
HealthSouth is a leading provider of post-acute healthcare services, offering both facility-based
and home-based post-acute services in 34 states and Puerto Rico through its network of
inpatient rehabilitation hospitals, home health agencies, and hospice agencies.
Investor Reference Book
Post Q4 2017 Earnings Release
Last Updated March 13, 2018

Encompass Health 2
Forward-Looking Statements
The information contained in this Investor Reference Book includes certain estimates, projections and other forward-
looking information that reflect Encompass Health’s current outlook, views and plans with respect to future events,
including legislative and regulatory developments, strategy, capital expenditures, acquisition and other development
activities, cyber security, dividend strategies, repurchases of securities, effective tax rates, financial performance,
financial assumptions, business model, balance sheet and cash flow plans, disintermediation, and shareholder value-
enhancing transactions. These estimates, projections and other forward-looking information are based on assumptions
the Company believes, as of the date hereof, are reasonable. Inevitably, there will be differences between such
estimates and actual events or results, and those differences may be material.
There can be no assurance any estimates, projections or forward-looking information will be realized.
All such estimates, projections and forward-looking information speak only as of the date hereof. Encompass
Health undertakes no duty to publicly update or revise the information contained herein.
You are cautioned not to place undue reliance on the estimates, projections and other forward-looking information in
this Investor Reference Book as they are based on current expectations and general assumptions and are subject to
various risks, uncertainties and other factors, including those set forth in the Form 10-K for the year ended
December 31, 2017 and in other documents Encompass Health previously filed with the SEC, many of which are
beyond Encompass Health’s control, that may cause actual events or results to differ materially from the views,
beliefs, and estimates expressed herein.
Note Regarding Presentation of Non-GAAP Financial Measures
The following Investor Reference Book includes certain “non-GAAP financial measures” as defined in Regulation G
under the Securities Exchange Act of 1934, including Adjusted EBITDA, leverage ratios, adjusted earnings per share,
and adjusted free cash flow. Schedules are attached that reconcile the non-GAAP financial measures included in the
following Investor Reference Book to the most directly comparable financial measures calculated and presented in
accordance with Generally Accepted Accounting Principles in the United States. The Company’s Form 8-K, dated
March 13, 2018, to which the following Investor Reference Book is attached as Exhibit 99.1, provides further
explanation and disclosure regarding Encompass Health’s use of non-GAAP financial measures and should be read in
conjunction with this Investor Reference Book.

Encompass Health 3
Company Overview . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 4-16
Investment Thesis and Strategy . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 17-24
Business Outlook, Including Guidance . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 25-40
Growth . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 41-52
Alternative Payment Models . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 53-58
Capital Structure . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 59-64
Information Technology. . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 65-68
Operational Metrics . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 69-74
Industry Structure . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 75-87
Segment Operating Results . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 88-92
Reconciliations to GAAP and Share Information . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 93-105
End Notes. . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 106-110
Table of Contents

Encompass Health 4
Company Overview
Encompass Health is a leading provider of inpatient rehabilitation and
home-based care committed to delivering high-quality, cost-effective,
integrated care across the post-acute continuum.
Encompass Health 5
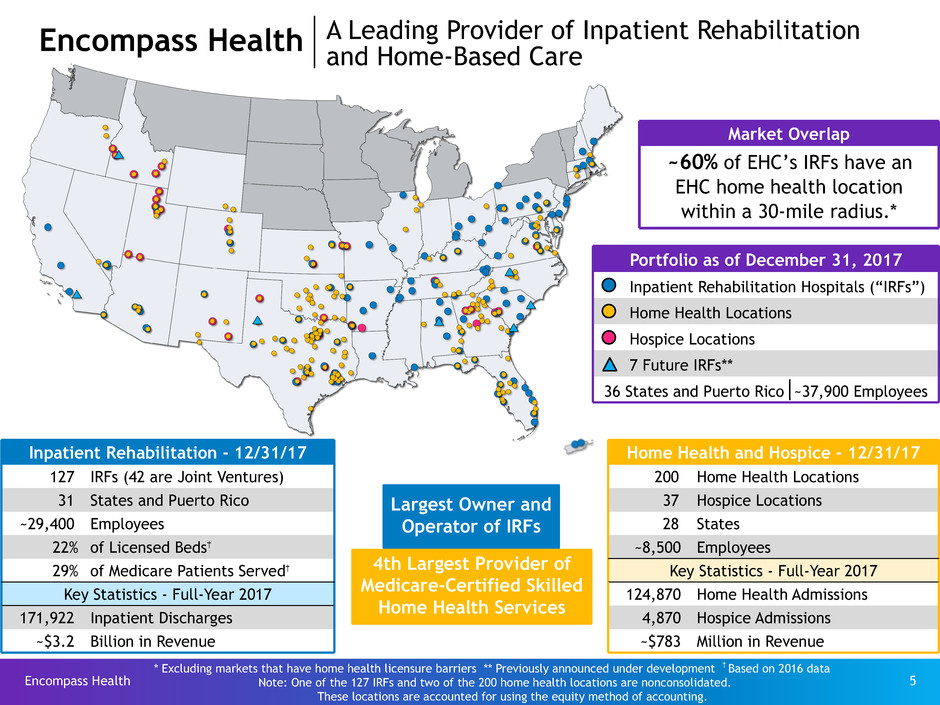
Portfolio as of December 31, 2017
Inpatient Rehabilitation Hospitals (“IRFs”)
Home Health Locations
Hospice Locations
7 Future IRFs**
36 States and Puerto Rico ~37,900 Employees
* Excluding markets that have home health licensure barriers ** Previously announced under development † Based on 2016 data
Note: One of the 127 IRFs and two of the 200 home health locations are nonconsolidated.
These locations are accounted for using the equity method of accounting.
Encompass Health A Leading Provider of Inpatient Rehabilitation and Home-Based Care
Market Overlap
~60% of EHC’s IRFs have an
EHC home health location
within a 30-mile radius.*
Inpatient Rehabilitation - 12/31/17
127 IRFs (42 are Joint Ventures)
31 States and Puerto Rico
~29,400 Employees
22% of Licensed Beds†
29% of Medicare Patients Served†
Key Statistics - Full-Year 2017
171,922 Inpatient Discharges
~$3.2 Billion in Revenue
Largest Owner and
Operator of IRFs
4th Largest Provider of
Medicare-Certified Skilled
Home Health Services
Home Health and Hospice - 12/31/17
200 Home Health Locations
37 Hospice Locations
28 States
~8,500 Employees
Key Statistics - Full-Year 2017
124,870 Home Health Admissions
4,870 Hospice Admissions
~$783 Million in Revenue

Encompass Health 6
Major Services
• Rehabilitation Physicians: manage and treat medical conditions and oversee rehabilitation program
• Rehabilitation Nurses: provide personal care and oversee treatment plan for patients
• Physical Therapists: address physical function, mobility, strength, balance, and safety
• Occupational Therapists: promote independence through activities of daily living (“ADLs”)
• Speech-Language Therapists: address speech/voice functions, swallowing, memory/cognition, and
language/communication
• Case Managers: coordinate care plan with physician, Care Transition Coordinators, caregivers and family
• Post-Discharge Services: outpatient therapy and home health
Inpatient Rehabilitation
Hospitals
Refer to pages 106-110 for end notes.
105 of the Company’s IRFs hold one or more disease-specific
certifications from The Joint Commission’s Disease-Specific
Care Certification Program.(1)
Company Overview Inpatient Rehabilitation

