing approval for or market our product candidates, if approved. Our failure, or the failure of
our contract manufacturers, to comply with applicable regulations could result in sanctions being imposed on us, including fines,
injunctions, civil penalties, delays, suspension or withdrawal of approvals, license revocation, seizures or recalls of product candidates
or drugs, operating restrictions and criminal prosecutions, any of which could significantly and adversely affect supplies of our product
candidates or drugs and harm our business and results of operations.
We depend on strategic partnerships, collaborations and license agreements in connection with the research, development and
commercialization of our Vaxxine Platform and product candidates. If our existing or future partners, collaborators or licensees do
not perform as expected, if we fail to maintain any of these strategic partnerships, collaborations or license agreements, or if they
are not successful, our ability to commercialize our product candidates successfully and to generate revenues may be materially
adversely affected.
We have established and intend to continue to establish strategic partnerships, collaborations, licensing agreements, or other
arrangements with third parties. For our research, development and commercialization activities, we have depended, and will continue
to depend, on our partners to design and conduct their own clinical studies. As a result, these activities may not be able to be conducted
in the manner or on the time schedule we currently contemplate, which may negatively impact our business operations. While we have
certain contractual rights to information about pre-clinical and clinical developments and results under certain of our collaboration and
license agreements, including our agreements with UBIA and Aurobindo, we cannot be certain that clinical trials conducted in
connection with such collaboration programs will be conducted in a manner consistent with the best interests of our business. In addition,
if any of our partners, collaborators or licensees withdraw support for these programs or proposed products or otherwise impair their
development, our business could be negatively affected. Also, our inability to find a partner for any of our product candidates may result
in our termination of that specific product candidate program or evaluation of a product candidate in a particular indication. Because of
contractual restraints and the limited number of contract manufacturers with the expertise, required regulatory approvals and facilities
to manufacture our product candidates on a commercial scale, replacement of a contract manufacturer may be expensive and time-
consuming and may cause interruptions in the production of our product candidates, which could delay our clinical trials or interrupt
our potential future commercial sales. Even if we find or establish a strategic partner, collaborator or licensee for one or more of our
product candidates, there is no assurance that upon the approval of one or more of such product candidates that such product candidates
will be successfully commercialized.
Furthermore, our licenses and collaboration agreements impose, and any future agreement we enter into may also impose, restrictions
on our ability to license certain of our intellectual property to third parties or to develop or commercialize certain product candidates or
technologies ourselves.
In the future, we may enter into additional collaborations or license agreements to fund our development programs or to gain access to
sales, marketing or distribution capabilities of other parties. While certain of our existing collaboration and license agreements, including
our agreements with Aurobindo, impose development or commercialization obligations on our collaborators or licensees, we cannot be
certain that our collaboration partners will allocate sufficient resources or attention to our collaboration programs, that they will progress
our collaboration programs consistent with the best interests of our business or that they will otherwise meet their obligations under
these agreements in a timely manner or at all. Our existing collaborations and licenses, and any future collaborations and licenses we
enter into, therefore may pose a number of risks, including the following:
• collaborators or licensees may have significant discretion in determining the efforts and resources that they will apply to
developing or commercializing our product candidates, and they may not sufficiently fund the development or
commercialization of a product candidate;
64
• collaborators and licensees may not perform their obligations as expected by us or by health authorities, such as the FDA,
the TFDA or comparable foreign regulatory authorities;
• collaborators and licensees may dissolve, merge, be bought or may otherwise become unwilling to fulfill the initial terms
of the collaboration with us, or we may be unwilling to continue our arrangement following such an occurrence;
• collaborators and licensees may fail to perform their obligations under their agreements or may be slow in performing their
obligations;
• collaborations and licensees may be terminated for the convenience of the collaborator or licensee and, if terminated, we
could be required to raise additional capital to pursue further development or commercialization of the applicable product
candidates;
• collaborators and licensees may not pursue commercialization of any product candidates that achieve regulatory approval
or may elect not to continue or renew development or commercialization programs based on clinical trial results, changes
in the collaborators’ or licensees’ strategic focus or available funding, or external factors, such as an acquisition, that divert
resources or create competing priorities, or due to the actual or perceived competitive situation in a specific indication;
• collaborators and licensees may delay clinical trials, stop a clinical trial or abandon a product candidate, repeat or conduct
additional clinical trials or may require a new formulation of a product candidate for clinical testing;
• collaborators and licensees could independently develop, or develop with third parties, products that compete directly or
indirectly with our products or product candidates if the collaborators believe that competitive products are more likely to
be successfully developed or can be commercialized under terms that are more economically attractive than ours;
• product candidates discovered in collaboration with us may be viewed by our collaborators as competitive with their own
product candidates or products, which may cause collaborators to cease to devote resources to the commercialization of
our product candidates;
• disagreements with collaborators or licensees, including disagreements over proprietary rights, contract interpretation and
breach of contract claims, payment obligations or the preferred course of development, might cause delays or termination
of the research, development or commercialization of products or product candidates, might lead to additional
responsibilities, including financial obligations for us with respect to products or product candidates, or delays or
withholding of payments due to us or might result in litigation or arbitration, any of which would be time- consuming and
expensive, and could limit our ability to execute on our strategies and delay or prevent our ability to devote resources to
other product candidates;
• collaborators or licensees may not properly obtain, maintain, enforce or defend our intellectual property or may use our
proprietary information in such a way that could jeopardize or invalidate our intellectual property or proprietary
information or expose us to potential litigation; and
• collaborators may infringe, misappropriate or otherwise violate the intellectual property of third parties, which may expose
us to litigation and potential liability.
If our collaborations and licenses related to the research, development and commercialization of product candidates do not result in the
successful development and commercialization of our product candidates, or if one of our collaborators or licensees terminates its
agreement with us, we may not receive any future research funding or milestone or royalty payments under the collaboration or license,
and we may be unable to continue the development and commercialization of the product candidate. Further, even if our collaborations
and licenses do result in successful development and commercialization of products, if one of our collaborators breaches its obligations
under its agreement with us or enters bankruptcy or insolvency, there may be a material delay in our receipt of payments under such
agreements, or we may never receive such payments. If we do not receive the payments we expect under these agreements, our own
development and commercialization activities could be delayed or prevented altogether, and we may need to secure additional resources
to develop our proprietary product candidates. Moreover, maintaining our relationships with our collaborators and licensees may divert
significant time and effort of our scientific staff and management team, which may harm our ability to effectively allocate our resources
to multiple internal and other projects. All of the risks relating to product development, regulatory approval and commercialization
described in this report also apply to the activities of our collaborators and licensees.
Additionally, subject to its contractual obligations to us, if one of our collaborators or licensors is involved in a business combination,
merger, acquisition or other similar transaction, the collaborator or licensor might deprioritize or terminate the development or
commercialization of any product candidate licensed to it by us. If one of our collaborators or licensors terminates its agreement with
us, we may be unable to attract new collaborators in a timely manner or at all, which may delay or prevent our ability to develop or
commercialize one or more of our product candidates.
65
We rely on third parties to conduct our pre-clinical studies and clinical trials and perform other tasks for us. If these third parties do
not successfully carry out their contractual duties, meet expected deadlines, or comply with legal and regulatory requirements, we
may not be able to obtain regulatory approval for or commercialize our product candidates and our business could be substantially
harmed.
We have relied upon and plan to continue to rely upon CROs to execute certain of our pre-clinical and clinical trials, and to monitor and
manage data for our ongoing pre-clinical and clinical programs and to provide us with significant data and other information related to
our projects, pre-clinical studies and clinical trials. If such third parties provide inaccurate, misleading or incomplete data, our business,
financial condition and results of operations and prospects could be materially adversely affected. We have control over limited aspects
of our CROs’ activities; nevertheless, we are responsible for, and our reliance on CROs does not relieve us of our responsibilities for,
ensuring that each of our trials is conducted in accordance with the applicable protocol, legal, regulatory, scientific and ethical standards.
We and our CROs and other vendors are required to comply with cGMP, GCP, Good Laboratory Practice (“GLP”) and other laws,
regulations and guidelines enforced by applicable regulatory authorities for all of our product candidates during both pre-clinical and
clinical development. Regulatory authorities enforce these regulations through periodic inspections of study sponsors, principal
investigators, trial sites and other contractors. If we or any of our CROs or vendors fail to comply with applicable regulations, the data
generated in our pre-clinical and clinical trials may be deemed unreliable and regulatory authorities may require us to perform additional
pre-clinical and clinical trials before approving our marketing applications. We cannot assure you that upon inspection by a given
regulatory authority, such regulatory authority will determine that all of our clinical trials comply with cGCP regulations or other
applicable laws and regulations. Our failure to comply with applicable laws and regulations may require us to repeat clinical trials, which
would delay the regulatory approval process and require significant additional expenditures, which we may be unable to meet.
If any of our relationships with these CROs terminates, we may not be able to enter into arrangements with alternative CROs or do so
on commercially reasonable terms or in a timely manner. We would also incur additional costs and delays while engaging a new CRO,
which we may not be able to engage on commercially reasonable terms or at all. In addition, our CROs are not our employees, and
except for remedies available to us under our agreements with such CROs, we cannot control whether or not they devote sufficient time
and resources to our ongoing pre-clinical and clinical programs. If CROs do not successfully carry out their contractual duties or
obligations, meet expected deadlines, conduct our studies in accordance with regulatory requirements or our stated study plans and
protocols, if they need to be replaced or if the quality or accuracy of the data they obtain is compromised due to the failure to adhere to
our protocols, regulatory requirements, or for other reasons, our clinical trials may be extended, delayed or terminated and we may not
be able to obtain regulatory approval for or successfully commercialize our product candidates in a timely manner or at all. For example,
due to an error by the CRO responsible for administering blinded placebo and active doses to trial subjects, which reduced the confidence
of subsequently collected data, we decided to discontinue a Phase 2a LTE trial for UB-311. In that case, however, we determined that
we had collected sufficient data on UB-311’s tolerability and immunogenicity. CROs or any of our other collaborators may also generate
higher costs than anticipated. As a result, our results of operations and the commercial prospects for our product candidates could be
harmed, our costs could increase and our ability to generate revenue could be delayed.
Though we carefully manage our relationships with our CROs, there can be no assurance that we will not encounter challenges or delays
in the future or that these delays or challenges will not have a material adverse impact on our business, financial condition, results of
operations and prospects.
We do not have multiple sources of commercial supply for some of the components used in our product candidates, nor long-term
supply contracts with our existing suppliers, and certain of our suppliers are critical to our production. If we were to lose a critical
supplier or if an approved supplier experiences delays due to raw material constraints, it could have a material adverse effect on our
ability to complete the development of our product candidates. If we obtain regulatory approval for any of our product candidates,
we cannot guarantee that our suppliers will be able to meet our increased demands for supply.
We do not have multiple sources of commercial supply for each of the components used in the manufacturing of our product candidates,
nor do we have long-term supply agreements with all of our component suppliers. Manufacturing suppliers are subject to cGMP quality
and regulatory requirements, covering manufacturing, testing, quality control and record keeping relating to our product candidates and
are subject to ongoing inspections by applicable regulatory authorities. Manufacturing suppliers are also subject to licensing
requirements as well as local, state and federal regulations and regulations in foreign jurisdictions in which they operate. Failure by any
of our suppliers to comply with all applicable regulations and requirements may result in long delays and interruptions in supply.
The number of suppliers of the raw material components of our product candidates is limited. In the event it is necessary or desirable to
acquire supplies from alternative suppliers, we might not be able to obtain such supply on commercially reasonable terms, if at all. It
could also require significant time and expense to redesign our manufacturing processes to work with another company and redesign of
processes can trigger the need for conducting additional studies such as comparability or bridging studies. Additionally, certain of our
suppliers are critical to our production, and the loss of these suppliers to one of our competitors or otherwise would materially adversely
affect our development and commercialization efforts. Further, if such critical suppliers experience delays in their ability to supply of
components due to limited availability of raw materials or other difficulties which may be beyond our or their control, our manufacturing
efforts may be materially adversely affected.
66
As part of any marketing approval, regulatory authorities conduct inspections that must be successful prior to the approval of a product
candidate. Failure of manufacturing suppliers to successfully complete these regulatory inspections will result in delays. If supply from
the approved supplier is interrupted, an alternative vendor would need to be qualified through an NDA amendment or supplement, and
this could result in significant disruption in commercial supply. Regulatory authorities may also require additional studies if a new
supplier is relied upon for commercial production. Switching vendors may involve substantial costs and is likely to result in a delay in
our desired clinical and commercial timelines.
If we are unable to obtain the supplies we need at a reasonable price or on a timely basis, it could have a material adverse effect on our
ability to complete the development of our product candidates or, if we obtain regulatory approval for our product candidates, to
commercialize them.
Risks Related to Our Intellectual Property Rights
We depend on intellectual property licensed from UBI and its affiliates, the termination of which could result in the loss of significant
rights, which would harm our business.
We are dependent on technology, patents, know-how and proprietary information, both our own and those licensed from UBI and its
affiliates. We entered into the Platform License Agreement in August 2021 pursuant to which we obtained a worldwide, sublicensable
(subject to certain conditions), perpetual, fully paid-up, royalty-free (i) exclusive license (even as to the Licensors) under all patents
owned or otherwise controlled by the Licensors or their affiliates existing as of the effective date of the Platform License Agreement,
(ii) exclusive license (except as to the Licensors) under all patents owned or otherwise controlled by the Licensors or their affiliates
arising after the effective date during the term of the Platform License Agreement, and (iii) non-exclusive license under all know-how
owned or otherwise controlled by the Licensors or their affiliates existing as of the effective date or arising during the term of the
Platform License Agreement, in each of the foregoing cases, to research, develop, make, have made, utilize, import, export, market,
distribute, offer for sale, sell, have sold, commercialize or otherwise exploit peptide-based vaccines in the field of all human prophylactic
and therapeutic uses, except for such vaccines related to human immunodeficiency virus, herpes simplex virus and Immunoglobulin E.
The patents licensed to us under the Platform License Agreement include patents directed to a CpG delivery system, artificial T helper
cell epitopes and certain designer peptides and proteins, each of which is utilized in UB-612. Any termination of these licenses will
result in the loss of significant rights and will restrict our ability to develop and commercialize our product candidates.
Our reliance on in-licensed intellectual property and technology results in a number of risks to the development and
commercialization of our product candidates, including the loss of such rights, our licensors’ inability or refusal to enforce or defend
such rights, and the requirement to pay royalties, milestones, and other amounts.
Agreements under which we license intellectual property or technology to or from UBI, its affiliates and from other third parties may
be complex, and certain provisions in such agreements may be susceptible to multiple interpretations. The resolution of any contract
interpretation disagreement that may arise could narrow what we believe to be the scope of our rights to the relevant intellectual property
or technology or increase what we believe to be our financial or other obligations under the relevant agreement, either of which could
have a material adverse effect on our business, financial condition, results of operations and prospects. Moreover, if disputes over
intellectual property that we have licensed prevent or impair our ability to maintain our current licensing arrangements on commercially
acceptable terms, we may be unable to successfully develop and commercialize the affected product candidates. Our business may also
suffer if any current or future licensors fail to abide by the terms of the license, if the licensors fail to enforce licensed patents against
infringing third parties, if the licensed patents or other rights are found to be invalid or unenforceable, or if we are unable to enter into
necessary licenses on acceptable terms or at all. In the event of a bankruptcy by one of our licensors, our intellectual property licenses
could also be affected. For example, while the U.S. Bankruptcy Code allows a licensee to retain its rights under its license
notwithstanding the bankrupt licensor’s rejection of such license, such protections may not be available to us in the event a licensor
declares bankruptcy in a foreign jurisdiction. Our licensors may also own or control intellectual property that has not been licensed to
us and, as a result, we may be subject to claims, regardless of their merit, that we are infringing or otherwise violating the licensors’
rights.
Furthermore, while we cannot currently determine the amount of the royalty obligations we would be required to pay on sales of future
products, if any, the amounts may be significant. The amount of our future royalty obligations will depend on the technology and
intellectual property we use in products that we successfully develop and commercialize, if any. Therefore, even if we successfully
develop and commercialize products, we may be unable to achieve or maintain profitability.
We believe the growth of our business may depend in part on our ability to acquire or in-license additional intellectual property rights,
including to advance our research or allow commercialization of our product candidates. If we are unable to obtain additional licenses
we need to develop and commercialize our product candidates, or if we obtain such licenses and they are terminated, we may be required
to expend considerable time and resources in an attempt to develop or license replacement technology. We may also need to cease use
of the compositions or methods covered by such third-party intellectual property rights, and our ability to license or develop alternative
67
approaches that do not infringe on such intellectual property rights may entail significant additional costs and development delays, even
if we were able to develop or license such alternatives, which may not be feasible.
The licensing and acquisition of third-party intellectual property rights is a competitive practice, and companies that may be more
established, or have greater resources than we do, may also be pursuing strategies to license or acquire third-party intellectual property
rights that we may consider necessary or attractive in order to commercialize our product candidates. More established companies may
have a competitive advantage over us due to their larger size and cash resources or greater clinical development and commercialization
capabilities. There can be no assurance that we will be able to successfully complete such negotiations and ultimately acquire the rights
to the intellectual property surrounding the additional product candidates that we may seek to acquire. Even if we are able to obtain a
license under such intellectual property rights, any such license may be non-exclusive, which may allow our competitors’ access to the
same technologies licensed to us.
Licensing of intellectual property is of critical importance to our business and involves complex legal, business and scientific issues and
is complicated by the rapid pace of scientific discovery in our industry. Disputes may also arise between us and our licensors regarding
intellectual property subject to a license agreement, including those relating to:
• the scope of rights granted under the license agreement and other interpretation-related issues;
• whether and the extent to which our technology and processes infringe on intellectual property of the licensor that is not
subject to the license agreement;
• our right to sublicense patent and other rights to third parties under collaborative development relationships;
• our compliance with reporting, financial or other obligations under the license agreement;
• the amount and timing of payments owed under license agreements; and
• the allocation of ownership of inventions and know-how resulting from the creation or use of intellectual property by our
licensors and by us and our partners.
We may also not be able to fully protect our licensed intellectual property rights or maintain our licenses under our licensing
arrangements. Our existing and future licensors could retain the right to prosecute, maintain, defend and enforce the intellectual property
rights licensed to us, in which case we would depend on the ability and will of our licensors to do so. Our licensors may take different
approaches to prosecuting patents than we would, and it is possible our inability to control such activities could harm our business.
Furthermore, our licensors may determine not to pursue litigation against other companies or may pursue such litigation less aggressively
than we would. We may also rely upon obtaining the consent of our licensors to settle legal claims. If our licensors do not adequately
protect or enforce such licensed intellectual property, competitors may be able to use such intellectual property and erode or negate any
competitive advantage we may have, which could materially harm our business, negatively affect our position in the marketplace, limit
our ability to commercialize our products and product candidates and delay or render impossible our achievement of profitability.
If disputes over intellectual property that we have licensed prevent or impair our ability to maintain our current licensing arrangements
on acceptable terms or at all, we may be unable to successfully develop and commercialize the affected product candidates. We are
generally also subject to all of the same risks with respect to protection of intellectual property that we license as we are for intellectual
property that we own, which are described below. If we or our licensors fail to adequately protect this intellectual property, our ability
to develop or commercialize our products could suffer.
Furthermore, our existing license agreements may impose, and we expect that future license agreements will impose, various diligence,
milestone payment, royalty and other obligations on us and if our licensors, licensees or collaborators conclude that we have failed to
comply with our obligations under these agreements, including due to the impact of the COVID-19 pandemic on our business operations
or our use of the intellectual property licensed to us in a manner the licensor believe is unauthorized, or we are subject to a bankruptcy,
we may be required to pay damages and the licensor may have the right to terminate the license. Any of the foregoing could result in us
being unable to develop, manufacture and sell products that are covered by the licensed technology or enable a competitor to gain access
to the licensed technology. We might not have the necessary rights or the financial resources to develop, manufacture or market our
current or future product candidates without the rights granted under our licenses, and the loss of sales or potential sales in such product
candidates could have a material adverse effect on our business, financial condition, results of operations and prospects.
Moreover, our rights to our in-licensed patents and patent applications may depend, in part, on inter- institutional or other operating
agreements between the joint owners of such in-licensed patents and patent applications or the owners of such in-licensed patents and
patent applications and their affiliates. We may not be aware of each party’s rights and obligations under such inter-institutional or other
operating agreements and, as such, the ownership of our in-licensed patents and patent applications may be uncertain. If one or more of
these owners breaches such inter-institutional or other operating agreements, our rights to such in-licensed patents and patent
applications may be adversely affected. In addition, the development of certain of our product candidates may be funded by grants that
68
impose certain pricing limitations on such product candidates and limit our ability to commercialize such product candidates and to
achieve or maintain profitability. Any of the foregoing could have a material adverse effect on our competitive position, business,
financial conditions, results of operations and prospects.
We may be required to license or obtain rights to use third party intellectual property or technology in connection with the
development and commercialization of our product candidates.
We may not be aware of all technologies developed or under development by third parties, and other pharmaceutical companies or
academic institutions may also have filed or may be planning to file patent applications potentially relevant to our business and product
candidates. The technologies used in connection with the formulations of our product candidates may also be covered by intellectual
property rights held by others. From time to time, in order to avoid infringing these third-party patents, we may be required to license
technology from additional third parties to further develop, manufacture, use, sell or commercialize our product candidates, or that we
otherwise deem necessary for our business operations. We may fail to obtain any such licenses at a reasonable cost or on reasonable
terms, if at all, and as a result we may be unable to develop or commercialize the affected product candidates, and we may have to
abandon development of the relevant research programs or product candidates, which would harm our business.
If we are unable to obtain and maintain intellectual property protection for our products or product candidates, or if the duration or
scope of our intellectual property protection is not sufficiently broad, our ability to commercialize our product candidates successfully
and to compete effectively may be materially adversely affected.
Our success depends on our ability to obtain and maintain patent and other intellectual property protection in the United States and other
countries with respect to our current and future proprietary product candidates. We rely upon a combination of patents, trade secret
protection and confidentiality agreements to protect the intellectual property related to our technology, manufacturing processes,
products and product candidates. We, UBI and our other collaborators and licensors have primarily sought to protect our proprietary
positions by filing patent applications in the United States and abroad related to our proprietary technology, manufacturing processes
and product candidates that are important to our business. Despite our or our third party collaborators’ or licensors’ efforts to protect
these proprietary rights, unauthorized parties may be able to obtain and use information that we regard as proprietary. Third parties may
also seek to invalidate our patents or those of our licensors. If we are unable to obtain rights to required third-party intellectual property
rights or maintain the existing intellectual property rights we have, we may be required to expend significant time and resources to
redesign our technology, product candidates or the methods for manufacturing them or to develop or license replacement technology,
all of which may not be feasible on a technical or commercial basis. We could also lose expected revenues under license agreements we
maintain with third parties. If we are unable to obtain or maintain our intellectual property, we may be unable to develop or
commercialize the affected technology and product candidates or could lose revenue, either of which could harm our business, financial
condition, results of operations and prospects significantly.
The patent prosecution process is expensive and time-consuming, and we may not be able to file and prosecute all necessary or desirable
patent applications at a reasonable cost or in a timely manner or in all jurisdictions where protection may be commercially advantageous.
It is also possible that we may fail to identify patentable aspects of our research and development output before it is too late to obtain
patent protection.
In addition, we, UBI or our other collaborators and licensors, may only pursue, obtain or maintain patent protection in a limited number
of countries. Because patent applications in the United States, Europe and many other foreign jurisdictions are typically not published
until 18 months after filing, or in some cases not at all, and because publications of discoveries in scientific literature lag behind actual
discoveries, we cannot be certain that we or our licensors were the first to make the inventions claimed in any of our owned or any in-
licensed issued patents or pending patent applications, or that we or our licensors were the first to file for protection of the inventions
set forth in our patents or patent applications. As a result, we may not be able to obtain or maintain protection for certain inventions, and
there can be no assurance that the patents we file, or those that are issued, will not be vulnerable to claims of invalidity or
unenforceability.
Even if patents do successfully issue, our owned or in-licensed patents may not adequately protect our intellectual property, provide
exclusivity for our products or product candidates, prevent others from designing around our claims or otherwise provide us with a
competitive advantage. Competitors may use our technologies in jurisdictions where we have not obtained or are unable to adequately
enforce patent protection to develop their own products and, further, may export otherwise infringing products to territories where we
have patent protection, but enforcement is not as strong as that in the United States and Europe. These products may compete with our
products, and our patents or other intellectual property rights may not be effective or sufficient to prevent them from competing with us.
We also cannot offer any assurances about which, if any, patents will issue, the breadth of any such patents or whether any issued patents
will be found invalid or unenforceable or will be threatened by third parties. In addition, third parties may challenge the validity,
enforceability, ownership, inventorship or scope of any of our patents. Any successful challenge to any of our patents or our in-licensed
patents could deprive us of rights necessary for the successful commercialization of any product candidate that we may develop and
could impair or eliminate our ability to collect future revenues and royalties with respect to such products or product candidates. If any
of our patent applications with respect to our product candidates fail to issue as patents, if their breadth or strength of protection is
69
narrowed or threatened, or if they fail to provide meaningful exclusivity or competitive position, it could dissuade companies from
collaborating with us or otherwise adversely affect our competitive position.
In addition, patents have a limited lifespan. In the United States, for example, the natural expiration of a patent is generally 20 years
after its effective filing date. Various extensions may be available, however, the life of a patent and the protection it affords is limited.
Given the amount of time required for the development, testing, regulatory review and approval of new product candidates, our patents
protecting such candidates might expire before or shortly after such candidates are commercialized. If we encounter delays in obtaining
regulatory approvals, the period of time during which we could market a product under patent protection could be further reduced. Even
if patents covering our product candidates are obtained, once such patents expire, or if such patents are waived or suspended, we may
be vulnerable to competition from similar or biosimilar products. For example, in 2021, the Biden administration indicated its support
for a proposal at the World Trade Organization to waive patent rights with respect to COVID-19 vaccines. The current proposal is for a
temporary waiver of intellectual property rights that cover COVID-19 vaccines, however, the ultimate timing and scope of the waiver,
if approved, is unknown. The scope and timing of such waiver will likely be subject to extensive negotiations given the complexity of
the matter, which may result in prolonged uncertainty and therefore could adversely affect our business. Any expiration, waiver or
suspension of our patent or other intellectual property protection by the U.S. or other foreign governments could lead to the launch of a
similar or biosimilar version of one of our products and would likely result in an immediate and substantial reduction in the demand for
our product, which could have a material adverse effect on our business, financial condition, results of operations and prospects.
We may not be able to protect or enforce our intellectual property rights in all jurisdictions, and we cannot guarantee that the patent
rights we have will prevent others from competing with us.
The patent position of pharmaceutical companies is generally uncertain because it involves complex legal, scientific and factual
considerations for which legal principles remain unsolved. The standards applied by the United States Patent and Trademark Office
(“USPTO”) and foreign patent offices in granting patents are not always applied uniformly or predictably, and can change. Additionally,
the laws of some foreign countries do not protect intellectual property rights to the same extent as the laws of the United States, and
many companies have encountered significant challenges in protecting and defending such rights in foreign jurisdictions. We may face
similar challenges. The legal systems of certain countries, particularly certain developing countries, do not favor the enforcement of
patents and other intellectual property rights, particularly those relating to biotechnology, which could make it difficult for us to stop
the infringement, misappropriation or other violation of our patents or other intellectual property, including the unauthorized
reproduction of our manufacturing or other know-how or the marketing of competing products in violation of our intellectual property
rights generally. Any of these outcomes could impair our ability to prevent competition from third parties, which may have a material
adverse effect on our business, financial condition, results of operations and prospects.
Further, the existence of issued patents does not guarantee our right to practice the patented technology or commercialize a patented
product candidate. Third parties may design around our patents, or have or obtain rights to patents which they may use to prevent or
attempt to prevent us from practicing our patented technology or commercializing any of our patented product candidates. As a result,
we could be prevented from selling our products unless we were able to obtain a license under such third-party patents, which may not
be available on commercially reasonable terms or at all. In addition, third parties may seek approval to market their own products similar
to or otherwise competitive with our products and such products may not violate our patent rights. We may also need to assert our
patents against third parties, including by filing lawsuits alleging patent infringement. In any such proceeding, a third party may assert,
and a court or agency of competent jurisdiction may find, our asserted patents to be invalid or unenforceable. Any of the foregoing could
have a material adverse effect on our business, financial condition, results of operations and prospects.
There is a substantial amount of intellectual property litigation in the biotechnology and pharmaceutical industries, and we may become
party to, or threatened with, litigation or other adversarial proceedings regarding intellectual property rights. Proceedings to defend or
enforce our patent rights, whether or not successful and whether or not meritorious, could result in substantial costs and divert our efforts
and attention from other aspects of our business, could put our patents at risk of being invalidated or held unenforceable, or interpreted
more narrowly. There can be no assurance that we will have sufficient financial or other resources to file and pursue such claims, which
often last for years before they are concluded. Some claimants may have substantially greater resources than we do and may be able to
sustain the costs of complex intellectual property litigation to a greater degree and for longer periods of time than we could. In addition,
patent holding companies that focus solely on extracting royalties and settlements by enforcing patent rights may target us, especially
as we gain greater visibility and market exposure as a public company. In addition, our enforcement of our patent rights could provoke
third parties to assert counterclaims against us. Third parties also may raise similar claims before administrative bodies in the United
States or abroad, even outside the context of litigation. We may not prevail in any lawsuits or administrative proceedings that we initiate
and the damages or other remedies awarded, if any, may not be commercially meaningful. If a third party were to prevail on a legal
assertion of invalidity or unenforceability, we could lose part or all of the patent protection on one or more of our product candidates,
which could result in our competitors and other third parties using our technology to compete with us. An adverse outcome in a litigation
or administrative proceeding involving our patents could limit our ability to assert our patents against competitors, affect our ability to
receive royalties or other licensing consideration from our licensees, and may curtail or preclude our ability to exclude third parties from
making, using and selling similar or competitive products. Any of these occurrences could have a material adverse effect on our business,
financial condition, results of operations and prospects. Accordingly, our efforts to enforce our intellectual property rights around the
world may be inadequate to obtain a significant commercial advantage from the intellectual property that we develop, acquire or license.
70
Many countries, including certain countries in Asia, have compulsory licensing laws under which a patent owner may be compelled to
grant licenses to third parties. In addition, many countries limit the enforceability of patents against government agencies or government
contractors. In these countries, the patent owner may have limited remedies, which could materially diminish the value of such patent.
If we or any of our licensors is forced to grant a license to third parties with respect to any patents relevant to our business, our competitive
position may be impaired, and our business, financial condition, results of operations and prospects may be adversely affected. Our
owned and in-licensed patents may be subject to a reservation of rights by one or more third parties. For example, the research resulting
in certain of our licensors’ patents and technology, including patents and technology relating to UB-612, was funded in part by the
Taiwanese government. As a result, the Taiwanese government may have certain rights to such patent rights and technology.
Furthermore, certain of our patents and technology, including patents and technology relating to UB-312, were funded in part by grants
from nonprofit third parties, including the MJFF. We are required to fulfill certain contractual obligations with respect to products
created using such grant funding, including certain reporting requirements. We also have submitted grant proposals relating to our UB-
612 product candidate. If these grant proposals are awarded, or if we receive funding from other nonprofit third parties in the future, we
may be required to fulfill other contractual obligations, such as publishing the results of our scientific studies, making certain products
available at an affordable price in a list of clearly defined low and lower-middle income countries and ensuring that certain products are
available in geographic regions where there has been an outbreak of an infectious disease at certain reduced economic rates.
If we or our licensors infringe, misappropriate, or otherwise violate intellectual property of third parties, we may face increased costs
or we may be unable to commercialize our product candidates.
Many of our current and former employees, consultants and independent contractors including our senior management, were previously
employed at universities or at other biotechnology or pharmaceutical companies, including some which may be competitors or potential
competitors. Although we try to ensure that our employees, consultants and independent contractors do not use the proprietary
information or know-how of others in their work for us, we may be subject to claims that we or these employees, consultants or
independent contractors have used or disclosed intellectual property, including trade secrets or other proprietary information, of such
individual’s current or former employers, or that patents and applications we have filed to protect inventions of these individuals, even
those related to one or more of our current or future product candidates, are rightfully owned by their former or concurrent employer. In
addition, while we typically require our employees, consultants and independent contractors who may be involved in the development
of intellectual property to execute agreements assigning such intellectual property to us, we may be unsuccessful in executing such an
agreement with each party who in fact develops intellectual property that we regard as our own, or such agreements may be breached
or alleged to be ineffective, and the assignment may not be self-executing, which may result in claims by or against us related to the
ownership of such intellectual property or may result in such intellectual property becoming assigned to third parties.