Encompass Health 7
Major Services
• Skilled Nurses: comprehensively assess, teach, train, and manage care related to injury or illness
• Home Health Aides: provide personal care and assistance with ADLs
• Physical Therapists: address physical function, mobility, strength, balance, and safety
• Occupational Therapists: promote independence through training on self-management of ADLs
• Speech-Language Therapists: address speech/voice functions, swallowing, memory/cognition, and
language/communication
• Medical Social Workers: provide assessment of social and emotional factors; assist with obtaining
community resources
Home Health Agencies
The Company offers evidence-based specialty programs
related to: Post-Operative Care, Fall Prevention, Chronic
Disease Management, and Transitional Care.
Hospice: provides services to terminally ill patients and their families to address patients’ physical needs,
including pain control and symptom management, and also provides emotional and spiritual support.
Company Overview Home Health and Hospice
Encompass Health 8
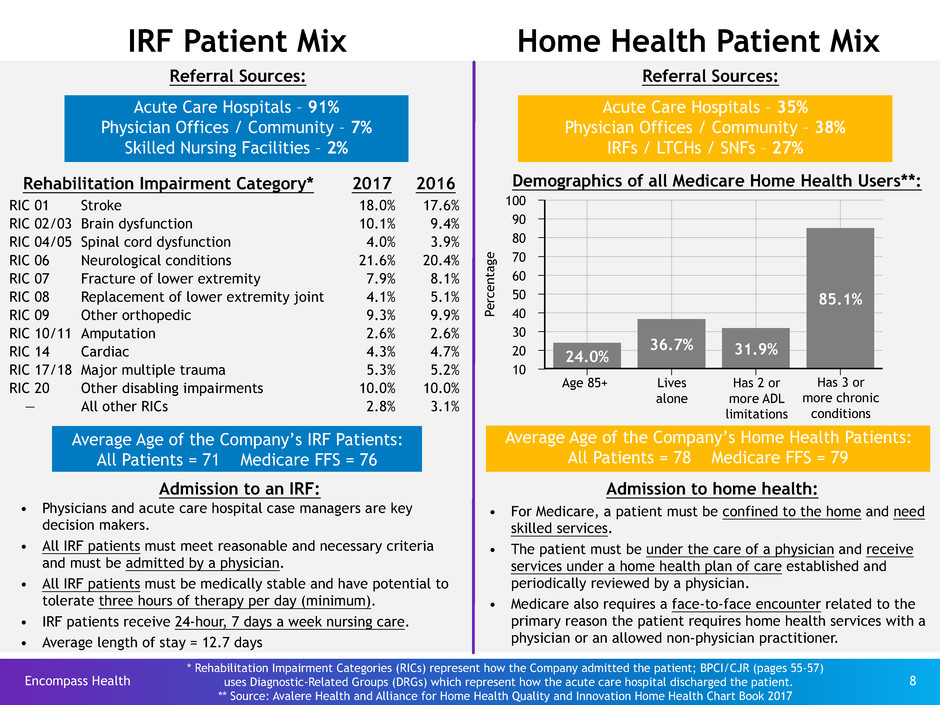
IRF Patient Mix
Referral Sources:
• Physicians and acute care hospital case managers are key
decision makers.
• All IRF patients must meet reasonable and necessary criteria
and must be admitted by a physician.
• All IRF patients must be medically stable and have potential to
tolerate three hours of therapy per day (minimum).
• IRF patients receive 24-hour, 7 days a week nursing care.
• Average length of stay = 12.7 days
Admission to an IRF:
Average Age of the Company’s IRF Patients:
All Patients = 71 Medicare FFS = 76
Home Health Patient Mix
Acute Care Hospitals – 91%
Physician Offices / Community – 7%
Skilled Nursing Facilities – 2%
Referral Sources:
• For Medicare, a patient must be confined to the home and need
skilled services.
• The patient must be under the care of a physician and receive
services under a home health plan of care established and
periodically reviewed by a physician.
• Medicare also requires a face-to-face encounter related to the
primary reason the patient requires home health services with a
physician or an allowed non-physician practitioner.
Admission to home health:
100
90
80
70
60
50
40
30
20
10
Pe
rc
en
ta
ge
24.0%
36.7% 31.9%
85.1%
Age 85+ Lives
alone
Has 2 or
more ADL
limitations
Has 3 or
more chronic
conditions
Demographics of all Medicare Home Health Users**:
* Rehabilitation Impairment Categories (RICs) represent how the Company admitted the patient; BPCI/CJR (pages 55-57)
uses Diagnostic-Related Groups (DRGs) which represent how the acute care hospital discharged the patient.
** Source: Avalere Health and Alliance for Home Health Quality and Innovation Home Health Chart Book 2017
Rehabilitation Impairment Category* 2017 2016
RIC 01 Stroke 18.0% 17.6%
RIC 02/03 Brain dysfunction 10.1% 9.4%
RIC 04/05 Spinal cord dysfunction 4.0% 3.9%
RIC 06 Neurological conditions 21.6% 20.4%
RIC 07 Fracture of lower extremity 7.9% 8.1%
RIC 08 Replacement of lower extremity joint 4.1% 5.1%
RIC 09 Other orthopedic 9.3% 9.9%
RIC 10/11 Amputation 2.6% 2.6%
RIC 14 Cardiac 4.3% 4.7%
RIC 17/18 Major multiple trauma 5.3% 5.2%
RIC 20 Other disabling impairments 10.0% 10.0%
— All other RICs 2.8% 3.1%
Acute Care Hospitals – 35%
Physician Offices / Community – 38%
IRFs / LTCHs / SNFs – 27%
Average Age of the Company’s Home Health Patients:
All Patients = 78 Medicare FFS = 79
Encompass Health 9
2015 2016 2017
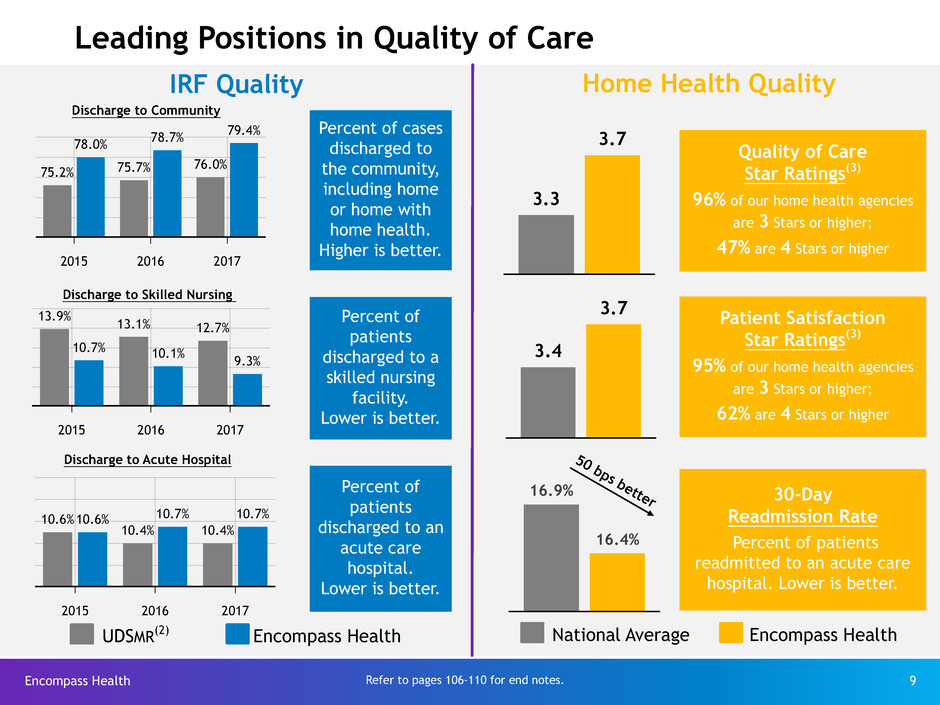
10.6%
10.4% 10.4%
10.6% 10.7% 10.7%
2015 2016 2017
13.9% 13.1% 12.7%
10.7% 10.1% 9.3%
2015 2016 2017
75.2% 75.7% 76.0%
78.0% 78.7%
79.4%
Home Health QualityIRF Quality
Discharge to Community
Discharge to Skilled Nursing
Discharge to Acute Hospital
Refer to pages 106-110 for end notes.
3.3
3.7 Quality of Care
Star Ratings(3)
96% of our home health agencies
are 3 Stars or higher;
47% are 4 Stars or higher
3.4
3.7 Patient Satisfaction
Star Ratings(3)
95% of our home health agencies
are 3 Stars or higher;
62% are 4 Stars or higher
Encompass Health
16.9%
16.4%
30-Day
Readmission Rate
Percent of patients
readmitted to an acute care
hospital. Lower is better.
50 bps bette
r
UDSMR(2) Encompass Health
Leading Positions in Quality of Care
National Average
Percent of cases
discharged to
the community,
including home
or home with
home health.
Higher is better.
Percent of
patients
discharged to a
skilled nursing
facility.
Lower is better.
Percent of
patients
discharged to an
acute care
hospital.
Lower is better.
Encompass Health 10
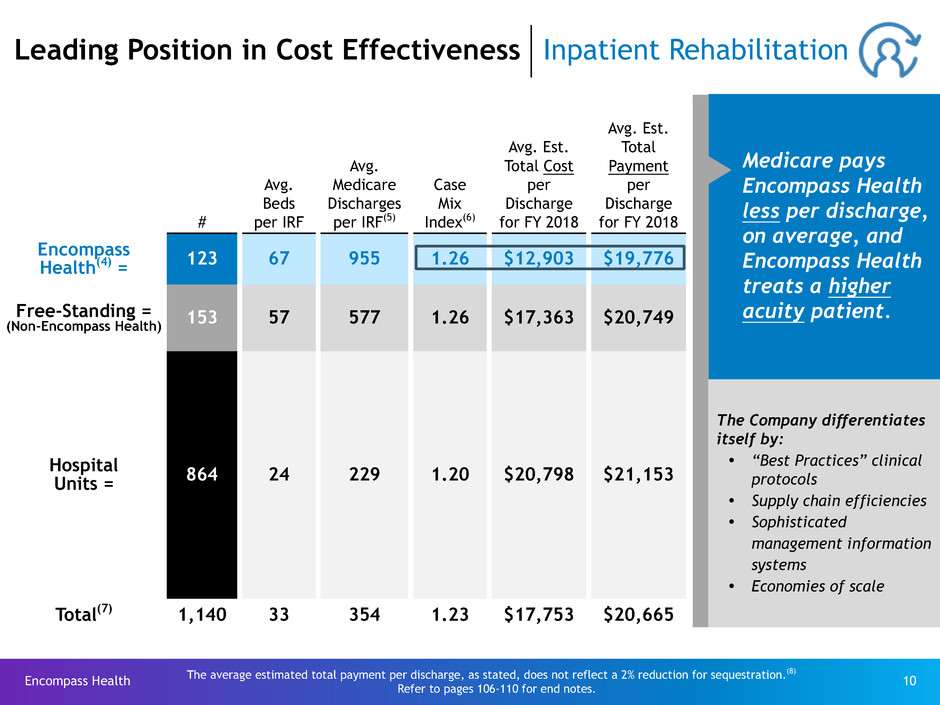
Leading Position in Cost Effectiveness Inpatient Rehabilitation
Medicare pays
Encompass Health
less per discharge,
on average, and
Encompass Health
treats a higher
acuity patient.
#
Avg.
Beds
per IRF
Avg.
Medicare
Discharges
per IRF(5)
Case
Mix
Index(6)
Avg. Est.
Total Cost
per
Discharge
for FY 2018
Avg. Est.
Total
Payment
per
Discharge
for FY 2018
Encompass
Health(4) = 123 67 955 1.26 $12,903 $19,776
Free-Standing =
(Non-Encompass Health) 153 57 577 1.26 $17,363 $20,749
Hospital
Units = 864 24 229 1.20 $20,798 $21,153
Total(7) 1,140 33 354 1.23 $17,753 $20,665
The average estimated total payment per discharge, as stated, does not reflect a 2% reduction for sequestration.(8)
Refer to pages 106-110 for end notes.
The Company differentiates
itself by:
Ÿ “Best Practices” clinical
protocols
Ÿ Supply chain efficiencies
Ÿ Sophisticated
management information
systems
Ÿ Economies of scale
Encompass Health 11
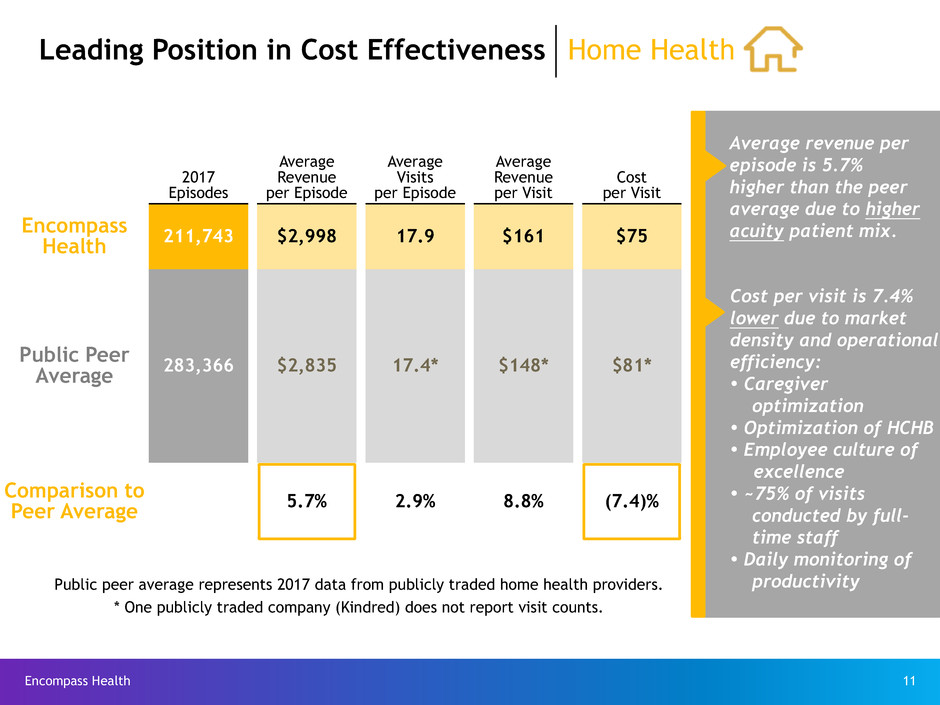
2017
Episodes
Average
Revenue
per Episode
Average
Visits
per Episode
Average
Revenue
per Visit
Cost
per Visit
Encompass
Health 211,743 $2,998 17.9 $161 $75
Public Peer
Average 283,366 $2,835 17.4* $148* $81*
Comparison to
Peer Average 5.7% 2.9% 8.8% (7.4)%
Public peer average represents 2017 data from publicly traded home health providers.
* One publicly traded company (Kindred) does not report visit counts.
Average revenue per
episode is 5.7%
higher than the peer
average due to higher
acuity patient mix.
Cost per visit is 7.4%
lower due to market
density and operational
efficiency:
Ÿ Caregiver
optimization
Ÿ Optimization of HCHB
Ÿ Employee culture of
excellence
Ÿ ~75% of visits
conducted by full-
time staff
Ÿ Daily monitoring of
productivity
Leading Position in Cost Effectiveness Home Health
Encompass Health 12* Includes consolidated inpatient rehabilitation hospitals classified as same store during each period ** Data provided by UDSMRRefer to pages 106-110 for end notes.
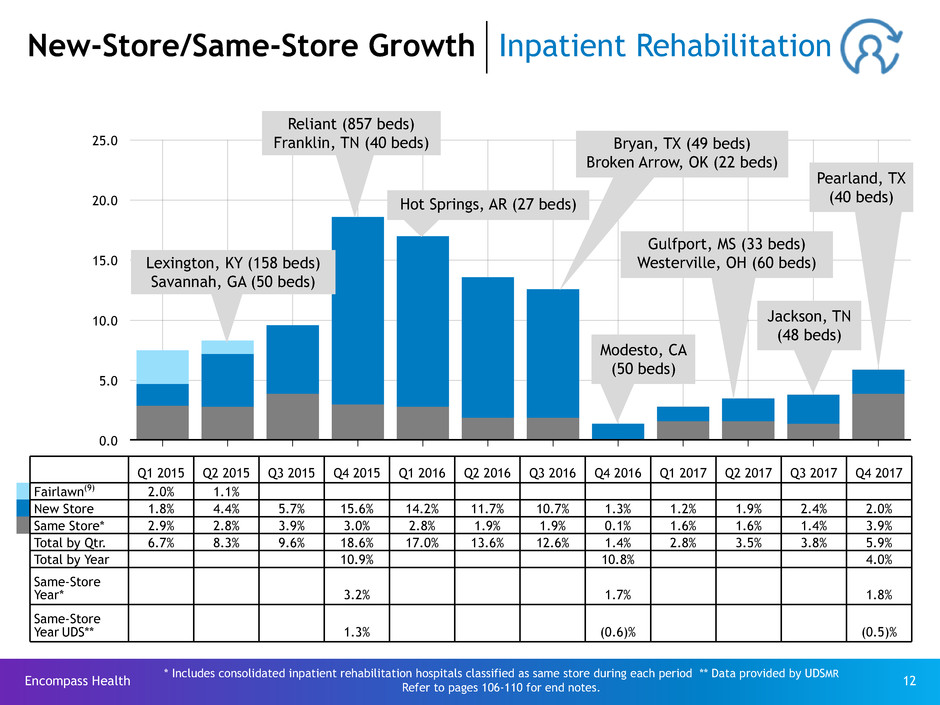
New-Store/Same-Store Growth Inpatient Rehabilitation
25.0
20.0
15.0
10.0
5.0
0.0
Q1 2015 Q2 2015 Q3 2015 Q4 2015 Q1 2016 Q2 2016 Q3 2016 Q4 2016 Q1 2017 Q2 2017 Q3 2017 Q4 2017Q1 2015 Q2 2015 Q3 2015 Q4 2015 Q1 2016 Q2 2016 Q3 2016 Q4 2016 Q1 2017 Q2 2017 Q3 2017 Q4 2017
Fairlawn(9) 2.0% 1.1%
New Store 1.8% 4.4% 5.7% 15.6% 14.2% 11.7% 10.7% 1.3% 1.2% 1.9% 2.4% 2.0%
Same Store* 2.9% 2.8% 3.9% 3.0% 2.8% 1.9% 1.9% 0.1% 1.6% 1.6% 1.4% 3.9%
Total by Qtr. 6.7% 8.3% 9.6% 18.6% 17.0% 13.6% 12.6% 1.4% 2.8% 3.5% 3.8% 5.9%
Total by Year 10.9% 10.8% 4.0%
Same-Store
Year* 3.2% 1.7% 1.8%
Same-Store
Year UDS** 1.3% (0.6)% (0.5)%
Reliant (857 beds)
Franklin, TN (40 beds)
Lexington, KY (158 beds)
Savannah, GA (50 beds)
Pearland, TX
(40 beds)
Modesto, CA
(50 beds)
Gulfport, MS (33 beds)
Westerville, OH (60 beds)
Bryan, TX (49 beds)
Broken Arrow, OK (22 beds)
Hot Springs, AR (27 beds)
Jackson, TN
(48 beds)
Encompass Health 13* Includes consolidated home health agencies classified as same store during each period
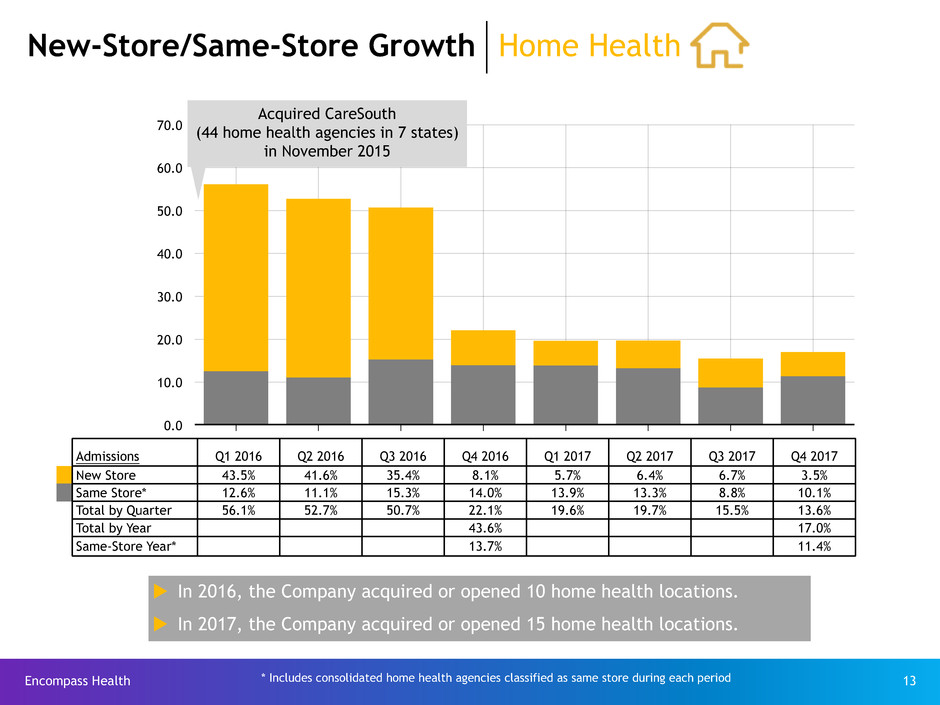
New-Store/Same-Store Growth Home Health
70.0
60.0
50.0
40.0
30.0
20.0
10.0
0.0
Q1 2016 Q2 2016 Q3 2016 Q4 2016 Q1 2017 Q2 2017 Q3 2017 Q4 2017Admissions Q1 2016 Q2 2016 Q3 2016 Q4 2016 Q1 2017 Q2 2017 Q3 2017 Q4 2017
New Store 43.5% 41.6% 35.4% 8.1% 5.7% 6.4% 6.7% 3.5%
Same Store* 12.6% 11.1% 15.3% 14.0% 13.9% 13.3% 8.8% 10.1%
Total by Quarter 56.1% 52.7% 50.7% 22.1% 19.6% 19.7% 15.5% 13.6%
Total by Year 43.6% 17.0%
Same-Store Year* 13.7% 11.4%
Acquired CareSouth
(44 home health agencies in 7 states)
in November 2015
u In 2016, the Company acquired or opened 10 home health locations.
u In 2017, the Company acquired or opened 15 home health locations.
Encompass Health 14
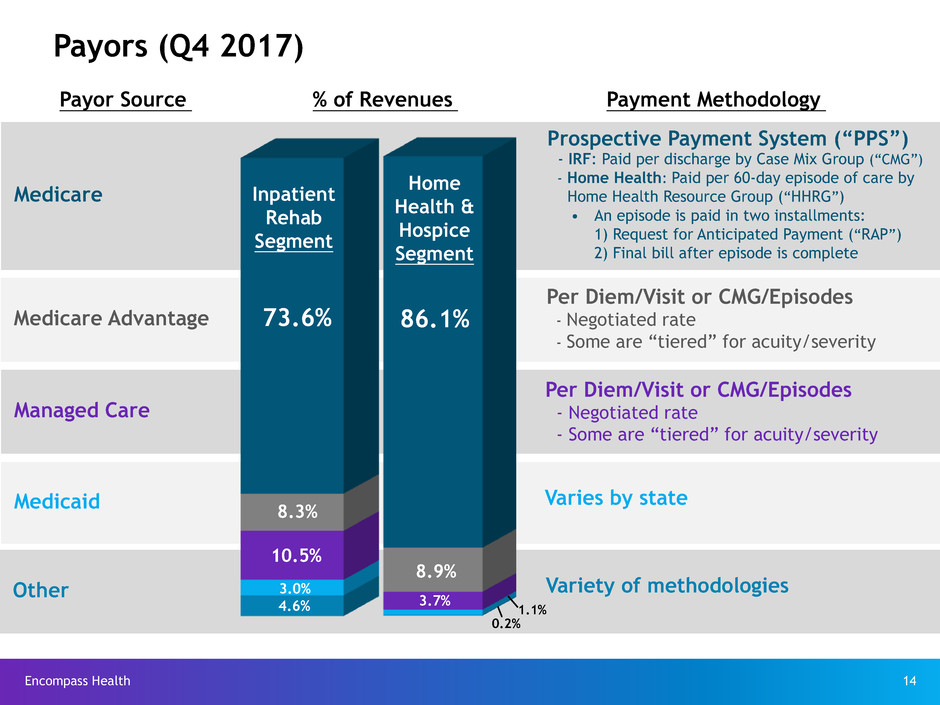
Medicaid
Medicare Advantage
Managed Care
Medicare
Other
Per Diem/Visit or CMG/Episodes
- Negotiated rate
- Some are “tiered” for acuity/severity
Per Diem/Visit or CMG/Episodes
- Negotiated rate
- Some are “tiered” for acuity/severity
Prospective Payment System (“PPS”)
- IRF: Paid per discharge by Case Mix Group (“CMG”)
- Home Health: Paid per 60-day episode of care by
Home Health Resource Group (“HHRG”)
• An episode is paid in two installments:
1) Request for Anticipated Payment (“RAP”)
2) Final bill after episode is complete
Varies by state
Payors (Q4 2017)
Payor Source Payment Methodology% of Revenues
86.1%73.6%
8.9%
8.3%
3.7%
10.5%
3.0%
1.1%4.6%
0.2%
Inpatient
Rehab
Segment
Home
Health &
Hospice
Segment
Variety of methodologies

Encompass Health 15
Independent Research Concludes IRFs are a Better
Rehabilitation Option for Stroke Patients than SNFs
“If the hospital suggests sending your loved one to
a skilled nursing facility after a stroke, advocate
for the patient to go to an inpatient
rehabilitation facility instead…”*
“Whenever possible, the American Stroke Association
strongly recommends that stroke patients be treated
at an inpatient rehabilitation facility rather than a
skilled nursing facility. While in
an inpatient rehabilitation facility, a patient participates in at
least three hours of rehabilitation a day from physical therapists,
occupational therapists, and speech therapists. Nurses are
continuously available and doctors typically visit daily.”*
*
**
AHA/ASA press release, “Inpatient rehab recommended over nursing homes for stroke rehab,”
issued May 4, 2016 (newsroom.heart.org)
“Guidelines for Adult Stroke Rehabilitation and Recovery,” issued May 2016 (stroke.ahajournals.org)
“The studies that have compared outcomes in hospitalized stroke
patients first discharged to an IRF, a SNF, or a nursing home have
generally shown that IRF patients have higher rates of return
to community living and greater functional recovery,
whereas patients discharged to a SNF or a nursing home have higher
rehospitalization rates and substantially poorer survival.”**
103 of the Company’s IRFs hold The Joint
Commission’s Disease-Specific Care
Certification in Stroke Rehabilitation.
Encompass Health 16
• Largest provider of inpatient rehabilitation services
• 4th largest provider of Medicare-certified skilled home health services
• Consistent delivery of high-quality, cost-effective, integrated facility-
based and home-based care
• Enhanced utilization of technology (e.g., clinical, data management,
and technology-enabled business processes)
Strong and Sustainable Business Fundamentals
• Effective labor management
• Efficient supply chain
• Economies related to scale and market density
• Strong balance sheet and liquidity, no significant near-term maturities
(credit agreement matures in 2022; bonds mature in 2023 and beyond)
• Substantial free cash flow generation
• Attractive organic growth opportunities in both segments
• Flexible inpatient rehabilitation de novo and acquisition strategy
• Home health and hospice platform with track record of growth through
acquisitions
• Portfolio of 127* IRFs as of December 31, 2017
P 88 owned and 39 leased
• Favorable demographic trends driving increased demand
• Nondiscretionary nature of many conditions treated
• Highly fragmented post-acute sectors present acquisition and joint
venture opportunities
* Includes one nonconsolidated entity.
Real Estate Ownership
Attractive Healthcare Sectors
Growth Opportunities
Cost-Effectiveness
Financial Strength
Industry Leading Positions

Encompass Health 17
Investment Thesis
and Strategy
Encompass Health’s ability to adapt to changes, build strategic
relationships, and consistently provide high-quality, cost-effective care
positions the Company for success in the evolving healthcare industry.
Encompass Health 18
Investment Thesis
Encompass Health is positioned to become the nation's leading provider of integrated post-acute services.
The healthcare industry is evolving toward integrated delivery models and value-based care.
Providers must be able to adapt to changes, build strategic relationships across the healthcare
continuum, and consistently provide high-quality, cost-effective care to be successful.
Change Agility Demonstrated ability to adapt across economic cycles and in the face of numerousand significant regulatory and legislative changes
Strategic
Relationships
Joint ventures with acute-care partners comprise one-third of IRF portfolio.
Formed Post-Acute Innovation Center in collaboration with Cerner Corporation to
develop enhanced tools to manage patients across the continuum of care
Partnered with the American Heart Association/American Stroke Association to
jointly work to elevate national and local awareness that stroke is treatable and
beatable through rehabilitation and community support
Quality of
Patient Outcomes Outcomes in both operating segments exceed national industry standards.
Cost
Effectiveness
Treatment of more medically complex patients at lower average costs than other
post-acute providers through superior clinical protocols, economies of scale, and
technology-enabled business processes
Growth Both of the Company's segments benefit from favorable demographic trends and thenondiscretionary nature of many conditions treated.
Encompass Health 19
Elements of Strategy
Strategy
The Company’s strategy is to expand its network of inpatient rehabilitation
hospitals and home health and hospice agencies, further strengthen its relationships
with healthcare systems, provider networks, and payors in order to connect patient
care across the healthcare continuum, and to deliver superior outcomes.
Clinical Expertise
and High-Quality
Outcomes
Financial
Resources
Advanced
Technology
Sustained
Growth
Post-Acute
Innovation
Encompass Health 20
Elements of Strategy
Clinical
Expertise
and
High-Quality
Outcomes
Institutional programs and advanced treatment protocols connect care and allow
seamless transition of patients across the healthcare continuum
Leverage technology to strengthen clinical data analytics
Integration of care transition coordinators
105 Encompass Health inpatient rehabilitation hospitals hold one or more disease-
specific certifications, including 103 with stroke-specific certifications
Outcomes in both operating segments exceed national industry standards (see page 9)
Financial
Resources
Strong, well-capitalized balance sheet
Free cash flow funds growth and shareholder distributions
Advanced
Technology
Proprietary rehabilitation-specific clinical information system (known as "ACE-IT")
Proprietary management reporting system (known as "Beacon")
Optimization of Homecare Homebase
Sustained
Growth
Highly fragmented sectors present acquisition and joint venture growth opportunities
Technology-facilitated and data-driven sales processes
Barriers to entry include capital investments, clinical expertise, regulatory compliance,
and Certificate of Need (“CON”) requirements
Post-Acute
Innovation
Predictive analytics used to enhance patient outcomes (e.g., ReACT; Sepsis Alert)
Ongoing innovation with initiatives such as the Post-Acute Innovation Center
Active participant in various alternative payment models

Encompass Health 21
Home-Based Post-Acute Services
• More care in the home (lowest cost setting)
• Ability to care for high-acuity patients with
multiple chronic conditions
Future Post-Acute Providers
Inpatient Rehabilitation Hospitals
• Full range: low acuity à high acuity
• 24/7 nursing coverage
• Eliminates payment silos
• Integrated Delivery
Payment Models
• Value-Based
Payments
• Site Neutrality
Current Post-Acute Providers
Facility-Based Post Acute Services
Skilled Nursing Facilities
Home Health
Long-Term Acute Care Hospitals
• Medicare payments/regulations are site
specific (e.g., 60% Rule, 3-Hour Rule,
“preponderance” of one-to-one therapy).
▪ The Company believes the healthcare industry is moving toward integrated delivery
payment models, value-based purchasing, and site neutrality.
▪ To succeed, providers must be able to adapt to changes in the regulatory and
operating environments, build strategic relationships across the healthcare continuum,
and consistently provide high-quality care at a cost-effective price.
The Healthcare Landscape is Changing.
• Medicare payments/regulations will be
outcome focused.
• Many existing regulations will become
unnecessary.
Encompass Health 22
Always Available
Sometimes Available
Seldom Available
Therapy
Gym &
Training
Systems for
All PAC
Patients
Staff Trained
for All Acuity
Therapy
Gym &
Training
Systems for
All PAC
Patients
Staff Trained
for All Acuity
Therapy
Gym &
Training
Systems for
All PAC
Patients
Staff Trained
for All Acuity
LTACs IRFs SNFs
Home Health
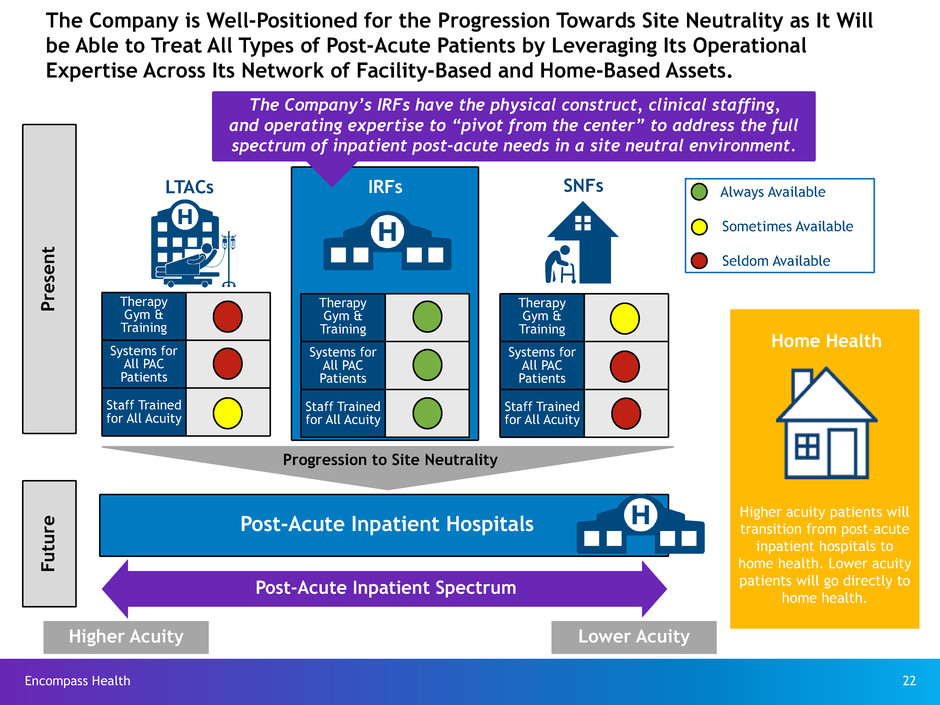
The Company is Well-Positioned for the Progression Towards Site Neutrality as It Will
be Able to Treat All Types of Post-Acute Patients by Leveraging Its Operational
Expertise Across Its Network of Facility-Based and Home-Based Assets.
Higher acuity patients will
transition from post-acute
inpatient hospitals to
home health. Lower acuity
patients will go directly to
home health.Post-Acute Inpatient Spectrum
Higher Acuity Lower Acuity
Progression to Site Neutrality
Post-Acute Inpatient Hospitals
Presen
t
Futur
e
The Company’s IRFs have the physical construct, clinical staffing,
and operating expertise to “pivot from the center” to address the full
spectrum of inpatient post-acute needs in a site neutral environment.
Encompass Health 23
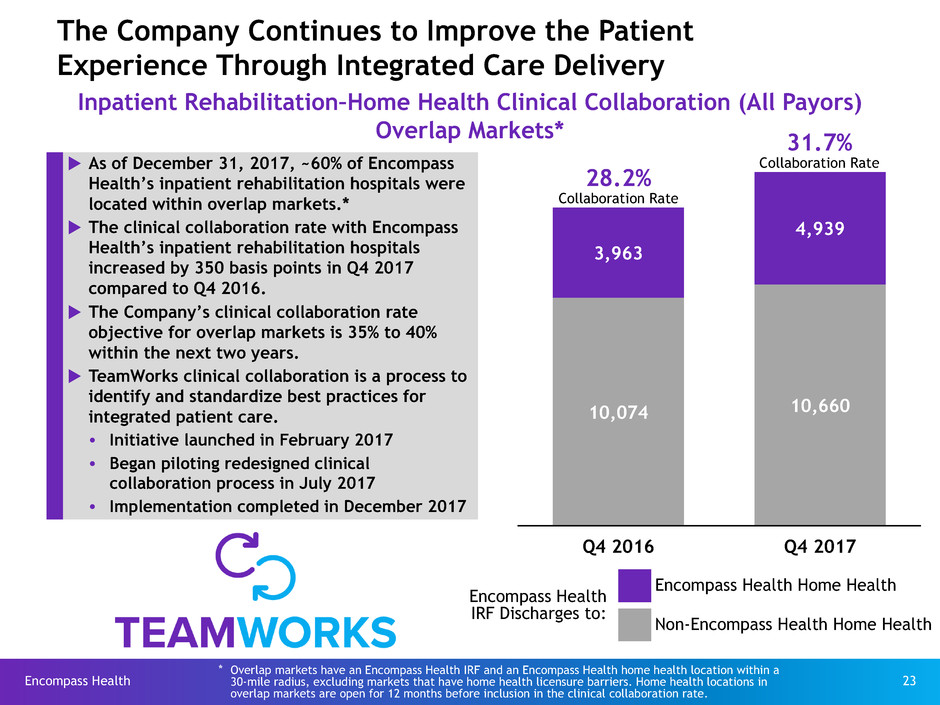
The Company Continues to Improve the Patient
Experience Through Integrated Care Delivery
Inpatient Rehabilitation–Home Health Clinical Collaboration (All Payors)
Overlap Markets*
Q4 2016 Q4 2017
10,074 10,660
3,963
4,939
28.2%
Collaboration Rate
31.7%
Collaboration Rateu As of December 31, 2017, ~60% of Encompass
Health’s inpatient rehabilitation hospitals were
located within overlap markets.*
u The clinical collaboration rate with Encompass
Health’s inpatient rehabilitation hospitals
increased by 350 basis points in Q4 2017
compared to Q4 2016.
u The Company’s clinical collaboration rate
objective for overlap markets is 35% to 40%
within the next two years.
u TeamWorks clinical collaboration is a process to
identify and standardize best practices for
integrated patient care.
Ÿ Initiative launched in February 2017
Ÿ Began piloting redesigned clinical
collaboration process in July 2017
Ÿ Implementation completed in December 2017
Encompass Health
IRF Discharges to:
Encompass Health Home Health
Non-Encompass Health Home Health
* Overlap markets have an Encompass Health IRF and an Encompass Health home health location within a
30-mile radius, excluding markets that have home health licensure barriers. Home health locations in
overlap markets are open for 12 months before inclusion in the clinical collaboration rate.