Third parties have, and may in the future have, U.S. and non-U.S. issued patents and pending patent applications relating to compounds,
methods of manufacturing compounds or methods of use for the treatment of the disease indications for which we are developing our
product candidates that may cover our product candidates. For example, we are aware of certain third-party U.S. and non-U.S. patents
and patent applications, including those of our competitors, that relate to anti-alpha synuclein binding molecules that may be construed
to cover the technology used in our anti-alpha synuclein vaccine product candidate. We are also aware of certain third-party U.S. and
non-U.S. patents and patent applications, including those of our competitors, that relate to coronavirus vaccines and treatments and
vaccines against other infectious diseases and we expect such third parties to have filed additional patent applications, which have not
yet been published and to file additional patent applications in the future.
In the event that any of these patent rights were asserted against us, we believe that we have defenses against any such action, including
that such patents would not be infringed by our product candidates and/or that such patents are not valid. However, if any such patent
rights were to be asserted against us and our defenses to such assertion were unsuccessful, unless we obtain a license to such patents,
we could be liable for damages, which could be significant and include treble damages and attorneys’ fees if we are found to willfully
infringe such patents. We could also be precluded from commercializing any product candidates that were ultimately held to infringe
such patents, any of which could have a material adverse effect on our business, financial condition, results of operations and prospects.
Uncertainties resulting from our participation in patent litigation or other proceedings could have a material adverse effect on our ability
to compete in the marketplace. Furthermore, because of the substantial amount of discovery required in certain jurisdictions in
connection with intellectual property litigation, there is a risk that some of our confidential information could be compromised by
disclosure during this type of litigation. There could also be public announcements of the results of hearings, motions or other interim
proceedings or developments. If securities analysts or investors perceive these results to be negative, the perceived value of our product
candidates or intellectual property could be diminished. Accordingly, the market price of our Class A common stock could decline.
Uncertainties resulting from the initiation and continuation of patent litigation or other proceedings could have a material adverse effect
on our business, financial condition, results of operations and prospects.
71
Changes to the patent law in the United States and other jurisdictions could increase the uncertainties and costs surrounding the
prosecution of our patent applications and the enforcement or defense of our issued patents, thereby impairing our ability to protect
our technologies and product candidates.
As is the case with other biopharmaceutical companies, our success is heavily dependent on intellectual property, particularly patents.
Obtaining and enforcing patents in the biopharmaceutical industry involves both technological and legal complexity and is therefore
costly, time-consuming and inherently uncertain. Changes in either the patent laws or interpretation of the patent laws in the United
States or abroad could increase the uncertainties and costs surrounding the prosecution of patent applications and the enforcement or
defense of issued patents. For example, recent U.S. Supreme Court rulings have narrowed the scope of patent protection available in
certain circumstances and weakened the rights of patent owners in certain situations. Specifically, these decisions stand for the
proposition that patent claims that recite laws of nature are not themselves patentable unless those patent claims have sufficient additional
features that provide practical assurance that the processes are genuine inventive applications of those laws. What constitutes a
“sufficient” additional feature is uncertain. Furthermore, in view of these decisions, since December 2014, the USPTO has published
and continues to publish revised guidelines for patent examiners to apply when examining process claims for patent eligibility. This
combination of events has created uncertainty with respect to the validity and enforceability of patents, even once they are obtained.
Depending on future actions by the U.S. Congress, the federal courts and the USPTO, the laws and regulations governing patents could
change in unpredictable ways. In addition, the complexity and uncertainty of European and Asian patent laws have also increased in
recent years. For example, in October 2020, China adopted amendments to its patent law (the “Amended PRC Patent Law”), which
became effective on June 1, 2021. The Amended PRC Patent Law contains both patent term extension and a mechanism for early
resolution of patent disputes. However, the provisions for patent term extension and an early resolution mechanism are unclear and
remain subject to the approval of implementing regulations that have yet to be finalized, leading to uncertainty about their scope and
implementation. Complying with these laws and regulations could have a material adverse effect on our existing patent portfolio and
our ability to protect and enforce our intellectual property in the future.
Obtaining and maintaining our patent protection, including patents licensed from third parties, depends on compliance with various
procedural, documentary, fee payment and other requirements imposed by governmental patent agencies, and our patent protection
could be reduced or eliminated for noncompliance with these requirements.
Periodic maintenance fees, renewal fees, annuity fees and various other governmental fees on patents and patent applications will be
due to be paid to the USPTO and various government patent agencies outside the United States over the lifetime of our patents and
patent applications and any patent rights we may own or license in the future. Additionally, the USPTO and various government patent
agencies outside the United States require compliance with a number of procedural, documentary, fee payment and other similar
provisions during the patent application process. In certain cases, an inadvertent lapse can be cured by payment of a late fee or by other
means in accordance with rules applicable to the particular jurisdiction. However, there are situations in which noncompliance can result
in abandonment or lapse of the patent or patent application, resulting in partial or complete loss of patent rights in the relevant
jurisdiction. For example, certain of our patents which include claims utilized in our UB-311 anti-Aβ vaccine product candidate recently
lapsed in certain European and Asian countries due to non-payment of fees. Noncompliance events that could result in abandonment or
lapse of a patent or patent application include failure to respond to official communications within prescribed time limits, non-payment
of fees and failure to properly legalize and submit formal documents. If we or our licensors fail to maintain the patents and patent
applications covering or otherwise protecting our technologies or our product candidates, our competitors may be able to enter the
market with similar or identical products or technology without infringing our patents, which could have a material adverse effect on
our business. In addition, to the extent that we have responsibility for taking any action related to the prosecution or maintenance of
patents or patent applications in-licensed from a third party, any failure on our part to maintain the in-licensed intellectual property could
jeopardize our rights under the relevant license and may have a material adverse effect on our business, financial condition, results of
operations and prospects.
If we do not obtain patent term extensions and data exclusivity for each of our product candidates, our business may be materially
harmed.
Depending upon the timing, duration and specifics of any FDA marketing approval in the United States of any product candidates we
may develop, one or more of our U.S. patents may be eligible for limited patent term extension under the Drug Price Competition and
Patent Term Restoration Action of 1984 (“Hatch-Waxman Amendments”). The Hatch-Waxman Amendments permit a patent extension
term of up to five years as compensation for patent term lost during the FDA regulatory review process. A patent term extension cannot
extend the remaining term of a patent beyond a total of 14 years from the date of product approval, only one patent applicable to an
approved drug may be extended and only those claims covering the approved drug, a method for using it, or a method for manufacturing
it may be extended. The length of the patent term extension is typically calculated as one half of the clinical trial period plus the entire
period of time during the review of the NDA or BLA by the FDA, minus any time of delay by the applicant during these periods. We
might not be granted a patent term extension at all, because of, for example, failure to apply within the applicable period, failure to apply
prior to the expiration of relevant patents or otherwise failure to satisfy any of the numerous applicable requirements.
In the European Union, a maximum of five and a half years of supplementary protection can be achieved for an active ingredient or
combinations of active ingredients of a medicinal product protected by a basic patent, if a valid marketing authorization exists (which
72
must be the first authorization to place the product on the market as a medicinal product) and if the product has not already been the
subject of supplementary protection. Although all countries in Europe must provide supplementary protection certificates, there is no
unified legislation among European countries and so supplementary protection certificates must be applied for and granted on a country-
by-country basis. This can lead to a substantial cost to apply for and receive these certificates, which may vary among countries or not
be provided at all. Further, we may not receive an extension because of, for example, failing to exercise due diligence during the testing
phase or regulatory review process, failing to apply within applicable deadlines, failing to apply prior to expiration of relevant patents,
or otherwise failing to satisfy applicable requirements. Moreover, the length of the extension could be less than we request. If we are
unable to obtain patent term extension or if the term of any such extension is less than we request, our competitors may obtain approval
of competing products earlier than expected following our patent expiration, and our business, financial condition, results of operations
and prospects could be materially harmed.
If we are unable to protect the confidentiality of our proprietary information and trade secrets, the value of our technology and
products could be materially adversely affected.
In addition to patent protection, we also rely on trade secrets and confidentiality agreements to protect other proprietary information that
is not patentable or that we elect not to patent. To maintain the confidentiality of trade secrets and proprietary information, we enter into
confidentiality agreements with our employees, consultants, independent contractors, collaborators, contract manufacturers, CROs and
others upon the commencement of their relationships with us. These agreements require that all confidential information developed by
the individual or entity or made known to the individual or entity by us during the course of the individual’s or entity’s relationship with
us be kept confidential and not disclosed to third parties. Our agreements with employees as well as our personnel policies also generally
provide that any inventions conceived by the individual in the course of rendering services to us shall be our exclusive property or that
we may obtain full rights to such inventions at our election. However, we cannot guarantee that we have entered into such agreements
with each party that may have or has had access to our trade secrets or proprietary technology and processes and cannot guarantee that
individuals with whom we have these agreements will comply with their terms. In the event of unauthorized use or disclosure of our
trade secrets or proprietary information, these agreements, even if obtained, may not provide meaningful protection, particularly for our
trade secrets.
We may not have adequate remedies in the event of unauthorized use or disclosure of our proprietary information in the case of a breach
of any such agreements and our trade secrets and other proprietary information could be disclosed to third parties, including our
competitors. Many of our partners also collaborate with our competitors and other third parties. The disclosure of our trade secrets to
our competitors, or more broadly, would impair our competitive position and may materially harm our business, financial condition,
results of operations and prospects. Costly and time-consuming litigation could be necessary to enforce and determine the scope of our
proprietary rights, and failure to maintain trade secret protection could adversely affect our competitive business position. The
enforceability of confidentiality agreements may vary from jurisdiction to jurisdiction. Courts outside the United States are sometimes
less willing to protect proprietary information, technology and know-how. In addition, others may independently discover or develop
substantially equivalent or superior proprietary information and techniques, and the existence of our own trade secrets affords no
protection against such independent discovery.
If our trademarks and trade names are not adequately protected, we may not be able to build name recognition in our markets of
interest and our business, financial condition, results of operations and prospects may be adversely affected.
We rely on our trademarks for name recognition by potential partners and customers in our markets of interest. However, our trademarks
or trade names may be challenged, infringed, circumvented or declared generic or determined to be infringing on other marks. We may
not be able to protect our rights to these trademarks and trade names or may be forced to stop using these names or marks. During
trademark registration proceedings, we may receive rejections that we may be unable to overcome. In addition, in the USPTO and in
comparable agencies in many foreign jurisdictions, third parties are given an opportunity to oppose pending trademark applications and
to seek to cancel registered trademarks. Opposition or cancellation proceedings may be filed against our trademarks, and our trademarks
or trademark applications may not survive such proceedings. If we are unable to establish name recognition based on our trademarks
and trade names, we may not be able to compete effectively and our business, financial condition, results of operations and prospects
may be adversely affected.
Intellectual property rights do not necessarily address all potential threats.
The degree of future protection afforded by our proprietary and intellectual property rights is uncertain because such rights offer only
limited protection and may not adequately protect our rights or permit us to gain or keep our competitive advantage. For example:
• others may be able to develop products that are similar to, or better than, our product candidates in a way that is not covered
by the claims of the patents we license or may own currently or in the future;
• we, or our licensing partners or current or future collaborators, might not have been the first to make or file patent
applications for the inventions covered by issued patents or pending patent applications that we license or may own
currently or in the future;
73
• we may not have the financial or other resources necessary to enforce a patent infringement or other proprietary rights
violation action;
• we may choose not to file a patent for certain trade secrets or know-how, and a third party may subsequently file a patent
covering such intellectual property;
• our trade secrets or proprietary know-how may be unlawfully disclosed, thereby losing their trade secret or proprietary
status;
• our competitors or other third parties might conduct research and development activities in countries where we do not have
patent rights and then use the information learned from such activities to develop competitive products for sale in our
major commercial markets;
• it is possible that there are prior public disclosures that could invalidate our or our licensors’ patents;
• the patents of third parties or pending or future applications of third parties, if issued, may have an adverse effect on our
business;
• third parties could design around our patents, or independently develop trade secrets that provide them with an advantage
over us;
• any patents that we obtain may not provide us with any competitive advantages or may ultimately be found not to be owned
by us, or to be invalid or unenforceable; or
• we may not develop additional proprietary technologies that are patentable.
Should any of these events occur, they could significantly harm our business, financial conditions, results of operations and prospects.
Risks Related to Our Business and Industry
Even if we, or any current or future collaborators, are able to commercialize any product candidate that we or they develop, the
successful commercialization of our product candidates will depend in part on the extent to which governmental authorities, private
health insurers and other third-party payors provide coverage and adequate reimbursement levels and implement pricing policies
favorable for our product candidates. Failure to obtain or maintain coverage and adequate reimbursement for our product
candidates, if approved, could limit our ability to market those products and decrease our ability to generate revenue.
The healthcare industry is acutely focused on cost containment, both in the United States and elsewhere. Government authorities and
third-party payors have attempted to control costs by limiting coverage and the amount of reimbursement. The insurance coverage and
reimbursement status of newly approved products is uncertain and failure to obtain or maintain adequate coverage and reimbursement
for our product candidates could limit our ability to generate revenue. Our business model is also focused on lowering the cost and
increasing the accessibility of healthcare. Even if we are successful in driving down the cost of healthcare, third- party payors may still
not view our product candidates, if approved, as cost-effective, and coverage and reimbursement may not be available to our patients or
may not be sufficient to allow our products, if any, to be marketed on a competitive basis. If coverage and reimbursement are not
available, or reimbursement is available only to limited levels, patient subpopulations of labeled indications, or otherwise restricted, we,
or any collaborators, may not be able to successfully commercialize our product candidates. Even if coverage is provided, the approved
reimbursement amount may not be high enough to allow us, or any collaborators, to establish or maintain pricing sufficient to realize a
sufficient return on our or their investments. Cost-control initiatives could also cause us to decrease any price we might establish for our
product candidates, which could result in lower than anticipated product revenues. Moreover, eligibility for reimbursement does not
imply that any product will be paid for in all cases or at a rate that covers our costs, including our costs related to research, development,
manufacture, sale and distribution. Reimbursement rates may vary, by way of example, according to the use of the product and the
clinical setting in which it is used. For products administered under the supervision of a physician, obtaining coverage and adequate
reimbursement may be difficult because of the higher costs often associated with administering such drugs. If the prices for our product
candidates, if approved, decrease or if governmental and other third-party payors do not provide adequate coverage or reimbursement,
our business, financial condition, results of operations and prospects will suffer, perhaps materially.
There is significant uncertainty related to the insurance coverage and reimbursement of newly approved products. In the United States,
the Centers for Medicare and Medicaid Services (“CMS”), the federal agency responsible for administering the Medicare program,
makes the principal decisions about coverage and reimbursement for new treatments under Medicare. Private payors may follow CMS
to a substantial degree. It is difficult to predict what CMS will decide with respect to reimbursement for novel products such as ours. In
addition, certain Affordable Care Act marketplace and other private payor plans are required to include coverage for certain preventative
services, including vaccinations recommended by the U.S. Centers for Disease Control’s Advisory Committee on Immunization
74
Practices (“ACIP”) without cost share obligations (i.e., co- payments, deductibles or co-insurance) for plan members. For Medicare
beneficiaries, our product candidates, apart from UB-612, may be covered for reimbursement under either the Part B program or Part D
depending on several criteria, including the type of vaccine and the beneficiary’s coverage eligibility. If our product candidates, once
approved, are reimbursed only under the Part D program, physicians may be less willing to use our products because of the claims
adjudication costs and time related to the claims adjudication process and collection of copayments associated with the Part D program.
If our product candidates, once approved, are reimbursed only under the Part B program, certain potential drawbacks associated with
the Part B program, such as the time and effort required to seek reimbursement after purchase, may make our product candidates less
attractive to clinics or other potential customers. Outside of Medicare, private insurance is likely to raise similar claims adjudication and
copayment considerations, which may also make our product candidates less attractive to potential customers using private insurance.
Outside the United States, certain countries set prices and reimbursement for pharmaceutical products, with limited participation from
the marketing authorization holders. We cannot be sure that such prices and reimbursement will be acceptable to us or our collaborators.
If the regulatory authorities in these jurisdictions set prices or reimbursement levels that are not commercially attractive for us or our
collaborators, our revenues from sales by us or our collaborators, and the potential profitability of our product candidates, in those
countries would be negatively affected. Additionally, some countries require approval of the sale price of a product before it can be
marketed. In many countries, the pricing review period begins after marketing or product licensing approval is granted. As a result, we
might obtain marketing approval for a product in a particular country, but then may experience delays in the reimbursement approval of
our product or be subject to price regulations that would delay our commercial launch of the product, possibly for lengthy time periods,
which could negatively impact the revenues we are able to generate from the sale of the product in that particular country.
Moreover, an increasing number of countries are taking initiatives to attempt to reduce large budget deficits by focusing cost-cutting
efforts on pharmaceuticals for their state-run healthcare systems. These international price control efforts have impacted all regions of
the world, notably in the European Union. In some countries, in particular in many Member States of the European Union, we may be
required to conduct a clinical trial or other studies that compare the cost-effectiveness of our product candidates to other available
therapies in order to obtain or maintain reimbursement or pricing approval. In addition, publication of discounts by third- party payors
or authorities may lead to further pressure on the prices or reimbursement levels within the country of publication and other countries.
If reimbursement of our products is unavailable or limited in scope or amount, or if pricing is set at unsatisfactory levels, our business,
financial condition, results of operations or prospects could be materially adversely affected. Cost-control initiatives could cause us, or
any collaborators, to decrease the price we, or they, might establish for products, which could result in lower than anticipated product
revenues. Further, our competitors have more experience dealing with and contracting with payors for preferred coverage, which could
potentially put us at a competitive disadvantage. An inability to promptly obtain coverage and adequate payment rates from both
government-funded and private payors for any of our product candidates for which we, or any future collaborator, obtain marketing
approval could significantly harm our operating results, our ability to raise capital needed to commercialize products and our overall
financial condition.
Our business and current and future relationships with third-party payors, healthcare professionals and customers in the United
States and elsewhere will be subject to applicable healthcare laws and regulations, which could expose us to significant penalties.
Healthcare providers, physicians and third-party payors in the United States and elsewhere will play a primary role in the
recommendation and prescription of any product candidates for which we obtain marketing approval. Our current and future
arrangements with healthcare professionals, third-party payors and customers expose us to broadly applicable fraud and abuse and other
healthcare laws and regulations, including, without limitation, the federal Anti-Kickback Statute and the federal civil False Claims Act,
that may constrain the business or financial arrangements and relationships through which we conduct clinical research, sell, market and
distribute any products for which we obtain marketing approval. In addition, we may be subject to physician payment transparency laws
and patient privacy regulation by the federal government and by the U.S. states and foreign jurisdictions in which we conduct our
business.
Efforts to ensure that our business arrangements with third parties will comply with applicable healthcare laws and regulations may
involve substantial costs. It is possible that governmental authorities will conclude that our business practices, including our relationships
with physicians and other healthcare providers, some of whom may recommend, purchase or prescribe our product candidate, if
approved, may not comply with current or future statutes, regulations or case law involving applicable fraud and abuse or other
healthcare laws and regulations.
If our operations are found to be in violation of any of these laws or any other governmental regulations that may apply to us, we may
be subject to significant civil, criminal and administrative penalties, including, without limitation, damages, fines, disgorgement,
individual imprisonment, exclusion from participation in government healthcare programs, such as Medicare and Medicaid, additional
reporting requirements and oversight if we become subject to a corporate integrity agreement or similar agreement to resolve allegations
of noncompliance with these laws and the curtailment or restructuring of our operations, which could have a material adverse effect on
our business. If any of the physicians or other healthcare providers or entities with whom we expect to do business is found not to be in
compliance with applicable laws, they may be subject to criminal, civil or administrative sanctions, including exclusions from
participation in government healthcare programs, which could also materially affect our business.
75
Cyberattacks or other failures in our or our third-party vendors’, contractors’ or consultants’ telecommunications or information
technology systems could result in information theft, compromise, or other unauthorized access, data corruption and significant
disruption of our business operations, and could harm our reputation and subject us to liability, lawsuits and actions from
governmental authorities.
The success of our research and development programs depends on data which is stored and transmitted digitally, the corruption or loss
of which could cause significant setback to one or all of our programs. We face a number of risks related to our use, processing, storage
and security of this critical information, including loss of access, inappropriate use or disclosure, inappropriate modification corruption,
unauthorized access or processing. Because we use third-party vendors and subcontractors to manage our sensitive information, we also
may not have the ability to adequately monitor, audit or modify the security controls over this critical information. Despite the
implementation of security measures, given the size and complexity of our internal information technology (“IT”) systems and those of
our third-party vendors, contractors and consultants, such IT systems are potentially vulnerable to breakdown or other damage or
interruption from service interruptions, system malfunction, natural disasters, terrorism, war, and telecommunication and electrical
failures.
Cyber threats are persistent and constantly evolving. Such threats, which may include ransomware or other malware, phishing attacks,
denial of services attacks, man-in-the-middle attacks and others, have increased in frequency, scope and potential impact in recent years,
which increase the difficulty of detecting and successfully defending against them. We may not be able to anticipate all types of security
threats, and, despite our efforts, we may not be able to implement preventive measures effective against all such security threats. The
techniques used by cyber criminals change frequently, may not be recognized until launched, and can originate from a wide variety of
sources, including outside groups such as external service providers, organized crime affiliates, terrorist organizations or hostile foreign
governments or agencies. There can be no assurance that we or our third-party service providers, contractors or consultants will be
successful in preventing cyberattacks or successfully mitigating their effects. Our IT systems and those of our third-party service
providers, contractors or consultants are additionally vulnerable to security breaches from inadvertent or intentional actions by our
employees, third-party vendors, contractors, consultants, business partners and/or other third parties. These threats pose a risk to the
security of our systems and networks, the confidentiality and the availability, security and integrity of our data, and these risks apply
both to us and to third parties on whose systems we rely for the conduct of our business. If the IT systems of our third-party vendors and
other contractors and consultants become subject to disruptions or security breaches, we may have insufficient recourse against such
third parties and we may have to expend significant resources to mitigate the impact of such an event, and to develop and implement
protections to prevent future events of a similar nature from occurring. Any cyberattack or destruction or loss of, unauthorized access
to, processing of, or exfiltration of data could have a material adverse effect on our business, financial condition, results of operations
and prospects. For example, if such an event were to occur and cause interruptions in our operations, or those of our third-party vendors
and other contractors and consultants, it could result in a material disruption or delay of the development of our product candidates. In
addition, we may suffer reputational harm or face litigation or adverse regulatory action as a result of cyberattacks or other data security
breaches, particularly those involving personal information or protected health information, and may incur significant additional expense
to implement further data protection measures. As cyber threats continue to evolve, we may be required to incur material additional
expenses in order to enhance our protective measures or to remediate any information security vulnerability.
We are subject to stringent privacy laws, information security laws, regulations, policies and contractual obligations related to data
privacy and security and changes in such laws, regulations, policies and contractual obligations could adversely affect our business,
financial condition, results of operations and prospects.
We are subject to data privacy and security laws and regulations that apply to the collection, transmission, storage, use, processing,
destruction, retention and security of personal information, which among other things, including additional laws or regulations relating
to health information. The legislative and regulatory landscape for privacy and data protection continues to evolve in jurisdictions
worldwide, and these laws may at times be conflicting. It is possible that these laws may be interpreted and applied in a manner that is
inconsistent with our practices and our efforts to comply with the evolving data protection rules may be unsuccessful. We must devote
significant resources to understanding and complying with this changing landscape. Failure to comply with federal, state and
international laws regarding privacy and security of personal information could expose us to penalties under such laws, orders requiring
that we change our practices, claims for damages or other liabilities, regulatory investigations and enforcement action, litigation and
significant costs for remediation, any of which could adversely affect our business. Even if we are not determined to have violated these
laws, government investigations into these issues typically require the expenditure of significant resources and generate negative
publicity, which have a material adverse effect on our business, financial condition, results of operations and prospects. Failure to comply
with any of these laws and regulations could result in enforcement action against us, including fines, criminal prosecution of employees,
claims for damages by affected individuals and damage to our reputation and loss of goodwill, any of which could have a material
adverse effect on our business, financial condition, results of operations and prospects. Additionally, if we are unable to properly protect
the privacy and security of personal information, including protected health information, we could be found to have breached our
contracts with certain third parties.
There are numerous U.S. federal and state laws and regulations related to the privacy and security of personal information. In particular,
HIPAA, as amended by the Health Information Technology for Economic and Clinical Health Act of 2009 (“HITECH”) and their
76
respective implementing regulations, establish privacy and security standards that limit the use and disclosure of individually identifiable
health information, or protected health information, and require the implementation of administrative, physical and technological
safeguards to protect the privacy of protected health information and ensure the confidentiality, integrity and availability of electronic
protected health information. Determining whether protected health information has been handled in compliance with applicable privacy
standards and our contractual obligations can be complex and may be subject to changing interpretation. If we fail to comply with
applicable privacy laws, including applicable HIPAA privacy and security standards, we could face civil and criminal penalties. The
HHS has the discretion to impose penalties without attempting to first resolve violations. HHS enforcement activity can result in financial
liability and reputational harm, and responses to such enforcement activity can consume significant internal resources. Even when
HIPAA does not apply, failing to take appropriate steps to keep consumers’ personal information secure can constitute unfair acts or
practices in or affecting commerce and be construed as a violation of Section 5(a) of the Federal Trade Commission Act (the “FTCA”),
15 U.S.C § 45(a). The FTC expects a company’s data security measures to be reasonable and appropriate in light of the sensitivity and
volume of consumer information it holds, the size and complexity of its business, and the cost of available tools to improve security and
reduce vulnerabilities. Individually identifiable health information is considered sensitive data that merits stronger safeguards and the
FTC’s guidance for appropriately securing consumers’ personal information is similar to what is required by the HIPAA Security Rule.
In addition, state attorneys general are authorized to bring civil actions seeking either injunctions or damages in response to violations
that threaten the privacy of state residents. We cannot be sure how these regulations will be interpreted, enforced or applied to our
operations. In addition to the risks associated with enforcement activities and potential contractual liabilities, our ongoing efforts to
comply with evolving laws and regulations at the federal and state level may be costly and require ongoing modifications to our policies,
procedures and systems.
Internationally, laws, regulations and standards in many jurisdictions apply broadly to the collection, transmission, storage, use,
processing, destruction, retention and security of personal information. For example, in the European Union, the collection, transmission,
storage, use, processing, destruction, retention and security of personal data is governed by the provisions of the General Data Protection
Regulation (the “GDPR”) in addition to other applicable laws and regulations. The GDPR came into effect in May 2018, repealing and
replacing the European Union Data Protection Directive, and imposing revised data privacy and security requirements on companies in
relation to the processing of personal data of European Union data subjects. The GDPR, together with national legislation, regulations
and guidelines of the European Union Member States governing the collection, transmission, storage, use, processing, destruction,
retention and security of personal data, impose strict obligations with respect to, and restrictions on, the collection, use, retention,
protection, disclosure, transfer and processing of personal data. The GDPR also imposes strict rules on the transfer of personal data to
countries outside the European Union that are not deemed to have protections for personal information, including the United States. The
GDPR authorizes fines for certain violations of up to 4% of the total global annual turnover of the preceding financial year or €20 million,
whichever is greater. Such fines are in addition to any civil litigation claims by data subjects. Separately, Brexit has led and could also
lead to legislative and regulatory changes and may increase our compliance costs. As of January 1, 2021, and the expiry of transitional
arrangements agreed to between the United Kingdom and the European Union, data processing in the United Kingdom is governed by
a United Kingdom version of the GDPR (combining the GDPR and the Data Protection Act 2018), exposing us to two parallel regimes,
each of which authorizes similar fines and other potentially divergent enforcement actions for certain violations. On June 28, 2021, the
European Commission adopted an adequacy decision for the United Kingdom, allowing for the relatively free exchange of personal
information between the European Union and the United Kingdom. Other jurisdictions outside the European Union are similarly
introducing or enhancing privacy and data security laws, rules and regulations, which could increase our compliance costs and the risks
associated with noncompliance. We cannot guarantee that we are, or will be, in compliance with all applicable international regulations
as they are enforced now or as they evolve.
We face potential liability related to the privacy of health information we obtain from clinical trials sponsored by us.
Most healthcare providers, including research institutions from which we obtain patient health information, are subject to privacy and
security regulations promulgated under HIPAA, as amended by the Health Information Technology for Economic and Clinical Health
Act. We do not believe that we are currently classified as a covered entity or business associate under HIPAA and thus are not directly
subject to its requirements or penalties. However, any person may be prosecuted under HIPAA’s criminal provisions either directly or
under aiding-and-abetting or conspiracy principles. Consequently, depending on the facts and circumstances, we could face substantial
criminal penalties if we knowingly receive individually identifiable health information from a HIPAA -covered healthcare provider or
research institution that has not satisfied HIPAA’s requirements for disclosure of individually identifiable health information. Even
when HIPAA does not apply, according to the FTC failing to take appropriate steps to keep consumers’ personal information secure
constitutes unfair acts or practices in or affecting commerce in violation of the FTCA. The FTC expects a company’s data security
measures to be reasonable and appropriate in light of the sensitivity and volume of consumer information it holds, the size and
complexity of its business, and the cost of available tools to improve security and reduce vulnerabilities. Individually identifiable health
information is considered sensitive data that merits stronger safeguards.
In addition, we may maintain sensitive personally identifiable information, including health information, that we receive throughout the
clinical trial process, in the course of our research collaborations. As such, we may be subject to state laws, including the CCPA,
requiring notification of affected individuals and state regulators in the event of a breach of personal information, which is a broader
class of information than the health information protected by HIPAA. Our clinical trial programs outside the United States may implicate
international data protection laws, including the GDPR and legislation of the EU member states implementing it.
77
Our activities outside the United States impose additional compliance requirements and generate additional risks of enforcement for
noncompliance. Failure by our CROs and other contractors to comply with the strict rules on the transfer of personal data outside of the
EU into the United States may result in the imposition of criminal and administrative sanctions on such collaborators, which could
adversely affect our business. Furthermore, certain health privacy laws, data breach notification laws, consumer protection laws and
genetic testing laws may apply directly to our operations and/or those of our collaborators and may impose restrictions on our collection,
use and dissemination of individuals’ health information.
Moreover, patients about whom we or our collaborators obtain health information, as well as the providers who share this information
with us, may have statutory or contractual rights that limit our ability to use and disclose the information. We may be required to expend
significant capital and other resources to ensure ongoing compliance with applicable privacy and data security laws. Claims that we
have violated individuals’ privacy rights or breached our contractual obligations, even if we are not found liable, could be expensive
and time-consuming to defend and could result in adverse publicity that could harm our business.
If we or our contract manufacturers, CROs or other contractors or consultants fail to comply with applicable federal, state or local
regulatory privacy requirements, we could be subject to a range of regulatory actions that could affect our or our contractors’ ability to
develop and commercialize our product candidates and could harm or prevent sales of any affected products that we are able to
commercialize, or could substantially increase the costs and expenses of developing, commercializing and marketing our products. Any
threatened or actual government enforcement action could also generate adverse publicity and require that we devote substantial
resources that could otherwise be used in other aspects of our business. Increasing use of social media could give rise to liability,
breaches of data security or reputational damage. Any of the foregoing could have a material adverse effect on our business, financial
condition, results of operations and prospects.
We face substantial competition, which may result in others discovering, developing or commercializing products before or more
successfully than we do.
The biotechnology and pharmaceutical industries are characterized by rapidly advancing technologies, intense competition and a strong
emphasis on proprietary products. We face and will continue to face competition from third parties that use similar platforms and from
third parties focused on developing and commercializing other peptide and peptide-based product candidates. The competition is likely
to come from multiple sources, including large and specialty pharmaceutical and biotechnology companies, academic research
institutions, government agencies and public and private research institutions.