Encompass Health 24
Solution:
Utilize extensive proprietary
database of IRF patients to
engage in predictive modeling to
identify patients at risk for acute
care transfer and implement
intervention strategies as part
of the plan of care.
Solution:
Standardize and improve
infection control practices
across the company in order to
reduce the risk of infection to
patients and apply evidenced-
based decision making in the
Company’s IRFs.
Solution:
Develop clinical protocols and
coordinated discharge planning between
IRFs and home health agencies; implement
TeamWorks initiative to standardize best
practices across all overlap markets; and
integrate Care Transition Coordinators to
implement patient-centered transition
plans that promote quality, safety and
patient choice.
Problem:
Acute care transfers can
negatively influence patient
outcomes and result in
unnecessary healthcare
expenditures and penalties.
Problem:
Infections are a threat
to patient safety and add to
growing healthcare costs.
Problem:
Poor coordination of the discharge
process between healthcare
providers can result in challenges with
the transition of care, unnecessary
duplication of services, and avoidable
medical errors.
Clinical Initiatives to Further Improve Quality
Reduce Acute Care Transfers
(tracked in the IRF QRP*) Infection Control Clinical Collaboration
* IRF Quality Reporting Program

Encompass Health 25
Business Outlook, Including Guidance
(as of March 13, 2018)

Encompass Health 26
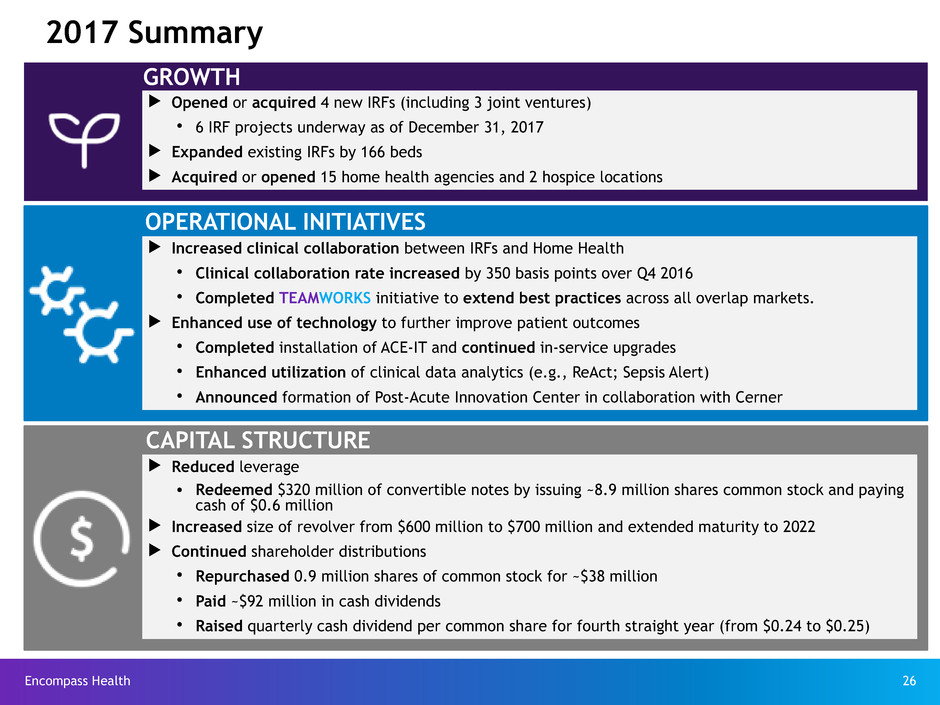
2017 Summary
GROWTH
CAPITAL STRUCTURE
OPERATIONAL INITIATIVES
u Opened or acquired 4 new IRFs (including 3 joint ventures)
Ÿ 6 IRF projects underway as of December 31, 2017
u Expanded existing IRFs by 166 beds
u Acquired or opened 15 home health agencies and 2 hospice locations
u Increased clinical collaboration between IRFs and Home Health
Ÿ Clinical collaboration rate increased by 350 basis points over Q4 2016
Ÿ Completed TEAMWORKS initiative to extend best practices across all overlap markets.
u Enhanced use of technology to further improve patient outcomes
Ÿ Completed installation of ACE-IT and continued in-service upgrades
Ÿ Enhanced utilization of clinical data analytics (e.g., ReAct; Sepsis Alert)
Ÿ Announced formation of Post-Acute Innovation Center in collaboration with Cerner
u Reduced leverage
Ÿ Redeemed $320 million of convertible notes by issuing ~8.9 million shares common stock and paying
cash of $0.6 million
u Increased size of revolver from $600 million to $700 million and extended maturity to 2022
u Continued shareholder distributions
Ÿ Repurchased 0.9 million shares of common stock for ~$38 million
Ÿ Paid ~$92 million in cash dividends
Ÿ Raised quarterly cash dividend per common share for fourth straight year (from $0.24 to $0.25)
Encompass Health 27
GROWTH
OPERATIONAL INITIATIVES
CAPITAL STRUCTURE
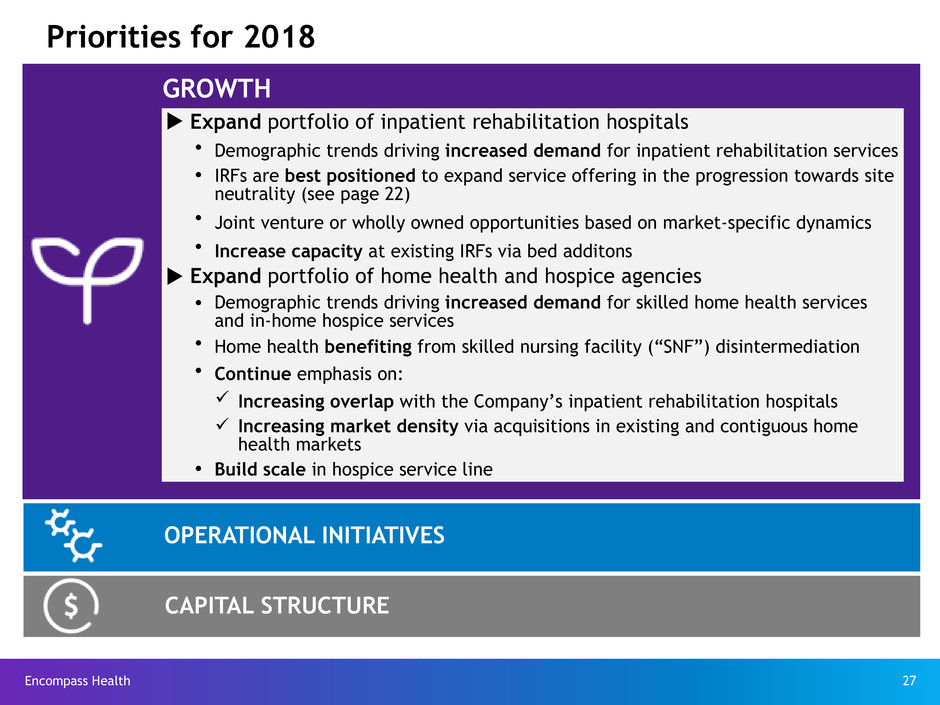
Priorities for 2018
u Expand portfolio of inpatient rehabilitation hospitals
Ÿ Demographic trends driving increased demand for inpatient rehabilitation services
Ÿ IRFs are best positioned to expand service offering in the progression towards site
neutrality (see page 22)
Ÿ Joint venture or wholly owned opportunities based on market-specific dynamics
Ÿ Increase capacity at existing IRFs via bed additons
u Expand portfolio of home health and hospice agencies
Ÿ Demographic trends driving increased demand for skilled home health services
and in-home hospice services
Ÿ Home health benefiting from skilled nursing facility (“SNF”) disintermediation
Ÿ Continue emphasis on:
ü Increasing overlap with the Company’s inpatient rehabilitation hospitals
ü Increasing market density via acquisitions in existing and contiguous home
health markets
Ÿ Build scale in hospice service line
Encompass Health 28
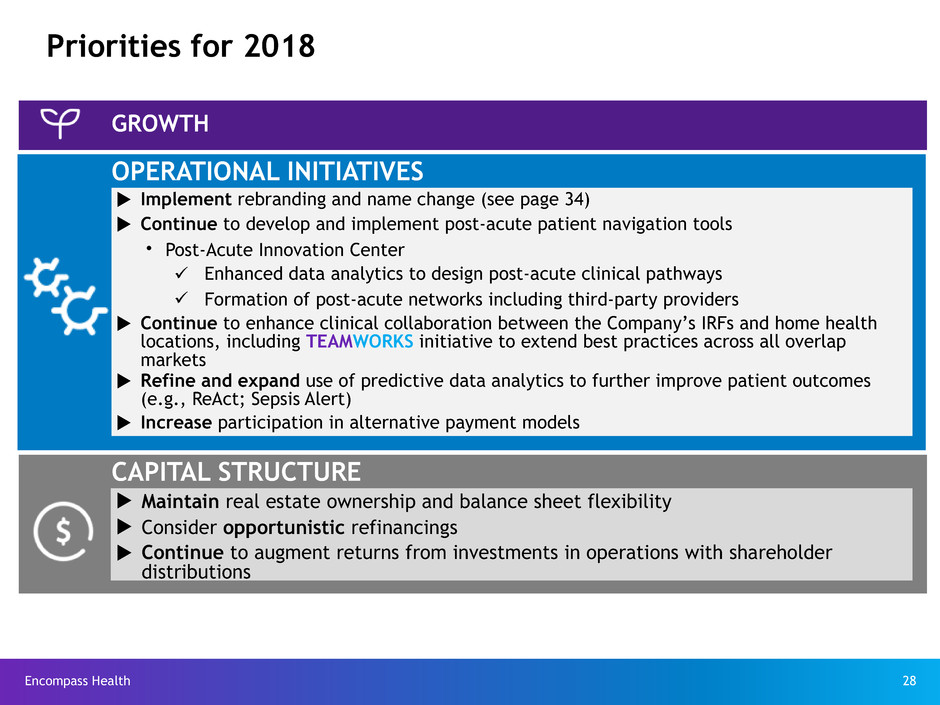
CAPITAL STRUCTURE
OPERATIONAL INITIATIVES
u Implement rebranding and name change (see page 34)
u Continue to develop and implement post-acute patient navigation tools
• Post-Acute Innovation Center
ü Enhanced data analytics to design post-acute clinical pathways
ü Formation of post-acute networks including third-party providers
u Continue to enhance clinical collaboration between the Company’s IRFs and home health
locations, including TEAMWORKS initiative to extend best practices across all overlap
markets
u Refine and expand use of predictive data analytics to further improve patient outcomes
(e.g., ReAct; Sepsis Alert)
u Increase participation in alternative payment models
Priorities for 2018
GROWTH
u Maintain real estate ownership and balance sheet flexibility
u Consider opportunistic refinancings
u Continue to augment returns from investments in operations with shareholder
distributions

Encompass Health 29Refer to pages 106-110 for end notes.
Guidance - as of March 13, 2018
Adjusted EBITDA(10)
Adjusted Earnings per Share
from Continuing Operations
Attributable to Encompass
Health(11)
Net Operating Revenues*
2018 Guidance
Net Operating Revenues*
Adjusted EBITDA(10)
$830 million to $850 million
Adjusted Earnings per Share
from Continuing Operations
Attributable to Encompass
Health(11)
$3.25 to $3.40
$3,919.0 million
$823.1 million
$2.76
$4,080 million to $4,190 million
2017 Actuals
* In the first quarter of 2018, the Company will adopt a new revenue recognition accounting standard. Under the new standard,
amounts the Company previously presented as provision for doubtful accounts become a component of consolidated net operating
revenues. See "Estimated Impact of the New Revenue Recognition Accounting Standard" on page 30 for more details.
Encompass Health 30
Expected Impact of the New Revenue Standard - Historical Periods
As Reported Recast
Q4-17 Q3-17 Q2-17 Q1-17 FY 2017 FY 2016 Q4-17 Q3-17 Q2-17 Q1-17 FY 2017 FY 2016
Net operating revenue
(millions) $1,019.7 $ 995.6 $ 981.3 $ 974.8 $3,971.4 $3,707.2 $1,010.0 $ 983.0 $ 967.6 $ 958.4 $3,919.0 $3,646.0
Provision for doubtful
accounts (millions) 9.7 12.6 13.7 16.4 52.4 61.2 — — — — — —
Inpatient rehabilitation
revenue/discharge 17,871 17,896 17,823 18,131 17,929 17,577 17,693 17,654 17,557 17,812 17,679 17,265
Home health revenue/
episode 2,989 3,022 2,989 2,991 2,998 3,031 2,976 3,008 2,975 2,978 2,984 3,017
Adjusted EBITDA (millions) 208.2 204.6 209.5 200.8 823.1 793.6 No Change
Adjusted EPS 0.70 0.66 0.71 0.70 2.76 2.67 No Change
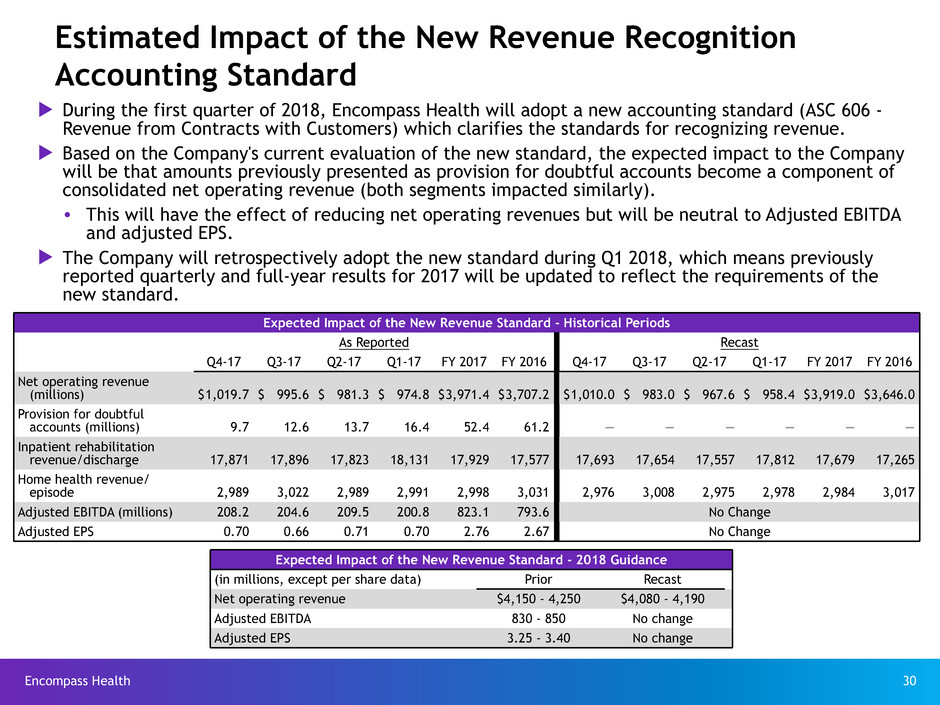
Estimated Impact of the New Revenue Recognition
Accounting Standard
Expected Impact of the New Revenue Standard - 2018 Guidance
(in millions, except per share data) Prior Recast
Net operating revenue $4,150 - 4,250 $4,080 - 4,190
Adjusted EBITDA 830 - 850 No change
Adjusted EPS 3.25 - 3.40 No change
u During the first quarter of 2018, Encompass Health will adopt a new accounting standard (ASC 606 -
Revenue from Contracts with Customers) which clarifies the standards for recognizing revenue.
u Based on the Company's current evaluation of the new standard, the expected impact to the Company
will be that amounts previously presented as provision for doubtful accounts become a component of
consolidated net operating revenue (both segments impacted similarly).
• This will have the effect of reducing net operating revenues but will be neutral to Adjusted EBITDA
and adjusted EPS.
u The Company will retrospectively adopt the new standard during Q1 2018, which means previously
reported quarterly and full-year results for 2017 will be updated to reflect the requirements of the
new standard.

Encompass Health 31
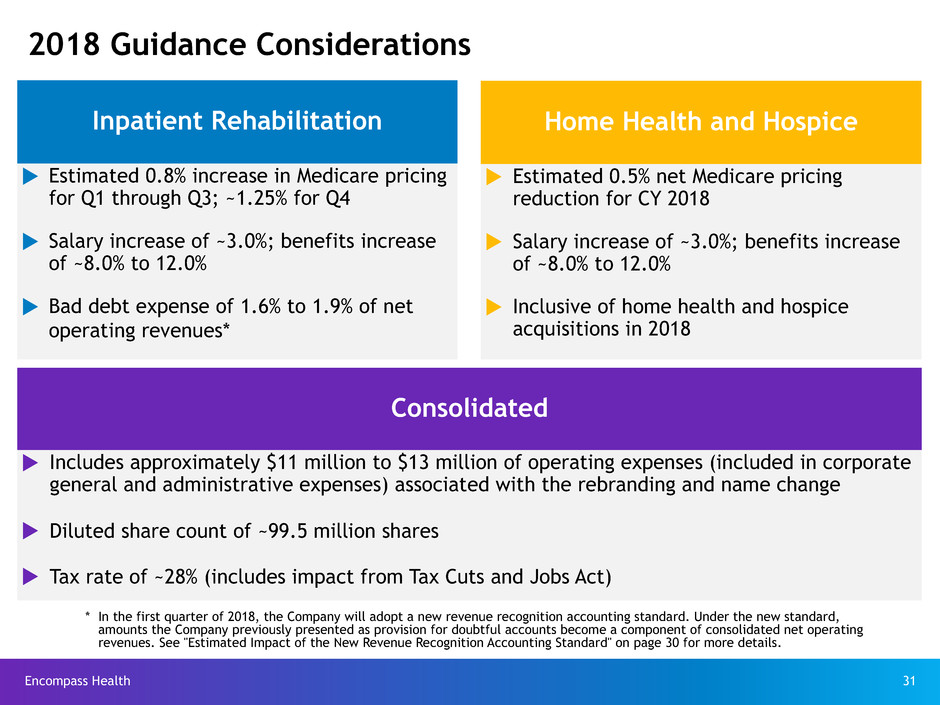
2018 Guidance Considerations
Inpatient Rehabilitation
u Estimated 0.8% increase in Medicare pricing
for Q1 through Q3; ~1.25% for Q4
u Salary increase of ~3.0%; benefits increase
of ~8.0% to 12.0%
u Bad debt expense of 1.6% to 1.9% of net
operating revenues*
Home Health and Hospice
u Estimated 0.5% net Medicare pricing
reduction for CY 2018
u Salary increase of ~3.0%; benefits increase
of ~8.0% to 12.0%
u Inclusive of home health and hospice
acquisitions in 2018
Consolidated
u Includes approximately $11 million to $13 million of operating expenses (included in corporate
general and administrative expenses) associated with the rebranding and name change
u Diluted share count of ~99.5 million shares
u Tax rate of ~28% (includes impact from Tax Cuts and Jobs Act)
* In the first quarter of 2018, the Company will adopt a new revenue recognition accounting standard. Under the new standard,
amounts the Company previously presented as provision for doubtful accounts become a component of consolidated net operating
revenues. See "Estimated Impact of the New Revenue Recognition Accounting Standard" on page 30 for more details.

Encompass Health 32Reconciliations to GAAP provided on pages 93-104. Refer to pages 106-110 for end notes.
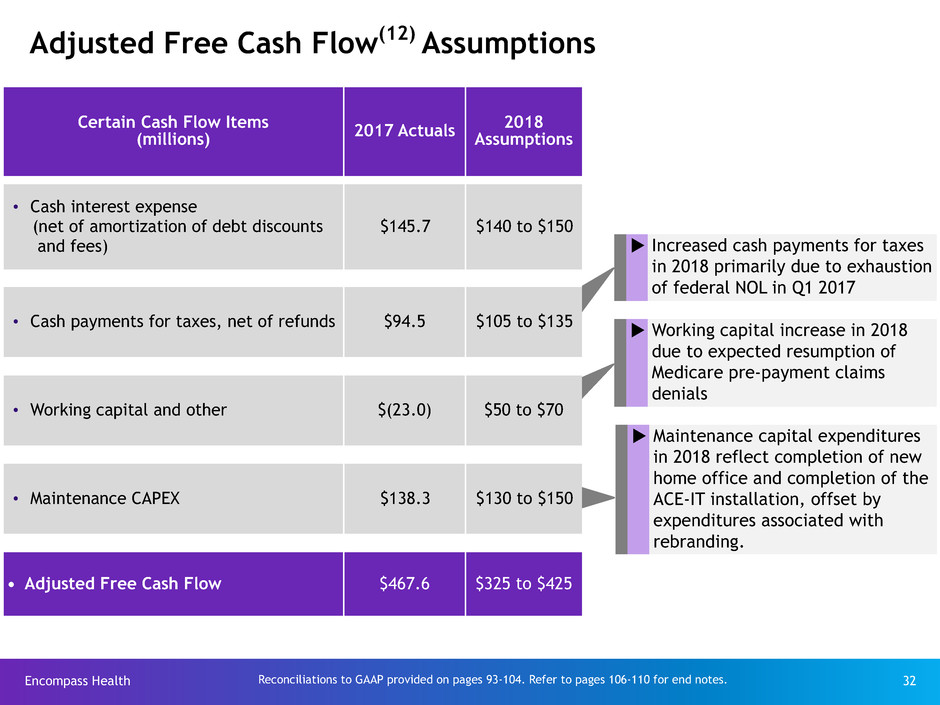
u Increased cash payments for taxes
in 2018 primarily due to exhaustion
of federal NOL in Q1 2017
Adjusted Free Cash Flow(12) Assumptions
Certain Cash Flow Items
(millions) 2017 Actuals
2018
Assumptions
• Cash interest expense
(net of amortization of debt discounts
and fees)
$145.7 $140 to $150
• Cash payments for taxes, net of refunds $94.5 $105 to $135
• Working capital and other $(23.0) $50 to $70
• Maintenance CAPEX $138.3 $130 to $150
• Adjusted Free Cash Flow $467.6 $325 to $425
u Maintenance capital expenditures
in 2018 reflect completion of new
home office and completion of the
ACE-IT installation, offset by
expenditures associated with
rebranding.
u Working capital increase in 2018
due to expected resumption of
Medicare pre-payment claims
denials
Encompass Health 33See the debt schedule on page 62. Refer to pages 106-110 for end notes.
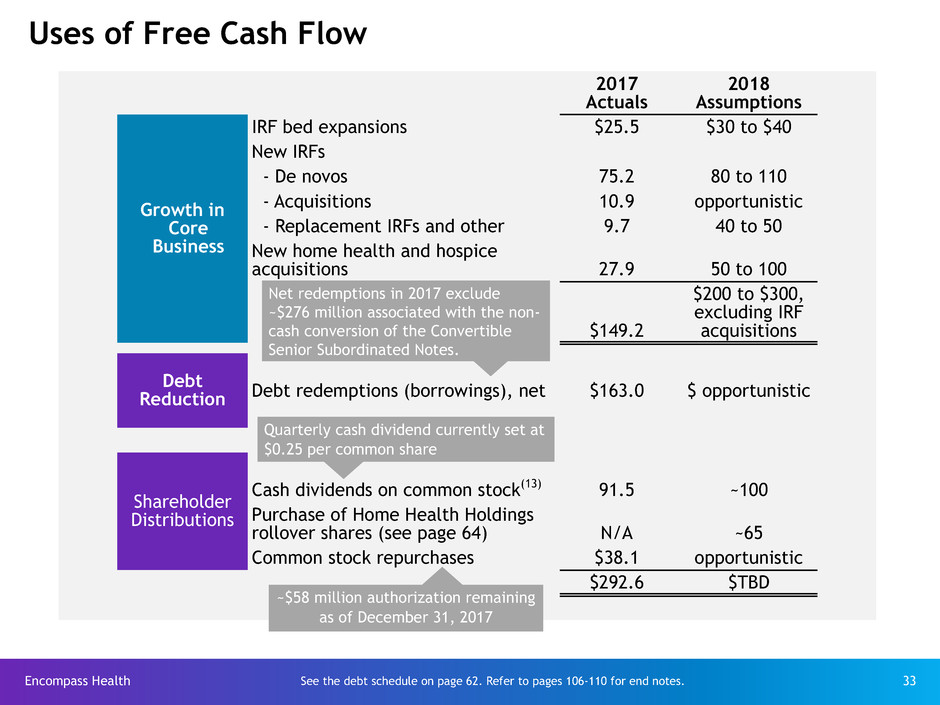
Uses of Free Cash Flow
2017
Actuals
2018
Assumptions
Growth in
Core
Business
IRF bed expansions $25.5 $30 to $40
New IRFs
- De novos 75.2 80 to 110
- Acquisitions 10.9 opportunistic
- Replacement IRFs and other 9.7 40 to 50
New home health and hospice
acquisitions 27.9 50 to 100
$149.2
$200 to $300,
excluding IRF
acquisitions
Debt
Reduction Debt redemptions (borrowings), net $163.0 $ opportunistic
Shareholder
Distributions
Cash dividends on common stock(13) 91.5 ~100
Purchase of Home Health Holdings
rollover shares (see page 64) N/A ~65
Common stock repurchases $38.1 opportunistic
$292.6 $TBD
Quarterly cash dividend currently set at
$0.25 per common share
~$58 million authorization remaining
as of December 31, 2017
Net redemptions in 2017 exclude
~$276 million associated with the non-
cash conversion of the Convertible
Senior Subordinated Notes.

Encompass Health 34
Rebranding and Name Change
u The Company’s rebranding and name change reinforce its existing strategy and position as an
integrated provider of inpatient and home-based care.
Ÿ Effective January 1, 2018, HealthSouth Corporation changed its name to Encompass Health
Corporation, with a corresponding ticker symbol change from “HLS” to “EHC.”
Ÿ Both business segments — inpatient rehabilitation and home health and hospice — will fully transition
to the Encompass Health branding by the end of the first quarter of 2019.
Ÿ Total rebranding investment estimated to be ~$25 million to $30 million, to be incurred between 2017
and 2019
2017 2018 2019 Total
Operating expenses* ~$6 million ~$11 to $13 million ~$1 to $2 million ~$18 to $21 million
Capital expenditures ~$1 million ~$5 to $6 million ~$1 to $2 million ~$7 to $9 million
Total rebranding investment ~$7 million ~$16 to $19 million ~$2 to $4 million ~$25 to $30 million
* Included in corporate general and administrative expenses line item
Encompass Health 35
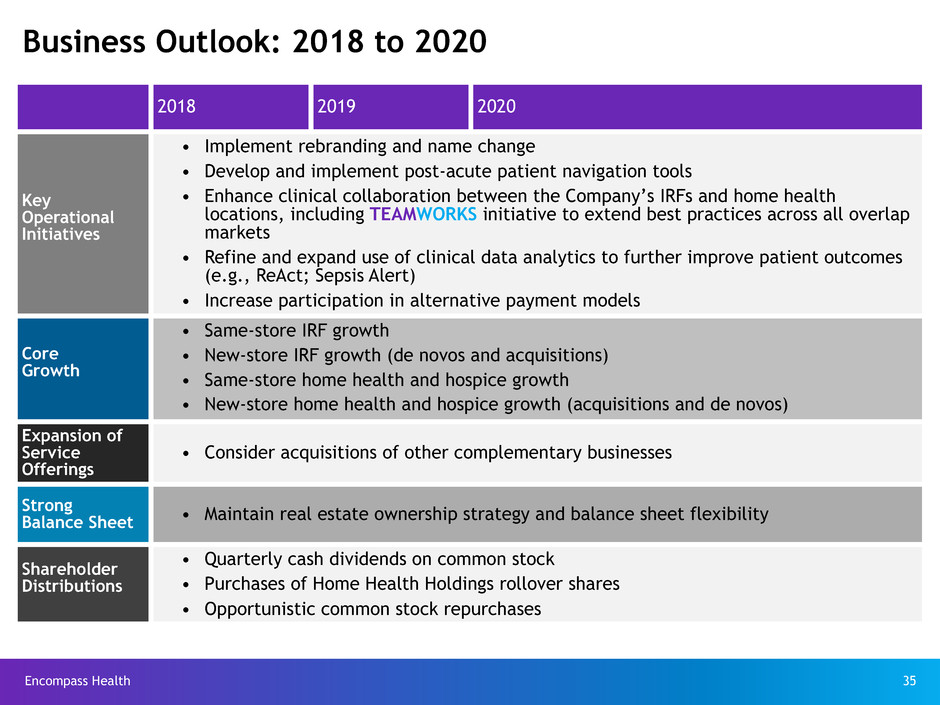
Business Outlook: 2018 to 2020
2018 2019 2020
Key
Operational
Initiatives
• Implement rebranding and name change
• Develop and implement post-acute patient navigation tools
• Enhance clinical collaboration between the Company’s IRFs and home health
locations, including TEAMWORKS initiative to extend best practices across all overlap
markets
• Refine and expand use of clinical data analytics to further improve patient outcomes
(e.g., ReAct; Sepsis Alert)
• Increase participation in alternative payment models
Core
Growth
• Same-store IRF growth
• New-store IRF growth (de novos and acquisitions)
• Same-store home health and hospice growth
• New-store home health and hospice growth (acquisitions and de novos)
Expansion of
Service
Offerings
• Consider acquisitions of other complementary businesses
Strong
Balance Sheet • Maintain real estate ownership strategy and balance sheet flexibility
Shareholder
Distributions
• Quarterly cash dividends on common stock
• Purchases of Home Health Holdings rollover shares
• Opportunistic common stock repurchases
Encompass Health 36
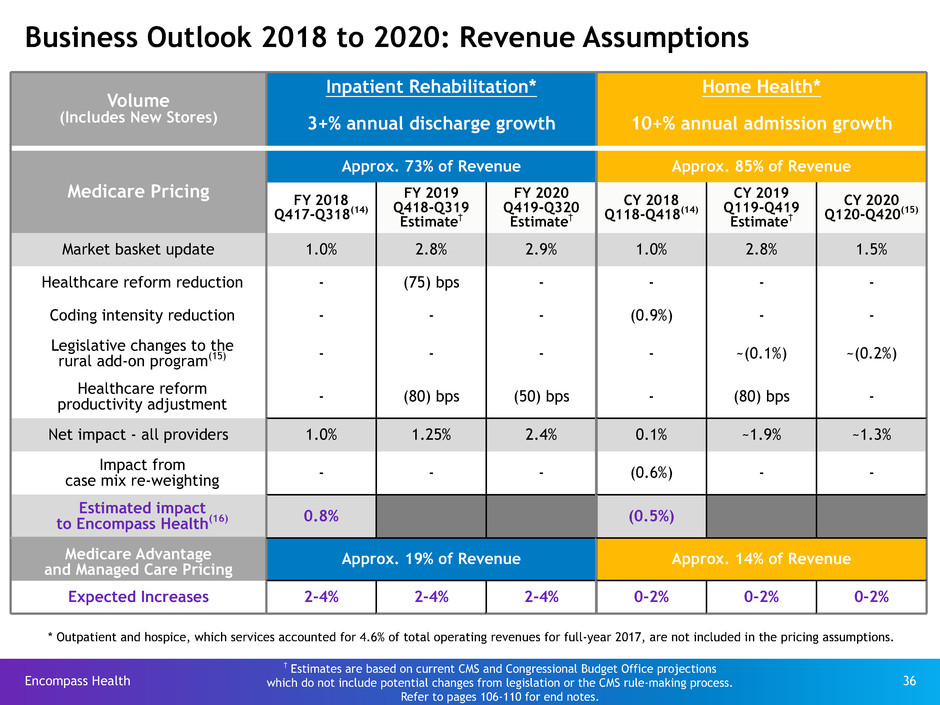
Business Outlook 2018 to 2020: Revenue Assumptions
Volume
(Includes New Stores)
Inpatient Rehabilitation* Home Health*
3+% annual discharge growth 10+% annual admission growth
Medicare Pricing
Approx. 73% of Revenue Approx. 85% of Revenue
FY 2018
Q417-Q318(14)
FY 2019
Q418-Q319
Estimate†
FY 2020
Q419-Q320
Estimate†
CY 2018
Q118-Q418(14)
CY 2019
Q119-Q419
Estimate†
CY 2020
Q120-Q420(15)
Market basket update 1.0% 2.8% 2.9% 1.0% 2.8% 1.5%
Healthcare reform reduction - (75) bps - - - -
Coding intensity reduction - - - (0.9%) - -
Legislative changes to the
rural add-on program(15) - - - - ~(0.1%) ~(0.2%)
Healthcare reform
productivity adjustment - (80) bps (50) bps - (80) bps -
Net impact - all providers 1.0% 1.25% 2.4% 0.1% ~1.9% ~1.3%
Impact from
case mix re-weighting - - - (0.6%) - -
Estimated impact
to Encompass Health(16) 0.8% (0.5%)
Medicare Advantage
and Managed Care Pricing Approx. 19% of Revenue Approx. 14% of Revenue
Expected Increases 2-4% 2-4% 2-4% 0-2% 0-2% 0-2%
* Outpatient and hospice, which services accounted for 4.6% of total operating revenues for full-year 2017, are not included in the pricing assumptions.
† Estimates are based on current CMS and Congressional Budget Office projections
which do not include potential changes from legislation or the CMS rule-making process.
Refer to pages 106-110 for end notes.
Encompass Health 37
Inpatient Rehabilitation Home Health and Hospice
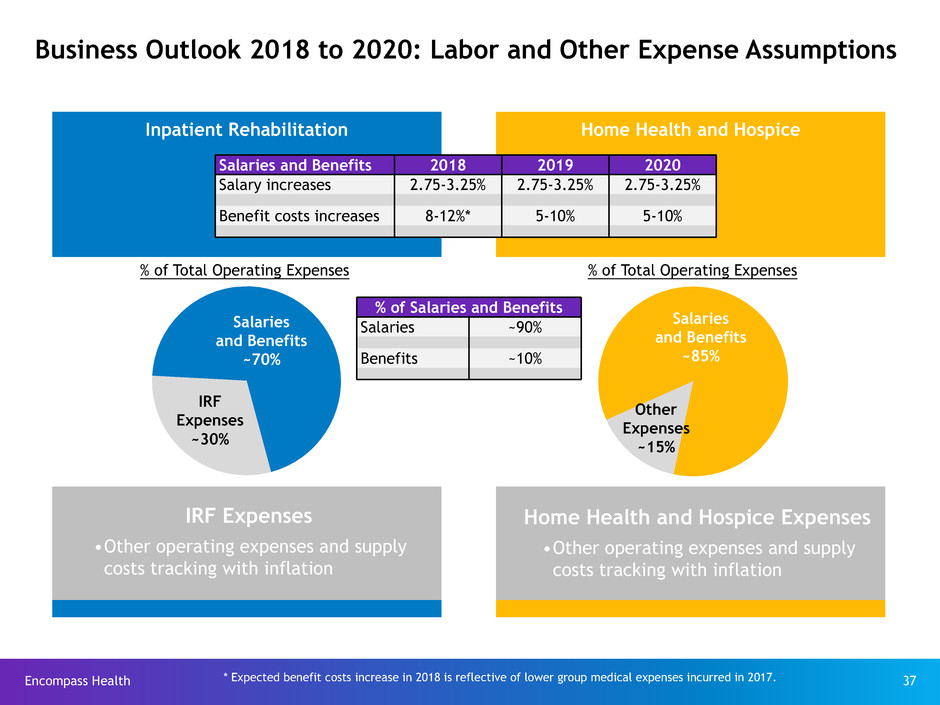
Business Outlook 2018 to 2020: Labor and Other Expense Assumptions
Salaries
and Benefits
~70%
IRF
Expenses
~30%
Salaries and Benefits 2018 2019 2020
Salary increases 2.75-3.25% 2.75-3.25% 2.75-3.25%
Benefit costs increases 8-12%* 5-10% 5-10%
IRF Expenses
•Other operating expenses and supply
costs tracking with inflation
Salaries
and Benefits
~85%
Other
Expenses
~15%
Home Health and Hospice Expenses
•Other operating expenses and supply
costs tracking with inflation
% of Salaries and Benefits
Salaries ~90%
Benefits ~10%
* Expected benefit costs increase in 2018 is reflective of lower group medical expenses incurred in 2017.
% of Total Operating Expenses % of Total Operating Expenses