Many of our potential competitors, alone or with their strategic partners, have substantially greater financial, technical and other
resources than we do, such as larger research and development, clinical, marketing and manufacturing organizations. Mergers and
acquisitions in the biotechnology and pharmaceutical industries may result in even greater concentration of resources among a smaller
number of competitors. Our commercial opportunity could be reduced or eliminated if competitors develop and commercialize products
that are safer, more effective, have fewer or less severe side effects, are more convenient or are less expensive than any products that
we may develop. Our competitors also may obtain FDA or other regulatory approvals for their products faster or earlier than we may
obtain approval for ours, which could result in our competitors establishing a strong market position before we are able to enter the
market. For example, some of our competitors have already received approval from the FDA and other regulatory authorities for their
COVID-19 vaccines and boosters to address variants of SARS-CoV-2. Additionally, technologies developed by our competitors may
render our product candidates uneconomical or obsolete, and we may not be successful in marketing our product candidates against
competitors’ products. In addition, the availability of our competitors’ products and the lack of complementary products offered by our
sales and distribution team as compared to competitors with more extensive product lines, could limit the demand and the prices we are
able to charge for any products that we may develop and commercialize.
78
Developments by competitors may render our products or technologies obsolete or non-competitive or may reduce the size of our
markets.
Our industry has been characterized by extensive research and development efforts, rapid developments in technologies, intense
competition and a strong emphasis on proprietary products. We expect our product candidates to face intense and increasing competition
as new products enter the relevant markets and advanced technologies become available. We face potential competition from many
different sources, including pharmaceutical, biotechnology and specialty pharmaceutical companies. Academic research institutions,
governmental agencies and public and private institutions are also potential sources of competitive products and technologies. Our
competitors may have or may develop superior technologies or approaches and have different business models from us which do not
focus on democratizing healthcare and on lower cost, all of which may provide them with competitive advantages. Many of these
competitors may also have compounds already approved or in development in the therapeutic categories that we are targeting with our
product candidates. The global vaccine market is highly concentrated among a small number of multinational pharmaceutical companies:
Pfizer, Merck, GlaxoSmithKline and Sanofi together control most of the global vaccine market. While we are not aware of all of our
competitors’ efforts, there are more than twenty COVID-19 vaccines already approved for use in one or more countries around the
world, including three in the United States. We also face substantial competition in therapeutic areas outside of COVID-19. For example,
the FDA approved aducanumab in June 2021 as the first FDA-approved immunotherapy for AD. In addition, many of our competitors,
either alone or together with their collaborative partners, may operate larger research and development programs or have substantially
greater financial resources than we do, as well as greater experience in:
• developing product candidates;
• undertaking pre-clinical testing and clinical trials;
• obtaining NDA approval by the FDA;
• obtaining comparable foreign regulatory approvals of product candidates;
• formulating and manufacturing products;
• launching, marketing and selling products; and
• competing for market share, obtaining reimbursement and securing payor contractors for preferential coverage.
If these competitors access the marketplace with safer, more effective, or less expensive therapeutics, our product candidates, if approved
for commercialization, may not be profitable to sell or worthwhile to continue to develop. Technology in the pharmaceutical industry
has undergone rapid and significant change, and we expect that it will continue to do so. Any compounds, products or processes that we
develop may become obsolete or uneconomical before we recover any expenses incurred in connection with their development. The
success of our product candidates will depend upon factors such as product efficacy, safety, reliability, availability, timing, scope of
regulatory approval, acceptance and price, among other things. Other important factors to our success include speed in developing
product candidates, completing clinical development and laboratory testing, obtaining regulatory approvals and manufacturing and
selling commercial quantities of potential products.
Our product candidates are intended to compete directly or indirectly with existing products and products currently in development.
Even if approved and commercialized, our product candidates may fail to achieve market acceptance with hospitals, physicians, patients
or third-party payors. Hospitals, physicians or patients may conclude that our products are less safe or effective or otherwise less
attractive than existing drugs. If our product candidates do not receive market acceptance for any reason, our revenue potential would
be diminished, which would materially adversely affect our ability to become profitable.
Many of our competitors have substantially greater capital resources, robust product candidate pipelines, established presence in the
market and expertise in research and development, manufacturing, pre-clinical and clinical testing, obtaining regulatory approvals and
reimbursement and marketing approved products than we do. As a result, our competitors may achieve product commercialization or
patent or other intellectual property protection earlier than we can. Smaller or early-stage companies may also prove to be significant
competitors, particularly through collaborative arrangements with large and established companies. These competitors also compete
with us in recruiting and retaining qualified clinical, regulatory, scientific, sales, marketing and management personnel and establishing
clinical trial sites and patient registration for clinical trials, as well as in acquiring technologies complementary to, or necessary for, our
programs. Our commercial opportunity could be reduced or eliminated if our competitors develop and commercialize products that are
safer, more effective, have fewer or less severe side effects, are more convenient, or are less expensive than any products that we may
develop or that would render any products that we may develop obsolete or noncompetitive.
79
We are subject to anti-corruption laws, including the U.S. Foreign Corrupt Practices Act (“FCPA”), and similar laws of non-U.S.
jurisdictions where we conduct business. If we fail to comply with these laws, we could be subject to civil or criminal penalties, other
remedial measures, and legal expenses, which could adversely affect our business, financial condition, results of operations and
prospects.
We are currently subject to anti-corruption laws, including the FCPA. The FCPA, the U.K. Bribery Act 2010 and other applicable anti-
bribery and anti-corruption laws generally prohibit us, our employees and intermediaries from bribing, being bribed or making other
prohibited payments to government officials or other persons to obtain or retain business or gain other business advantages. In
furtherance of our goal to democratize healthcare, we intend to distribute any product candidates that are approved or receive an EUA
in various countries around the world, including countries with a heightened corruption risk. This may raise the risk of non-compliance
with anti-corruption laws and other rules and regulations prohibiting bribery and other crimes. We also participate in collaborations and
relationships with third parties whose actions could potentially subject us to liability under the FCPA or other jurisdictions’ anti-
corruption laws, which in turn could result in internal and external investigations, associated legal costs and even civil fines and criminal
charges, any of which would divert time and resources away from our core business operations even if we and our employees and agents
do not violate laws and regulations. The FCPA also requires public companies to make and keep books and records that accurately and
fairly reflect the transactions of the corporation and to devise and maintain an adequate system of internal accounting controls. Our
business is heavily regulated and therefore involves significant interaction with public officials, including officials of non-U.S.
governments. Additionally, in many other countries, the health care providers who prescribe pharmaceuticals are (directly or indirectly)
employed by their government, and the purchasers of pharmaceuticals are government entities; therefore, our dealings with these
prescribers and purchasers are subject to regulation under, but not limited to, the FCPA. In recent years, the SEC and Department of
Justice have also increased their FCPA enforcement activities with respect to pharmaceutical companies.
We are in the process of establishing a program to govern the compliance of any potential sales or marketing operations of our products,
should any of them be approved or receive an EUA. To date, we have not had a robust compliance program. We cannot ensure that our
operations to date have complied, and that our future operations will comply, with our compliance program or laws, rules and regulations
governing the sales and marketing of pharmaceutical products, government contracting and other aspects of our business. We have used,
and plan to use, a network of agents in countries around the world to conduct our sales and marketing operations. These agents will not
be our employees, and while we intend to have a robust diligence program in connection with engaging agents, our diligence program
and compliance program may not be sufficient to prevent wrong-doing.
There is also no assurance that we will be completely effective in ensuring our compliance with all applicable anti-corruption laws,
including the FCPA, particularly given the high level of complexity of these laws. We have adopted a code of conduct applicable to all
of our employees and contractors, but it is not always possible to identify and deter misconduct by these parties and other third parties,
and the precautions we take to detect and prevent this activity may not be effective in controlling unknown or unmanaged risks or losses
or in protecting us from governmental investigations or other actions, claims or lawsuits stemming from a failure to comply with such
laws or regulations. If we are not in compliance with the FCPA or other anti-corruption laws, we may be subject to criminal and civil
penalties, disgorgement and other sanctions and remedial measures, and legal expenses, which could have an adverse impact on our
business, financial condition, results of operations and prospects. Similarly, any investigation of any potential violations of the FCPA
or other anti-corruption laws by authorities in the United States or other jurisdictions where we conduct business could also have an
adverse impact on our reputation, business, financial condition, results of operations and prospects.
As a result of our geographically diverse operations, we are more susceptible to certain risks.
We have offices in two different countries and additional operations in an additional two different countries. We have also used, and
plan to use, a network of agents in countries around the world to conduct our sales and marketing operations. If we are unable to manage
the risks of our global operations, including fluctuations in foreign exchange and inflation rates, international hostilities such as the
Russia-Ukraine conflict, natural disasters, security breaches, our ability to supply our product candidates on a timely and large scale
basis in local markets, lead times for shipping, accounts receivable collection times, import or export licensing requirements, language
barriers, failure to maintain compliance with our clients’ control requirements and multiple legal and regulatory systems, our results of
operations and ability to grow could be materially adversely affected. In particular, our business and stock price may be affected by
fluctuations in foreign exchange rates between currencies in different jurisdictions in which operate or in which we may have sales in
the future.
Certain legal and political risks are also inherent in foreign operations. Foreign sales of our product candidates could be adversely
affected by the imposition of governmental controls, political and economic instability, trade restrictions and changes in tariffs. In many
countries, the pricing of prescription pharmaceuticals is subject to governmental control. In these countries, pricing negotiations with
governmental authorities can take considerable time after the receipt of marketing approval for a drug. There is a risk that foreign
governments may nationalize private enterprises in certain countries where we may operate. In certain countries or regions, terrorist
activities and the response to such activities may threaten our operations more than in the United States. Social and cultural norms in
certain countries may not support compliance with our corporate policies, including those that require compliance with substantive laws
and regulations. Also, changes in general economic and political conditions in countries where we may operate are a risk to our financial
performance and future growth. Additionally, the need to identify financially and commercially strong partners for commercialization
80
outside the United States who will comply with the high manufacturing and legal and regulatory compliance standards we require is a
risk to our financial performance. As we operate our business globally, our success will depend, in part, on our ability to anticipate and
effectively manage these and other related risks. There can be no assurance that the consequences of these and other factors relating to
our international operations will not have an adverse effect on our business, financial condition, results of operations and prospects.
We are exposed to potential product liability and professional indemnity risks that are inherent in the research, development,
manufacturing, marketing and use of pharmaceutical products.
The use of our investigational medicinal products in clinical trials, the sale of our ELISA test and the sale of any approved products in
the future may expose us to liability claims. These claims might be made by patients who use the product, health care providers,
pharmaceutical companies or others selling such products. Any claims against us, regardless of their merit, could be difficult and costly
to defend and could materially adversely affect the market for our product candidates or any prospects for commercialization of our
product candidates.
In addition, regulations vary significantly across jurisdictions regarding the clinical trial sponsor’s responsibility to provide free medical
care and compensation to clinical trial participants who experience an injury or illness during the trial. For example, there is no legal
requirement in the United States for sponsors to provide free medical treatment or compensation to a participant injured during a study;
as a result, sponsors usually agree to pay for the medical care to diagnose and treat participant injuries to the extent related to the clinical
trial and typically do not pay unless the injury is determined to be related to participation in the trial. In contrast, India requires free
medical care until it is established that the injury is not related to the study and compensation for any injury that is determined to be
related to the study. In 2019, India’s Ministry of Health and Family Welfare published the “New Drugs and Clinical Trials Rules,”
which increased a clinical trial sponsor’s liability for injuries related to clinical trial trials. Under the regulation, sponsors are required
to (i) provide “free medical management” to participants that experience an injury that, in the investigator’s opinion, is related to the
study or until it is established that the injury is not related to the study and (ii) “compensate” clinical trial participants for trial-related
injuries. Clinical trials conducted in jurisdictions with broad compensation and medical care requirements could result in increased
overall research costs and adversely affect our ability to conduct clinical trials.
Although the clinical trial process is designed to identify and assess potential side effects, it is always possible that a product, even after
regulatory approval, may exhibit unforeseen side effects, including rare side effects more likely to be seen in commercial use than in
clinical studies. If any of our product candidates were to cause adverse side effects during clinical trials or after approval of the product
candidate, we may be exposed to substantial liabilities. Physicians and patients may not comply with any warnings that identify known
potential adverse effects and patients who should not use our product candidates.
To cover such liability claims, we purchase clinical trial insurances in the conduct of each of our clinical trials (typically conducted
through our CROs). It is possible that our liabilities could exceed our insurance coverage or that our insurance will not cover all situations
in which a claim against us could be made. We also intend to expand our insurance coverage to include the sale of commercial products
if we receive marketing approval for any of our proprietary products. However, we may not be able to maintain insurance coverage at a
reasonable cost or obtain insurance coverage that will be adequate to satisfy any liability that may arise. If a successful product liability
claim or series of claims is brought against us for uninsured liabilities or in excess of insured liabilities, our assets may not be sufficient
to cover such claims and our business operations could be impaired. Should any of the events described above occur, this could have a
material adverse effect on our business, financial condition, results of operations and prospects, including, but not limited to:
• decreased demand for our future product candidates;
• adverse publicity and injury to our reputation;
• withdrawal of clinical trial participants;
• initiation of investigations by regulators;
• costs to defend the related litigation;
• a diversion of management’s time and our resources;
• compensation in response to a liability claim;
• product recalls, withdrawals or labeling, marketing or promotional restrictions;
• loss of revenue;
• exhaustion of any available insurance and our capital resources; and
81
• the inability to commercialize our products or product candidates.
We could be adversely affected if we are subject to negative publicity. We could also be adversely affected if any of our products or any
similar products distributed by other companies prove to be, or are asserted to be, harmful to patients. Any adverse publicity associated
with illness or other adverse effects resulting from patients’ use or misuse of our products or any similar products distributed by other
companies could have a material adverse impact on our business, financial condition, results of operations or prospects.
We will need to expand our organization, and we may experience difficulties in managing this growth, which could disrupt our
operations.
We expect to expand our organization, and as a result, we may encounter difficulties in managing our growth, which could disrupt our
operations. We expect to experience significant growth in the number of our employees and the scope of our operations, particularly in
the areas of clinical development and regulatory affairs, as well as to support our public company operations. For example, we may
build our own focused sales, distribution and marketing infrastructure to market our product candidates, if approved, in markets around
the world, which involves significant expenses and risks. To manage these growth activities, we must continue to implement and improve
our managerial, operational and financial systems, expand our facilities and continue to recruit and train additional qualified personnel.
Our management may need to devote a significant amount of its attention to managing these growth activities. Due to our limited
financial resources and the limited experience of our management team in managing a company with such anticipated growth, we may
not be able to effectively manage the expansion of our operations, retain key employees or identify, recruit and train additional qualified
personnel. Our inability to manage the expansion or relocation of our operations effectively may result in weaknesses in our
infrastructure, give rise to operational mistakes, loss of business opportunities, loss of employees and reduced productivity among
remaining employees. Our expected growth could also require significant capital expenditures and may divert financial resources from
other projects, such as the development of additional product candidates. If we are unable to effectively manage our expected growth,
our expenses may increase more than expected, our ability to generate revenues could be reduced and we may not be able to implement
our business strategy, including the successful development and commercialization of our product candidates. Any of the foregoing
could have a material adverse effect on our business, financial condition, results of operations and prospects. Future growth would
impose significant additional responsibilities on our management, including:
• the need to identify, recruit, maintain, motivate and integrate additional employees, consultants and contractors;
• managing our internal development efforts effectively, including the clinical and regulatory review process for our product
candidates, while complying with our contractual obligations to contractors and other third parties; and
• improving our operational, financial and management controls, reporting systems and procedures. We currently rely, and
for the foreseeable future will continue to rely, in substantial part on certain related parties, independent organizations,
advisors and consultants to provide certain services, including substantially all aspects of regulatory approval, clinical trial
management and manufacturing. There can be no assurance that the services of independent organizations, advisors and
consultants will continue to be available to us on a timely basis when needed, or that we can find qualified replacements.
In addition, if we are unable to effectively manage our outsourced activities or if the quality or accuracy of the services
provided by consultants is compromised for any reason, our clinical trials may be extended, delayed or terminated, and we
may not be able to obtain regulatory approval of our product candidates or otherwise advance our business. There can be
no assurance that we will be able to manage our existing consultants or find other competent outside contractors and
consultants on economically reasonable terms, or at all. If we are not able to effectively expand our organization by hiring
new employees and expanding our groups of consultants and contractors, or we are not able to effectively build out new
facilities to accommodate this expansion, we may not be able to successfully implement the tasks necessary to further
develop and commercialize our product candidates and, accordingly, may not achieve our research, development and
commercialization goals.
Many of the biotechnology and pharmaceutical companies that we compete against for qualified personnel and consultants have greater
financial and other resources, different risk profiles and a longer history in the industry than we do. If we are unable to continue to attract
and retain high-quality personnel and consultants, the rate and success at which we can discover and develop product candidates and
operate our business will be limited.
We only have a limited number of employees to manage and operate our business, which may lead to certain operational issues.
As of December 31, 2021, we had 89 full-time employees. Our focus on the development of UB-311, UB-612 and other product
candidates requires us to manage and operate our business in a highly efficient manner. We have a limited number of employees upon
which we rely to effectively manage and operate our business and we cannot assure you that operational issues will not arise.
While we intend to identify, recruit, maintain, motivate and integrate additional employees, consultants and contractors to support our
growth, we cannot assure you that we will be able to hire and/or retain adequate staffing levels to develop our product candidates or run
our operations and/or to accomplish all of the objectives that we otherwise would seek to accomplish.
82
If we lose key management or scientific personnel, cannot recruit qualified employees, directors, officers or other significant
personnel or experience increases in our compensation costs, our business may materially suffer.
We are highly dependent on our management and directors. Due to the specialized knowledge each of our officers and key employees
possesses with respect to our product candidates and our operations, the loss of service of any of our officers or directors could delay or
prevent the successful enrollment and completion of our clinical trials. We do not carry key person life insurance on any officers or
directors. In general, the employment arrangements that we have with our executive officers do not prevent them from terminating their
employment with us at any time. Our agreements with our employees generally provide for at-will employment.
In addition, our future success and growth will depend in part on the continued service of our directors, employees and management
personnel and our ability to identify, hire and retain additional personnel. If we lose one or more of our executive officers or key
employees, our ability to implement our business strategy successfully could be seriously harmed. Furthermore, replacing executive
officers and key employees may be difficult or costly and may take an extended period of time because of the limited number of
individuals in our industry with the breadth of skills and experience required to develop, gain regulatory approval of and commercialize
product candidates successfully. Competition to hire from this limited pool is intense, and we may be unable to hire, train, retain or
effectively incentivize these additional key personnel on acceptable terms given the competition among numerous pharmaceutical and
biotechnology companies for similar personnel. We also experience competition for the hiring of scientific and clinical personnel from
universities and research institutions. In addition, we rely on consultants and advisors, including scientific and clinical advisors, to assist
us in formulating our research, development and commercialization strategy. Our consultants and advisors may be engaged by entities
other than us and may have commitments under consulting or advisory contracts with other entities that may limit their availability to
us. If we are unable to continue to attract and retain high quality personnel, our ability to develop and commercialize product candidates
will be limited.
Many of our employees have become or will soon become vested in a substantial amount of our Class A common stock or a number of
common stock options. Our employees may be more likely to leave us if the shares they own have significantly appreciated in value
relative to the original purchase prices of the shares, or if the exercise prices of the options that they hold are significantly below the
market price of Class A our common stock, particularly after the expiration of the lock-up agreements in connection with our initial
public offering. Our future success also depends on our ability to continue to attract and retain additional executive officers and other
key employees.
If we engage in future acquisitions, joint ventures or strategic collaborations, this may increase our capital requirements, dilute our
stockholders, cause us to incur debt or assume contingent liabilities and subject us to other risks.
We may evaluate various acquisitions and collaborations, including licensing or acquiring complementary products, intellectual property
rights, technologies, or businesses. Any potential acquisition, joint venture, or collaboration may entail numerous risks, including:
• increased operating expenses and cash requirements;
• the assumption of additional indebtedness or contingent liabilities;
• assimilation of operations, intellectual property and products of an acquired company, including difficulties associated
with integrating new personnel;
• the diversion of our management’s attention from our existing product programs and initiatives in pursuing such a strategic
merger or acquisition;
• retention of key employees, the loss of key personnel and uncertainties in our ability to maintain key business relationships;
• risks and uncertainties associated with the other party to such a transaction, including the prospects of that party and their
existing products or investigational medicines and regulatory approvals; and
• our inability to generate revenue from acquired technology or products sufficient to meet our objectives in undertaking the
acquisition or even to offset the associated acquisition and maintenance costs.
In addition, if we undertake acquisitions, we may utilize our cash, issue dilutive securities, assume or incur debt obligations, incur large
one-time expenses and acquire intangible assets that could result in significant future amortization expense.
Moreover, we may not be able to locate suitable acquisition or strategic collaboration opportunities, and this inability could impair our
ability to grow or obtain access to technology or products that may be important to the development of our business.
83
We or the third parties upon whom we depend may be adversely affected by natural disasters or pandemics and our business
continuity and disaster recovery plans may not adequately protect us from a serious disaster.
Natural disasters or pandemics, other than or in addition to COVID-19 and including any potential future waves of COVID-19, could
severely disrupt our operations and have a material adverse effect on our business, results of operations, financial condition and
prospects. For example, our main laboratory is located on the Eastern coast of Florida, a location that is at a higher risk of exposure to
hurricanes. If a hurricane or natural disaster causes us to sustain significant damage to our Florida laboratory, or if we must shut down
our operations there for an extended period of time, our business and financial results would be adversely impacted.
If a natural disaster, power outage, pandemic, such as the COVID-19 pandemic, or other event occurred that prevented us from using
all or a significant portion of our headquarters, that damaged critical infrastructure, such as the manufacturing facilities on which we
rely, or that otherwise disrupted operations, it may be difficult or, in certain cases, impossible for us to continue our business for a
substantial period of time. The disaster recovery and business continuity plans we have in place may prove inadequate in the event of a
serious disaster or similar event. We may incur substantial expenses as a result of the limited nature of our disaster recovery and business
continuity plans, which could have a material adverse effect on our business.
Unstable market and economic conditions may have serious adverse consequences on our business, financial condition and share
price.
The global economy, including credit and financial markets, has experienced extreme volatility and disruptions, including severely
diminished liquidity and credit availability, declines in consumer confidence, declines in economic growth, increases in unemployment
rates and uncertainty about economic stability. For example, the COVID-19 pandemic has resulted in widespread unemployment, an
economic slowdown and extreme volatility in the capital markets. While these effects of COVID-19 have abated as countries, including
the United States, have re-opened and the rate of vaccinations have increased, COVID-19 continues to cause significant disruptions both
in the United States and globally. If the equity and credit markets deteriorate, it may make any necessary debt or equity financing more
difficult to obtain in a timely manner or on favorable terms, more costly or more dilutive. In addition, there is a risk that one or more of
our CROs, suppliers, contract manufacturers or other third-party providers may not survive an economic downturn, or that industry
trends with respect to pricing models, supply chains and delivery mechanisms, among other things, deviate from our expectations. As a
result, our business, results of operations and price of our Class A common stock may be adversely affected.
Our insurance policies are expensive and protect us only from some business risks, which leaves us exposed to significant uninsured
liabilities.
Though we have insurance coverage for clinical trial product liability, we do not carry insurance for all categories of risk that our
business may encounter. Some of the policies we currently maintain include general liability, auto, renters’, workers’ compensation and
directors’ and officers’ insurance.
Any additional product liability insurance coverage we acquire in the future may not be sufficient to reimburse us for any expenses or
losses we may suffer. Moreover, insurance coverage is becoming increasingly expensive and in the future we may not be able to maintain
insurance coverage at a reasonable cost or in sufficient amounts to protect us against losses due to liability. If we obtain marketing
approval for any of our product candidates, we intend to acquire insurance coverage to include the sale of commercial products; however,
we may be unable to obtain product liability insurance on commercially reasonable terms or in adequate amounts. A successful product
liability claim or series of claims brought against us could cause our stock price to decline and, if judgments exceed our insurance
coverage, could adversely affect our results of operations and business, including preventing or limiting the development and
commercialization of any product candidates we develop. We do not carry specific biological or hazardous waste insurance coverage,
and our renters’ and general liability insurance policies specifically exclude coverage for damages and fines arising from biological or
hazardous waste exposure or contamination. Accordingly, in the event of contamination or injury, we could be held liable for damages
or be penalized with fines in an amount exceeding our resources, and our clinical trials or regulatory approvals could be suspended.
We also expect that operating as a public company will make it more difficult and more expensive for us to obtain director and officer
liability insurance, and we may be required to accept reduced policy limits and coverage or incur substantially higher costs to obtain the
same or similar coverage. As a result, it may be more difficult for us to attract and retain qualified people to serve on our board of
directors, our board committees or as executive officers. We do not know, however, if we will be able to maintain existing insurance
with adequate levels of coverage. Any significant uninsured liability may require us to pay substantial amounts, which would adversely
affect our cash and cash equivalents position and results of operations.
The ongoing coronavirus pandemic has caused interruptions or delays of our business plan. Delays caused by the coronavirus
pandemic may have a significant adverse effect on our business.
In December 2019, a strain of coronavirus, COVID-19, was reported to have surfaced in Wuhan, China, and on March 12, 2020, the
World Health Organization declared COVID-19 to be a pandemic. In an effort to contain and mitigate the spread of COVID-19, many
countries, including the United States, Canada and China, have imposed unprecedented restrictions on travel, quarantines and other
84
public health safety measures. The extent to which the pandemic may impact our business will depend on future developments, which
are highly uncertain and cannot be predicted, but the development of clinical supply materials could be delayed and enrollment of
patients in our studies may be delayed or suspended, as hospitals and clinics in areas where we are conducting trials shift resources to
cope with the COVID-19 pandemic and may limit access or close clinical facilities due to the COVID-19 pandemic. Additionally, if our
trial participants are unable to travel to our clinical study sites as a result of quarantines or other restrictions resulting from the COVID-
19 pandemic, we may experience higher drop-out rates or delays in our clinical studies. We have manufacturers and collaboration
partners located in foreign jurisdictions, and travel restrictions have limited, and may continue to limit, our ability to visit their locations
in person and conduct on-site inspections.
Government-imposed quarantines and restrictions may also require us to temporarily suspend or terminate activity at our clinical sites.
Furthermore, if we determine that our trial participants may suffer from exposure to COVID-19 as a result of their participation in our
clinical trials, we may voluntarily terminate certain clinical sites as a safety measure until we reasonably believe that the likelihood of
exposure has subsided. As a result, we may encounter difficulties or delays in initiating, enrolling, conducting or completing our planned
and ongoing clinical trials, and our expected development timelines for our product candidates may be negatively impacted. We cannot
predict the ultimate impact of the COVID-19 pandemic as consequences of such an event are highly uncertain and subject to change.
We do not yet know the full extent of potential delays or impacts on our business, our clinical studies or as a whole; however, the
COVID-19 pandemic may materially disrupt or delay our business operations, further divert the attention and efforts of the medical
community to coping with COVID-19, disrupt the marketplace in which we operate, and/or have a material adverse effect on our
operations.
Moreover, the various precautionary measures taken by many governmental authorities around the world in order to limit the spread of
COVID-19 has had and may continue to have an adverse effect on the global markets and global economy generally, including on the
availability and pricing of employees, resources, materials, manufacturing and delivery efforts and other aspects of the global economy.
There have been business closures and a substantial reduction in economic activity in countries that have had significant outbreaks of
COVID-19. Significant uncertainty remains as to the potential impact of the COVID-19 pandemic on the global economy as a whole. It
is currently not possible to predict how long the pandemic will last or the time that it will take for economic activity to return to prior
levels. The COVID-19 pandemic could materially disrupt our business and operations, interrupt our sources of supply, hamper our
ability to raise additional funds or sell or securities, continue to slow down the overall economy or curtail consumer spending.
Due to the vaccination rate, the demand for our COVID-19 product candidate may decrease significantly or disappear entirely.
An EUA for UB-612 was denied by the TFDA in August 2021. In addition to appealing that decision, we are exploring paths to approval
of UB-612 as a three-dose regimen and as a heterologous boost (boosting the immunity of a subject who has already received a different
vaccine). Other companies have also responded to the pandemic at a faster pace, and to date more than twenty COVID-19 vaccines have
been approved for use in one or more countries around the world, including three in the United States. As our competitors continue to
develop, receive regulatory approval for and commercialize their own COVID-19 vaccines and boosters, vaccination rates will continue
to increase, which will result in a material decrease in demand for our COVID-19 product candidate and a corresponding decrease in
our potential revenues. Further, the existence and significance of the opportunity to provide COVID-19 boosters in the future is highly
uncertain, and there can be no assurance that we will commercially benefit from the development of a COVID-19 booster market.
Risks Related to Our Class A Common Stock
An active trading market for our Class A common stock may not continue to be developed or sustained.
Prior to our initial public offering, there was no public market for our Class A common stock. Although our Class A common stock is
now listed on The Nasdaq Global Market, an active trading market for our shares of Class A common stock may never develop or be
sustained. If an active market for our Class A common stock does not develop or is not sustained, it may be difficult for you to sell
shares of our Class A common stock at an attractive price or at all. An inactive market may also impair our ability to raise capital by
selling shares of our common stock, our ability to motivate our employees through equity incentive awards, and our ability to acquire
other companies, products or technologies by using our common stock as consideration for such acquisitions.
The price of our Class A common stock may be volatile and may be affected by market conditions beyond our control, and purchasers
of our Class A common stock could incur substantial losses.
Our results of operations are likely to fluctuate in the future as a publicly traded company. In addition, securities markets worldwide
have experienced, and are likely to continue to experience, significant price and volume fluctuations. This market volatility, as well as
general economic, market or political conditions, could subject the market price of our shares of Class A common stock to wide price
fluctuations regardless of our operating performance, which could cause a decline in the market price of our common stock. Price
volatility may be greater if the public float and trading volume of shares of our Class A common stock is low. Some factors that may
cause the market price of our Class A common stock to fluctuate, in addition to the other risks mentioned in this Report, include:
• our operating and financial performance and prospects;
85
• our announcements or our competitors’ announcements regarding new products or services, enhancements, significant
contracts, acquisitions or strategic investments;
• any delay in our development or regulatory filings for our product candidates and any adverse development or perceived
adverse development with respect to the applicable regulatory authority’s review of such filings;
• if any of our product candidates receives an EUA or regulatory approval, the terms of such approval and market acceptance
and demand for such product candidates;
• the success of any efforts to acquire or in-license additional technologies, products or product candidates;
• changes in earnings estimates or recommendations by securities analysts who cover our Class A common stock;
• fluctuations in our financial results or, in the event we provide it from time to time, earnings guidance, or the financial
results or earnings guidance of companies perceived by investors to be similar to us;
• changes in our capital structure, such as future issuances of securities, sales of large blocks of common stock by our
stockholders, including our principal stockholders, or the incurrence of additional debt;
• additions and departure of key personnel;
• any disputes relating to our intellectual property, including any intellectual property infringement lawsuit or opposition,
interference or cancellation proceeding in which we may become involved;
• reputational issues, including reputational issues involving our competitors and their products;
• actions by institutional stockholders;
• changes in general economic and market conditions, including related to the COVID-19 pandemic;
• changes in industry conditions or perceptions or changes in the market outlook for the industry in which we compete,
including changes in the structure of healthcare payment systems; and
• changes in applicable laws, rules or regulations or regulatory actions affecting us or our clients and other dynamics.
These and other factors may cause the market price for shares of our Class A common stock to fluctuate substantially, which may limit
or prevent investors from readily selling their shares of our Class A common stock and may otherwise negatively affect the liquidity of
our Class A common stock. In addition, in the past, when the market price of a stock has been volatile, holders of that stock sometimes
have instituted securities class action litigation against the company that issued the stock. Securities litigation against us, regardless of
the merits or outcome, could result in substantial costs and divert the time and attention of our management from the business, which
could significantly harm our business, results of operation, financial condition or reputation.
86
The dual-class structure of our common stock and the Voting Agreement will have the effect of concentrating voting power, which
will significantly limit stockholders’ ability to influence the outcome of matters submitted to our stockholders for approval, including
the election of our board of directors, the adoption of amendments to our Charter and Bylaws and the approval of any merger,
consolidation, sale of all or substantially all of our assets or other major corporate transaction.