Encompass Health 38
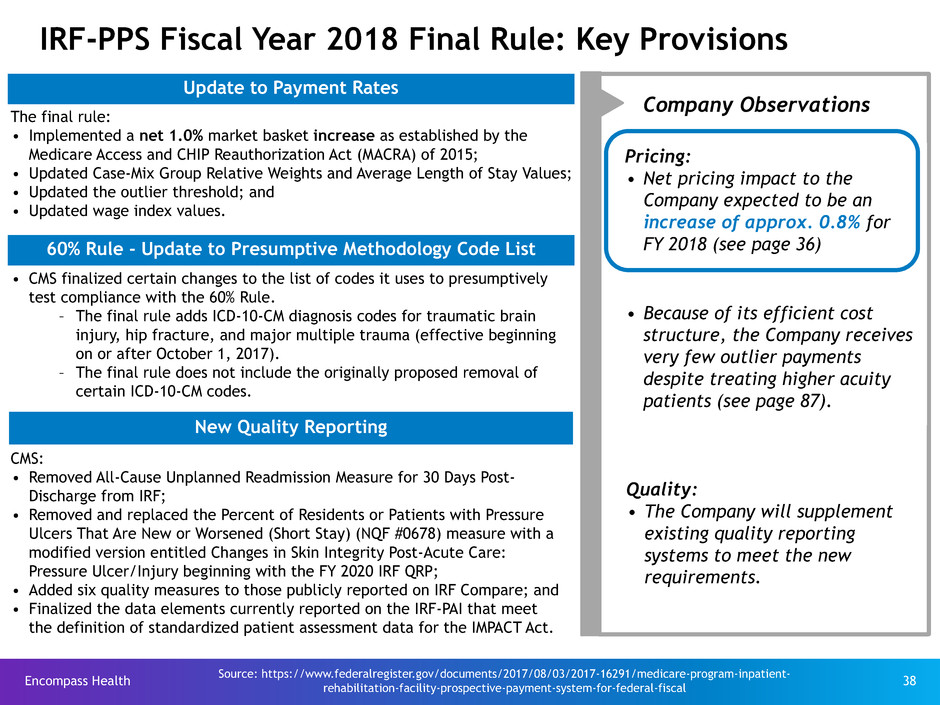
IRF-PPS Fiscal Year 2018 Final Rule: Key Provisions
Company Observations
Pricing:
• Net pricing impact to the
Company expected to be an
increase of approx. 0.8% for
FY 2018 (see page 36)
• Because of its efficient cost
structure, the Company receives
very few outlier payments
despite treating higher acuity
patients (see page 87).
Quality:
• The Company will supplement
existing quality reporting
systems to meet the new
requirements.
Source: https://www.federalregister.gov/documents/2017/08/03/2017-16291/medicare-program-inpatient-
rehabilitation-facility-prospective-payment-system-for-federal-fiscal
CMS:
• Removed All-Cause Unplanned Readmission Measure for 30 Days Post-
Discharge from IRF;
• Removed and replaced the Percent of Residents or Patients with Pressure
Ulcers That Are New or Worsened (Short Stay) (NQF #0678) measure with a
modified version entitled Changes in Skin Integrity Post-Acute Care:
Pressure Ulcer/Injury beginning with the FY 2020 IRF QRP;
• Added six quality measures to those publicly reported on IRF Compare; and
• Finalized the data elements currently reported on the IRF-PAI that meet
the definition of standardized patient assessment data for the IMPACT Act.
New Quality Reporting
Update to Payment Rates
The final rule:
• Implemented a net 1.0% market basket increase as established by the
Medicare Access and CHIP Reauthorization Act (MACRA) of 2015;
• Updated Case-Mix Group Relative Weights and Average Length of Stay Values;
• Updated the outlier threshold; and
• Updated wage index values.
60% Rule - Update to Presumptive Methodology Code List
• CMS finalized certain changes to the list of codes it uses to presumptively
test compliance with the 60% Rule.
– The final rule adds ICD-10-CM diagnosis codes for traumatic brain
injury, hip fracture, and major multiple trauma (effective beginning
on or after October 1, 2017).
– The final rule does not include the originally proposed removal of
certain ICD-10-CM codes.

Encompass Health 39
The final rule:
• Implemented a net 1.0% market basket increase as established by the
Medicare Access and CHIP Reauthorization Act (MACRA) of 2015 and
• Implemented year three of a three-year nominal case-mix coding
intensity reduction adjustment of (0.9%).
The final rule would have implemented the expiration of the rural add-on
(0.5%), but Congress elected to extend the adjustment through 2022(15),
albeit declining in amount along the way.
New Quality Reporting Measures
Final Rule Update to 2018 Payment Rates
Company Observations
CMS adopted, for the CY 2020 payment determination, three measures to
meet the requirements of the IMPACT Act:
• Changes in skin integrity post-acute care pressure ulcer/injury;
• Application of % of residents experiencing one or more falls with major
injury; and
• Application of % of long-term care hospital patients with an admit and
discharge functional assessment and care plan that addresses function.
These finalized measures will be calculated from OASIS data.
Sources: https://www.federalregister.gov/documents/2017/11/07/2017-23935/medicare-and-medicaid-
programs-cy-2018-home-health-prospective-payment-system-rate-update-and-cy
Proposed Home Health Groupings Model Not Finalized(15)
CMS did not finalize its proposal to implement significant changes to the
home health payment system beginning on January 1, 2019. These changes
were known as the Home Health Groupings Model (“HHGM”).
Payment System(15):
• The Company will continue to
engage with CMS, Congress, and
other stakeholders to ensure any
change to the underlying payment
system maintains access to needed
home health services.
Pricing:
• Net pricing impact to the
Company expected to be a
decrease of approx. 0.5% for
CY 2018 (see page 36)
Quality:
• The Company will supplement
existing processes and systems to
meet the new requirements.
HH-PPS Calendar Year 2018 Final Rule: Key Provisions

Encompass Health 40
Company observations and considerations with respect to the IMPACT Act:
▪ It was developed on a bi-partisan basis by the House Ways and Means and Senate Finance Committees and
incorporated feedback from healthcare providers and provider organizations that responded to the
Committees’ solicitation of post-acute payment reform ideas and proposals.
▪ It directs the United States Department of Health and Human Services (“HHS”), in consultation with
healthcare stakeholders, to implement standardized data collection processes for post-acute quality and
resource use measures.
▪ Although the IMPACT Act does not specifically call for the implementation of a new post-acute payment
system, the Company believes this act will lay the foundation for possible future post-acute payment
policies that would be based on patients’ medical conditions and other clinical factors rather than the
setting where the care is provided.
▪ It will create additional data reporting requirements for the Company’s IRFs(17) and home health agencies.
The precise details of these new reporting requirements, including timing and content, will be developed
and implemented by the Centers for Medicare and Medicaid Services through the regulatory process the
Company expects will take place over the next several years.
▪ While the Company cannot quantify the potential financial effect of the IMPACT Act on Encompass Health,
the Company believes any post-acute payment system that is data driven and focuses on the needs and
underlying medical conditions of post-acute patients will be positive for providers who offer high-quality,
cost-effective care. Encompass Health believes it is doing just that and expects this act will be positive for
the Company.
▪ However, it will likely take years for the quality data to be gathered, standardized patient assessment data
to be assembled and disseminated, and potential payment policies to be developed, tested and
promulgated. As the nation’s largest owner and operator of inpatient rehabilitation hospitals, the Company
looks forward to working with HHS, the Medicare Payment Advisory Commission and other healthcare
stakeholders on these initiatives.
IMPACT Act of 2014 - Enacted October 6, 2014
Source: https://www.govtrack.us/congress/bills/113/hr4994/text
Refer to pages 106-110 for end notes.

Encompass Health 41
Growth
Encompass Health is a leader in serving the post-acute patient population
and has multiple avenues available for sustained growth in both segments.
Favorable demographic trends are driving increased demand.