Our Class A common stock has one vote per share, and our Class B common stock has ten votes per share. Our principal stockholders
have entered into the Voting Agreement. Mei Mei Hu, as proxyholder under the Voting Agreement, controls approximately 58.6% of
the total voting power of our outstanding capital stock. The Voting Agreement provides Mei Mei Hu with the authority (and irrevocable
proxies) to direct the vote and vote the shares of capital stock held by the parties to the voting agreement at her discretion on all matters
to be voted upon by stockholders. The voting power covered by the Voting Agreement may increase over time as the UBI Warrant is
exercised and as our principal stockholders exercise or vest equity awards that were outstanding at the time of the completion of our
initial public offering. If all such equity awards held by our principal stockholders had been exercised or vested and exchanged for shares
of common stock and the UBI Warrant had been exercised in full for shares of Class A common stock as of the date of the completion
of our initial public offering, assuming no other equity awards had been exercised or vested, the Voting Agreement would have covered,
in the aggregate as of the completion of our initial public offering, approximately 67.6% of the total voting power of our outstanding
capital stock. As a result, if our principal stockholders retain all or a large portion their common stock, including the common stock
issuable upon the exercise or vesting of such principal stockholders’ outstanding equity awards or upon the exercise of the UBI Warrant,
our principal stockholders will be able to significantly influence (if not control) any action requiring the approval of our stockholders,
including the election of our board of directors, the adoption of amendments to our amended and restated certificate of incorporation
(the “Charter”) and our amended and restated bylaws (the “Bylaws”) and the approval of any merger, consolidation, sale of all or
substantially all of our assets or other major corporate transaction. Assuming our principal stockholders retain their equity interests and
the Voting Agreement remains in effect, our principal stockholders will effectively control all such matters submitted to the stockholders
for the foreseeable future. Our principal stockholders will also have the voting power to determine the composition of our board of
directors, which in turn will be able to determine matters affecting us, including, among others:
• any determination with respect to our business direction and policies, including the appointment and removal of officers;
• the adoption of amendments to our Charter and Bylaws;
• determinations with respect to mergers, business combinations or disposition of assets;
• compensation and benefit programs and other human resources policy decisions;
• the payment of dividends on our common stock; and
• determinations with respect to tax matters.
Our principal stockholders may have interests that differ from yours and may vote in a way with which you disagree and which may be
adverse to your interests. This concentrated control may have the effect of delaying, preventing or deterring a change in control of the
Company, could deprive our stockholders of an opportunity to receive a premium for their capital stock as part of a sale in the Company
and might ultimately affect the market price of our Class A common stock. In addition, each share of Class B common stock will
automatically convert into one share of Class A common stock upon any transfer, whether or not for value and whether voluntary or
involuntary or by operation of law, except for certain transfers described in our Charter, including, without limitation, certain transfers
for tax and estate planning purposes. Such issuances will be dilutive to holders of our Class A common stock.
We are an “emerging growth company” and a “smaller reporting company” and will be able to avail ourselves of reduced disclosure
requirements applicable to emerging growth companies and smaller reporting companies, which could make our Class A common
stock less attractive to investors and adversely affect the market price of our Class A common stock.
We are an “emerging growth company,” as defined in the JOBS Act. We will remain an emerging growth company until the earliest of
(i) the last day of the fiscal year in which we have annual gross revenues of $1.07 billion or more; (ii) the date on which we have issued
more than $1.0 billion in non-convertible debt in the previous three years; (iii) the date we qualify as a “large accelerated filer” under
the Exchange Act, which would occur at the end of a given fiscal year if the market value of our common stock that is held by non-
affiliates is $700 million or more as of the last business day of the second fiscal quarter of such year (and we have been a public company
for at least 12 months and have filed one annual report on Form 10-K); and (iv) the last day of the fiscal year ending after the fifth
anniversary of our initial public offering. For so long as we remain an emerging growth company, we are permitted and intend to rely
on exemptions from certain disclosure requirements that are applicable to other public companies that are not emerging growth
companies. These exemptions include:
• not being required to comply with the auditor attestation requirements of Section 404 of the Sarbanes-Oxley Act;
87
• not being required to comply with any requirement that may be adopted by the Public Company Accounting Oversight
Board regarding mandatory audit firm rotation or a supplement to the auditor’s report providing additional information
about the audit and the financial statements;
• being required to provide only two years of audited financial statements in addition to any required unaudited interim
financial statements;
• permitting an extended transition period for complying with new or revised accounting standards, which allows an
emerging growth company to delay the adoption of certain accounting standards until those standards would otherwise
apply to private companies;
• reduced disclosure obligations regarding executive compensation; and
• exemptions from the requirements of holding a nonbinding advisory vote on executive compensation and shareholder
approval of any golden parachute payments not previously approved.
We may choose to take advantage of some, but not all, of the available exemptions. We have elected to use the extended transition
period for new or revised accounting standards during the period in which we remain an emerging growth company. To the extent that
we continue to qualify as a “smaller reporting company,” as such term is defined in Rule 12b-2 under the Exchange Act, after we cease
to qualify as an emerging growth company, we will continue to be permitted to make certain reduced disclosures in our periodic reports
and other documents that we file with the SEC. We cannot predict whether investors will find our Class A common stock less attractive
as a result of our reliance on these exemptions. If some investors find our Class A common stock less attractive as a result, there may
be a less active trading market for our Class A common stock and our stock price may be more volatile.
As long as our principal stockholders hold a majority of the voting power of our capital stock, we may rely on certain exemptions
from the corporate governance requirements of the Nasdaq available for “controlled companies.”
We are a “controlled company” within the meaning of the corporate governance requirements of the Nasdaq because our principal
stockholders will continue to hold more than 50% of the voting power of our outstanding shares of capital stock as a result of our dual-
class common stock structure and the Voting Agreement. A controlled company may elect not to comply with certain corporate
governance requirements of the Nasdaq. Accordingly, our board of directors will not be required to have a majority of independent
directors and our Compensation Committee and Nominating and Governance Committee will not be required to meet the director
independence requirements to which we would otherwise be subject until such time as we cease to be a “controlled company.”
Accordingly, you will not have certain of the protections afforded to stockholders of companies that are subject to all of the corporate
governance requirements of the Nasdaq.
Your percentage ownership in us may be diluted by future issuances of capital stock, which could reduce your influence over matters
on which stockholders vote.
Pursuant to our Charter and Bylaws, our board of directors has the authority, without action or vote of our stockholders, to issue all or
any part of our authorized but unissued shares of common stock, including shares issuable upon the exercise of options, or shares of our
authorized but unissued preferred stock. Issuances of shares of common stock or shares of voting preferred stock would reduce your
influence over matters on which our stockholders vote and, in the case of issuances of shares of preferred stock, would likely result in
your interest in us being subject to the prior rights of holders of that preferred stock.
Future sales of a substantial number of shares of our Class A common stock may depress the price of our shares.
If our stockholders sell a large number of shares of our Class A common stock, or if we issue a large number of shares of our Class A
common stock in connection with future acquisitions, financings or other circumstances, the market price of shares of our Class A
common stock could decline significantly. Moreover, the perception in the public market that our stockholders might sell shares of our
Class A common stock could depress the market price of those shares. In addition, sales of a substantial number of shares of our common
stock by our principal stockholders could adversely affect the market price of our Class A common stock.
We do not anticipate declaring or paying regular dividends on our Class A common stock in the near term, and any indebtedness
could limit our ability to pay dividends on our Class A common stock.
We have never declared and do not anticipate declaring or paying regular cash dividends on our Class A common stock in the near term.
We currently intend to use our future earnings, if any, to pay any debt obligations, to fund our growth and develop our business and for
general corporate purposes. Therefore, you are not likely to receive any cash dividends on your Class A common stock in the near term,
and the success of an investment in shares of our Class A common stock will depend upon any future appreciation in their value, which
is not certain to occur. There is no guarantee that shares of our Class A common stock will appreciate in value or even maintain the price
at which they are initially offered. Any future declaration and payment of cash dividends or other distributions of capital will be at the
88
discretion of our board of directors and the payment of any future cash dividends or other distributions of capital will depend on many
factors, including our financial condition, earnings, cash needs, regulatory constraints, capital requirements (including requirements of
our subsidiaries) and any other factors that our board of directors deems relevant in making such a determination. We cannot assure you
that we will establish a dividend policy or pay cash dividends in the future or continue to pay any cash dividend if we do commence
paying cash dividends pursuant to a dividend policy or otherwise.
Our Charter designates courts in the State of Delaware as the sole and exclusive forum for certain types of actions and proceedings
that may be initiated by our stockholders, and also provide that the federal district courts will be the exclusive forum for resolving
any complaint asserting a cause of action arising under the Securities Act, each of which could limit our stockholders’ ability to
choose the judicial forum for disputes with us or our directors, officers, stockholders or employees.
Our Charter provides that, subject to limited exceptions, the Court of Chancery for the State of Delaware or other specified courts in the
State of Delaware will be the sole and exclusive forum to the fullest extent of the law for:
• any derivative action or proceeding brought on our behalf;
• any action asserting a claim of breach of a fiduciary duty owed by any of our directors, officers or other employees to us
or our stockholders;
• any action asserting a claim against us arising pursuant to any provision of the Delaware General Corporation Law (the
“DGCL”), our Charter or our Bylaws;
• any action to interpret, apply, enforce or determine the validity of our Charter or Bylaws; and
• any other action asserting a claim against us that is governed by the internal affairs doctrine.
Our Charter also provides that the federal district courts of the United States of America will be the exclusive forum for the resolution
of any complaint asserting a cause of action against us or any of our directors, officers, employees or agents and arising under the
Securities Act. However, Section 22 of the Securities Act provides that federal and state courts have concurrent jurisdiction over lawsuits
brought pursuant to the Securities Act or the rules and regulations thereunder. To the extent the exclusive forum provision restricts the
courts in which claims arising under the Securities Act may be brought, there is uncertainty as to whether a court would enforce such a
provision. We note that investors cannot waive compliance with the federal securities laws and the rules and regulations thereunder.
This provision does not apply to claims brought under the Exchange Act.
Any person or entity purchasing or otherwise acquiring any interest in shares of our capital stock shall be deemed to have notice of and
to have consented to these provisions. These provisions may limit a stockholder’s ability to bring a claim in a judicial forum that it finds
favorable for disputes with us or our directors, officers or other employees, which may discourage such lawsuits against us and our
directors, officers and employees. Alternatively, if a court were to find these provisions of our Charter inapplicable to, or unenforceable
in respect of, one or more of the specified types of actions or proceedings, we may incur additional costs associated with resolving such
matters in other jurisdictions, which could adversely affect our business or financial condition.
Delaware law and provisions in our Charter and Bylaws might discourage, delay or prevent a change in control of the Company or
changes in our management and, therefore, depress the trading price of our Class A common stock.
Provisions of our Charter and Bylaws and of state law may delay, deter, prevent or render more difficult a takeover attempt that our
stockholders might consider in their best interests, including the following provisions:
• our dual-class common stock structure and the Voting Agreement, which provide our principal stockholders with a
majority of the voting power of our capital stock will enable our principal stockholders to influence the outcome of matters
submitted to our stockholders for approval even if they own significantly less than a majority of the number of shares of
our outstanding common stock;
• our Charter does not provide for cumulative voting in the election of directors;
• vacancies on our board of directors may be filled only by our board of directors and not by stockholders;
• our stockholders may act by written consent only so long as the Voting Agreement is in effect and our principal
stockholders hold a majority of the voting power of then-outstanding shares of our capital stock;
• a special meeting of our stockholders may only be called by the chairperson of our board of directors, our Chief Executive
Officer, our President, a majority of our board of directors or, so long as the Voting Agreement is in effect and our principal
stockholders hold a majority of the voting power of then-outstanding shares of our capital stock, our stockholders;
89
• amendments to certain provisions of our Charter and stockholder-proposed amendments to our Bylaws require the
affirmative vote of the holders of at least 66 2/3% in voting power of all the then outstanding shares of our capital stock
entitled to vote thereon at any time the Voting Agreement is not in effect or our principal stockholders do not hold, in the
aggregate, a majority of the voting power of then-outstanding shares of our capital stock;
• our Charter authorizes our board of directors, subject to the limitations imposed by Delaware law or the Nasdaq’s listing
rules, without any further vote or action by our stockholders, to issue preferred stock in one or more series and to fix the
designations, powers, preferences, limitations and rights of the shares of each series; and
• advance notice procedures apply for stockholders to nominate candidates for election as directors or to bring matters before
an annual meeting of stockholders.
Such provisions or laws may prevent our stockholders from receiving the benefit from any premium to the market price of our Class A
common stock offered by a bidder in a takeover context. Even in the absence of a takeover attempt, the existence of these provisions
may adversely affect the prevailing market price of our Class A common stock if they are viewed as discouraging takeover attempts in
the future.
Provisions in our Charter and Bylaws, including the dual-class structure of our common stock, might discourage or prevent
institutional investors from purchasing or holding our Class A common stock, and, therefore, depress the trading price of our Class
A common stock.
Our governance structure and our Charter may negatively affect the decision by certain institutional investors to purchase or hold shares
of our Class A common stock. The holding of low-voting stock, such as our Class A common stock, may not be permitted by the
investment policies of certain institutional investors or may be less attractive to the portfolio managers of certain institutional investors.
In addition, in July 2017, FTSE Russell and Standard & Poor’s announced that they would cease to allow most newly public companies
utilizing dual- or multi-class capital structures to be included in their indices. Affected indices include the Russell 2000 and the S&P
500, S&P MidCap 400 and S&P SmallCap 600, which together make up the S&P Composite 1500. Our dual-class common stock capital
structure may make us ineligible for inclusion in any of these and certain other indices, and as a result, mutual funds, exchange-traded
funds and other investment vehicles that attempt to passively track these indices would not invest in our stock. These policies may
depress our valuation compared to those of other similar companies that are included in such indices.
If securities or industry analysts do not publish research or publish inaccurate or unfavorable research about us, our business or
our market, or if they change their recommendation regarding our Class A common stock adversely, the trading price and trading
volume of our Class A common stock could decline.
The trading market for our Class A common stock will depend in part on the research and reports that securities or industry analysts
publish about us, our business, our market or our competitors. If no or few securities or industry analysts cover us, the price and trading
volume of our Class A common stock likely would be negatively impacted. If one or more of the securities or industry analysts who
cover us downgrade our Class A common stock or publish inaccurate or unfavorable research about us, the trading price of our Class A
common stock would likely decline. If analysts publish target prices for our Class A common stock that are below our then-current
public price of our Class A common stock, it could cause the trading price of our Class A common stock to decline significantly. Further,
if one or more of these analysts cease coverage of the Company or fail to publish reports on us regularly, demand for our Class A
common stock could decrease, which might cause our Class A common stock trading price and trading volume to decline.
General Risk Factors
We incur increased costs as a result of operating as a public company, and our management is required to devote substantial time
to new compliance initiatives.
As a public company, and particularly after we are no longer an “emerging growth company” or “smaller reporting company,” we will
incur significant legal, accounting and other expenses that we did not incur as a private company. In addition, the Sarbanes-Oxley Act
and rules subsequently implemented by the SEC and the Nasdaq impose various requirements on public companies, including
establishment and maintenance of effective disclosure and financial controls and corporate governance practices. Our management and
other personnel need to devote a substantial amount of time to these compliance initiatives. Moreover, these rules and regulations have
increased our legal and financial compliance costs and will make some activities more time- consuming and costly. For example, these
rules and regulations have made it more difficult and more expensive for us to obtain director and officer liability insurance.
Pursuant to Section 404, we are required to furnish a report by our management on our internal control over financial reporting, including
an attestation report on internal control over financial reporting issued by our independent registered public accounting firm. However,
while we remain an emerging growth company, we will not be required to include an attestation report on internal control over financial
reporting issued by our independent registered public accounting firm. To achieve compliance with Section 404 within the prescribed
90
period, we are engaged in a process to document and evaluate our internal control over financial reporting, which is both costly and
challenging. Further, despite our efforts, there is a risk that neither we nor our independent registered public accounting firm will be
able to conclude within the prescribed timeframe that our internal control over financial reporting is effective as required by Section
404. This could result in an adverse reaction in the financial markets due to a loss of confidence in the reliability of our financial
statements. In addition, if we are not able to continue to meet these requirements, we may not be able to remain listed on the Nasdaq.
Our internal controls over financial reporting are not currently effective and our independent registered public accounting firm may
not be able to certify as to their effectiveness, which could have a significant and adverse effect on our business and reputation.
Upon becoming a public company, we are now required to comply with the SEC’s rules implementing Sections 302 and 404 of the
Sarbanes-Oxley Act, which will require management to certify financial and other information in our quarterly and annual reports and
provide an annual management report on the effectiveness of internal control over financial reporting. Although we are required to
disclose changes that have materially affected, or are reasonably likely to materially affect, our internal control over financial reporting
on a quarterly basis, we will not be required to make our first annual assessment of our internal control over financial reporting pursuant
to Section 404 until at least our second annual report required to be filed with the SEC, and we are not required to have our independent
registered public accounting firm formally assess our internal controls for as long as we remain an “emerging growth company” as
defined in the JOBS Act.
When formally evaluating our internal controls over financial reporting, we have identified and may identify further material weaknesses
that we may not be able to remediate in time to meet the applicable deadline imposed upon us for compliance with the requirements of
Section 404 of the Sarbanes-Oxley Act. In addition, if we fail to achieve and maintain the adequacy of our internal controls, as such
standards are modified, supplemented or amended from time to time, we may not be able to ensure that we can conclude on an ongoing
basis that we have effective internal controls over financial reporting in accordance with Section 404 of the Sarbanes-Oxley Act. We
cannot be certain as to the timing of completion of our evaluation, testing and any remediation actions or the impact of the same on our
operations. If we are not able to implement the requirements of Section 404 of the Sarbanes-Oxley Act in a timely manner or with
adequate compliance, our independent registered public accounting firm may issue an adverse opinion due to ineffective internal controls
over financial reporting, and we may be subject to sanctions or investigation by regulatory authorities, such as the SEC. As a result,
there could be a negative reaction in the financial markets due to a loss of confidence in the reliability of our financial statements. In
addition, we may be required to incur additional costs in improving our internal control system and the hiring of additional personnel.
Any such action could have a significant and adverse effect on our business and reputation, which could negatively affect our results of
operations or cash flows.
Further, we believe that any disclosure controls and procedures or internal controls and procedures, no matter how well-conceived and
operated, can provide only reasonable, not absolute, assurance that the objectives of the control system are met. These inherent
limitations include the facts that judgments in decision-making can be faulty and that breakdowns can occur because of simple error or
mistake. Additionally, controls can be circumvented by the individual acts of some persons, by collusion of two or more people or by
an unauthorized override of the controls. Accordingly, because of the inherent limitations in our control system, misstatements due to
error or fraud may occur and not be detected.
We have identified material weaknesses in our internal control over financial reporting. If we are unable to remediate our existing
material weaknesses and otherwise develop and maintain an effective system of internal control over financial reporting, we may
not be able to accurately report our financial results or prevent fraud, and as a result, shareholders could lose confidence in our
financial and other public reporting, which would harm our business and the trading price of our Class A common stock.
Effective internal controls over financial reporting are necessary for us to provide reliable financial reports and, together with adequate
disclosure controls and procedures, are designed to prevent fraud. Any failure to implement required new or improved controls, or
difficulties encountered in their implementation, could cause us to fail to meet our reporting obligations. A material weakness is a
deficiency or a combination of deficiencies in internal control over financial reporting such that there is a reasonable possibility that a
material misstatement of our financial statements will not be prevented or detected on a timely basis.
During the preparation of our audited consolidated financial statements for the year ended December 31, 2021, we identified certain
errors in our previously issued financial statements that were determined not to be material. Further, as disclosed in Item 9A of this
Report, we identified material weaknesses in the design and operation of our internal control over financial reporting relating to
maintaining and performing our financial close process, ensuring that formal processes exist for identifying, analyzing and accounting
for complex, non-routine transactions and proper segregation of duties and responsibilities within our finance department. We are in
the process of implementing measures designed to improve internal control over financial reporting to remediate the control deficiencies
that led to these material weaknesses. We cannot assure you that we will be able to successfully remediate these material weaknesses or
other material weaknesses that may be discovered in the future. If we are unable to successfully remediate these issues or future issues
or if we fail to design and operate effective internal controls, it could result in material misstatements or omissions in our financial
statements and potentially require us to restate our financial statements, which may result in the trading value of our Class A common
stock being materially adversely affected.
91
If our estimates or judgments relating to our critical accounting policies are based on assumptions that change or prove to be
incorrect, our operating results could fall below our publicly announced guidance or the expectations of securities analysts and
investors, resulting in a decline in the market price of our Class A common stock.
The preparation of financial statements in conformity with U.S. generally accepted accounting principles (“GAAP”) requires
management to make estimates and assumptions that affect the amounts reported in our consolidated financial statements and
accompanying notes. We base our estimates on historical experience and on various other assumptions that we believe to be reasonable
under the circumstances, the results of which form the basis for making judgments about the carrying values of assets, liabilities, equity,
revenue and expenses that are not readily apparent from other sources. If our assumptions change or if actual circumstances differ from
our assumptions, our operating results may be adversely affected and could fall below our publicly announced guidance or the
expectations of securities analysts and investors, resulting in a decline in the market price of our Class A common stock.
Item 1B. Unresolved Staff Comments.
None.
Item 2. Properties.
Facilities
Our principal executive offices are located in Dallas, Texas, where we sublease 3,631 square feet of office space from UBI. UBI’s lease
for the premises is currently scheduled to terminate in January 2023. In addition to our principal executive offices, we have additional
offices in Florida and Taiwan. We do not currently own any real property. We believe that our current facilities are adequate to meet
our immediate needs and believe that we should be able to renew each of our leases and subleases without an adverse impact on our
operations. In addition, we believe that if we require additional office space or manufacturing facilities, we will be able to obtain
additional facilities on commercially reasonable terms.
Item 3. Legal Proceedings.
From time to time we are a party to various litigation matters incidental to the conduct of our business. We are not presently party to
any legal proceedings the resolution of which we believe would have a material adverse effect on our business, prospects, financial
condition, liquidity, results of operation, cash flows or capital levels.
Item 4. Mine Safety Disclosures.
The disclosure required by this item is not applicable.
92
PART II
Item 5. Market for Registrant’s Common Equity, Related Stockholder Matters and Issuer Purchases of Equity Securities.
Market Price for the Common Stock
Our Class A common stock is listed on the Nasdaq Global Market under the symbol “VAXX .” As of March 24, 2022, the number of
shares of our Class A common stock outstanding was 111 ,966,892 held by approximately 135 shareholders of record, not including
shareholders whose shares are held in securities position listings.
Our Class B common stock is not listed on any exchange nor traded on any public market. As of March 24, 2022, the number of shares
of our Class B common stock outstanding was 13,874,132 held by approximately 4 shareholders of record.
Dividends
We have never declared or paid, and do not anticipate declaring or paying in the foreseeable future, any cash dividends on our capital
stock. Any future determination to declare and pay cash dividends will be at the discretion of our board of directors in accordance with
applicable laws and will depend on, among other things, our financial condition, results of operations, cash requirements, contractual
restrictions and such other factors as our board of directors deems relevant. Our ability to pay dividends may also be limited by covenants
of any future outstanding indebtedness we or our subsidiaries incur.
Issuer Purchases of Equity Securities
We did not repurchase any shares during the years ended December 31, 2021, 2020, or 2019.
Unregistered Sales of Equity Securities
There were no unregistered sales of equity securities during the fourth quarter of 2021.
Use of Proceeds
On November 15, 2021, the Company closed its IPO, as discussed in Note 1 of our consolidated financial statements for the year ended
December 31, 2021. The aggregate net proceeds to us from the offering, after deducting underwriting discounts and commissions and
other offering expenses payable by us, was approximately $71.1 million. The proceeds from our IPO have been invested primarily in
money market accounts. There has been no material change in the expected use of the net proceeds from our IPO as described in our
prospectus filed pursuant to Rule 424(b)(4) under the Securities Act with the SEC on November 12, 2021.
Item 6. [Reserved].
Item 7. Management’s Discussion and Analysis of Financial Condition and Results of Operations.
The following discussion and analysis of our financial condition and results of operations should be read together with our
consolidated financial statements and related notes and other financial information appearing elsewhere in this Annual Report. We
intend for this discussion to provide you with information that will assist you in understanding our consolidated financial statements,
the changes in key items in those consolidated financial statements from year to year and the primary factors that accounted for those
changes.
Some of the information contained in this discussion and analysis or set forth elsewhere in this Annual Report, including
information with respect to our plans and strategy for our business and related financing, includes forward-looking statements that
involve risks, uncertainties and assumptions. See the section of this Annual Report titled “Special Note Regarding Forward-Looking
Statements” for a discussion of forward-looking statements. As a result of many factors, including those factors set forth in the “Risk
Factors” section of this Annual Report, our actual results could differ materially from management’s expectations and the results
described in or implied by the forward-looking statements contained in the following discussion and analysis.
Overview
Vaxxinity is engaged in the development and commercialization of rationally designed prophylactic and therapeutic vaccines to combat
chronic disorders and infectious diseases with large patient populations and unmet medical needs. While vaccines have traditionally
been unable to effectively and safely combat such disorders, we believe our platform could overcome the traditional hurdles facing
vaccines in this area. Our Vaxxine Platform relies on a synthetic peptide vaccine technology first developed by UBI and subsequently
refined over the last two decades. We believe our vaccines have the potential to combat conditions that have not yet been successfully
93
treated, or which have primarily been addressed with monoclonal antibodies (mAbs) which, while generally effective, are extremely
costly and cumbersome, and thus have limited accessibility. Our pipeline primarily consists of five programs focused on chronic disease,
particularly neurodegenerative disorders, in addition to other neurology and cardiovascular indications. Given the global COVID-19
pandemic and our Vaxxine Platform’s applicability to infectious disease, we are also opportunistically advancing product candidates
that address SARS-CoV-2.
We separated our business from UBI through two separate transactions: a spin-out from UBI in 2014 of operations focused on developing
chronic disease product candidates that resulted in UNS, and a second spin-out from UBI in 2020 of operations focused on the
development of a COVID-19 vaccine that resulted in COVAXX. On February 2, 2021, Vaxxinity was incorporated for the purpose of
reorganizing and combining UNS and COVAXX and did so on March 2, 2021 through the Reorganization. In connection with the
Reorganization, (i) all outstanding shares of UNS and COVAXX preferred stock and common stock were contributed to Vaxxinity and
exchanged for an aggregate of 57,702,458 shares of our Class A common stock, 10,999,149 shares of our Class B common stock and
58,175,751
were terminated and substituted with options to purchase an aggregate of 19,712,504 shares of our Class A common stock, (iii) the
outstanding warrant to purchase shares of COVAXX common stock was cancelled and exchanged for a warrant that is exercisable for
112,373 shares of our Class A common stock, and (iv) the outstanding Convertible Notes and the Related Note were contributed to
Vaxxinity and the former holders of such notes received an aggregate of
4,047,344
the Reorganization, COVAXX and UNS became our wholly-owned subsidiaries. All shares of our Series A preferred stock converted
into shares of our Class A common stock concurrently with the closing. The Reorganization was determined to be a common control
transaction, so the carrying values of all contributed assets and assumed liabilities remained unchanged and the financial information
for all periods in this section of the financial statements presented prior to the Reorganization are presented on consolidated basis.
COVA XX was incorporated on March 23, 2020, so periods prior to March 23, 2020 in this section of the financial statements only
reflect the historical financial information of UNS. Unless the context requires otherwise, in this section we use the terms “Vaxxinity,”
“we,” “us” and “our” to refer to our operations (including through UNS and COVAXX) both prior to and after the Reorganization.
Since our spin-out transactions from UBI, we have focused on organizing and staffing our business, business planning, raising capital,
developing our Vaxxine Platform, identifying and testing potential product candidates and conducting clinical trials. We have also
developed a SARS CoV-2 antibody ELISA test, which received an EUA from the FDA in January 2021.
Our current pipeline consists of six programs from early to late-stage development, including five programs focused on chronic disease.
Our neurodegenerative chronic disease program has three primary programs: UB-311, our leading neurology product candidate, which
targets AD; UB-312, which targets PD and other synucleinopathies; and an anti-tau product candidate which has the potential to address
multiple neurodegenerative conditions, including AD. Additionally, we have two other primary programs focused on chronic disease:
UB-313, which targets CGRP to prevent migraines; and our anti-PCSK9 program, which targets hypercholesterolemia to reduce the risk
of cardiac events. Through our Vaxxine Platform, we believe we may be able to address a wide range of other chronic diseases, including
chronic diseases that are or could potentially be successfully treated by mAbs, which increasingly dominate the treatment paradigm for
many chronic diseases.
In addition to our chronic disease pipeline, given our Vaxxine Platform’s applicability to infectious disease and the global need for
additional vaccines to address SARS-CoV-2, we are advancing an infectious disease product candidate. We have reported interim results
of our UB-612 Phase 1, Phase 2, and Phase 1 extension clinical trials. An EUA application for UB-612 was denied by the TFDA in
August 2021. We are appealing the TFDA’s decision in partnership with UBIA. At the same time, we are pursuing accelerated pathways
to authorization with regulators in multiple jurisdictions, including high income countries and LMICs, based on a heterologous booster
trial of UB-612 in the first half of 2022.
To date, our revenue has been generated from the modest sales of our ELISA test and the sale of an option to negotiate a license with
UNS (which option has expired). As a result, our ability to generate revenue sufficient to achieve profitability will depend on the eventual
regulatory approval, and commercialization of one or more of our product candidates. We have not yet obtained any regulatory approvals
for our product candidates or conducted sales and marketing activities for our product candidates.
We have principally funded our operations through financing transactions. Through December 31, 2021, we received gross proceeds of
$306.1 million in connection with various financial instruments, including the sale of preferred and common stock, the issuance of
promissory notes (including convertible promissory notes (“Convertible Notes”)), and the entry into simple agreements for future equity
(“SAFEs”).
Costs associated with research and development are the most significant component of our expenses. These costs can vary greatly from
period to period depending on the timing of various trials for our product candidates. We expect our allocated research and development
costs and general and administrative expenses to increase over time as we expand the number of product candidates that we are advancing
and incur increased costs as a result of operating as a public company. Further, we anticipate incurring greater selling and marketing
expenses if we commercialize any of our product candidates in the future. Our product candidates are in clinical stage or pre-clinical
stage development, and we have generated limited revenue to date and have incurred significant operating losses since inception. Net
losses were $137.2 million and $40.0 million for the years ended December 31, 2021 and 2020, respectively. As of December 31, 2021,
94
we had an accumulated deficit of $229.5 million. We expec
t our expenses and capital requirements will increase over time in connection
with our planned operations, which include:
•
continuing pre-clinical studies, existing clinical trials, or initiating new clinical trials for product candidates UB-311, UB-312,
UB-313, our COVID-19 product candidate and other product candidates;
•
advancing the development of our product candidate pipeline of other product candidates, including through business
development efforts to invest in or in-license other technologies or product candidates;
•
hiring additional clinical, quality control, medical, scientific and other technical personnel to support clinical and research and
development programs;
•
expanding operational, financial and management systems and infrastructure, expanding our facilities and increasing personnel
to support operations;
•
undertaking actions to meet the requirements and demands of being a public company;
•
maintaining, expanding and protecting our intellectual property portfolio;
•
seeking regulatory approvals for any product candidates that successfully complete clinical trials; and
•
undertaking pre-commercialization activities to establish sales, marketing and distribution capabilities for any product
candidates for which we may receive regulatory approval in regions where we elect to commercialize products on our own or
jointly with third parties.
As of the date of this Report, we expect our existing cash and cash equivalents will be sufficient to fund our operating expenses and
capital expenditure requirements for at least the next 12 months. We also believe that cash and cash equivalents will enable us to fund
our operating expenses and capital expenditure requirements into 2023. Thereafter, our viability will be dependent on our ability to raise
additional capital to finance operations, to successfully commercialize our product candidates and/or to enter into collaborations with
third parties for the development of our product candidates. If we are unable to do any of the foregoing, we would be forced to delay,
limit, reduce or terminate our product candidate development or future commercialization efforts. Our estimates are based on a variety
of assumptions that may prove to be wrong, and we could exhaust our available capital resources sooner than expected. See “— Liquidity
and Capital Resources.”
Business Update Regarding COVID-19 Pandemic
In March 2020, the World Health Organization declared the COVID-19 outbreak a pandemic. The onset of the pandemic led to our
institutional prioritization of COVID-19 vaccine development efforts, which correlated to a decline in research and development
expenditures for our chronic disease product candidates. To date, our operations have not been negatively impacted by the COVID-19
pandemic in a material manner. However, at this time, we cannot predict the specific extent, duration or full impact that the COVID-19
pandemic will have on our financial condition and operations, but the development of clinical supply materials could be delayed and
enrollment of patients in our studies may be delayed or suspended, as hospitals and clinics in areas where we are conducting trials shift
resources to cope with the COVID-19 pandemic and may limit access or close clinical facilities due to the COVID-19 pandemic.
Additionally, if our trial participants are unable to travel to our clinical study sites as a result of quarantines or other restrictions resulting
from the COVID-19 pandemic, we may experience higher drop-out rates or delays in our clinical studies. The impact of the COVID-19
pandemic on our financial performance will depend on future developments, including the duration and spread of the pandemic and
related governmental advisories and restrictions. These developments and the impact of the COVID-19 pandemic on the financial
markets and the overall economy are highly uncertain and cannot be predicted. If the financial markets and/or the overall economy are
impacted for an extended period, our results may be materially adversely affected. See “Risk Factors—Risks Related to Our Business
and Industry—The ongoing coronavirus pandemic has caused interruptions or delays of our business plan. Delays caused by the
coronavirus pandemic may have a significant adverse effect on our business.”
Components of Our Consolidated Results of Operations
Revenue
Revenue for the years ended December 31, 2021 and 2020 was $0.1 million and $0.6 million, respectively, and consisted of commercial
sales of our ELISA tests. While we continue to expect some revenue from sales of our ELISA tests, we do not expect to generate any
meaningful revenue unless and until we obtain regulatory approval of and commercialize our product candidates, and we do not know
when, or if, this will occur. If our development efforts for our product candidates are successful and result in commercialization, we
may generate additional revenue in the future from a combination of product sales or payments from collaboration or license agreements
95
that we have entered into or may enter into with third parties. See Risk Factors—Risks Related to the Discovery and Development of
Product Candidates. We have incurred significant losses since our inception. We expect to incur losses for the foreseeable future and
may never achieve or maintain profitability.
Cost of Revenue
Cost of revenue consists of kit production costs consisting of materials, labor and overhead expenses directly related to ELISA tests sold
and the costs of expired ELISA tests, which are not available for commercial sale.
If our development efforts in respect of our current pipeline of product candidates are successful and result in regulatory approval, we
expect our cost of revenue will increase in relative proportion to the level of our revenue as we commercialize the applicable product
candidate. We expect that cost of revenue will increase in absolute dollars as and if our revenue grows and will vary from period to
period as a percentage of revenue.
Research and Development Expenses
The design, initiation and execution of candidate discovery and development programs of our future potential product candidates is key
to our success and involves significant expenses. Prior to initiating these programs, project teams incorporating individuals from the
essential disciplines within Vaxxinity scope out the activities, timing, requirements, inclusion and exclusion criteria and the primary and
secondary endpoint. Once we have decided to proceed, our Vaxxine Platform enables the iteration of drug candidates in the discovery
phase through rapid, rational design and formulation. After we have identified drug candidates, the costs of scaling the formulation from
research grade to clinical grade, then to commercial grade, typically consumes significant resources. In addition, to internal research
and development, we utilize service providers, including related parties, to complete activities we do not have the internal resources to
handle.
Research and development expenses consist primarily of costs incurred for research activities, including drug discovery efforts and the
development of our product candidates. We expense research and development costs as incurred, which include:
•
expenses incurred to conduct the necessary preclinical studies and clinical trials required to obtain regulatory approval;
•
expenses incurred under agreements with CROs that are primarily engaged in the oversight and conduct of our clinical trials,
preclinical studies and drug discovery efforts and contract manufacturers that are primarily engaged to provide preclinical
and clinical drug substance and product for our research and development programs;
•
other costs related to acquiring and manufacturing materials in connection with our drug discovery efforts and preclinical
studies and clinical trial materials, including manufacturing validation batches, as well as investigative sites and consultants
that conduct our clinical trials, preclinical studies and other scientific development services;
•
payments made in cash or equity securities under third-party licensing, acquisition and option agreements;
•
employee-related expenses, including salaries and benefits, travel and stock-based compensation expense for employees
engaged in research and development functions;
•
costs related to compliance with regulatory requirements; and
•
facilities-related costs, depreciation and other expenses, which include rent and utilities.
We recognize external development costs based on an evaluation of the progress to completion of specific tasks using information
provided to us by service providers. This process involves reviewing open contracts and purchase orders, communicating with personnel
to identify services that have been performed on our behalf and estimating the level of service performed and the associated cost incurred
for the service when we have not yet been invoiced or otherwise notified of actual costs. Any nonrefundable advance payments that we
make for goods or services to be received in the future for use in research and development activities are recorded as prepaid expenses.
Such amounts are expensed as the related goods are delivered or the related services are performed, or until it is no longer expected that
the goods will be delivered or the services rendered, at which point the net remainder is expensed.
We are heavily reliant on related parties for the advancement of our research and development programs, including for manufacturing,
quality control, testing, validation, supply services, research support, development and clinical functions. During the years ended
December 31, 2021 and 2020, related party expenses were approximately 29% and 56% of our operating expenses, respectively. We
expect this reliance on related parties to diminish significantly in the future.
Where appropriate, we allocate our third-party research and development expenses on a program-by-program basis. These expenses
primarily relate to outside consultants, CROs, contract manufacturers and research laboratories in connection with pre-clinical
96
development, process development, manufacturing and clinical development activities. We do not allocate our internal costs, such as
employee costs, costs associated with our discovery efforts, laboratory supplies and facilities, including depreciation or other indirect
costs, to specific programs because these costs often relate to platform development, to multiple programs simultaneously or to discovery
of new programs, and any such allocation would necessarily involve significant estimates and judgments and, accordingly, would be
imprecise. When we refer to the research and development expenses associated with a specific program, these refer exclusively to the
allocated third-party expenses associated with that product candidate. All other research and development costs are referred to as
unallocated costs.
Product candidates in later stages of clinical development generally have higher development costs than those in earlier stages of clinical
development, primarily due to the increased size and duration of later-stage clinical trials. Additionally, greater research and
development overhead is required to support broader and more rapid development of our Vaxxine Platform and new product candidates.
As a result, we expect that our research and development expenses will increase as we continue our existing and planned clinical trials
and conduct increased pre-clinical and clinical development activities, including submitting regulatory filings for product candidates,
and focus more generally on the development of our chronic disease product candidates. A significant driver of such increases would
be the initiation of our Phase 2b trial for UB-311. We currently expect to initiate a Phase 2b early AD efficacy trial in the second half
of 2022. If we decide to advance UB-311 through the clinic without a strategic partner, our costs would increase more significantly than
if we engage a partner to fund the development of UB-311.
At this time, we cannot reasonably estimate or know the nature, timing and costs of the efforts that will be necessary to complete the
pre-clinical and clinical development of any of our product candidates or when, if ever, material net cash inflows may commence from
any of our product candidates
General and Administrative Expenses
General and administrative expenses consist primarily of salaries and benefits, travel and stock-based compensation expense for
personnel in executive, business development, finance, human resources, legal, information technology and administrative functions.
General and administrative expenses also include facility- related costs as well as insurance costs and professional fees for legal, patent,
consulting, investor and public relations, accounting and audit services and other general operating expenses not otherwise classified as
research and development expenses. We expense general and administrative costs as incurred.
We also anticipate that our general and administrative expenses will increase in the future as a result of increased costs associated with
being a public company. In each case these increases will likely include increased costs related to the hiring of additional personnel and
fees to outside consultants, personnel-related stock-based compensation costs, lawyers and accountants, among other expenses, and, in
the case of public company-related expenses, services associated with maintaining compliance with Nasdaq listing and SEC
requirements, director and officer liability insurance costs and investor and public relations costs.
Other Expense (Income)
Interest Expense
Interest expense consists of (i) interest expense recognized on the note payable entered into during June 2020 for the acquisition of an
airplane (the “2025 Note”), (ii) interest expense recognized on the Convertible Notes and (iii) interest expense recognized on other
promissory notes, including $0.1 million borrowed from our Chief Executive Officer (the “Executive Note”) and a related party
Convertible Note payable for $2.0 million in aggregate proceeds that was received in three tranches (the “2018 Related Notes”). The
Executive Note was repaid in full in August 2021 and the 2018 Related Notes were converted into Series A preferred stock concurrently
with the Reorganization.
Interest Income
Interest income consists of income earned on our cash and cash equivalents.
Change in Fair Value of Convertible Notes, SAFEs and Series A-1 Warrant Liability
We issued a series of Convertible Notes during the years ended December 31, 2018 through 2021, a series of SAFEs during the years
ended December 31, 2020 and 2021, and warrants to purchase shares of our Series A-1 preferred stock (“Series A-1 Warrants”) during
the year ended December 31, 2020, each of which were measured and accounted for at fair value. We remeasured the fair value of each
of the Convertible Notes, SAFEs and Series A-1 Warrants at each reporting date and recognize changes in the fair value in our
consolidated statements of operations. Inputs to the calculation of fair value generally include market and acquisition comparable(s) as
well as other variables. In connection with the Reorganization, all outstanding Convertible Notes, SAFEs, and Series A-1 Warrants were
exchanged for shares of Series A preferred stock, which were subsequently exchanged into shares of Class A common stock upon
closing of the IPO in November 2021.
97
Loss on Foreign Currency Translation, Net
Our foreign subsidiaries, which are wholly-owned by COVAXX and UNS, use the U.S. dollar as their functional currency and maintain
records in the local currency. Nonmonetary assets and liabilities are remeasured at historical rates and monetary assets and liabilities are
remeasured at exchange rates in effect at the end of the reporting period. Income statement accounts are remeasured at average exchange
rates for the reporting period. The resulting gains or losses are included in foreign currency (losses) gains in the consolidated financial
statements.
Provision for Income Taxes
We have not recorded any significant amounts related to income tax but have reserved $0.6 million of unrecognized tax benefits against
NOLs. We have not recorded any income tax benefits for the majority of our net losses we incurred to date.
We account for income taxes using the asset and liability method, which requires the recognition of deferred tax assets and liabilities
for the expected future tax consequences of events that have been included in the consolidated financial statements or our tax returns.
Deferred tax assets and liabilities are determined based on the difference between the financial statement carrying amounts and tax basis
of existing assets and liabilities and for loss and credit carryforwards, which are measured using the enacted tax rates and laws in effect
in the years in which the differences are expected to reverse. The realization of our deferred tax assets is dependent upon the generation
of future taxable income, the amount and timing of which are uncertain. Valuation allowances are provided, if, based upon the weight
of available evidence, it is more likely than not that some or all of the deferred tax assets will not be realized. As of December 31, 2021,
we continue to maintain a full valuation allowance against all of our deferred tax assets based on evaluation of all available evidence.
We file income tax returns in the U.S. federal and state jurisdictions and may become subject to income tax audit and adjustments by
related tax authorities. Our tax return periods (for entities then in existence) for U.S. federal income taxes for the tax years since 2017
remain open to examination under the statute of limitations by the Internal Revenue Service and state jurisdictions. We record reserves
for potential tax payments to various tax authorities related to uncertain tax positions, if any. The nature of uncertain tax positions is
subject to significant judgment by management and subject to change, which may be substantial. These reserves are based on a
determination of whether and how much a tax benefit taken by us in our tax filings or positions is more likely than not to be realized
following the resolution of any potential contingencies related to the tax benefit. We develop our assessment of uncertain tax positions,
and the associated cumulative probabilities, using internal expertise and assistance from third-party experts. As additional information
becomes available, estimates are revised and refined. Differences between estimates and final settlement may occur resulting in
additional tax expense. Potential interest and penalties associated with such uncertain tax positions is recorded as a component of our
provision for income taxes.
Factors Affecting the Comparability of Our Consolidated Results of Operations
On March 2, 2021, Vaxxinity entered into the Contribution and Exchange Agreement, pursuant to which the outstanding equity interests
of UNS and COVAXX were contributed to Vaxxinity in return for equity interests in Vaxxinity, resulting in UNS and COVAXX
becoming wholly owned subsidiaries of Vaxxinity. Accordingly, all share and per share amounts prior to the Reorganization have been
adjusted to reflect the Reorganization. In addition, we formed COVAXX, and commenced our COVAXX business, on March 23, 2020.
As a result, the historical financial information between March 23, 2020 and March 2, 2021 described in this Annual Report refers to
the combined historical financial information of UNS and COVAXX and the historical financial information prior to March 23, 2020
described in this Annual Report refers only to the historical financial information of UNS. Our operations for the year ended December
31, 2021 reflects the operations of UNS and COVAXX businesses on a consolidated basis for the period from January 1, 2021 to March
1, 2021 and of Vaxxinity and its subsidiaries for the remainder of that twelve-month period. Our business operations for year ended
December 31, 2020 reflects the operations of our UNS business from January 1, 2020 to March 22, 2020 and our UNS and COVAXX
businesses on a consolidated basis for the remainder of that twelve-month period. See Note 1 to our consolidated financial statements
included elsewhere in this Form 10-K filing.
Consolidated Results of Operations
Comparison of the Years Ended December 31, 2021 and 2020
The following table summarizes our consolidated results of operations for the years ended December 31, 2021 and 2020, together with
the dollar change in those items from year to year (in thousands):
98
Yea rs Ended December 31,
Change
2021
2020
$
%
Revenue
$
66
$
557
(491)
(88)%
Costs of revenue
1,937
52
1,885
3624%
Gross (loss) profit
(1,871)
505
2,376
470%
Operating expenses:
Research and development
71,379
20,570
50,809
247%
General and administrative
51,825
12,217
39,608
324%
Total operating expenses
123,204
32,787
(90,417)
(276)%
Loss from operations
(125,075)
(32,282)
(92,793)
287%
Other (income) expense:
Interest expense
840
1,182
(342)
(29)%
Interest income
(9)
(1)
(8)
838%
Change in fair value of convertible notes
2,667
5,761
(3,094)
(54)%
Change in fair value of simple agreements for future equity
8,365
615
7,750
1260%
Change in fair value of warrant liability
214
41
173
422%
Loss on foreign currency translation, net
23
77
(54)
(70)%
Other (income) expense, net
12,100
7,675
(4,425)
(58)%
Net loss
$
(137,175)
$
(39,957)
(97,218)
243%
Revenue
Total revenue was $0.1 million and $0.6 million for the years ended December 31, 2021 and 2020, respectively. All revenue and
comparable decreases were due to sales of our ELISA tests. We are not actively pursuing commercialization of our ELISA tests at this
time.
Gross Margin
The gross margin for the year ended December 31, 2021 was negative however the sales volume was de minimis. During the year ended
December 31, 2021, we wrote off , to cost of revenue, $1.9 million in expired ELISA tests that had no commercial value, driving a
significant change in gross profit percentage.
Research and Development Expenses
Research and development expenses were $71.4 million and $20.6 million for the years ended December 31, 2021 and 2020,
respectively. The $50.8 million increase was primarily due to an increase of $42.6 million in costs related to UB-612, primarily
consisting of materials and manufacturing costs and CRO costs associated with our ongoing clinical trial in Taiwan, which program was
only in early development in the corresponding 2020 period. The remaining $8.2 million increase was driven by an increase in
unallocated costs of $6.2 million, resulting primarily from increased salaries and personnel-related costs in connection with our UB-612
development efforts, as well as an increase in other allocated costs driven primarily by pre-clinical activities for our UB-313 program.
General and Administrative Expenses
General and administrative expenses were $51.8 million and $12.2 million for the years ended December 31, 2021 and 2020,
respectively. The $39.6 million increase was primarily due to a $28.3 million increase in stock-based compensation expense, including
$23.1 million related to performance-based grants that vested upon the successful completion of the Company’s initial public offering
in November 2021. The remaining $11.3 million increase was due to increased salaries and personnel-related costs and professional
services costs related to our continued organizational growth to support our ramp-up in research and development efforts, as well as
increased costs for preparations for being a public company.
Interest Expense
Interest expense was $0.8 million and $1.2 million for the years ended December 31, 2021 and 2020, respectively. The $0.3 million
decrease was due to the exchange of Convertible Notes for Series A preferred stock in connection with the Reorganization.
Interest Income
99
Interest income on cash was less than $0.1 million for each of the years ended December 31, 2021 and 2020.
Change in Fair Value of Convertible Notes, SAFEs and Series A-1 Warrant Liability
The decrease in the change in fair value of the Convertible Notes of $3.1 million for the year ended December 31, 2021 was primarily
related to the revaluation of the Convertible Notes upon conversion to equity. The increase in the change in fair value of SAFEs of $7.8
million for the year ended December 31, 2021 compared to the year ended December 31, 2020 was primarily related to insight into the
pricing of Vaxxinity’s next stock issuance at a higher valuation. The increase in the change in fair value of Series A-1 Warrants of $0.2
million for the year ended December 31, 2021 compared to the year ended December 31, 2020 was primarily related to an increase in
value of the Series A-1 preferred stock. In connection with the Reorganization, all outstanding Convertible Notes, SAFEs and Series A-
1 Warrants were exchanged into shares of Series A preferred stock, which were subsequently exchanged into shares of Class A common
stock upon the closing of the IPO in November 2021 as described in Note 8 to our consolidated financial statements included elsewhere
in this Report.
Loss on Foreign Currency Translation, Net
The net loss of foreign currency translation reflected a de minimis increase in the foreign exchange rate for the year ended December
31, 2021 compared to the year ended December 31, 2020.
Liquidity and Capital Resources
Sources of Liquidity
We have generated limited revenue from sales of our ELISA tests and have not yet commercialized any of our product candidates, which
are in various phases of pre-clinical and clinical development. We have financed operations primarily through the issuance of convertible
preferred stock, borrowings under promissory notes (including Convertible Notes) and the execution of SAFEs. Through December 31,
2020, we received gross proceeds of $99.3 million in connection with the issuance of various financial instruments, including the sale
of preferred stock, the issuance of promissory notes (including Convertible Notes), and the execution of SAFEs. In addition, we also
generated revenue from the sale of an option to negotiate a license with UNS (which option has expired) and the sales of ELISA tests
in 2020 and 2021. During the year ended December 31, 2021, we raised a total of $198.8 million, which consisted of $71.1 million in
net proceeds from the issuance of common stock in connection with the IPO, $122.8 million in net proceeds from the issuance of Series
B preferred shares, $2.0 million in net proceeds from the issuance of convertible debt, and $2.9 million in net proceeds from the issuance
of SAFEs. At December 31, 2021, we had $144.9 million in cash and cash equivalents, compared to $31.1 million as of December 31,
2020. The increase in cash and cash equivalents balances for the periods reported are primarily due to the factors described under “Cash
Flows” below.
Cash Flows
The following table provides information regarding our cash flows for the years ended December 31, 2021 and 2020 (in thousands):
Years Ended December 31,
2021
2020
Balance Sheet Data:
Cash and cash equivalents
144,885
31,143
Restricted cash
172
55
Total assets
166,673
50,141
Total liabilities
38,054
75,041
Total stockholders' equity (deficit)
128,619
(87,375)
Statement of Cash Flow Data:
Net cash flows used in operating activities
$
(80,990)
$
(33,910)
Net cash flows used in investing activities
(1,318)
(1,477)
Net cash flows provided by financing activities
196,167
66,109
Net increase in cash, cash equivalents and restricted cash
$
113,859
$
30,722
Operating Activities
Net cash used in operating activities for the year ended December 31, 2021 was $81.0 million, primarily due to a $137.2 million net
loss, offset by a favorable $12.9 million change in operating assets and liabilities and total non-cash items of $43.3 million. The cash
flow impact from changes in net operating assets and liabilities were primarily due to $11.4 million in amounts due to related party as
well as $3.9 million related to accrued expense, accounts payable and other liabilities. These increases were offset by $4.7 million in
100
prepaid expenses for UB-612 production. The primary non-cash adjustments to net loss included an $11.2 million change in the fair
market value of financial instruments as well as $30.4 million of stock-based compensation and $1.1 million in depreciation.
Investing Activities
Net cash used in investing activities totaled $1.3 million for the year ended December 31, 2021. The cash used in investing activities
consisted primarily of the acquisition of equipment.
Financing Activities
Net cash provided by financing activities totaled $196.2 million for the year ended December 31, 2021. We raised capital to support our
operations through the issuance of Class A Common Stock upon IPO, with net proceeds of $71.1 million, the issuance prior to the
Reorganization of SAFEs and Convertible Notes, with net proceeds of $2.9 million and $2.0 million, respectively, as well as the issuance
of Series B convertible preferred stock, with net proceeds of $122.8 million. We also repaid $2.0 million in relation to a Convertible
Note, $0.1 million in relation to a note payable with related party, $0.3 million in repayment for Paycheck Protection Program, and $0.4
million in relation to a note payable entered into for the acquisition of an Airplane.
Funding Requirements
We have generated approximately $3.7 million in revenue since inception and have incurred net losses in each reporting period since
inception. We do not expect to generate any meaningful revenue unless and until we obtain regulatory approval of and commercialize
our product candidates. We do not know when, or if, this will occur. If we do not receive regulatory approval for any of our product
candidates, or if we receive approval but our commercialization results fall short of our expectations, we will continue to incur significant
losses for the foreseeable future, and we expect the losses to increase as we continue the development of, and seek regulatory approvals
for, our product candidates and begin to commercialize any approved products.
As of the date of this Annual Report, we expect our existing cash and cash equivalents will be sufficient to fund our operating expenses
over the next 12 months. As of December 31, 2021, other than our 2025 Note, we have no material debt obligations.
We have based our projections of operating capital requirements on assumptions that may prove to be incorrect, and we may use all of
our available capital resources sooner than we expect. Our future capital requirements will depend on many factors, which include:
•
the number of discovery and pre-clinical programs that we pursue and the speed with which they are advanced;
•
the number, size, and nature of clinical trials that we conduct;
•
the length of time it takes for regulators to review and approve any product candidates that successfully complete clinical
trials;
•
the timing and manner in which we manufacture our pre-clinical and clinical drug material, the terms on which we can have
such manufacturing completed, and the extent to which we undertake commercialization of any drug products, if approved;
•
the extent to which we establish sales, marketing, medical affairs and distribution infrastructure to commercialize any product
candidates;
•
the timing and extent to which we expand our operational, financial and management systems and infrastructure, and
facilities;
•
the timing and extent to which we increase our personnel to support operations, including necessary increases in headcount to
conduct and expand our clinical trials, commercialize any approved products and support our operations as a public
company; and
•
the number of patent applications we must file and claims we must defend in order to maintain, expand and protect our
intellectual property portfolio, and the costs of preparing, filing and prosecuting patent applications, maintaining and
protecting our intellectual property rights.
Until such time, if ever, as we can generate positive cash flows from operations, we expect to finance our cash needs through public or
private equity offerings, strategic collaborations and debt financing. To the extent that we raise additional capital through the sale of our
Class A common stock, convertible securities or other equity securities, shareholders’ ownership interest will be diluted and the terms
of these securities could include liquidation or other preferences and anti-dilution protections. In addition, debt financing, if available,
101
may result in fixed payment obligations and may involve agreements that include restrictive covenants that limit our ability to take
specific actions, such as incurring additional debt, making capital expenditures, creating liens, redeeming shares or declaring dividends.
If we raise additional funds through strategic collaborations or marketing, distribution or licensing arrangements with third parties, we
may have to relinquish valuable rights to our technologies, future revenue streams or product candidates or grant licenses on terms that
may not be favorable to us. If we are unable to raise additional funds when needed, we may be required to delay, limit, reduce or
terminate our product candidate development or future commercialization efforts or grant rights to third parties to develop and market
product candidates that we would otherwise prefer to develop and market ourselves.
Contract Research and Manufacturing Organizations
We recorded accrued expenses of $4.5 million and $0.3 million in our balance sheet for expenditures incurred by CROs and contract
manufacturers as of December 31, 2021 and 2020, respectively.
Tax-Related Obligations
We have reserved $0.6 million of unrecognized tax benefits against NOLs. Additionally, as of December 31, 2021, we accrued $0.2
million in interest and penalties related to prior year tax filings.
Off-Balance Sheet Arrangements
We did not have during the periods presented, and do not currently have, any off-balance sheet arrangements, as defined in the rules and
regulations of the SEC.
Critical Accounting Policies and Estimates
The preparation of financial statements in accordance with GAAP requires management to make estimates and assumptions that affect
the amounts reported in our consolidated financial statements and accompanying notes. Management bases its estimates on historical
experience, market and other conditions, and various other assumptions it believes to be reasonable. Although these estimates are based
on management’s best knowledge of current events and actions that may impact us in the future, the estimation process is, by its nature,
uncertain given that estimates depend on events over which we may not have control. In addition, if our assumptions change, we may
need to revise our estimates, or take other corrective actions, either of which may also have a material effect on our consolidated financial
statements. Significant estimates contained within these consolidated financial statements include, but are not limited to, the estimated
fair value of our common stock, convertible notes payable and SAFEs, stock-based compensation, warrant liabilities, income tax
valuation allowance and the accruals of research and development expenses. We base our estimates on historical experience, known
trends and other market-specific or other relevant factors that we believe to be reasonable under the circumstances. On an ongoing basis,
management evaluates its estimates, as there are changes in facts and circumstances. If market and other conditions change from those
that we anticipate, our consolidated financial statements may be materially affected.
While our significant accounting policies are described in more detail in the notes to our consolidated financial statements appearing
elsewhere in this Annual Report, we believe that the following critical accounting policies and estimates have a higher degree of inherent
uncertainty and require our most significant judgments.
Accrued Research and Development Expenses
As part of the process of preparing our consolidated financial statements, we are required to estimate accrued research and development
expenses. As we advance our programs, we anticipate more complex clinical studies resulting in greater research and development
expenses, which will place even greater emphasis on the accrual. This process involves reviewing open contracts and purchase orders,
communicating with our applicable personnel to identify services that have been performed on our behalf and estimating the level of
service performed and the associated cost incurred for the service when we have not yet been invoiced or otherwise notified of actual
costs. The majority of our service providers invoice in arrears for services performed, on a pre-determined schedule or when contractual
milestones are met; however, some require advance payments. We make estimates of accrued expenses as of each balance sheet date in
the consolidated financial statements based on facts and circumstances known to us at that time. We periodically confirm the accuracy
of the estimates with the service providers and make adjustments if necessary. Examples of estimated accrued research and development
expenses include fees paid to:
•
vendors, including research laboratories, in connection with pre-clinical development activities;
•
CROs and investigative sites in connection with pre-clinical studies and clinical trials; and
•
contract manufacturers in connection with drug substance and drug product formulation of pre-clinical studies and clinical
trial materials.
102
We base our expenses related to pre-clinical studies and clinical trials on our estimates of the services received and efforts expended
pursuant to quotes and contracts with multiple research institutions and CROs that supply, conduct and manage pre-clinical studies and
clinical trials on our behalf. The financial terms of these agreements are subject to negotiation, vary from contract to contract and may
result in uneven payment flows. There may be instances in which payments made to our vendors will exceed the level of services
provided and result in a prepayment of the expense. Payments under some of these contracts depend on factors such as the successful
enrollment of patients and the completion of clinical trial milestones. In accruing service fees, we estimate the time period over which
services will be performed and the level of effort to be expended in each period. If the actual timing of the performance of services or
the level of effort varies from the estimate, it adjusts the accrual or the prepaid expense accordingly. Although we do not expect our
estimates to be materially different from amounts actually incurred, our understanding of the status and timing of services performed
relative to the actual status and timing of services performed may vary and may result in reporting amounts that are too high or too low
in any particular period. To date, our estimated accruals have not differed materially from actual costs incurred.
Stock-Based Compensation
We measure all stock-based awards granted to employees, directors and non-employees based on their fair value on the date of the grant
and recognize the corresponding compensation expense of those awards over the requisite service period, which is generally the vesting
period of the respective award. Forfeitures are accounted for as they occur. We grant stock options and restricted stock awards that are
subject to service vesting conditions.
We classify stock-based compensation expense in our consolidated statements of operations in the same manner in which the award
recipient’s payroll costs are classified or in which the award recipient’s service payments are classified.
We estimate the fair value of each stock option grant using the Black-Scholes option-pricing model, which requires the use of subjective
assumptions that could materially impact the estimation of fair value and related compensation expense to be recognized. These
assumptions include (i) the expected volatility of our stock price, (ii) the periods of time over which recipients are expected to hold their
options prior to exercise (expected lives), (iii) expected dividend yield on our common stock, and (iv) risk-free interest rates, which are
based on quoted U.S.Treasury rates for securities with maturities approximating the options’ expected lives. Developing these
assumptions requires the use of judgment. Both prior to and after the IPO, we lacked company-specific historical and implied volatility
information. Therefore, we estimate our expected stock volatility based on the historical volatility of a publicly traded set of peer
companies. The expected term of the Company’s options has been determined utilizing the “simplified” method for awards that qualify
as “plain-vanilla” options. The expected term of options granted to non-employees is equal to the contractual term of the option award.
The expected dividend yield is zero as we have never paid dividends and do not currently anticipate paying any in the foreseeable future.
Determination of the Fair Value of Common Stock
Before there was a public market for our common stock, the estimated fair value of common stock was determined by its most recently
available third-party valuations of common stock. These third- party valuations were performed in accordance with the guidance outlined
in the American Institute of Certified Public Accountants’ Accounting and Valuation Guide, Valuation of Privately-Held-Company
Equity Securities Issued as Compensation. Our common stock valuations were prepared using an option pricing method (“OPM”). The
OPM treats common stock and preferred stock as call options on the total equity value of a company, with exercise prices based on the
value thresholds at which the allocation among the various holders of a company’s securities changes. Under this method, the common
stock has value only if the funds available for distribution to stockholders exceeded the value of the preferred stock liquidation
preferences at the time of the liquidity event, such as a strategic sale or a merger. A discount for lack of marketability of the common
stock is then applied to arrive at an indication of value for the common stock.
In addition to considering the results of these third-party valuations, our board of directors considered various objective and subjective
factors to determine the fair value of our common stock as of each grant date, including:
•
the prices at which we sold shares of preferred stock and the superior rights and preferences of the preferred stock relative to
our common stock at the time of each grant;
•
the progress of our research and development programs, including the status and results of pre-clinical studies and clinical
trials for our product candidates;
•
our stage of development and commercialization and our business strategy;
•
external market conditions affecting the biopharmaceutical industry and trends within the biopharmaceutical industry;
•
our financial position, including cash on hand, and our historical and forecasted performance and results of operations;
103
•
the lack of an active public market for our common stock and our preferred stock;
•
the likelihood of achieving a liquidity event, such as an initial public offering or our sale in light of prevailing market
conditions; and
•
the analysis of initial public offerings and the market performance of similar companies in the biopharmaceutical industry.
The assumptions underlying these valuations represented management’s best estimate, which involved inherent uncertainties and the
application of management’s judgment. As a result, if we had used significantly different assumptions or estimates, the fair value of our
common stock and our stock-based compensation expense could have been materially different.
Once a public trading market for our common stock has been established for a sufficient period of time, it will no longer be necessary
to estimate the fair value of our common stock in connection with its accounting for granted stock options and other such awards we
may grant, as the fair value of our common stock will be determined based on the quoted market price of our common stock.
Awards Granted
The following table sets forth information on stock options awarded to employees since January 1, 2019:
Grant Date
Number of
shares subject
to award
Per share
exercise price
of options
Per share fair value
of common stock on
grant date
Per share estimated
fair value of award
on grant date
December 30, 2019
1,139,717
$0.57
$0.64
$0.40
August 22, 2020
1,984,553
$1.21
$1.65
$0.75
August 24, 2020
521,406
$1.21
$1.65
$0.75
September 2, 2020
160,161
$0.57
$1.43
$1.18
January 26, 2021
9,043,916
$4.12
$4.12
$2.26
February 11, 2021
1,404,291
$4.01
$4.01
$2.53
June 16, 2021
690,266
$4.81
$4.81
$3.59
July 16, 2021
282,776
$4.81
$4.81
$3.63
July 28, 2021
562,605
$10.07
$10.07
$7.47
November 11, 2021
1,499,085
$13.00
$13.00
$9.77
Simple Agreement for Future Equity
During the years ended December 31, 2021 and 2020, we entered into SAFEs. The SAFEs were not mandatorily redeemable, nor did
they require us to repurchase a fixed number of shares. We determined that the SAFEs contained a liquidity event provision that
embodied an obligation indexed to the fair value of the equity shares and could require us to settle the SAFE obligation by transferring
assets or cash. Our SAFEs represented a recurring measurement that is classified within Level 3, disclosed and defined in Note 3 to our
consolidated financial statements included elsewhere in this Report, of the fair value hierarchy wherein fair value is estimated using
significant unobservable inputs, including an estimate of the number of months to a liquidity event, volatility rates and the estimation
of the most likely conversion feature for converting the SAFE.