Encompass Health 42
The Company Has Multiple Avenues Available
for Sustained Growth in Both Segments
u The Company continues to have excellent organic growth opportunities ininpatient rehabilitation, home health, and hospice.
— Track record of consistent market share gains
— IRF organic growth supplemented by bed additions
— Maturation of acquired home health locations
u Target four to six new inpatient rehabilitation hospitals per year to complementorganic growth
— De novos and acquisitions will allow entry into, and growth in, new markets.
— Proven track record of success
u Target $50 to $100 million per year toward home health and hospice acquisitionsto complement organic growth
— Home health acquisitions and new-store growth prioritized in Encompass Health
IRF markets without current overlap
— Build additional scale in hospice via acquisitions and de novos
Encompass Health 43
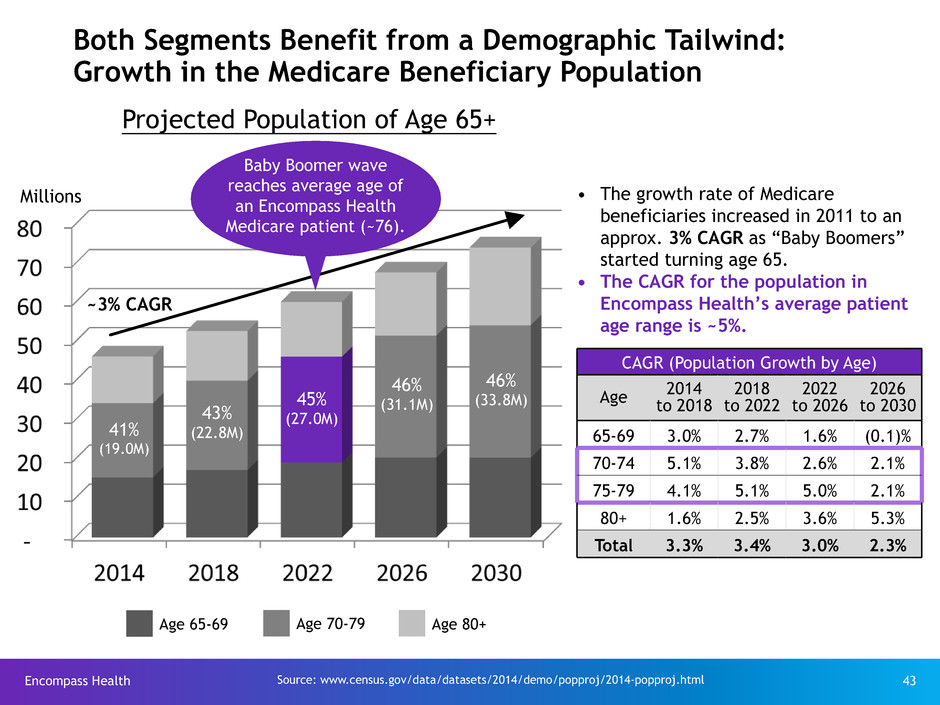
Both Segments Benefit from a Demographic Tailwind:
Growth in the Medicare Beneficiary Population
Projected Population of Age 65+
Age 80+Age 70-79Age 65-69
Millions • The growth rate of Medicare
beneficiaries increased in 2011 to an
approx. 3% CAGR as “Baby Boomers”
started turning age 65.
• The CAGR for the population in
Encompass Health’s average patient
age range is ~5%.
41%
(19.0M)
43%
(22.8M)
45%
(27.0M)
46%
(31.1M)
46%
(33.8M)
CAGR (Population Growth by Age)
Age 2014to 2018
2018
to 2022
2022
to 2026
2026
to 2030
65-69 3.0% 2.7% 1.6% (0.1)%
70-74 5.1% 3.8% 2.6% 2.1%
75-79 4.1% 5.1% 5.0% 2.1%
80+ 1.6% 2.5% 3.6% 5.3%
Total 3.3% 3.4% 3.0% 2.3%
~3% CAGR
Source: www.census.gov/data/datasets/2014/demo/popproj/2014-popproj.html
Baby Boomer wave
reaches average age of
an Encompass Health
Medicare patient (~76).
Encompass Health 44
1,600
1,400
1,200
1,000
800
600
400
200
0
132
127
122
117
112
107
102
97
92
87
82
77
72
2013 2014 2015 2016 2017 Projected
2018
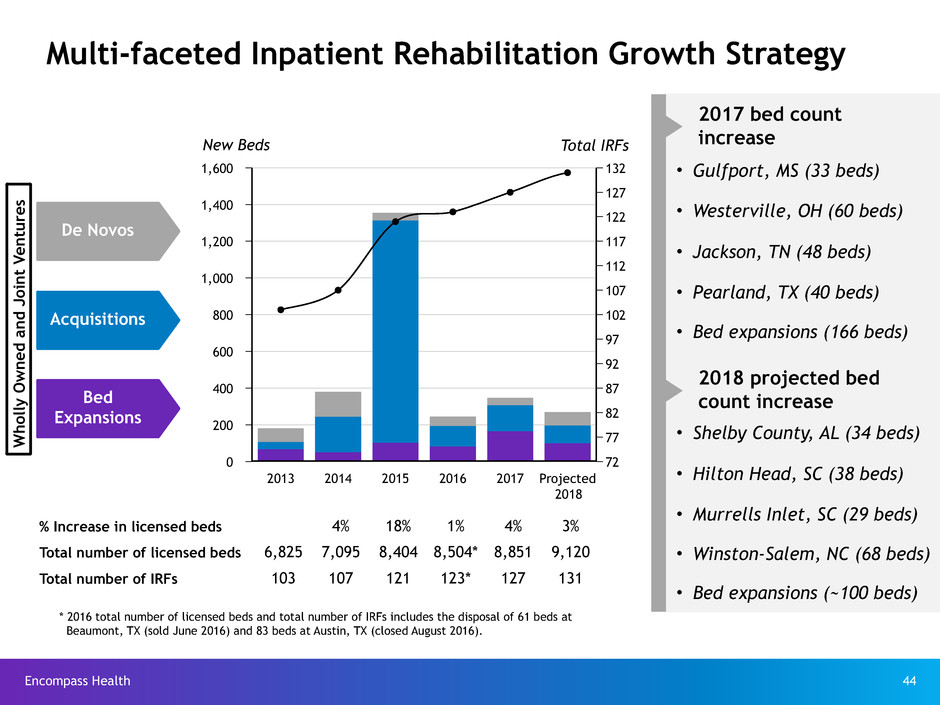
% Increase in licensed beds 4% 18% 1% 4% 3%
Total number of licensed beds 6,825 7,095 8,404 8,504* 8,851 9,120
Total number of IRFs 103 107 121 123* 127 131
Multi-faceted Inpatient Rehabilitation Growth Strategy
Total IRFsNew Beds
2017 bed count
increase
• Gulfport, MS (33 beds)
• Westerville, OH (60 beds)
• Jackson, TN (48 beds)
• Pearland, TX (40 beds)
• Bed expansions (166 beds)
2018 projected bed
count increase
• Shelby County, AL (34 beds)
• Hilton Head, SC (38 beds)
• Murrells Inlet, SC (29 beds)
• Winston-Salem, NC (68 beds)
• Bed expansions (~100 beds)
* 2016 total number of licensed beds and total number of IRFs includes the disposal of 61 beds at
Beaumont, TX (sold June 2016) and 83 beds at Austin, TX (closed August 2016).
Wholly Owned and Joint
Venture
s
Bed
Expansions
De Novos
Acquisitions
Encompass Health 45
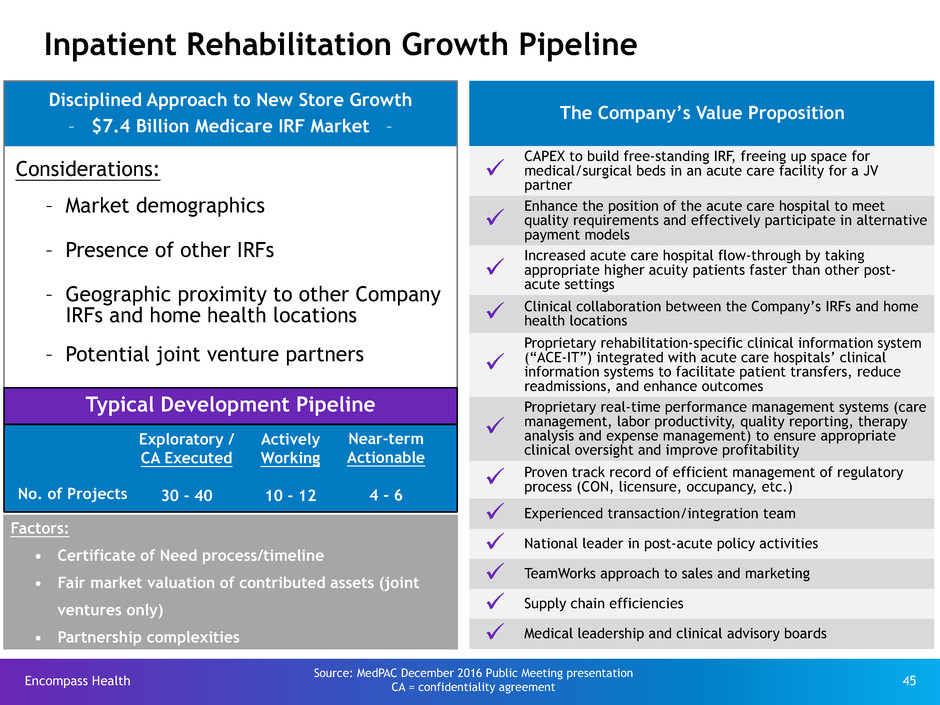
Disciplined Approach to New Store Growth
– $7.4 Billion Medicare IRF Market –
Considerations:
– Market demographics
– Presence of other IRFs
– Geographic proximity to other Company
IRFs and home health locations
– Potential joint venture partners
Source: MedPAC December 2016 Public Meeting presentation
CA = confidentiality agreement
Inpatient Rehabilitation Growth Pipeline
Typical Development Pipeline
Factors:
• Certificate of Need process/timeline
• Fair market valuation of contributed assets (joint
ventures only)
• Partnership complexities
The Company’s Value Proposition
ü CAPEX to build free-standing IRF, freeing up space formedical/surgical beds in an acute care facility for a JV
partner
ü Enhance the position of the acute care hospital to meetquality requirements and effectively participate in alternative
payment models
ü Increased acute care hospital flow-through by takingappropriate higher acuity patients faster than other post-
acute settings
ü Clinical collaboration between the Company’s IRFs and homehealth locations
ü
Proprietary rehabilitation-specific clinical information system
(“ACE-IT”) integrated with acute care hospitals’ clinical
information systems to facilitate patient transfers, reduce
readmissions, and enhance outcomes
ü
Proprietary real-time performance management systems (care
management, labor productivity, quality reporting, therapy
analysis and expense management) to ensure appropriate
clinical oversight and improve profitability
ü Proven track record of efficient management of regulatoryprocess (CON, licensure, occupancy, etc.)
ü Experienced transaction/integration team
ü National leader in post-acute policy activities
ü TeamWorks approach to sales and marketing
ü Supply chain efficiencies
ü Medical leadership and clinical advisory boards
No. of Projects
Exploratory /
CA Executed
30 - 40
Actively
Working
10 - 12
Near-term
Actionable
4 - 6

Encompass Health 46
• The Company’s IRF joint ventures began in 1991 with Vanderbilt University Medical Center.
• The Company’s joint venture acute care hospital partners own equity that ranges from 2.5% to 50%.
• 41 of 42 IRFs are consolidated joint ventures, with one accounted for under the equity method.
Inpatient Rehabilitation Acute Care Joint Venture Partnerships
42* IRF joint venture hospitals in place with major healthcare systems such as:
Joint ventures with acute care hospitals establish a solid foundation for integrated delivery
and alternative payment models.
• Barnes-Jewish • Monmouth Medical Center (Barnabas Health)
• University of Virginia Medical Center • Yuma Regional Medical Center
• Vanderbilt University Medical Center • Mercy Health System
• Geisinger Health System • Maine Medical Center
• Martin Health System • Methodist Healthcare-Memphis Hospitals,
a subsidiary of Methodist Le Bonheur Healthcare
* Excludes IRF joint venture hospitals that have been announced but were not operational as of December 31, 2017:
Winston-Salem, NC; Murrells Inlet, SC; Lubbock, TX; and Boise, ID.
Encompass Health 47
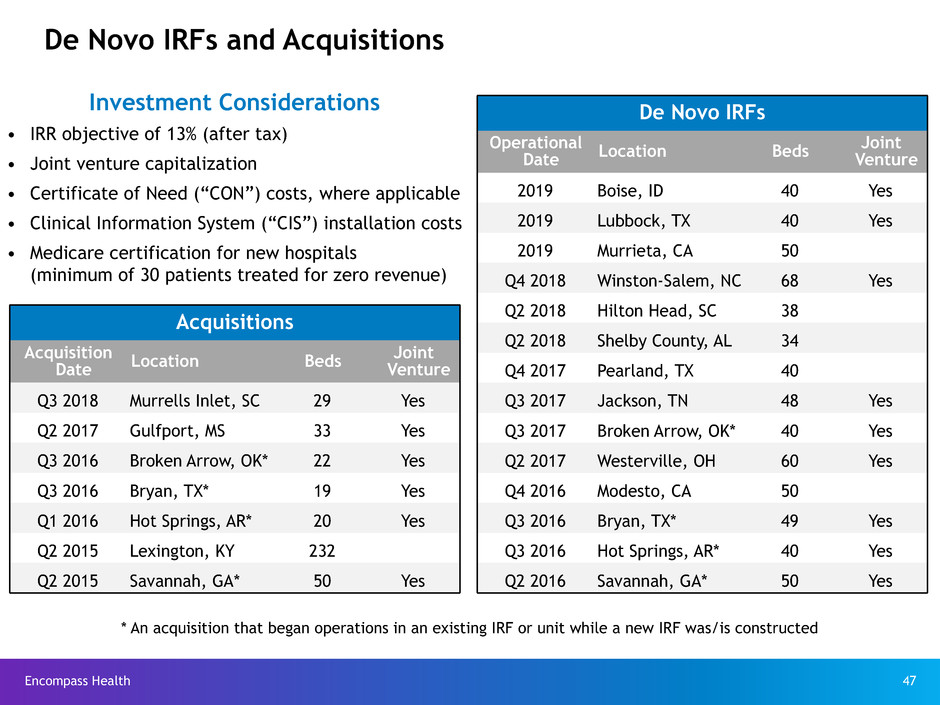
De Novo IRFs and Acquisitions
Investment Considerations
• IRR objective of 13% (after tax)
• Joint venture capitalization
• Certificate of Need (“CON”) costs, where applicable
• Clinical Information System (“CIS”) installation costs
• Medicare certification for new hospitals
(minimum of 30 patients treated for zero revenue)
De Novo IRFs
Operational
Date Location Beds
Joint
Venture
2019 Boise, ID 40 Yes
2019 Lubbock, TX 40 Yes
2019 Murrieta, CA 50
Q4 2018 Winston-Salem, NC 68 Yes
Q2 2018 Hilton Head, SC 38
Q2 2018 Shelby County, AL 34
Q4 2017 Pearland, TX 40
Q3 2017 Jackson, TN 48 Yes
Q3 2017 Broken Arrow, OK* 40 Yes
Q2 2017 Westerville, OH 60 Yes
Q4 2016 Modesto, CA 50
Q3 2016 Bryan, TX* 49 Yes
Q3 2016 Hot Springs, AR* 40 Yes
Q2 2016 Savannah, GA* 50 Yes
Acquisitions
Acquisition
Date Location Beds
Joint
Venture
Q3 2018 Murrells Inlet, SC 29 Yes
Q2 2017 Gulfport, MS 33 Yes
Q3 2016 Broken Arrow, OK* 22 Yes
Q3 2016 Bryan, TX* 19 Yes
Q1 2016 Hot Springs, AR* 20 Yes
Q2 2015 Lexington, KY 232
Q2 2015 Savannah, GA* 50 Yes
* An acquisition that began operations in an existing IRF or unit while a new IRF was/is constructed

Encompass Health 48
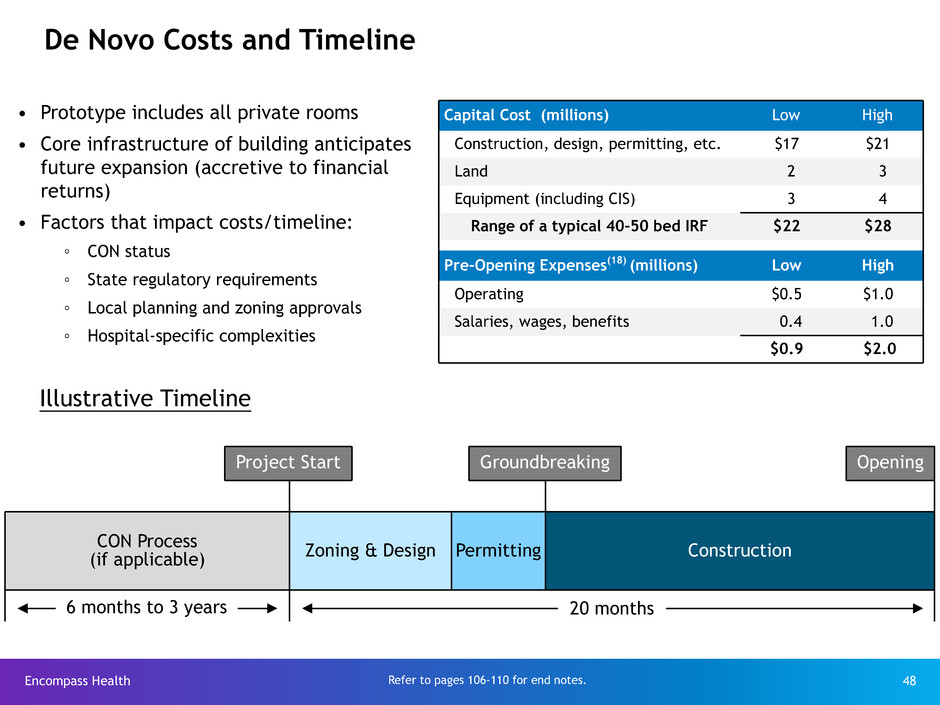
CON Process
(if applicable) Zoning & Design Permitting Construction
OpeningGroundbreaking
De Novo Costs and Timeline
Capital Cost (millions) Low High
Construction, design, permitting, etc. $17 $21
Land 2 3
Equipment (including CIS) 3 4
Range of a typical 40-50 bed IRF $22 $28
Pre-Opening Expenses(18) (millions) Low High
Operating $0.5 $1.0
Salaries, wages, benefits 0.4 1.0
$0.9 $2.0
• Prototype includes all private rooms
• Core infrastructure of building anticipates
future expansion (accretive to financial
returns)
• Factors that impact costs/timeline:
◦ CON status
◦ State regulatory requirements
◦ Local planning and zoning approvals
◦ Hospital-specific complexities
Project Start
20 months6 months to 3 years
Illustrative Timeline
Refer to pages 106-110 for end notes.
Encompass Health 49
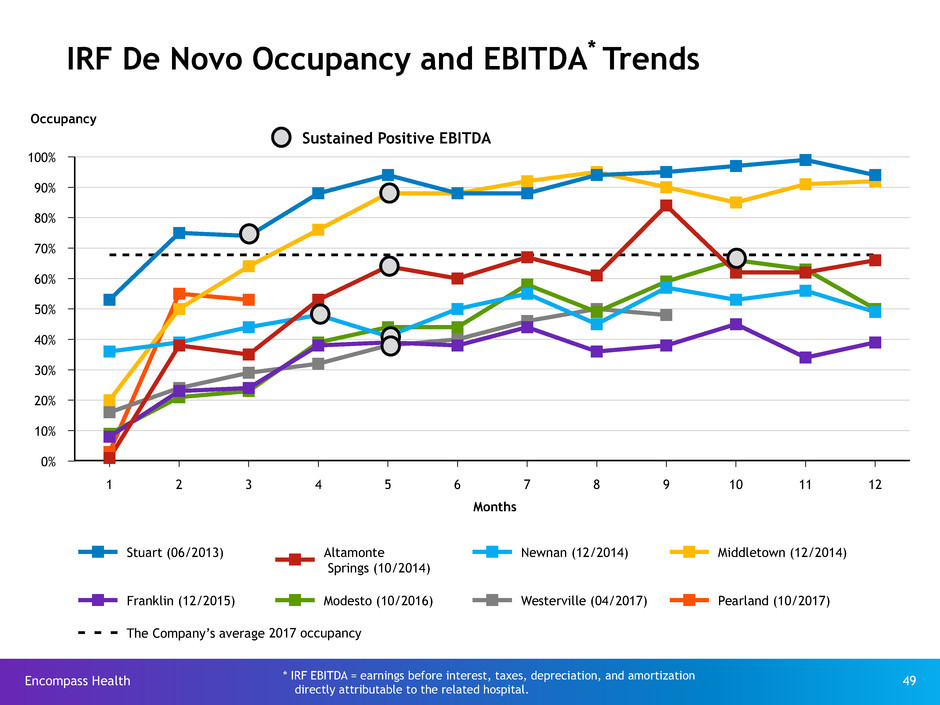
Stuart (06/2013) Altamonte
Springs (10/2014)
Newnan (12/2014) Middletown (12/2014)
Franklin (12/2015) Modesto (10/2016) Westerville (04/2017) Pearland (10/2017)
The Company’s average
100%
90%
80%
70%
60%
50%
40%
30%
20%
10%
0%
1 2 3 4 5 6 7 8 9 10 11 12
Months
IRF De Novo Occupancy and EBITDA* Trends
Occupancy
Sustained Positive EBITDA
* IRF EBITDA = earnings before interest, taxes, depreciation, and amortization
directly attributable to the related hospital.
2017 occupancy