The fair value of the SAFEs on the date of issuance was determined to equal the proceeds we received. The value of the SAFEs on the
date of conversion into Series A preferred stock was determined to be equal to the fair value of the Series A preferred stock issued in
connection with the Reorganization.
Convertible Notes
Beginning in 2018, we issued Convertible Notes that bore simple interest at annual rates ranging from 4.8% to 6%. All unpaid principal,
together with the accrued interest thereon, for the Convertible Notes were payable upon the event of default or upon maturity, which
ranged from one to three years. The Convertible Notes contained a number of provisions addressing automatic and optional conversion,
events of default and prepayment provisions. We determined that a portion of the Convertible Notes contained a liquidity event
provision, requiring them to be measured and accounted for at fair value at each reporting date. We determined the Convertible Notes
requiring a measurement to fair value represented a recurring measurement that was classified within Level 3, disclosed and defined in
Note 3 to our consolidated financial statements included elsewhere in this Annual Report, of the fair value hierarchy wherein fair value
is estimated using significant unobservable inputs.
104
Taiwan Centers for Disease Control Grant
UBIA, which is responsible for applying for and managing grants on our behalf, was awarded a grant by the Taiwan Centers for Disease
Control (“TCDC”) for COVID-19 vaccine development. The grant provides that costs incurred to complete the two phases of the clinical
trial will be reimbursed based on the achievement of certain milestones as defined in the agreement. We are entitled to reimbursement
under the TCDC grant. At each reporting date, we assess the status of all of the activities involved in completing the clinical study in
relation to the milestones. We account for the amounts that have been received from the TCDC to reimburse costs incurred on the
clinical study and not expected to be refunded back to the TCDC as contra research and development expenses in the accompanying
consolidated statement of operations.
Item 7A. Quantitative and Qualitative Disclosures About Market Risk.
We are exposed to market risk in the ordinary course of our business. These risks primarily relate to foreign currency and changes in
interest rates.
Foreign Currency Exchange Risk
We have limited exposure to foreign currency exchange risk as most of our operating activities are primarily denominated in U.S.
dollars. We believe actual foreign exchange gains and losses did not have a significant impact on our results of operations for any periods
presented herein. The results of the analysis based on our financial position as of December 31, 2021, indicated that a hypothetical 10%
increase or decrease in applicable foreign currency exchange rates would not have a material effect on our financial results.
Interest Rate Risk
We are exposed to market risk related to changes in interest rates. As of December 31, 2020 and 2021, our cash equivalents consisted
of interest-bearing checking accounts and money market accounts. We issued Convertible Notes, which Convertible Notes were
exchanged for Series A preferred stock in connection with the Reorganization. The Convertible Notes bore simple interest at the annual
rates ranging from 4.8% to 6%, with redemption terms payable at the earlier of one year, or upon the event of default. In addition, the
Convertible Notes contained provisions addressing automatic and optional conversion. Given the redemption of the Convertible Notes,
and the short-term nature and fixed interest rate, we believe there is no material exposure to interest rate risk. Additionally, the 2025
Note we entered into for the year ended December 31, 2020 bears an annual interest rate of 3.4% and matures in June 2025. Given the
fixed interest rate of the 2025 Note, we believe there is no material exposure to interest rate risk. The results of the analysis based on
our financial position as of December 31, 2021, indicated that a hypothetical 100 basis point increase or decrease in risk-free rates would
not have a material effect on our financial results.
Our measurement of interest rate risk involves assumptions that are inherently uncertain and, as a result, cannot precisely estimate the
impact of changes in interest rates on net interest revenues. Actual results may differ from simulated results due to balance growth or
decline and the timing, magnitude, and frequency of interest rate changes, as well as changes in market conditions and management
strategies, including changes in asset and liability mix.
105
Item 8. Financial Statements and Supplementary Data
VAXXINITY, INC.
INDEX TO FINANCIAL STATEMENTS
Audited Consolidated Financial Statements as of and for the years ended December 31, 2021 and 2020
)
106
107
108
109
111
113
106
REPORT OF INDEPENDENT REGISTERED PUBLIC ACCOUNTING FIRM
The Board of Directors and Stockholders
Vaxxinity, Inc. Dallas, Texas
Opinion on the Consolidated Financial Statements
We have audited the accompanying consolidated balance sheets of Vaxxinity, Inc. and Subsidiaries (collectively the “Company”) as of
December 31, 2021 and 2020, and the related consolidated statements of operations, convertible preferred stock and stockholders’ equity
(deficit), and cash flows for each of the years in the two-year period ended December 31, 2021, and the related notes (collectively
referred to as the “consolidated financial statements”).
In our opinion, the consolidated financial statements present fairly, in all material respects, the consolidated financial position of the
Company as of December 31, 2021 and 2020, and the results of their operations and cash flows for each of the two years in the period
ended December 31, 2021, in conformity with U.S. generally accepted accounting principles.
Basis for Opinion
The Company’s management is responsible for these consolidated financial statements. Our responsibility is to express an opinion on
the Company’s consolidated financial statements based on our audits. We are a public accounting firm registered with the Public
Company Accounting Oversight Board (United States) (the “PCAOB”) and are required to be independent with respect to the Company
in accordance with the U.S. federal securities laws and the applicable rules and regulations of the Securities and Exchange Commission
and the PCAOB.
We conducted our audits in accordance with the standards of the PCAOB. Those standards require that we plan and perform the audit
to obtain reasonable assurance about whether the consolidated financial statements are free of material misstatement, whether due to
error or fraud. The Company is not required to have, nor were we engaged to perform, an audit of its internal control over financial
reporting. As part of our audits we are required to obtain an understanding of internal control over financial reporting but not for the
purpose of expressing an opinion on the effectiveness of the Company’s internal control over financial reporting. Accordingly, we
express no such opinion.
Our audits included performing procedures to assess the risks of material misstatement of the consolidated financial statements, whether
due to error or fraud, and performing procedures that respond to those risks. Such procedures included examining, on a test basis,
evidence regarding the amounts and disclosures in the consolidated financial statements. Our audits also included evaluating the
accounting principles used and significant estimates made by management, as well as evaluating the overall presentation of the
consolidated financial statements. We believe that our audits provide a reasonable basis for our opinion.
We have served as the Company’s auditor since 2018.
/s/
March 24, 2022
107
VAXXINITY, INC.
CONSOLIDATED BALANCE SHEETS
(in thousands, except share and per share amounts)
December 31,
2021
2020
Assets
Current assets:
Cash and cash equivalents
$
$
Accounts receivable
Amounts due from related parties
Prepaid expenses and other current assets
Total current assets
Deferred offering costs
Property and equipment, net
Long-term prepaid fixed assets
199
—
Restricted cash
Total assets
$
$
Liabilities, convertible preferred stock, and stockholders’ equity (deficit)
Current liabilities:
Accounts payable
$
$
Amounts due to related parties
Accrued expenses and other current liabilities
Notes payable
Notes payable with related parties
Convertible notes payable
Convertible notes with related parties, net of discount
Total current liabilities
Other liabilities
Simple agreement for future equity
Notes payable, net of current portion
Warrant liability
Other long-term liabilities
Total liabilities
Commitments and contingencies (Note 16)
Preferred stock: $
respectively
Convertible preferred stock:
Series seed stock, 0 and
liquidation preference $0 and $
Series seed-1 stock,
December 31, 2021 and 2020, respectively; liquidation preference $0 and $
respectively
Series seed-2 stock, 0 and
respectively; liquidation preference $0 and $
Series A-1 stock, 0 and
31, 2021 and 2020, respectively; liquidation preference $0 and $
Series A-2 stock, 0 and
respectively; liquidation preference $0 and $
Series A stock, 0 shares designated, issued and outstanding at December 31, 2021 and 2020; liquidation preference $0
at December 31, 2021 and 2020
Series B stock, 0 shares designated, issued and outstanding at December 31, 2021 and 2020; liquidation preference $0
at December 31, 2021 and 2020
Total convertible preferred stock
Stockholders’ equity (deficit):
Class A common stock, $
shares issued and outstanding at December 31, 2021 and 2020, respectively
Class B common stock, $
shares issued and outstanding at December 31, 2021 and 2020, respectively
Class A treasury stock, par value of $
0.0001
; 0
0
(23 )
Additional paid-in capital
Accumulated deficit
(229,481 )
(92,306 )
Total stockholders’ equity (deficit)
(87,375 )
Total liabilities, convertible preferred stock, and stockholders’ equity (deficit)
$
$
The accompanying notes are an integral part of the consolidated financial statements.
108
VAXXINITY, INC.
CONSOLIDATED STATEMENTS OF OPERATIONS
(in thousands, except share and per share amounts)
Years Ended December 31,
2021
2020
Revenue
$
$
Cost of revenue
Gross (loss) profit
(1,871 )
Operating expenses:
Research and development
General and administrative
Total operating expenses
Loss from operations
(125,075 )
(32,282 )
Other (income) expense:
Interest expense
Interest income
(9)
(1)
Change in fair value of convertible notes
Change in fair value of simple agreement for future equity
Change in fair value of warrant liability
Loss on foreign currency translation, net
Other (income) expense
Loss before income taxes
(137,175 )
(39,957 )
Provision for income taxes
Net loss
$
(137,175 )
$
(39,957 )
Net loss per share, basic and diluted
$
(1.79 )
$
(0.61 )
Weighted average common shares outstanding, basic and diluted
The accompanying notes are an integral part of the consolidated financial statements.
109
VAXXINITY, INC.
CONSOLIDATED STATEMENTS OF CONVERTIBLE PREFERRED STOCK
(in thousands, except share amounts)
Convertible Preferred Stock
Series Seed
Series Seed-1
Series Seed-2
Series A-1
Series A-2
Series A
Series B
Shares
Amount
Shares
Amount
Shares
Amount
Shares
Amount
Shares
Amount
Shares
Amount
Shares
Amount
Total
Balance at December 31, 2019
$
$
$
$
$
—
$
—
—
$
—
$
Issuance of Series Seed-1 preferred stock, net of issuance costs
of $18
—
—
—
—
—
—
—
—
—
—
—
—
Issuance of Series Seed-2 preferred stock, net of issuance costs
of $45
—
—
—
—
—
—
—
—
—
—
—
—
Conversion of Simple Agreement for Future Equity to Series
Seed-2 preferred stock
—
—
—
—
—
—
—
—
—
—
—
—
Issuance of Series A-1 preferred stock, net of issuance costs of
$585
—
—
—
—
—
—
—
—
—
—
—
—
Exercise of warrants for Series A-1 preferred stock
—
—
—
—
—
—
—
—
—
—
—
—
Conversion of Simple Agreement for Future Equity to Series
A-2 preferred stock, net of issuance costs of $41
—
—
—
—
—
—
—
—
—
—
—
—
Balance at December 31, 2020
$
$
$
$
$
$
$
$
Exchange of Series Seed, Series Seed-1, Series Seed-2, Series
A-1 and Series A-2 for Series A
(7,831,528 )
(10,383 )
(22,876,457 )
(20,903 )
(14,615,399 )
(11,315 )
(1,871,511 )
(4,640 )
(6,307,690 )
(15,234 )
—
—
—
Conversion of convertible notes to Series A preferred stock,
net of debt issuance costs
—
—
—
—
—
—
—
—
—
—
—
—
Conversion of notes payable with related parties to Series A
convertible preferred
—
—
—
—
—
—
—
—
—
—
—
—
Conversion of Simple Agreement for Future Equity to Series A
convertible preferred
—
—
—
—
—
—
—
—
—
—
—
—
Conversion of warrant liability to Series A convertible
preferred
—
—
—
—
—
—
—
—
—
—
—
—
Issuance of Series B convertible preferred stock, net of
issuance costs of $133
—
—
—
—
—
—
—
—
—
—
—
—
Conversion of Series A and Series B to Class A common stock
concurrently with initial public offering
—
—
—
—
—
—
—
—
—
—
(62,223,095 )
(128,439 )
(15,365,574 )
(122,791 )
(251,230 )
Balance at December 31, 2021
$
$
$
$
$
$
$
$
The accompanying notes are an integral part of the consolidated financial statements.
110
VAXXINITY, INC.
CONSOLIDATED STATEMENTS OF STOCKHOLDERS’ EQUITY (DEFICIT)
(in thousands, except share amounts)
Stockholders’ Deficit
Common Stock
Common Stock-Class A
Common Stock-Class B
Treasury Stock
Shares
Amount
Shares
Amount
Shares
Amount
Shares
Amount
Additional Paid-
in Capital
Accumulated
Deficit
Stockholders’
Equity (Deficit)
Balance at December 31, 2019
$
$
$
—
(3,169,093 )
$
(23 )
$
$
(52,349 )
$
(48,512 )
Issuance of common stock upon exercise of stock options
—
—
—
—
—
—
—
Vesting of restricted stock
—
—
—
—
—
—
—
—
Issuance of common stock
—
—
—
—
—
—
—
—
—
—
Stock-based compensation expense
—
—
—
—
—
—
—
—
—
Reclassification of common stock to Class A common stock
(60,360,523 )
(272 )
—
—
—
—
—
—
—
Reclassification of common stock to Class B common stock
(10,999,149
—
—
—
—
—
—
—
—
—
Net loss
—
—
—
—
—
—
—
—
—
(39,957 )
(39,957 )
Balance at December 31, 2020
—
$
$
$
—
(3,169,093 )
$
(23 )
$
$
(92,306 )
$
(87,375 )
Issuance of common stock upon exercise of stock options
—
—
186,202
—
—
—
—
—
—
Vesting of restricted stock
—
—
—
—
—
—
—
—
—
—
Reclassification of Class A common stock to Class B common stock
—
—
(2,874,983 )
—
—
—
—
—
—
—
Issuance of common stock upon stock grant
—
—
—
—
—
—
—
—
Retirement of treasury stock upon reorganization
—
—
(3,169,093 )
—
—
—
(23 )
—
—
Proceeds from initial public offering, net of offering expenses of $13,913
—
—
—
—
—
—
71,076
—
71,077
Exercise of warrants concurrently with initial public offering
—
—
—
—
—
—
—
—
Conversion of Series A and Series B to Class A common stock concurrently with initial public
offering
—
—
—
—
—
—
—
Stock-based compensation expense
—
—
—
—
—
—
—
—
—
Net loss
—
—
—
—
—
—
—
—
—
(137,175 )
(137,175 )
Balance at December 31, 2021
—
$
—
$
$
—
$
$
$
(229,481 )
$
The accompanying notes are an integral part of the consolidated financial statements.
111
VAXXINITY, INC.
CONSOLIDATED STATEMENTS OF CASH FLOWS
(in thousands)
Years Ended December 31,
2021
2020
Cash flows from operating activities:
Net loss
$
(137,175 )
$
(39,957 )
Adjustments to reconcile net loss to net cash used in operating activities:
Depreciation expense
Amortization of debt issuance costs
Stock-based compensation expense
Non-cash consulting expense
Non-cash interest expense
Change in fair value of convertible notes
Change in fair value of warrant liability
Change in fair value of simple agreement for future equity
Changes in operating assets and liabilities:
Accounts receivable
(26 )
Amounts due from related parties
(31 )
(1,743 )
Prepaid expenses and other current assets
(4,704 )
(3,488 )
Deferred offering costs
(2,254 )
Accounts payable
(267 )
Amounts due to related parties
Accrued expenses and other current liabilities
Other long-term liabilities
(12 )
Net cash used in operating activities
(80,990 )
(33,910 )
Cash flows from investing activities:
Purchase of property and equipment
(1,318 )
(1,477 )
Net cash used in investing activities
(1,318 )
(1,477 )
Cash flows from financing activities:
Proceeds from initial public offering, net of offering expenses of $13,913
Proceeds from issuance of convertible notes payable
Repayment of convertible notes payable
(2,000 )
(5,500 )
Repayment of notes payable
(414 )
(202 )
Repayment of note payable with related party
(100 )
Proceeds from issuance of Series B convertible preferred stock, net of issuance costs
Proceeds from issuance of simple agreement for future equity
Proceeds from issuance of Series Seed-1 convertible preferred stock, net of issuance costs
Proceeds from issuance of Series Seed-2 convertible preferred stock, net of issuance costs
Proceeds from issuance of Series A-1 convertible preferred stock, net of issuance costs
Payment for Series A-2 convertible preferred stock issuance costs
(41 )
Debt issuance costs for related party convertible notes
(300 )
Repayment of Paycheck Protection Program
(257)
—
Proceeds from Paycheck Protection Program
Proceeds from exercise of stock options
Net cash provided by financing activities
Increase in cash, cash equivalents, and restricted cash
Cash, cash equivalents, and restricted cash at beginning of period
Cash, cash equivalents, and restricted cash at end of period
$
$
Supplemental Disclosure
Cash paid for interest
$
$
Noncash Financing Activities
Conversion of Series A and Series B to Class A common stock concurrently with initial public offering
$
$
Exchange of Series Seed, Series Seed-1, Series Seed-2, Series A-1 and Series A-2 for Series A
$
$
Conversion of simple agreement for future equity into Series A preferred stock
$
$
Conversion of convertible notes payable into Series A preferred stock
$
$
Conversion of notes payable with related parties into Series A preferred stock
$
$
Conversion of warrant liability into Series A preferred stock
$
$
Cashless exercise of warrant into Class A common stock concurrently with initial public offering
$
Retirement of treasury stock upon reorganization
$
$
Conversion of simple agreement for future equity into Series A-2 preferred stock
$
$
Acquisition of airplane through issuance of note payable
$
$
Fair value of warrants issued in connection with preferred stock issuance
$
$
Conversion of simple agreement for future equity into Series Seed-2 preferred stock
$
$
Warrant liability reclassified to Series A-1 preferred stock upon warrant exercise
$
$
Fair value of restricted stock vesting during the period
$
$
112
The accompanying notes are an integral part of the consolidated financial statements.
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
113
1. Nature of the Business
Vaxxinity, Inc., a Delaware corporation (“Vaxxinity ,” and together with its subsidiaries, the “Company”), was formed through the
combination of two separate businesses that originated from United Biomedical, Inc. (“UBI”) in two separate transactions: a spin-out
from UBI in 2014 of operations focused on developing chronic disease product candidates that resulted in United Neuroscience (“UNS”),
and a second spin-out from UBI in 2020 of operations focused on the development of a COVID-19 vaccine that resulted in C19 Corp.
(“COVAXX”). On February 2, 2021, Vaxxinity was incorporated for the purpose of reorganizing and combining UNS and COVAXX
and on March 2, 2021, did so by acquiring all of the outstanding equity interests of UNS and COVAXX pursuant to a contribution and
exchange agreement (the “Contribution and Exchange Agreement”) whereby the existing equity holders of UNS and COVAXX
contributed their equity interests in each of UNS and COVAXX in exchange for equity in Vaxxinity (the “Reorganization”).
The Company is a biotechnology company currently focused on developing product candidates for human use in the fields of neurology
and coronaviruses utilizing its “Vaxxine Platform”—a peptide vaccine technology first developed by UBI and subsequently refined over
the last two decades. The Company is engaged in the development and commercialization of rationally designed prophylactic and
therapeutic vaccines to combat chronic disorders and infectious diseases with large patient populations and unmet medical need. UBI is
a significant shareholder of the Company and, therefore, considered a related party.
The Company is subject to risks and uncertainties common to early-stage companies in the biotechnology industry including, but not
limited to, uncertainty of product development and commercialization, lack of marketing and sales history, development by its
competitors of new technological innovations, dependence on key personnel, market acceptance of products, product liability, protection
of proprietary technology, ability to raise additional financing, and compliance with government regulations. If the Company does not
successfully commercialize any of its product candidates, it will be unable to generate recurring product revenue or achieve profitability.
The Company’s product candidates are in development and will require significant additional research and development efforts,
including extensive pre-clinical and clinical testing and regulatory approval prior to commercialization. These efforts require significant
amounts of additional capital, adequate personnel and infrastructure and extensive compliance-reporting capabilities. There can be no
assurance that the Company’s research and development will be successfully completed, that adequate protection for the Company’s
intellectual property will be obtained, that any products developed will obtain necessary government regulatory approval or that any
approved products will be commercially viable. Even if the Company’s product development efforts are successful, it is uncertain when,
if ever, the Company will generate significant revenue from product sales. The Company operates in an environment of rapid change in
technology and is dependent upon the services of its employees and consultants.
Contribution and Exchange Agreement
On March 2, 2021, in accordance with the Contribution and Exchange Agreement, (i) all outstanding shares of UNS and COVAXX
preferred stock and common stock were contributed to Vaxxinity and exchanged for like shares of stock in Vaxxinity, (ii) the outstanding
options to purchase shares of UNS and COVAXX common stock were terminated and substituted with options to purchase shares of
common stock in Vaxxinity, (iii) the outstanding warrant to purchase shares of COVAXX common stock was cancelled and exchanged
for a warrant to acquire common stock in Vaxxinity and (iv) each outstanding Reorganization Convertible Note (as defined below) was
contributed to Vaxxinity and the holders of such notes received Series A preferred stock in Vaxxinity. In particular:
•
Each UNS common share and convertible preferred share was exchanged for 0.2191 shares of Vaxxinity common stock or
Series A preferred stock, as applicable;
•
Each share of COVAXX common and convertible preferred stock was exchanged for
stock or Series A preferred stock, as applicable (and prior to the closing of the Reorganization, all the holders of outstanding
COVAXX SAFEs agreed to convert such SAFEs into shares of Series A-3 preferred stock of COVAXX, which shares were
then exchanged for shares of Vaxxinity’s Series A preferred stock);
•
The Reorganization Convertible Notes were exchanged for an aggregate of
preferred stock; and
•
Each outstanding option of both UNS and COVAXX to purchase common shares of UNS or COVAXX was terminated and
substituted with an option to purchase shares of Class A common stock of Vaxxinity. Each outstanding UNS option was
exchanged based on a conversion ratio of
. Each outstanding COVAXX option was exchanged based on a conversion
ratio of
.
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
114
All parties to the Contribution and Exchange Agreement intend that the contribution of outstanding equity interests to Vaxxinity in
exchange for Vaxxinity’s common stock and preferred stock will be treated as an integrated transaction for U.S. federal income tax
purposes that is governed by Section 351(a) of the Internal Revenue Code of 1986, as amended.
The Reorganization was determined to be a common control transaction, so the carrying values of all contributed assets and assumed
liabilities remained unchanged and the financial information for all periods in the financial statements presented prior to the
Reorganization are presented on a consolidated basis.
Reverse Stock Split
On October 29, 2021, the Company effectuated a reverse stock split of 1-for-
Class B common stock pursuant to an amendment to the Company’s Amended and Restated Certificate of Incorporation approved by
the Company’s board of directors and stockholders. As a result of the Stock Split, the Company also adjusted the share and per share
amounts associated with its options and warrants to purchase shares of its common stock. These consolidated financial statements
including the notes have been retroactively adjusted to reflect the Stock Split for all periods presented. Any fractional shares that would
have resulted from the Stock Split have been rounded down to the nearest whole share.
Initial Public Offering
On November 15, 2021, the Company closed its IPO of
per share. On November 18, 2021 the Company held a subsequent closing for the issuance of an additional
common stock pursuant to a 30-day option granted to the underwriters to purchase up to an additional
stock at the IPO price, less underwriting discounts and commissions. The aggregate net proceeds to the Company from the offering,
after deducting underwriting discounts and commissions and other offering expenses payable by the Company, was approximately $
million. Upon the closing of the IPO, all previously outstanding shares of the Company’s redeemable convertible preferred stock were
automatically converted at the same ratio used for the Stock Split (1-for-
) into shares of its Class A common stock.
Liquidity
As of December 31, 2021, the Company had $144.9 million of cash and cash equivalents. To date, the Company has primarily financed
its operations through the sale of convertible preferred stock and common stock and borrowings under promissory notes (including
Convertible Notes), a portion of which has been raised from related party entities. The Company has experienced significant negative
cash flows from operations since inception, and incurred a net loss of $137.2 million for the year ended December 31, 2021. Net cash
used in operating activities for the year ended December 31, 2021 was $81.0 million. In addition, as of December 31, 2021, the Company
has an accumulated deficit of $229.5 million. The Company expects to incur substantial operating losses and negative cash flows from
operations for the foreseeable future. As of the date these financial statements were available to be issued, the Company expects its
existing cash and cash equivalents to be sufficient to fund its operating expenses and capital expenditure requirements for at least the
next 12 months.
The Company will need to obtain additional funding beyond the period that is 12 months from the date these financial statements were
available to be issued whether through collaboration agreements, private or public equity or debt offerings or a combination thereof, and
such additional funding may not be available on terms the Company finds acceptable or at all. If the Company is unable to obtain
sufficient capital to continue to advance its programs, the Company would be forced to delay, limit, reduce or terminate its product
development or future commercialization efforts or grant rights to third parties to develop and market product candidates that the
Company would otherwise prefer to develop and market itself.
The accompanying consolidated financial statements have been prepared on a going concern basis, which contemplates the realization
of assets and satisfaction of liabilities in the ordinary course of business. The consolidated financial statements do not include any
adjustments relating to the recoverability and classification of recorded asset amounts or the amounts and classification of liabilities that
might result from the outcome of the uncertainties described above.
Impact of COVID-19 Pandemic
In March 2020, the World Health Organization declared the outbreak of a COVID-19 pandemic. The COVID-19 pandemic is evolving,
and to date, has led to the implementation of various responses, including government-imposed quarantines, travel restrictions and other
public health safety measures.
The Company is closely monitoring the impact of the COVID-19 pandemic on all aspects of its business, including how it will impact
its operations and the operations of its customers, suppliers, vendors and business partners. The Company does not yet know the full
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
115
extent of potential delays or impacts on its business, its clinical trials, its research programs, healthcare systems or the global economy
and it cannot presently predict the scope and severity of any potential business shutdowns or disruptions. The extent to which
COVID-19 impacts its business, results of operation and financial condition will depend on future developments, which are highly
uncertain and cannot be predicted with confidence, such as the duration of the outbreak, new information that may emerge concerning
the severity of COVID-19 or the effectiveness of actions to contain COVID-19 or treat its impact, among others. If the Company or any
of the third parties with whom the Company engages, however, were to experience shutdowns or other business disruptions, its ability
to conduct its business in the manner and on the timelines presently planned could be materially and negatively affected, which could
have a material adverse impact on its business, results of operation and financial condition.
The Company has not incurred impairment losses in the carrying values of its assets as a result of the COVID-19 pandemic and it is not
aware of any specific related event or circumstance that would require it to revise its estimates reflected in these consolidated financial
statements.
2. Summary of Significant Accounting Policies
Basis of presentation
The accompanying consolidated financial statements have been prepared using generally accepted accounting principles in the United
States of America (GAAP) and pursuant to the rules and regulations of the United States Securities and Exchange Commission (“SEC”)
for financial reporting. The consolidated financial statements for the periods presented include the accounts of UNS and COVAXX that
were parties to the Contribution and Exchange Agreement. All share and per share amounts, as originally recorded by each entity, have
been converted to a number of shares and per share amounts using the conversion ratios determined under the Contribution and Exchange
Agreement and the Stock Split ratio.
Foreign currency translation
The Company’s consolidated financial statements are prepared in U.S. dollars. Its foreign subsidiaries use the U.S. dollar as their
functional currency and maintain their records in the local currency. Nonmonetary assets and liabilities are re-measured at historical
rates and monetary assets and liabilities are re-measured at exchange rates in effect at the end of the reporting period. Income statement
accounts are re-measured at average exchange rates for the reporting period. The resulting gains or losses are included in foreign currency
(losses) gains in the consolidated statements of operations.
Segment information
Operating segments are defined as components of an entity for which separate financial information is available and that is regularly
reviewed by the Chief Operating Decision Maker (“CODM”) in deciding how to allocate resources to an individual segment and in
assessing performance. The Company’s CODM is its Chief Executive Officer (“CEO”). The Company has determined that it operates
as a single operating segment and has one reportable segment.
Use of estimates
The preparation of consolidated financial statements in accordance with GAAP requires the Company’s management to make estimates
and assumptions that affect the reported amounts of assets and liabilities and disclosure of contingent assets and liabilities at the date of
the consolidated financial statements and the reported amounts of expenses during the reporting period. Significant estimates contained
within these consolidated financial statements include, but are not limited to, the estimated fair value of the Company’s common stock
and convertible notes payable, simple agreements for future equity, warrant liabilities, stock-based compensation, income tax valuation
allowance and the accruals of research and development expenses. The Company bases its estimates on historical experience, known
trends and other market-specific or other relevant factors that it believes to be reasonable under the circumstances. On an ongoing basis,
management evaluates its estimates, as there are changes in facts and circumstances. Actual results may differ materially from those
estimates or assumptions.
Cash and cash equivalents
The Company considers all highly liquid investments with an original maturity of three months or less at the time of initial purchase to
be cash equivalents, including balances held in the Company’s money market accounts. The Company maintains its cash and cash
equivalents with financial institutions, in which balances from time to time may exceed the U.S. federally insured limits. The objectives
of the Company’s cash management policy are to safeguard and preserve funds to maintain liquidity sufficient to meet the Company’s
cash flow requirements, and to attain a market rate of return.
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
116
Restricted cash
As of December 31, 2021 and 2020 a deposit of $0.2 million and $0.1 million, respectively, was restricted from withdrawal. The
restriction relates to securing credit card obligations. This balance is included in restricted cash on the accompanying consolidated
balance sheets.
The Company’s consolidated statement of cash flows for the year ended December 31, 2021 and 2020 included restricted cash with cash
and cash equivalents when reconciling the beginning-of-period and end-of-period total amounts shown on such statements. A
reconciliation of cash, cash equivalents and restricted cash reported within the consolidated balance sheets that sum to the total of the
same amounts shown in the consolidated statements of cash flows is as follows (in thousands):
December 31,
2021
2020
Cash and cash equivalents
$
$
Restricted cash
Total cash, cash equivalents and restricted cash
$
$
Concentration of credit risk
Financial instruments that potentially expose the Company to concentrations of credit risk consist primarily of cash and cash equivalents.
Cash equivalents are occasionally invested in certificates of deposit. The Company maintains each of its cash balances with high-quality
and accredited financial institutions and accordingly, such funds are not exposed to unusual credit risk beyond the normal credit risk
associated with commercial banking relationships. The Company maintains a portion of its cash and cash equivalent balances in the
form of a money market account with a financial institution that management believes to be creditworthy.
The Company is dependent on contract manufacturers, several of whom are considered to be related parties, for manufacturing, quality
control, testing, validation and supply services, including production, including production and shipment of its enzyme-linked
immunosorbent assay (“ELISA”) tests, and for research and development and clinical activities. The Company’s future revenue as well
as research and development programs could be adversely affected by a significant supply interruption by one or more of its contract
manufacturers.
Accounts receivable
The Company’s trade accounts receivable consist of amounts due from distributors. The Company reserves against trade accounts
receivable for estimated losses that may arise from a customer’s inability to pay, and any amounts determined to be uncollectible are
written off against the reserve when it is probable that the receivable will not be collected. As of December 31, 2021 and 2020, the
Company has not recorded any allowance for bad debts against the trade accounts receivable.
Property and equipment
Property and equipment are stated at cost, less accumulated depreciation. Depreciation is computed on the straight-line basis over the
estimated useful life of the assets.
The estimated useful life of property and equipment is as follows:
Estimated
Useful
Life
Airplane
Facilities
15 years
Furniture and fixtures
Vehicles
5 years
Laboratory and computer equipment
Software
3 years
Upon retirement or sale, the cost of assets disposed of and the related accumulated depreciation are removed from the accounts and any
resulting gain or loss is included in gain or loss from operations. Expenditures for repairs and maintenance are charged to expense as
incurred.
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
117
Impairment of long-lived assets
Long-lived assets, comprised of property and equipment, are tested for recoverability whenever events or changes in business
circumstances indicate that the carrying amount of the assets may not be fully recoverable. Factors that the Company considers in
deciding when to perform an impairment review include significant underperformance of the business in relation to expectations,
significant negative industry or economic trends and significant changes or planned changes in the use of the assets. If an impairment
review is performed to evaluate a long-lived asset for recoverability, the Company compares forecasts of undiscounted cash flows
expected to result from the use and eventual disposition of the long-lived asset to its carrying value. An impairment loss would be
recognized when estimated undiscounted future cash flows expected to result from the use of an asset are less than its carrying amount.
The impairment loss would be based on the excess of the carrying value of the impaired asset over its fair value, determined based on
discounted cash flows. To date, the Company has not recorded any impairment losses or disposals on long-lived assets.
Deferred offering costs
The Company capitalizes certain legal, audit, accounting and other third-party fees that are directly associated with an in-process capital
financing effort as deferred offering costs until such financing is consummated. After consummation of the financing, these costs are
recorded as a reduction of additional paid-in capital generated as a result of the financing. Should the financing be abandoned, the
deferred offering costs are expensed immediately as a charge to operating expenses in the statement of operations.
Fair value measurements
Certain assets and liabilities are carried at fair value under GAAP. Fair value is defined as the exchange price that would be received for
an asset or paid to transfer a liability (an exit price) in the principal or most advantageous market for the asset or liability in an orderly
transaction between market participants on the measurement date. Valuation techniques used to measure fair value must maximize the
use of observable inputs and minimize the
use of unobservable inputs. Financial assets and liabilities carried at fair value are to be classified and disclosed in one of the following
three levels of the fair value hierarchy, of which the first two are considered observable and the last is considered unobservable:
Level 1—Quoted prices in active markets that are identical assets or liabilities.
Level 2—Observable inputs (other than Level 1 quoted prices), such as quoted prices in active markets for similar assets or liabilities,
quoted prices in markets that are not active for identical or similar assets or liabilities, or other inputs that are observable or can be
corroborated by observable market data.
Level 3—Unobservable inputs that are supported by little or no market activity that are significant to determining the fair value of the
assets or liabilities, including pricing models, discounted cash flow methodologies and similar techniques.
Prior to the conversion in accordance with the Contribution and Exchange Agreement, the majority of the Company’s convertible notes
and all of the simple agreement for future equity (“SAFE”) and warrant liabilities were carried at fair value and were classified as Level
3 liabilities.
Convertible notes payable
The Company issued convertible notes payable at various times from 2014 to 2021. The Company accounts for the convertible notes
payable at fair value in accordance with ASC 480, Distinguishing Liabilities from Equity (“ASC 480”). The notes payable with related
parties are accounted for as straight debt under ASC 470, Debt (“ASC 470”). The Company has elected to separate interest expense
from the full change in fair value of the convertible notes. Debt issuance costs incurred by the Company are amortized to interest expense
over the term of the convertible notes using the effective interest method in the accompanying consolidated statements of operations.
On March 2, 2021, each convertible note that was outstanding was exchanged for shares of Series A preferred stock (see Note 8).
Debt issuance costs
The Company records debt issuance costs as a reduction to the carrying value of the debt. The debt discounts are amortized over the
term of the debt using the effective interest method and recognized as interest expense in the accompanying consolidated statement of
operations.
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
118
Simple Agreement for Future Equity—SAFE
The Company accounts for SAFEs at fair value in accordance with ASC 480. The SAFEs are subject to revaluation at the end of each
reporting period, with changes in fair value recognized in the accompanying consolidated statements of operations.
On March 2, 2021, each SAFE that was outstanding was converted into shares of the Company’s Series A preferred stock (see Note 11).
Classification of convertible preferred stock
The Company records all convertible preferred stock at its original issuance price, less direct and incremental issuance costs, as stipulated
by its terms. The Company’s convertible preferred stock is classified outside of stockholders’ deficit because the holders of such shares
have liquidation rights in the event of a deemed liquidation that, in certain situations, are not solely within the control of the Company.
All shares of the Company’s Series A and Series B preferred stock converted into shares of the Company’s Class A common stock
concurrently with the closing of the initial public offering (see Note 10).
Revenue recognition
The Company accounts for revenue in accordance with ASC Topic 606, Revenue from Contracts With Customers (“ASC 606”). Under
ASC 606, an entity recognizes revenue when its customer obtains control of promised goods or services, in an amount that reflects the
consideration that the entity expects to be entitled to in exchange for those goods or services. The Company applies ASC 606 to contracts
with customers only when it is probable that the entity will collect the consideration to which it is entitled in exchange for the goods or
services it transfers to the customer.
The Company assesses the goods or services promised within each contract and determines those that are performance obligations by
evaluating whether each promised good or service is distinct. This assessment involves subjective determinations and requires
management to make judgments about the individual promised goods or services, the intended benefit of the contract and whether each
good or service is separately identifiable from the other aspects of the contractual relationship. If a promised good or service is not
distinct, an entity is required to combine that good or service with other promised goods or services until it identifies a bundle of goods
or services that is distinct.
If the consideration promised in a contract includes a variable amount, the Company estimates the amount of consideration to which it
will be entitled in exchange for transferring the promised goods or services to a customer. The Company determines the amount of
variable consideration by using the most likely amount method and applies the constraint on variable consideration, which requires the
amount included in the transaction price to be constrained to the amount for which it is probable that a significant reversal of cumulative
revenue recognized will not occur. At the end of each subsequent reporting period, the Company re-evaluates the estimated variable
consideration included in the transaction price and any related constraint, and if necessary, adjusts its estimate of the overall transaction
price.
The Company recognizes as revenue the amount of the transaction price that is allocated to the respective performance obligation when
(or as) each performance obligation is satisfied, either at a point in time or over time, and, if over time, recognition is based on the use
of an output or input method. In the Company’s sole revenue contract, the performance obligation was satisfied at the point in time the
data and related samples were made available for the customer’s review.
For its sales of ELISA tests, the Company recognizes revenue once control is transferred upon delivery to the customer.
Taiwan Centers for Disease Control grant
United Biomedical, Inc., Asia (“UBI-Asia”), a related party through common ownership which is responsible for applying for and
managing grants on the Company’s behalf, was awarded a grant by the Taiwan Centers for Disease Control (“Taiwan CDC”) for
COVID-19 vaccine development. UBI-Asia contracted with the Company to conduct a two-phase study of a COVID-19 vaccine clinical
trial in Taiwan. The grant provides that costs incurred to complete the two phases of the clinical trial will be reimbursed based on the
achievement of certain milestones as defined in the agreement. At each reporting date, the Company assesses the status of all the
activities involved in completing the clinical trials in relation to the milestones. The Company accounts for the amounts that have been
received from the Taiwan CDC to reimburse costs incurred on the clinical trials and not expected to be refunded back to the Taiwan
CDC as contra research and development expenses in the accompanying consolidated statements of operations.
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
119
Research and development
Research and development expenses include employee related costs, consulting, contract research, depreciation, rent, stock-based
compensation and other corporate costs attributable to research and development activities and are expensed as incurred.
The Company has entered into various research, development and manufacturing contracts, some of which are with related parties (see
Note 18). These agreements are generally cancelable by either party, and related payments are recorded as research and development
expenses as incurred. The Company records accruals for estimated ongoing research costs. When evaluating the adequacy of the accrued
liabilities, the Company analyzes progress of the studies or trials, including the phase or completion of events, invoices received and
contracted costs. The Company’s historical accrual estimates have not been materially different from the actual costs.
Patent costs
Patent-related costs incurred in connection with filing and prosecuting patent applications are expensed as incurred due to the uncertainty
relating to the recovery of the expenditure. Amounts incurred are classified as general and administrative expenses.
Stock-based compensation
The Company measures all stock-based awards granted to employees, directors and non-employees based on the fair value on the date
of grant and recognizes compensation expense of those awards over the requisite service period, which is generally the vesting period
of the respective award. Forfeitures are accounted for as they occur.
The Company classifies stock-based compensation expense in its consolidated statements of operations in the same manner in which
the award recipient’s payroll costs are classified or in which the award recipient’s service payments are classified.
Prior to the Company's IPO in November 2021, there was no public market for the Company’s common stock and the estimated fair
value of its common stock was determined by its most recently available third-party valuations of common stock. There are significant
judgments and estimates inherent in the determination of the fair value of the Company’s common stock. These estimates and
assumptions include a number of objective and subjective factors, including external market conditions, the prices at which the Company
sold shares of preferred securities, the superior rights and preferences of securities senior to the common securities at the time of, and
the likelihood of, achieving a liquidity event, such as an initial public offering (“IPO”) or sale. Significant changes to the key assumptions
used in the valuations could result in different fair values of common stock at each valuation date.
The fair value of each restricted stock award is estimated on the date of grant based on the fair value of the Company’s common stock
on that same date. The fair value of each option grant is estimated on the date of grant using the Black-Scholes option pricing model
(“Black-Scholes”), which requires inputs based on certain subjective assumptions, including the expected stock price volatility, the
expected term of the award, the risk-free interest rate and expected dividends. The Company, both prior to and after the IPO in November
2021, lacks sufficient company-specific historical and implied volatility information for its stock, and therefore estimates its expected
stock volatility based on the historical volatility of a publicly traded set of peer companies and expects to continue to do so until such
time as it has adequate historical data regarding the volatility of its own traded stock price. The expected term of the Company’s options
has been determined utilizing the “simplified” method for awards that qualify as “plain-vanilla” options. The expected term of options
granted to non-employees is equal to the contractual term of the option award. The risk-free interest rate is determined by reference to
the U.S. Treasury yield curve in effect at the time of grant of the award for time periods approximately equal to the expected term of the
award. Expected dividend yield is based on the fact that the Company has never paid cash dividends on common stock and does not
expect to pay any cash dividends in the foreseeable future.
Performance-based options
The Company accounts for performance-based options according to the ASC 718, Compensation – Stock Compensation ("ASC 718"),
which are subject to different accounting depending on whether they meet the definition of performance conditions, market conditions,
or other conditions. The conditions present in the Company's grants contain both performance and market conditions. The effect of each
condition is reflected in the grant-date fair value and the performance-based options are measured considering the probability of
satisfying the performance and market conditions. The Company has used a Monte Carlo Simulation Model to calculate the fair value
of the performance condition (the completion of the IPO) and market condition (the 25% higher value after the IPO condition). The
performance condition was determined to not be probable at the time of the grant date, and the recognition of compensation cost was
deferred until the IPO was consummated in November 2021. The recognition of expense for the portion of the grant-date fair value
assigned to the market condition will be recognized as expense according to the derived service period in the valuation model.
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
120
Income taxes
The Company accounts for income taxes according to the ASC 740, Income Taxes (“ASC 740”) using the asset and liability method,
which requires the recognition of deferred tax assets and liabilities for the expected future tax consequences of events that have been
recognized in the consolidated financial statements or in the Company’s tax returns. Deferred taxes are determined based on the
difference between the financial statement and tax basis of assets and liabilities using enacted tax rates in effect in the years in which
the differences are expected to reverse. Changes in deferred tax assets and liabilities are recorded in the provision for income taxes. The
Company assesses the likelihood that its deferred tax assets will be realized and, to the extent it believes, based upon the weight of
available evidence, that it is more likely than not that all or a portion of the deferred tax assets will not be realized, a valuation allowance
is established through a charge to income tax expense. In evaluating its ability to recover its deferred tax assets, the Company considers
all available positive and negative evidence, including projected future taxable income, prudent and feasible tax planning strategies and
recent financial operations.
The Company accounts for uncertainty in income taxes recognized in the consolidated financial statements by applying a two-step
process to determine the amount of tax benefit to be recognized. First, the tax position must be evaluated to determine the likelihood
that it will be sustained upon external examination by the taxing authorities. If the tax position is deemed more-likely-than-not to be
sustained, the tax position is then assessed to determine the amount of benefit to recognize in the consolidated financial statements. The
amount of the benefit that may be recognized is the largest amount that has a greater than 50% likelihood of being realized upon ultimate
settlement. To the extent the Company determines that such tax positions will not be sustained, the provision for income taxes would
include the effects of any resulting income tax reserves, or unrecognized tax benefits, that are considered appropriate as well as the
related net interest and penalties.
Net loss per share
The Company follows the two-class method when computing net loss per share as the Company has issued shares that meet the definition
of participating securities. The two-class method determines net loss per share for each class of common and participating securities
according to dividends declared or accumulated, and participation rights in undistributed earnings. The two-class method requires loss
available to common stockholders for the period to be allocated between common and participating securities based upon their respective
rights to receive dividends as if all income for the period had been distributed.
Basic net loss per share is computed by dividing the net loss by the weighted average number of common shares outstanding for the
period. Diluted net loss is computed by adjusting net loss to reallocate undistributed earnings based on the potential impact of dilutive
securities. Diluted net loss per share is computed by dividing the diluted net loss by the weighted average number of common shares
outstanding for the period, including potential dilutive common stock. For purpose of this calculation, outstanding options, unvested
restricted stock and convertible preferred stock are considered potential dilutive common stock and are excluded from the computation
of net loss per share as their effect is anti-dilutive.
The Company’s convertible preferred stock contractually entitles the holders of such shares to participate in dividends but does not
contractually require the holders of such shares to participate in losses of the Company. Accordingly, in periods in which the Company
reports a net loss, such losses are not allocated to such participating securities. In periods in which the Company reports a net loss,
diluted net loss per share is the same as basic net loss per share attributable to common stockholders, since dilutive common shares are
not assumed to be outstanding if their effect is anti-dilutive.
Emerging growth company status
The Company is an “emerging growth company” (“EGC”), as defined in the Jumpstart Our Business Startups Act (“JOBS Act”) and is
permitted to and plans to take advantage of certain exemptions from various reporting requirements that are applicable to other public
companies that are not EGCs. The Company may take advantage of these exemptions until it is no longer an EGC under Section 107 of
the JOBS Act, which provides that an EGC can take advantage of the extended transition period afforded by the JOBS Act for the
implementation of new or revised accounting standards. The Company has elected to avail itself of the extended transition period and,
therefore, as long as the Company remains an EGC, it will not be subject to new or revised accounting standards at the same time that
they become applicable to other public companies that are not EGCs.
Reclassifications
We reclassified certain accrued payroll and related liabilities for employee bonuses from other long-term liabilities to accrued expenses
and other current liabilities within the Consolidated Balance Sheet. Prior year amounts have been reclassified to conform to current year
presentation. These changes have no impact on our previously reported consolidated net loss, financial position or net increase in cash,
cash equivalents, and restricted cash.
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
121
Recently issued accounting pronouncements
In February 2016, the FASB issued ASU 2016-02, “Leases (Topic 842), and associated ASUs related to Topic 842, which requires
organizations that lease assets to recognize on the balance sheet the assets and liabilities for the rights and obligations created by those
leases. The new guidance requires that a lessee recognize assets and liabilities for leases, and recognition, presentation and measurement
in the financial statements will depend on its classification as a finance or operating lease. In addition, the new guidance requires
disclosures to help investors and other financial statement users better understand the amount, timing and uncertainty of cash flows
arising from leases.
The Company has elected to apply the transition requirements as of January 1, 2022. This approach allows for a cumulative effect
adjustment in the period of adoption, and prior periods continue to be reported in accordance with historic accounting under ASC 840
“Leases.” Additionally, as an accounting policy election, the Company has chosen to not apply the standard to any existing short-term
leases (term of 12 months or less) as this is optional under U.S. GAAP. This adoption of the new standard on January 1, 2022 is not
expected to have a material impact to the consolidated balance sheets, consolidated statements of operations and consolidated statements
of cash flow.
3. Fair Value Measurements
The Company's money market accounts are shown at fair value based on unadjusted quoted market prices in active markets for identical
assets.
The value for the Convertible Notes, SAFE and warrant liability balances as of December 31, 2020 are based on significant inputs not
observable in the market, which represents a Level 3 measurement within the fair value hierarchy. In accordance with the Contribution
and Exchange Agreement, on March 2, 2021 the Convertible Notes, SAFEs and warrants were all converted into Series A preferred
stock.
The following table presents information about the Company’s financial instruments measured at fair value on a recurring basis and
indicate the level of the fair value hierarchy used to determine such fair values (in thousands):
December 31, 2021
Level 1
Level 2
Level 3
Total
Assets:
Money market account
$
$
—
$
—
$
Total assets
$
$
$
$
December 31, 2020
Level 1
Level 2
Level 3
Total
Assets:
Money market account
$
—
$
—
$
—
$
—
Total assets
$
—
$
—
$
—
$
—
Liabilities:
Convertible notes payable
$
—
$
—
$
$
Convertible notes with related parties
—
—
SAFEs
—
—
Warrant liability
—
—
Total liabilities
$
—
$
—
$
$
During the years ended December 31, 2021 and 2020, there were
Convertible Notes
During the years ended December 31, 2021 and 2020, the Company issued Convertible Notes. In accordance with ASC 480, a portion
of the Convertible Notes were required to be measured and accounted for at fair value at each reporting date. The Company determined
the Convertible Notes requiring a measurement to fair value represent a recurring measurement that is classified within Level 3 of the
fair value hierarchy wherein fair value is estimated using significant unobservable inputs.
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
122
Convertible Notes requiring a measurement to fair value are as follows (in thousands):
Convertible
Notes
Balance at December 31, 2019
$
Issuance of convertible notes
Repayments
(5,500 )
Change in fair value
Issuance costs
(300 )
Amortization of issuance costs
Accrued interest
Balance at December 31, 2020
Issuance of convertible notes
Repayments
(2,000 )
Change in fair value
Amortization of issuance costs
Accrued interest
Interest paid
(187 )
Conversion to Series A preferred stock
(27,545 )
The fair value of the Convertible Notes was estimated using a straight debt and conversion feature valuation model consisting of
probability assumptions on multiple conversion scenarios, discount rates and interest rates.
In accordance with the Contribution and Exchange Agreement, on March 2, 2021, the Convertible Notes were converted into Series A
preferred stock.
Simple Agreement for Future Equity—SAFE
During the years ended December 31, 2021 and 2020, the Company executed SAFE arrangements. The fair value of the SAFEs on the
date of issuance was determined to equal the proceeds received by the Company. The value of the SAFEs on the dates of conversion
into preferred stock was determined to be equal to the fair value of the preferred stock issued, or $
December 31, 2021 and $
The following table sets forth a summary of the activities of the SAFE arrangements, which represents a recurring measurement that is
classified within Level 3 of the fair value hierarchy wherein fair value is estimated using significant unobservable inputs (in thousands):
SAFE
Liability
Balance at December 31, 2019
$
—
Issuance of SAFEs
Change in fair value
Conversion to Series Seed-2 convertible preferred stock
(360 )
Conversion to Series A-2 convertible preferred stock
(15,275 )
Balance at December 31, 2020
Change in fair value
Issuance of SAFEs
Conversion to Series A preferred stock
(35,600 )
In accordance with the Contribution and Exchange Agreement, on March 2, 2021, the SAFEs were converted into Series A preferred
stock.
Warrants to Purchase Series A-1 Convertible Preferred Stock & Common Stock
In connection with the 2020 Series A-1 convertible preferred stock (“Series A-1 preferred”) financing transactions, the Company issued
fully vested warrants to purchase
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
123
assistance with the sale and issuance of the Series A-1 preferred. The warrants were determined to represent issuance costs and were
recorded as a reduction in the proceeds received from the sale.
The warrants were issued to advisors of the company and represented non-variable contingently redeemable instruments. As such, the
warrants were accounted for as liabilities and adjusted to fair value at each reporting period.
The warrants are exercisable on the date of issuance and have an exercise price of $
In December 2020, warrants were exercised for
$
. As of December 31, 2020, warrants to purchase
continued to re-measure the fair value of the liability associated with the warrant to purchase shares of Series A-1 preferred at the end
of each reporting period until the Reorganization, when the warrant converted into Series A preferred stock and subsequently, in
connection with the IPO, converted into Class A common stock.
The following table sets forth a summary of the activity of the warrant liability which represented a recurring measurement that is
classified within Level 3 of the fair value hierarchy wherein fair value is estimated using significant unobservable inputs (in thousands):
Warrant
Liability
Balance at December 31, 2019
$
—
Issuance of Series A-1 preferred warrants
Exercise of warrants
(214 )
Change in fair value
Balance at December 31, 2020
Change in fair value
Conversion to warrants for shares of Series A preferred stock
(614 )
4. Prepaid Expenses and Other Current Assets
Prepaid expenses and other current assets consist of the following (in thousands):
December 31,
2021
2020
Deposits
$
$
Prepaid materials and supplies
Other
$
$
The Company’s prepaid material and supplies related to ELISA test production, of which $
$
5. Property and Equipment
Property and equipment, net consisted of the following (in thousands):
December 31,
2021
2020
Airplane
$
$
Laboratory and computer equipment
Software
Vehicles
Facilities, furniture and fixtures
Total property and equipment
Less: accumulated depreciation
(1,981 )
(878 )
Property and equipment, net
$
$
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
124
Depreciation expense for the years ended December 31, 2021 and 2020 was $1.1 million and $0.7 million, respectively.
6. Accrued Expenses and Other Current Liabilities
Accrued expenses and other current liabilities consisted of the following (in thousands):
December 31,
2021
2020
Accrued bonuses
$
$
Accrued external research and development
Accrued professional fees and other
Accrued interest
$
$
7. Other Long-Term Liabilities
Other long-term liabilities consisted of the following (in thousands):
December 31,
2021
2020
Accrued tax provision
Accrued rent
$
$
As of December 31, 2021 and 2020, approximately $
may be subject to paying for late filing fees related to a foreign subsidiary. The Company expects these amounts to be forgiven but has
accrued for them until the statute of limitations expires and it is appropriate to write them off.
8. Convertible Notes Payable
Beginning in April 2018, the Company issued several Convertible Notes, some of which were issued to related parties. The Convertible
Notes bear simple interest at annual rates ranging from
% to
%. All unpaid principal, together with the accrued interest thereon, are
payable upon an event of default or upon maturity, which ranges from one to three years. The Convertible Notes contain a number of
provisions addressing automatic and optional conversion, events of default, and prepayment provisions.
The Company accounts for the Convertible Notes at fair value, in accordance with ASC 480, with any changes in fair value being
recognized through the consolidated statements of operations.
In accordance with the Contribution and Exchange Agreement, on March 2, 2021 each Reorganization Convertible Note that was
outstanding was exchanged for shares of Series A preferred stock, as set forth in the applicable Convertible Note agreements and the
Contribution and Exchange Agreement.
During the years ended December 31, 2021 and 2020, the Company recognized interest expense of $
respectively, related to the Convertible Notes. In addition, in the years ended December 31, 2021 and 2020, the Company recognized a
change in fair value of $
Convertible Notes, respectively.
The following table shows the activity of the Convertible Notes (in thousands):
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
125
Convertible Notes
Principal Amount Payable
Change in Fair Value
Accrued Interest
Issuance
Conversion to
Standard
Related
Party
Standard
Related
Party
Standard
Related
Party
Costs
Series A
Balance
December 31, 2019
$
$
$
$
$
$
$
$
$
Additions
(300 )
Settlements
(5,500 )
(264 )
(5,709 )
Amortization
December 31, 2020
(217 )
Additions
Settlements
(2,000 )
(187 )
(2,187 )
Amortization
Conversion of Convertible
Notes to Series A preferred
stock
(5,710 )
(12,510 )
(2,784 )
(5,703 )
(545 )
(293 )
(27,545 )
(27,545 )
December 31, 2021
$
$
$
$
$
$
$
$
(27,545 )
$
9. Notes Payable
Notes Payable with Related Parties
In December 2018, the Company entered into related party convertible notes payable (the “2018 Related Notes” and together with the
Convertible Notes, the “Reorganization Convertible Notes”) for $
Related Notes bore simple interest at an annual rate of
% and contain a number of provisions addressing events of default and
prepayment. In accordance with the Contribution and Exchange Agreement, on March 2, 2021, the 2018 Related Notes were converted
into Series A preferred stock.
During the years ended December 31, 2021 and 2020, the Company recognized interest expense of less than $
Related Notes.
2019 Executive Note
In November 2019, the Company borrowed $
agreement was executed. However, the Company has elected to accrue interest at an annual rate of
%, consistent with the terms and
conditions of the Convertible Notes and 2018 Related Notes, which was the closest benchmark the Company could evaluate. The 2019
Executive Note was repaid in August 2021.
The activity of the 2018 Related Notes and 2019 Executive Note is as follows (in thousands):
2018 Related Notes and 2019 Executive Note
Related Party
Principal
Accrued
Interest
Balance
December 31, 2019
$
$
$
Additions
December 31, 2020
Accrued interest
Repayment
(100 )
(100 )
Interest paid
(8 )
(8 )
Conversion
(2,000 )
(205 )
(2,205 )
December 31, 2021
$
$
$
Note Payable—Airplane
In connection with the acquisition of an airplane, the Company entered into a note payable agreement (the “2025 Note”) in June 2020
for $
% and a maturity date of June 9, 2025. Principal and interest payments are payable
monthly in the amount of $
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
126
of the Company. In addition, the Company incurred debt issuance costs of $
loan. There are no financial covenants associated with the 2025 Note.
The carrying value of the 2025 Note is as follows (in thousands):
2021
2020
Principal
$
$
Unamortized debt issuance cost
(184 )
(237 )
Carrying amount
Less: current portion
(376 )
(362 )
Note payable, net of current portion and debt issuance cost
$
$
As of December 31, 2021, the remaining principal payments for the 2025 Note, are as follows (in thousands):
Amount
2022
$
2023
2024
2025
$
Interest expense associated with the 2025 Note was $
respectively. As of December 31, 2021, accrued interest of less than $
in the accompanying consolidated balance sheets.
Note Payable—Paycheck Protection Program
The Company applied for and received a loan, which is in the form of a note dated May 5, 2020, from HSBC Bank USA, National
Association (“HSBC”) in the aggregate amount of approximately $
Program (“PPP”). The PPP, established as part of the Coronavirus Aid, Relief and Economic Security Act (“CARES Act”), provides
for loans to qualifying businesses for amounts up to 2.5 times of the average monthly payroll expenses of the qualifying business. As of
December 31, 2021, there were no events of default under the PPP Loan.
The Company paid off the PPP Loan in full, including all accrued but unpaid interest to the repayment date, in August 2021.
10. Convertible Preferred Stock
In connection with the Reorganization, each UNS convertible preferred share was exchanged for
stock and each share of COVAXX convertible preferred stock was exchanged for
the first and second quarters of 2021, the Company raised gross proceeds of $
stock financing. The Company issued a total of
preferred stock converted into shares of the Company’s Class A common stock concurrently with the closing of the initial public offering.
As of December 31, 2021, Vaxxinity’s Amended and Restated Certificate of Incorporation authorized
stock with a par value of $
The table below details the Company's Class A common stock which was issued upon conversion of Series A and Series B preferred
stock concurrently with the closing of the IPO in November 2021. The common stock issued upon conversion reflects the application
of the stock split described in Note 1.
As of December 31, 2021
Issuance Dates
Shares Issued and
Outstanding Prior to IPO
Common Stock Issued
Upon IPO Conversion
Series A preferred stock
March 2021
Series B preferred stock
March 2021
Series B preferred stock
June 2021
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
127
11. Simple Agreement for Future Equity—SAFE
During the years ended December 31, 2021 and 2020, the Company executed SAFE arrangements. The SAFEs were not mandatorily
redeemable, nor did they require the Company to repurchase a fixed number of shares. The Company determined that the SAFEs
contained a liquidity event provision that embodied an obligation indexed to the fair value of the Company’s equity shares and could
require the Company to settle the SAFE obligation by transferring assets or cash. For this reason, the Company recorded the SAFEs as
a liability under ASC 480 and re-measured the fair value at the end of each reporting period, with changes in fair value reported in
earnings.
In March 2020, the Company issued a SAFE (“SAFE 1”) for $
convertible preferred stock at
$
(“SAFE 2”) for $
at
$
The Company determined the fair value of SAFE 2 investment on the date of conversion and recognized the difference between the fair
value on the date of conversion and the initial fair value of SAFE 2 investment in the consolidated statements of operations.
In December 2020, the Company issued a series of SAFEs (collectively, “SAFE 3”) for $
issued additional SAFEs for $
Equity Financing
—Upon initial closing of a qualified financing of at least $
greater of (1) the number of shares of SAFE 3 preferred stock equal to the purchase amount divided by the SAFE 3 price, defined as the
price per share equal to the post-money valuation divided by all shares outstanding, all convertible securities, all issued, outstanding and
promised options, and the unissued option pool, or (2) the number of shares of SAFE 3 preferred stock equal to the purchase amount
divided by the discount price, defined as the price per share of the standard preferred stock sold in a qualified financing multiplied by
eighty percent (80%).
Liquidity Event
—If there is a liquidity event, as defined, before the termination of SAFE 3, SAFE 3 will automatically be entitled to
receive a portion of proceeds, subject to the liquidation priority set forth in the agreement, due and payable immediately prior to, or
concurrent with, the consummation of such liquidity event, equal to the greater of (i) the purchase amount or (ii) the amount payable on
the number of shares of common stock equal to the purchase amount divided by the liquidity price, as outlined in the agreements.
Dissolution Event
—If there is a dissolution event, as described in the agreements, before the termination of SAFE 3, the investor will
automatically be entitled, subject to the liquidation priority set forth in the agreement, to receive a portion of proceeds equal to the
purchase amount, due and payable to the investor immediately prior to the consummation of the dissolution event.
Termination
—SAFE 3 will automatically terminate immediately following the earliest to occur of: (i) the issuance of capital stock to
the investor pursuant to the automatic conversion provisions of SAFE 3 or (ii) the payment, or setting aside for payment, of amounts
due the investor. In connection with the Contribution and Exchange Agreement, the holders of SAFEs agreed to convert such SAFEs
into shares of Series A-3 preferred stock of COVAXX, which shares were then exchanged for shares of Vaxxinity’s preferred stock.
The SAFEs were converted into shares of the Company’s Series A preferred stock pursuant to the Contribution and Exchange
Agreement. Prior to the Reorganization, all the holders of outstanding COVAXX SAFEs agreed to convert such SAFEs into shares of
Series A-3 preferred stock of COVAXX, which shares were then exchanged for shares of the Company’s Series A preferred stock.
12. Common Stock
As explained in Note 1, in accordance with the Contribution and Exchange Agreement, on March 2, 2021, all outstanding shares of
common stock of UNS and COVAXX were contributed to Vaxxinity and exchanged for an aggregate of
Vaxxinity’s Class A common stock and
was exchanged for
shares of Vaxxinity common stock.
In June 2021, the Company converted
Executive Chairman on a one-to-one basis for shares of Class B common stock.
As of December 31, 2021, Vaxxinity’s Amended and Restated Certificate of Incorporation authorized
stock with a par value of $
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
128
Holders of Class A common stock and Class B common stock have identical rights, except with respect to voting and conversion. Except
as otherwise expressly provided in Vaxxinity’s Amended and Restated Certificate of Incorporation or Bylaws, or required by applicable
law, holders of Class A common stock will be entitled to one vote per share on all matters submitted to a vote of stockholders and
holders of our Class B common stock will be entitled to ten votes per share on all matters submitted to a vote of stockholders.
Holders of Class A common stock and Class B common stock vote together as a single class on all matters submitted to a vote of
stockholders, except (i) amendments to Vaxxinity’s Amended and Restated
Certificate of Incorporation to increase or decrease the par value of a class of capital stock, in which case the applicable class would be
required to vote separately to approve the proposed amendment and (ii) amendments to Vaxxinity’s Amended and Restated Certificate
of Incorporation that alter or change the powers, preferences or special rights of a class of capital stock in a manner that affects its
holders adversely, in which case the applicable class would be required to vote separately to approve the proposed amendment.
Holders of common stock are entitled to receive, ratably, dividends as may be declared by Vaxxinity’s board of directors out of funds
legally available therefor if the board of directors, in its discretion, determines to issue dividends.
The voting, dividend, and liquidation rights of the holders of common stock are subject to and qualified by the rights, powers, and
preferences of the holders of Vaxxinity’s preferred stock.
The Company has reserved shares of common stock for issuance for the following purposes:
December 31,
2021
2020
Series Seed preferred
—
Series Seed-1 preferred
—
Series Seed-2 preferred
—
Series A-1 preferred
—
Series A-2 preferred
—
Options issued and outstanding
Options available for future grants
Warrants issued and outstanding
13. Equity Incentive Plan
Stock Options
In March 2021, the Company replaced the 2017 and 2020 Stock Option and Grant Plans with the newly-adopted 2021 Stock Option and
Grant Plan (the “Existing 2021 Plan”), which provided for the Company to grant qualified incentive options, nonqualified options,
restricted stock awards, unrestricted stock awards, and restricted stock units to employees and non-employees to purchase the
Company’s Class A common stock. The Existing 2021 Plan authorized the issuance of up to
stock pursuant to awards.
In August 2021, the Company canceled existing options to purchase, in aggregate,
exchange for an equal number of options to purchase shares of Class B common stock. The Company accounted for this exchange as a
stock option modification.
In November 2021, the Company replaced the Existing 2021 Plan with the 2021 Omnibus Incentive Compensation Plan (the “New 2021
Plan”), which provides for the Company to grant nonqualified stock options, incentive (qualified) stock options, stock appreciation
rights, restricted share awards, restricted stock units, performance awards, cash incentive awards and other equity-based awards
(including fully vested shares). The New 2021 Plan replaced the Existing 2021 Plan and no further grants will be made under the Existing
2021 Plan. The following is a summary of certain terms and conditions of the New 2021 Plan.
The maximum number of shares of common stock that can be issued under the New 2021 Plan is
As of December 31, 2021,
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
129
Company prior to vesting, satisfied without the issuance of stock, withheld to cover the exercise price or tax withholdings, or otherwise
terminated, other than by exercise, shall be added back to the Shares available for issuance under the New 2021 Plan.
The exercise price for grants made pursuant to the terms of the New 2021 Plan is determined in the applicable grant by the board of
directors. Any incentive options granted to persons possessing less than 10% of the total combined voting power of all classes of stock
may not have an exercise price of less than 100% of the fair market value of the common stock on the grant date. Any incentive options
granted to persons possessing more than 10% of the total combined voting power of all classes of stock may not have an exercise price
of less than 110% of the fair market value of the common stock on the grant date.
The option term for incentive awards may not be greater than ten years from the date of the grant. Incentive options granted to persons
possessing more than 10% of the total combined voting power of all classes of stock may not have an option term of greater than five
years from the date of the grant. The vesting period for equity-based awards is determined at the discretion of the board of directors.
As of December 31, 2021 there were options for
Class B stock outstanding, of which
31, 2021, the maximum number of stock options awards available for future issuance under the Company’s plans is
.
Stock Option Activity
The following table summarizes stock option activity for the years ended December 31, 2021 and 2020:
Number of Stock
Options
Outstanding
Weighted Price
Per Share
Weighted
Contractual
Term (years)
Aggregate
Intrinsic Value
(in thousands)
Balance at December 31, 2019
$
$
Granted
Exercised
(283,290 )
Forfeited
(722,752 )
Balance at December 31, 2020
$
$
Granted
Exercised
(186,204 )
Forfeited
(1,185,201 )
Balance at December 31, 2021
$
$
Options vested and exercisable at December 31, 2021
$
$
The aggregate intrinsic value of options is calculated as the difference between the exercise price of the options and the fair value of the
common stock for those options that had exercise prices lower than the fair value of the common stock.
The intrinsic value of options exercised during each of the years ended December 31, 2021 and 2020 were less than $
The weighted-average grant-date fair value per share of options granted during the years ended December 31, 2021 and 2020 was $
and $
, respectively.
The total fair value of options vested during the years ended December 31, 2021 and 2020 was $
respectively.
Valuation of Stock Options Granted that Contain Service Conditions Only
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
130
The fair value of each option award granted with service-based vesting is estimated on the date of the grant using the Black-Scholes
option valuation model based on the assumptions noted in the table below for those options granted in the years ended December 31,
2021 and 2020:
December 31,
2021
2020
Risk-free interest rate
0.59% - 1.35%
0.34% - 0.38%
Expected term (in years)
5.00 - 6.30
5.60 - 6.08
Expected volatility
71.60% - 93.40%
70.90% - 86.84%
Expected dividend yield
0.00%
0.00%
In August 2021, the Company canceled 378,786 existing Class A common stock options with service-based conditions held by Mei Mei
Hu in exchange for an equal number of options to purchase shares of Class B common stock. The Company accounted for this exchange
as a stock option modification. There was no incremental stock-based compensation expense as a result of this modification as the fair-
value-based measures of the modified award immediately after the modification were less than the fair-value-based measures of the
original award immediately before the modification.
Stock Options Granted to Employees that Contain Performance and Market Conditions
Included in the stock options granted during the year ended December 31, 2021 were stock options to purchase
Class A common stock that contain performance- and market-based vesting conditions granted to the Mei Mei Hu, Louis Reese, and
Peter Diamandis.
In August 2021, the stock option awards for the Mei Mei Hu and Louis Reese totaling
an equal number of options to purchase shares of Class B common stock. The Company accounted for this exchange as a stock option
modification. The fair value of the awards granted to Mei Mei Hu and Louis Reese at the modification date was $
using the Monte-Carlo simulation model. The assumptions used in the Monte-Carlo simulation model were as follows:
Time to expiration (in years)
Volatility
75%
Risk-free interest rate
58%
Cost of equity
25%
Fair value of underlying common stock (as of valuation date)
$
The stock option awards for Peter Diamandis totaling
in the Monte-Carlo simulation model were as follows:
Time to expiration (in years)
Volatility
90%
Risk-free interest rate
0.09%
Cost of equity
25%
Fair value of underlying common stock (as of valuation date)
$
The compensation expense for these awards is recognized when the vesting condition is met for the performance-based criteria, and
over the derived service period for the market-based criteria.
The condition for the performance-based criteria in the stock options was based on the Company's completion of its IPO, and the
condition for the market-based criteria in the stock options was based on the future price of the Company's common stock trading at or
above a specified threshold. During the year ended December 31, 2021, stock options for an aggregate of
shares containing performance- and market-based vesting conditions were vested following the satisfaction of the performance-based
condition achieved through the Company’s completion of its IPO. As of December 31, 2021, the market-based vesting conditions had
not been achieved.
Restricted Stock
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
131
The following table summarizes the Company’s restricted stock activity for the year ended December 31, 2021:
Number of
Shares
Weighted
Average
Grant Date
Fair Value
Per Share
Unvested at December 31, 2020
$
Vested
(15,405 )
(0.50 )
Unvested at December 31, 2021
—
$
—
The aggregate fair value of restricted stock that vested was less than $
Stock-based compensation expense recognized on vested restricted stock was immaterial for the years ended December 31, 2021 and
2020.
Stock-Based Compensation Expense
The Company recorded stock-based compensation expense in the following expense categories in the accompanying consolidated
statements of operations (in thousands):
Years Ended December 31,
2021
2020
Research and development
$
$
General and administrative
Total stock-based compensation expense
$
$
As of December 31, 2021, total unrecognized compensation cost related to the unvested stock-based awards was $
is expected to be recognized over a weighted average period of
14. Income Taxes
The sources of losses from continuing operations, before income taxes, classified between domestic entities and those entities domiciled
outside of the U.S., are as follows (in thousands):
Years Ended December 31,
Losses before taxes
2021
2020
Domestic entities
$
(128,538 )
$
(31,053 )
Entities outside the U.S.
(8,636 )
(8,904 )
(137,175 )
$
(39,957 )
Tax Expense (Benefit)
The components of the provision for income taxes are as follows for the years ended December 31, 2021 and 2020 (in thousands):
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
132
Years Ended December 31,
2021
2020
Current:
Federal
$
—
$
—
State and local
—
—
Foreign
—
—
Total current tax expense
—
—
Deferred tax (benefit):
Federal
—
—
State and local
—
—
Foreign
—
—
Total deferred tax (benefit)
—
—
Tax Rate Reconciliation
The Company’s effective tax rate for the years ended December 31, 2021 and 2020 was
% and
%, respectively.
A reconciliation of the provision for income taxes at the statutory rate to the amount reflected in the consolidated statements of operations
is as follows (in thousands):
Years Ended December 31,
2021
2020
Income taxes at statutory rate
%
%
State income taxes, net of federal benefit
%
%
Stock compensation
(3.65)
%
%
Foreign rate differential
(0.74 )
%
(4.06 )
%
Uncertain tax positions
%
%
Other
(1.90 )
%
(0.36 )
%
Change in valuation allowance
(15.21 )
%
(16.87 )
%
Provision for income taxes
%
%
Deferred Tax Assets (Liabilities)
The Company computes income taxes using the liability method. This method requires recognition of deferred tax assets and liabilities,
measured by enacted rates, attributable to temporary differences between the financial statements and the income tax basis of assets and
liabilities. In assessing the realizability of deferred tax assets, the Company considers whether it is more likely than not that certain
deferred tax assets will be realized. The ultimate realization of deferred tax assets is dependent upon the generation of future taxable
income in those specific jurisdictions prior to the dates on which such net operating losses expire. The Company maintained a full
valuation allowance against its net deferred tax assets for December 31, 2021 and 2020 because the Company has determined that it is
more likely than not that these assets will not be fully realized based on a current evaluation of expected future taxable income and the
Company is in a cumulative loss position. The valuation allowance increased by $
and $
The Company reevaluates the positive and negative evidence at each reporting period.
Significant components of the Company’s deferred tax assets and liabilities are as follows (in thousands):
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
133
As of December 31,
2021
2020
Deferred tax assets:
Net operating loss carryforwards
$
$
Compensation accruals
Other
Total deferred tax assets
Less: valuation allowance
(34,106 )
(13,247 )
Net deferred tax assets
$
$
Deferred tax liabilities:
Depreciation
$
(61 )
$
(130 )
Net deferred tax liabilities
(61 )
(130 )
Net deferred income taxes
$
—
$
—
Net Operating Losses
The Company had total net operating loss carryforwards for U.S. federal income tax purposes of $
of December 31, 2021 and 2020, respectively, that have no expiration date. The Company has foreign net operating loss carryforwards
of $
Utilization of the NOL carryforwards and credits may be subject to a substantial annual limitation due to the ownership change
limitations provided by the Internal Revenue Code Sections 382 and 383 (the “Code”), as amended, and similar state provisions. The
Company has not completed a study to assess whether an ownership change has occurred or whether there have been multiple ownership
changes since the Company’s formation due to the complexity and cost associated with such a study, and the fact that there may be
additional ownership changes in the future. If the Company experienced an ownership change at any time since its formation, utilization
of the NOL or tax credit carryforwards to offset future taxable income and taxes, respectively, would be subject to annual limitation
under the Code. The annual limitation may result in the expiration of the NOL and credits before utilization. If impaired, the NOL and
credit carryforwards would be removed from the deferred tax asset schedule with a corresponding reduction in the valuation allowance.
On March 27, 2020, the President of the United States signed into law the CARES Act, which, along with earlier issued IRS guidance,
contains numerous provisions that may benefit the Company, including the deferral of certain taxes. There is no material impact to the
Company. The CARES Act did not have a material impact on the Company’s tax provision for the year ended December 31, 2021.
The Consolidated Appropriations Act, 2021, which was enacted on December 27, 2020, has expanded, extended, and clarified selected
CARES Act provisions, specifically on Paycheck Protection Program loan and Employee Retention Tax Credit, 100% deductibility of
business meals as well as other tax extenders. The Consolidated Appropriations Act did not have a material impact on the Company’s
tax provision for the year ended December 31, 2021.
The Company is subject to tax in the United States and many state and local jurisdictions. The Company, with certain exceptions, is
subject to income tax examinations by U.S. federal, state and local for tax years 2017 and future periods. The company is not currently
under audit for any US federal or state or foreign income tax audits.
Uncertain Tax Positions
A summary of the Company’s unrecognized tax benefits activity and related information is presented as follows (in thousands):
Years Ended December 31,
2021
2020
Uncertain tax position liability at the beginning of the year
$
$
Increases (decreases) related to tax positions taken during current period
Uncertain tax position liability at the end of the year
$
$
The unrecognized tax benefits for U.S. jurisdiction of $
tax rate assuming the Company continues to maintain a full valuation allowance position against its U.S. deferred tax assets. The
remaining unrecognized tax benefits of less than $
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
134
recognizes accrued interest and penalties related to unrecognized tax benefits in income tax expense. We accrued $
and penalties related to prior year’s tax filings, as of December 31, 2021.
The Company is subject to U.S. federal income tax as well as income tax of various foreign jurisdictions. Generally, the statute of
limitations for examination of the Company’s U.S. federal and foreign income tax filings are open for the years ended December 31,
2017 and future periods.
15. Net Loss Per Share
The Company’s unvested restricted common shares have been excluded from the computation of basic net loss per share.
The Company’s potentially dilutive securities, which include options, unvested restricted stock, convertible notes payable and
convertible preferred stock, have been excluded from the computation of diluted net loss per share as the effect would be to reduce the
net loss per share. Therefore, the weighted average number of common shares outstanding used to calculate both basic and diluted net
loss per share is the same. The Company excluded the following potential common shares, presented based on amounts outstanding at
each period end, from the computation of diluted net loss per share as of December 31, 2021 and 2020 because including them would
have had an anti-dilutive effect:
December 31,
2021
2020
Series Seed preferred
Series Seed-1 preferred
Series Seed-2 preferred
Series A-1 preferred
Series A-2 preferred
Unvested restricted stock
Options and RSUs issued and outstanding
Warrants issued and outstanding stock
16. Commitments and Contingencies
Contractual Obligations
The Company enters into agreements with contract research organizations (“CROs”) to conduct clinical trials and preclinical studies
and contract manufacturing organizations (“CMOs”) to produce vaccines and other potential product candidates. Contracts with CROs
and CMOs are generally cancellable, with notice, at the Company’s option.
As of December 31, 2021, the Company had remaining prepayments to CROs of $
$
product candidate.
Michael J. Fox Foundation Grant
On November 3, 2021, the Company was awarded a grant from the Michael J. Fox Foundation for Parkinson’s Research (“MJFF”) in
the amount of $
UB-312, an active
a
-Synuclein immunotherapy. The Company will oversee sample management, sample preparation (IgG fractions)
and distribution, as well as characterize the binding properties of the antibodies against pathological forms of aSyn. As funding is
expected to be utilized over a two-year period, as cash is received, the amount expected to the utilized within twelve months is recognized
to short-term restricted cash/deposits, with a corresponding short-term accrued liability, which is released as the related expenses are
offset. The Company recognizes payments from MJFF as a reduction of research and development expenses, in the same period as the
expenses that the grant is intended to reimburse are incurred. The remaining balance of cash received is recognized to long-term restricted
cash/deposits, with a corresponding long-term accrued liability. As of December 31, 2021, the balance of short-term restricted
cash/deposits and the corresponding short-term accrued liability was $
corresponding long-term accrued liability was $
. For the year ended December 31, 2021, the Company recognized less than $
million as a reduction of research and development expenses for amounts reimbursed through the grant.
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
135
Lease Agreements
The Company has multiple operating lease agreements for office and laboratory space that extend through August 2022. The Company
records total expense on a straight-line basis over the term of the lease agreement. One of the Company’s leases requires the Company
to provide a security deposit in the amount of less than $
its leases.
Rent expense for each of the years ended December 31, 2021 and 2020 amounted to less than $
In August 2021, the Company entered into a lease for
commencing August 12, 2021. The lease has an initial one-year term with an annual lease obligation of $
License Agreements
In October 2014, the Company entered into a contribution agreement with UBI, whereby UBI contributed and assigned to the Company
assets and granted a non-exclusive license to certain technologies deemed necessary or reasonably useful in the utilization of the licensed
intellectual property. In consideration, the Company issued
exploitation of all diagnostic, prophylactic, and therapeutic uses and indications in humans in the field of neurology. The agreement was
amended in August 2019 to provide the Company with exclusivity (except as to UBI) in the field of neurology and the flexibility to
pursue indications outside the initial field limitations.
In connection with the amendment, the Company agreed to execute an exclusive, worldwide license agreement for any product that is
developed by the Company outside the original field. The terms and conditions are to be negotiated in good faith and mutually agreed
upon. The Company anticipates that if it is required to enter into an exclusive license agreement, it will be able to negotiate financial
terms for the license at prevailing market rates within the pharmaceutical industry. Accordingly, the Company may be required to pay
UBI upfront fees, revenue royalties, development milestones, commercial milestones, sublicense fees, and other related fees.
Vaxxinity’s COVAXX subsidiary was formed in March 2020 through a transfer of technology from UBI, UBI IP Holdings, and UBI
US Holdings, LLC, all related parties of the Company, whereby the Company, pursuant to an April 2020 license agreement, obtained
exclusive rights to intellectual property and technology related to the discovery of vaccines, diagnostic assays, and antigens for use
against all coronaviruses including, without limitation, SARS, MERS, and COVID-19 in all strains in humans. The license is worldwide,
perpetual, exclusive and fully paid-up. There are no future royalty or milestone payment obligations associated with the agreement. The
Company has the right to grant sublicenses.
The Company considered ASC 805, “Business Combinations” and ASC 730, “Research and Development” in determining how to
account for the issuance of common stock. The license agreement is considered to be a common control transfer; however, the related
party did not have any basis in the assets licensed, so there was no accounting impact for the Company.
In August 2021, Vaxxinity entered into a license agreement (the “Platform License Agreement”) with UBI and certain of its affiliates
that expanded intellectual property rights previously licensed under previously issued license agreements with UBI. As part of the
agreement, Vaxxinity obtained a worldwide, sublicensable (subject to certain conditions), perpetual, fully paid-up, royalty-free license
to research, develop, make, have made, utilize, import, export, market, distribute, offer for sale, sell, have sold, commercialize or
otherwise exploit peptide-based vaccines in the field of all human prophylactic and therapeutic uses, except for such vaccines related to
human immunodeficiency virus (HIV), herpes simplex virus (HSE) and Immunoglobulin E (IgE). The patents and patent applications
licensed under the Platform License Agreement include claims directed to a CpG delivery system, artificial T helper cell epitopes and
certain designer peptides and proteins utilized in UB-612. As described above, in consideration for the Platform License Agreement,
the Company issued to UBI a warrant to purchase Class A common stock (the “UBI Warrant”).
The Company considered ASC 805, “Business Combinations” (“ASC 805”) and ASC 730, “Research and Development” (“ASC 730”)
in determining how to account for the issuance of the Class A common stock warrants. The Class A common stock warrants were issued
to a related party in exchange for a license agreement. The majority of the voting interests in the related party and that of the Company
were held by a group of immediate family members, at the time of the transaction, and as such the transaction constitutes a common
control transaction, which requires the license to be accounted for at the carrying value in the books of the transferor. As the related
party did not have any basis in the assets licensed, there was no accounting impact for the Company.
In connection with preparing its financial statements for the fiscal year ended December 31, 2021, the Company identified an immaterial
error relating to the recording of the UBI Warrant on its financial statements as of and for the nine months ended September 30, 2021.
The UBI Warrant was recorded on the balance sheet as additional paid in capital and recognized as an ‘intangible asset – licensed
intellectual property’ in the amount of $
However, as noted above, the UBI Warrant was issued to a related party whose basis in the rights and licenses received pursuant to the
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
136
Platform License Agreement was zero. As a result, the transaction should not have resulted in any accounting impact to the Company.
The Company has concluded that the error is not material to any previously issued financial statements.
Indemnification Agreements
In the ordinary course of business, the Company may provide indemnification of varying scope and terms to employees, consultants,
vendors, lessors, business partners and other parties with respect to certain matters including, but not limited to, losses arising out of
breach of such agreements or from intellectual property infringement claims made by third parties. In addition, the Company has entered
into indemnification agreements with members of its board of directors and executive officers that will require the Company, among
other things, to indemnify them against certain liabilities that may arise by reason of their status or service as directors or officers. The
maximum potential amount of future payments the Company could be required to make under these indemnification agreements is, in
many cases, unlimited. To date, the Company has not incurred any material costs as a result of such indemnifications. The Company is
not aware of any indemnification arrangements that could have a material effect on its financial position, results of operations, or cash
flows, and it has not accrued any liabilities related to such obligations as of December 31, 2021.
Legal Proceedings
From time to time, the Company may become involved in legal proceedings arising in the ordinary course of business. As of
December 31, 2021, the Company was not a party to any material legal matters or claims.
17. Benefit Plans
In March 2018, the Company established a defined contribution savings plan under Section 401(k) of the Code. This plan covers
substantially all U.S. employees who meet minimum age and service requirements and allows participants to defer a portion of their
annual compensation on a pre-tax basis. The Company does not make matching contributions to the Plan.
The Company offers its Ireland-based employees a Personal Retirement Savings Account (“PRSA”) that allows participants to defer a
portion of their annual compensation. The Company provides contributions equal to
% of each participant’s annual salary. During both
of the years ended December 31, 2021 and 2020, the Company contributed less than $
18. Related Party Transactions
The Company has a Related Party policy which defines related parties, and assigns oversight responsibility for related party transactions
to the Company's Audit Committee. The Committee reviews in advance related party transactions, and considers multiple factors,
including the proposed aggregate value of the transaction, or, in the case of indebtedness, the amount of principal that would be involved,
the benefits to the Company of the proposed transaction, the availability of other sources of comparable products or services, and an
assessment of whether the proposed transaction is on terms that are comparable to the terms available to or from, as the case may be,
unrelated third parties. Under the policy, related party transactions are approved only if the Committee determines in good faith that
the transaction is not inconsistent with the interests of the Company and its shareholders.
The Company has related party arrangements with UBI and a number of its affiliated companies listed namely, United Biomedical, Inc.,
Asia (“UBI-Asia”), UBI Pharma, Inc. (“UBI-P”), United BioPharma, Inc (“UBP”) and UBI IP Holding (“UBI-IP”).
As of December 31, 2021 UBI owned
% of the Company’s stock on an as converted basis. The majority of the voting interests in
both UBI and the Company were held by a group of immediate family members, and as such the entities are under common control.
These related parties are governed by various Master Services Agreements (“MSA”) detailed below.
UBI MSA - UBI provides research, development and clinical functions to the Company. There is also a purchase arrangement with
UBI for the production and shipment of the Company’s diagnostic test kits.
UBIA MSA - UBI-Asia for manufacturing, quality control, testing, validation, and supply services.
UBP MSA - United BioPharma, Inc provide the Company with manufacturing, testing and validation.
COVID MSA (“COVID MSA”) - COVID MSA provides that UBI acts as COVAXX’s agent with respect to matters relating the
Company’s COVID-19 program and provides research, development, manufacturing and back office administrative services to the
Company.
VAXXINITY, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
137
COVID-19 Relief MSA - A four-company MSA with UBI, UBI-Asia and UBP. The Company is an exclusive licensee of
technologies related to diagnostics, vaccines, and therapies for COVID-19. The MSA established the terms under which UBI-Asia
provides research, development, testing and manufacturing services to the Company and UBP provides contract development and
manufacturing services to the Company.
Total amounts due to related parties were $
due from related parties were $
fees incurred were $
Taiwan Centers for Disease Control Grant (“Taiwan CDC”)
UBI-Asia, which is responsible for applying for and managing grants on our behalf under the COVID-19 program, was awarded a grant
by the Taiwan CDC for COVID-19 vaccine development. The Company contracted with UBI-Asia to conduct a two-phase study of a
COVID-19 vaccine clinical trial in Taiwan. The grant provides that costs incurred to complete the two phases of the clinical trial will
be reimbursed based on the achievement of certain milestones as provided in the agreement.
The Company provides administrative services to UBI-IP. Under the arrangement, the Company issues vendor payments and provides
technical services mostly for legal services on behalf UBI-IP. The Company bills UBI-IP for services based on the costs incurred with
no markup.
Total related party operating activity, including the activity described above, for the years ended December 31, 2021 and 2020 are as
follows (in thousands):
December 31,
2021
2020
Consolidated balance sheet
Assets
Prepaid expenses and other current assets
$
$
Property and equipment, net
Accrued expenses
Amounts due from related parties
Liabilities
Amounts due to related parties
Years Ended December 31,
2021
2020
Consolidated statement of operations
Revenue
$
$
Cost of revenue
Operating expenses
Research and development
Services provided by related parties
Taiwan CDC grant reimbursement from related party
(7,199 )
(2,948 )
General and administrative
Services provided by related parties
19. Subsequent Events
The Company has evaluated subsequent events through March 24, 2022 and has concluded that no events or transactions have occurred
that require disclosure in the accompanying consolidated financial statements.
138
Item 9. Changes in and Disagreements with Accountants on Accounting and Financial Disclosure.
None.
Item 9A. Controls and Procedures.
Evaluation of disclosure controls and procedures
Our management, with the participation of our principal executive officer and principal accounting officer, evaluated, as of the end of
the period covered by this Annual Report on Form 10-K, the effectiveness of our disclosure controls and procedures (as defined in Rules
13a-15(e) and 15d-15(e) under the Exchange Act). In designing and evaluating our disclosure controls and procedures, management
recognizes that any controls and procedures, no matter how well designed and operated, can provide only reasonable assurance of
achieving the desired control objectives. In addition, the design of disclosure controls and procedures must reflect the fact that there are
resource constraints, and that management is required to apply judgment in evaluating the benefits of possible controls and procedures
relative to their costs. Based on management’s evaluation and as a result of the material weaknesses described below, our principal
executive officer and principal accounting officer concluded that, as of December 31, 2021, our disclosure controls and procedures were
not effective at the reasonable assurance level.
Report on Internal Control Over Financial Reporting
This Report does not include a report of management’s assessment regarding internal control over financial reporting or an attestation
report of our independent registered public accounting firm due to a transition period established by the rules of the SEC for newly
public companies.
Material Weaknesses in Internal Control over Financial Reporting
A material weakness is a deficiency, or combination of deficiencies, in internal control over financial reporting, such that there is a
reasonable possibility that a material misstatement of a company’s annual and interim financial statements will not be detected or
prevented on a timely basis.
Management identified material weaknesses in the design and operation of our internal controls over financial reporting during the
preparation of our audited consolidated financial statements for the year ended December 31, 2021. These material weaknesses related
to:
• performing our financial close process, including account reconciliation and analysis on a timely basis, accruing for related-party
transactions, recording stock-based compensation expense and aggregating and mapping amounts from trial balances to financial
statements;
• ensuring that formal processes exist for identifying, analyzing and accounting for key contracts and complex, non-routine
transactions; and
• proper segregation of duties and responsibilities within our finance department, including authorization and review of accounting
entries.
Remediation Measures
We are investing resources to remediate the material weaknesses identified in the preparation of our audited consolidated financial
statements for the year ended December 31, 2021 described above through a combination of hiring additional qualified accounting and
financial reporting personnel and further evolving and refining our accounting processes and policies. These remediation activities
involve the following:
• having hired, and continuing to hire, additional accounting personnel with the appropriate level of skill and experience for public
company financial reporting;
• designing and implementing a formal financial close process that includes multiple levels of reviews of accounting entries; and
• supplementing our resources for evaluating and accounting for complex transactions and stock options through the use of third-
party advisors.
While we are working to remediate the identified material weaknesses as timely and efficiently as possible, at this time we cannot
provide an estimate of costs expected to be incurred in connection with our remediation efforts, we cannot provide an estimate of the
time it will take to complete remediation, nor can we provide assurance that our efforts will successfully prevent any errors or omissions
that may result because of these material weaknesses.
139
Changes in Internal Control over Financial Reporting
Other than the measures described in “Remediation Measures” above, there were no changes in our internal control over financial
reporting (as defined in Rules 13a-15(f) and 15d-15(f) under the Exchange Act) during the quarter ended December 31, 2021 that have
materially affected, or are reasonably likely to materially affect, our internal control over financial reporting.
Item 9B. Other Information.
None.
Item 9C. Disclosure Regarding Foreign Jurisdictions that Prevent Inspections.
The disclosure required by this item is not applicable.
PART III
Items 10, 11, 12, 13 and 14.
Our independent registered public accounting firm is Armanino LLP, San Ramon, California, Auditor Firm ID: 32.
The information required by these items is incorporated by reference to our definitive proxy statement relating to our 2022 Annual
Meeting of Shareholders. We currently anticipate that our definitive proxy statement will be filed with the SEC not later than 120 days
after December 31, 2021, pursuant to Regulation 14A of the Securities Exchange Act of 1934, as amended.
PART IV
Item 15. Exhibits and Financial Statement Schedules.
(a) Documents filed as part of this Report:
(1) Financial Statements. The following consolidated financial statements and the notes thereto, and the Reports of Independent
Registered Public Accounting Firm are incorporated by reference as provided in Item 8 and Item 9A of this Report:
Audited Consolidated Financial Statements as of and for the years ended December 31, 2021 and 2020
106
107
108
109
109
111
113
(2) Financial Statement Schedules.
[IF ANY]
140
(b) Exhibits:
The following exhibits required by Item 601 of Regulation S-K are filed herewith or have been filed previously with the SEC as indicated
below:
Exhibit
No.
Index to Exhibits
Amended and Restated Certificate of Incorporation of Vaxxinity, Inc. to be in effect upon the completion of this
offering (incorporated by reference to Exhibit 3.1 of our Current Report on Form 8-K (File No. 001-41058) filed on
November 17, 2021).
Amended and Restated Bylaws of Vaxxinity, Inc. to be in effect upon the completion of this offering (incorporated by
reference to Exhibit 3.2 of our Current Report on Form 8-K (File No. 001-41058) filed on November 17, 2021).
Description of Registered Securities*
Registration Rights Agreement (incorporated by reference to Exhibit 10.2 of our Current Report on Form 8-K (File No.
001-41058) filed on November 17, 2021).
141
101.INS
Inline XBRL Instance Document*
101.SCH
Inline XBRL Taxonomy Extension Schema Document*
101.CAL
Inline XBRL Taxonomy Extension Calculation Linkbase Document*
101.DEF
Inline XBRL Taxonomy Extension Definition Linkbase Document*
101.LAB
Inline XBRL Taxonomy Extension Label Linkbase Document*
101.PRE
Inline XBRL Taxonomy Extension Presentation Linkbase Document*
104
Cover Page Interactive Data File (the cover page XBRL tags are embedded within the Inline XBRL document).*
__________________________
* Filed herewith.
† Indicates management contract or compensatory plan, contract or arrangement.
§ Portions of the exhibit, marked by brackets, have been omitted because the omitted information (i) is not material and (ii) would
likely cause competitive harm if publicly disclosed.
‡ The certifications attached as Exhibits 32.1 that accompany this Form 10-K are deemed furnished and not filed with the
Securities and Exchange Commission and are not to be incorporated by reference into any filing of Vaxxinity, Inc. under the
Securities Act of 1933, as amended, or the Securities Exchange Act of 1934, as amended, whether made before or after the date of this
Form 10-K, irrespective of any general incorporation language contained in such filing.
(c) Schedules:
None
Item 16. Form 10-K Summary.
None.
142
SIGNATURES
Pursuant to the requirements of the Securities Exchange Act of 1934, the registrant has duly caused this Annual Report on Form 10-K
to be signed on its behalf by the undersigned, thereunto duly authorized on March 24, 2022.
VAXXINITY, INC.
By:
/s/ Mei Mei Hu
Mei Mei Hu, President and
Chief Executive Officer
ADDITIONAL SIGNATURES AND POWERS OF ATTORNEY
KNOW ALL PERSONS BY THESE PRESENTS, that each person whose signature appears below constitutes and appoints Mei Mei
Hu and René Paula, jointly and severally, her or his attorney-in-fact, with the power of substitution, for her or him in any and all
capacities, to sign any amendments to this Annual Report on Form 10-K and to file the same, with exhibits thereto and other documents
in connection therewith, with the Securities and Exchange Commission, hereby ratifying and confirming all that each of said attorneys-
in-fact, or her or his substitute or substitutes, may do or cause to be done by virtue hereof.
Pursuant to the requirements of the Securities Exchange Act of 1934, as amended, this Annual Report on Form 10-K has been signed
below by the following persons in the capacities indicated on March 24, 2022.
Signature
Capacity in Which Signed
/s/: Mei Mei Hu
President, Chief Executive Officer and Director
Mei Mei Hu
(Principal executive officer)
/s/: Jason Pesile
Senior Vice President, Finance & Accounting
Jason Pesile
(Principal financial and accounting officer)
/s/: Louis Reese
Director
Louis Reese
/s/: George Hornig
Director
George Hornig
/s/: Greg Blatt
Director
Greg Blatt
/s/: Peter Diamandis
Director
Peter Diamandis
/s/: James Chui
Director
James Chui