Encompass Health 50
• Strong demand due to cost effectiveness of home-based care and
implementation of alternative payment models
• Strong organic growth from existing agencies
• Located in markets with attractive demographics
* Currently located in states that represent ~67% of total Medicare home
health and hospice spend
• Prioritization of existing home health markets
• Opportunity to build scale and leverage components of existing
infrastructure
• Attractive partner due to quality of outcomes, data management, scale
and market density, and willingness/ability to treat high acuity and/or
chronic patients
• Plan of care coordination with the Company’s IRFs
• Care Transition Coordinators serve as representatives in transitional care
activities and strategic relationships with other healthcare providers
• Highly fragmented market
• Prioritization of new IRF overlap markets
• Proven ability to consummate and integrate acquisitions
• Sustainable and replicable culture
• Implementation of best practices and technology
Organic Growth
Home Health
Acquisitions
and De Novos
Hospice
Acquisitions
and De Novos
Clinical
Collaboration
Multi-faceted Home Health and Hospice Growth Strategy
Encompass Health 51
13,000
12,000
11,000
10,000
9,000
8,000
7,000
6,000
5,000
4,000
#
of
Ag
en
ci
es
1996 1998 2000 2002 2004 2006 2008 2010 2012 2014
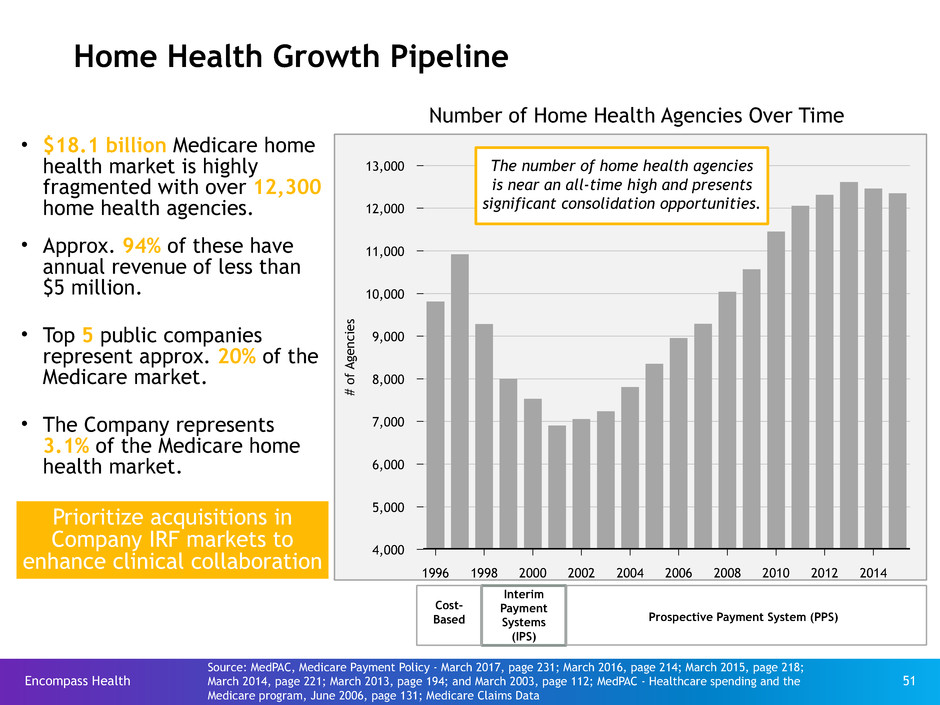
Home Health Growth Pipeline
• $18.1 billion Medicare home
health market is highly
fragmented with over 12,300
home health agencies.
• Approx. 94% of these have
annual revenue of less than
$5 million.
• Top 5 public companies
represent approx. 20% of the
Medicare market.
• The Company represents
3.1% of the Medicare home
health market.
Prioritize acquisitions in
Company IRF markets to
enhance clinical collaboration
Number of Home Health Agencies Over Time
Cost-
Based
Interim
Payment
Systems
(IPS)
Prospective Payment System (PPS)
The number of home health agencies
is near an all-time high and presents
significant consolidation opportunities.
Source: MedPAC, Medicare Payment Policy - March 2017, page 231; March 2016, page 214; March 2015, page 218;
March 2014, page 221; March 2013, page 194; and March 2003, page 112; MedPAC - Healthcare spending and the
Medicare program, June 2006, page 131; Medicare Claims Data
Encompass Health 52
Freestanding
Hospital/SNF
based
Home Health
based
4,000
3,000
2,000
1,000
0
2000 2007 2013 2014 2015
1,069
2,103
2,844 3,024 3,138807
704
578 558
547
378
443
503 510
514
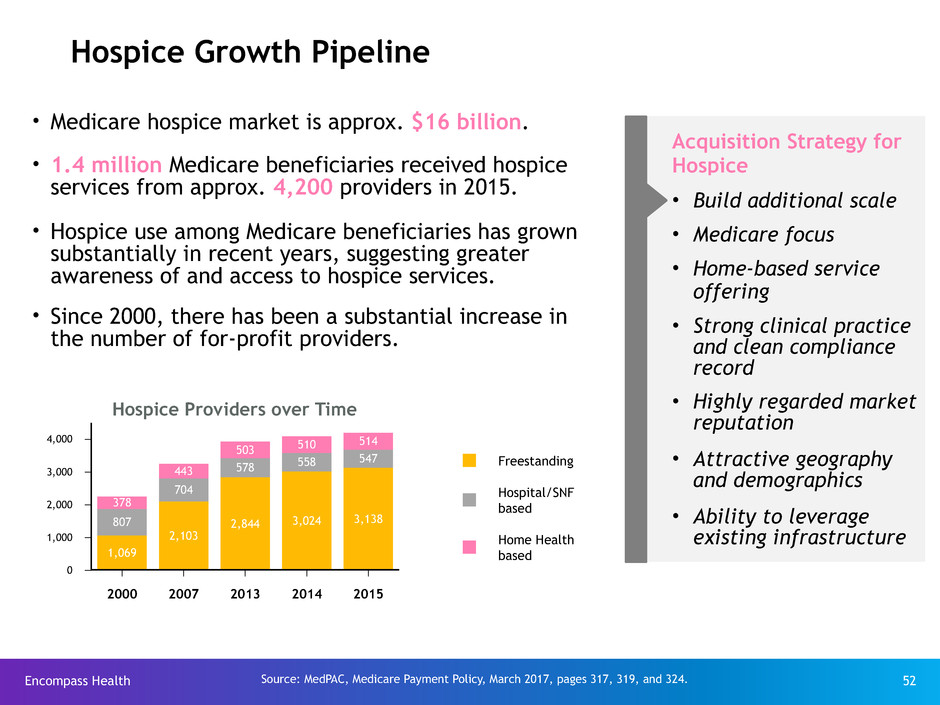
Hospice Growth Pipeline
• Medicare hospice market is approx. $16 billion.
• 1.4 million Medicare beneficiaries received hospice
services from approx. 4,200 providers in 2015.
• Hospice use among Medicare beneficiaries has grown
substantially in recent years, suggesting greater
awareness of and access to hospice services.
• Since 2000, there has been a substantial increase in
the number of for-profit providers.
Acquisition Strategy for
Hospice
• Build additional scale
• Medicare focus
• Home-based service
offering
• Strong clinical practice
and clean compliance
record
• Highly regarded market
reputation
• Attractive geography
and demographics
• Ability to leverage
existing infrastructure
Hospice Providers over Time
Source: MedPAC, Medicare Payment Policy, March 2017, pages 317, 319, and 324.

Encompass Health 53
Alternative Payment Models

Encompass Health 54
Accountable Care Organizations (“ACOs”)
Medicare Shared Savings Program (MSSP)
(2018 - 561 ACOs / 10.5 million Medicare beneficiaries)
• Performance Year 4 (2016) results:
◦ 241 of 432 ACOs (56%) held spending below their benchmark.
▪ 107 of these ACOs reduced health costs compared to their benchmark, but did not meet
the minimum savings threshold for shared savings.
◦ 191 ACOs (44%) did not reduce costs compared to their benchmark.
◦ Shared Savings Program ACOs generated total program savings of $652 million.
• A new MSSP model called Track 1+ Model began with 55 ACOs in 2018 and incorporates more limited
downside risk than Tracks 2 or 3 (two-sided risk models) of the MSSP
Source: CMS/HHS press releases and public use files
The Company serves as Premier ACO’s exclusive preferred home health provider.
(~22,000 covered lives in north Texas and southern Oklahoma)
Ÿ Receives increased referrals for Medicare home health patients from the ACO
Ÿ Eligible to receive a portion of the ACO’s shared savings
Ÿ Total shared savings achieved by ACO in 2016 was $12.5 million.
- Ranked 2nd in savings rate out of all MSSP ACOs with >20,000 assigned beneficiaries
- Met the minimum savings rate to participate in shared savings
Next Generation ACOs
(2018 - 58 ACOs / ~2.0 million Medicare beneficiaries)
• Initiative launched in January 2016 for ACOs that are experienced in coordinating care for populations
of patients
• Allows providers to assume higher levels of financial risk and reward than are available under the MSSP
• Performance Year 1 (2016) results:
◦ 11 out of 18 ACOs generated savings and received shared savings of $58 million.
◦ Remaining 7 ACOs generated losses and were required to pay back $20 million to CMS.
As of
January 2018,
there were
619
MSSP and
Next Generation
ACOs serving
~12.5 million
Medicare
and/or Medicaid
beneficiaries.
Performance
results so far
have been
mixed.

Encompass Health 55
Bundled Payments
Model 1
All acute patients (all DRGs)
– Concluded December 31, 2016 –
The Bundled Payments for Care Improvement
(BPCI) initiative currently tests
four types of bundles
(i.e. “Models”):
Model 2*
Hospital plus post-acute period (selected DRGs)
Model 3*
Post acute only (selected DRGs)
Model 4*
Hospital plus readmissions
(selected DRGs)
How the Retrospective Models Work
Ÿ The BPCI “convener” is responsible for bringing
providers together to provide a continuum of services
throughout an episode of care. The BPCI “awardee”
is the entity that bears the financial risk and receives
the shared savings from CMS.
Ÿ Each participating provider in the care sequence
continues to receive its traditional reimbursement
from Medicare.
Ÿ The sum of all payments made to each provider for
selected DRGs is then retroactively reconciled to a
target payment determined by CMS. Payment
reconciliations are performed quarterly, typically
with a 9- to 12-month lag.
Ÿ Payment reconciliations: If actual spending exceeds
the target, the awardee is responsible for paying a
portion of the difference to CMS. If actual spending is
less than the target, the awardee keeps a portion of
the savings.
Ÿ The convener can choose to partner with other
providers in shared savings agreements and allocate
the savings across the providers who participated in
providing the continuum of care.
Ÿ Shared savings agreements must be reviewed and
approved by the Center for Medicare and Medicaid
Innovation.
Models 2 & 3 have the most impact on post-acute providers.
Notes: Models 1, 2, and 3 are retrospective models; model 4 is a prospective model.
The convener and awardee can be, but may not be, the same entity.
* BPCI Models 2, 3, and 4 will end on September 30, 2018 and be replaced by the BPCI Advanced model which begins on October 1, 2018 and runs through
December 31, 2023. BPCI Advanced is a new voluntary episode payment model that will test a new iteration of bundled payments for 29 inpatient clinical
episodes and 3 outpatient clinical episodes. For more information regarding BPCI Advanced, see https://innovation.cms.gov/initiatives/bpci-advanced.
Encompass Health 56
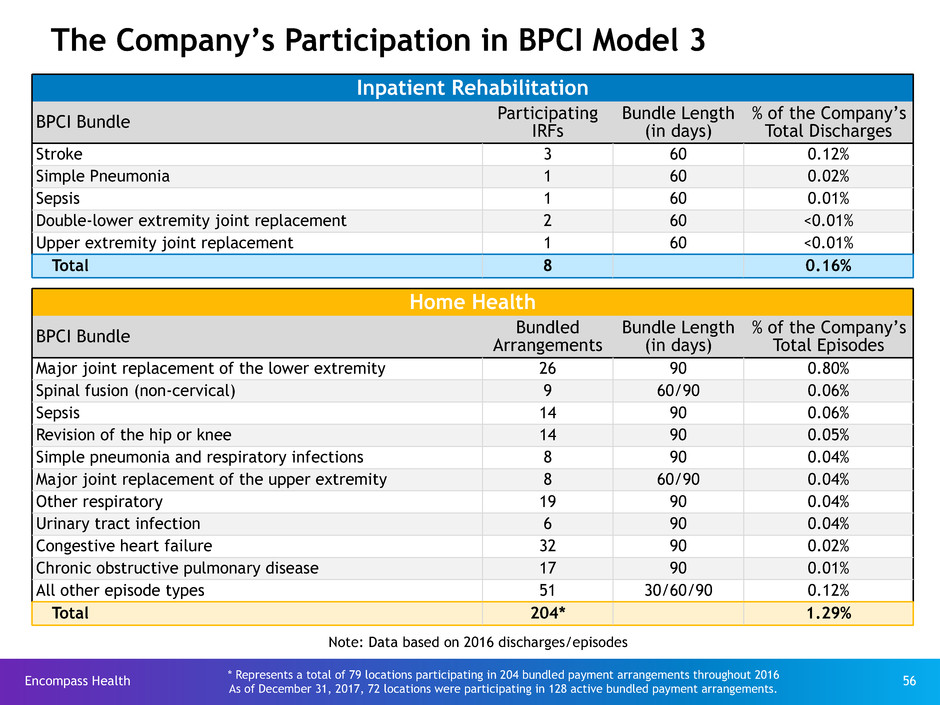
The Company’s Participation in BPCI Model 3
Inpatient Rehabilitation
BPCI Bundle ParticipatingIRFs
Bundle Length
(in days)
% of the Company’s
Total Discharges
Stroke 3 60 0.12%
Simple Pneumonia 1 60 0.02%
Sepsis 1 60 0.01%
Double-lower extremity joint replacement 2 60 <0.01%
Upper extremity joint replacement 1 60 <0.01%
Total 8 0.16%
Home Health
BPCI Bundle BundledArrangements
Bundle Length
(in days)
% of the Company’s
Total Episodes
Major joint replacement of the lower extremity 26 90 0.80%
Spinal fusion (non-cervical) 9 60/90 0.06%
Sepsis 14 90 0.06%
Revision of the hip or knee 14 90 0.05%
Simple pneumonia and respiratory infections 8 90 0.04%
Major joint replacement of the upper extremity 8 60/90 0.04%
Other respiratory 19 90 0.04%
Urinary tract infection 6 90 0.04%
Congestive heart failure 32 90 0.02%
Chronic obstructive pulmonary disease 17 90 0.01%
All other episode types 51 30/60/90 0.12%
Total 204* 1.29%
* Represents a total of 79 locations participating in 204 bundled payment arrangements throughout 2016
As of December 31, 2017, 72 locations were participating in 128 active bundled payment arrangements.
Note: Data based on 2016 discharges/episodes
Encompass Health 57* These comorbidities are specific to acute care hospitals and are defined differently than IRFs’ comorbidities.Source: https://innovation.cms.gov/initiatives/cjr
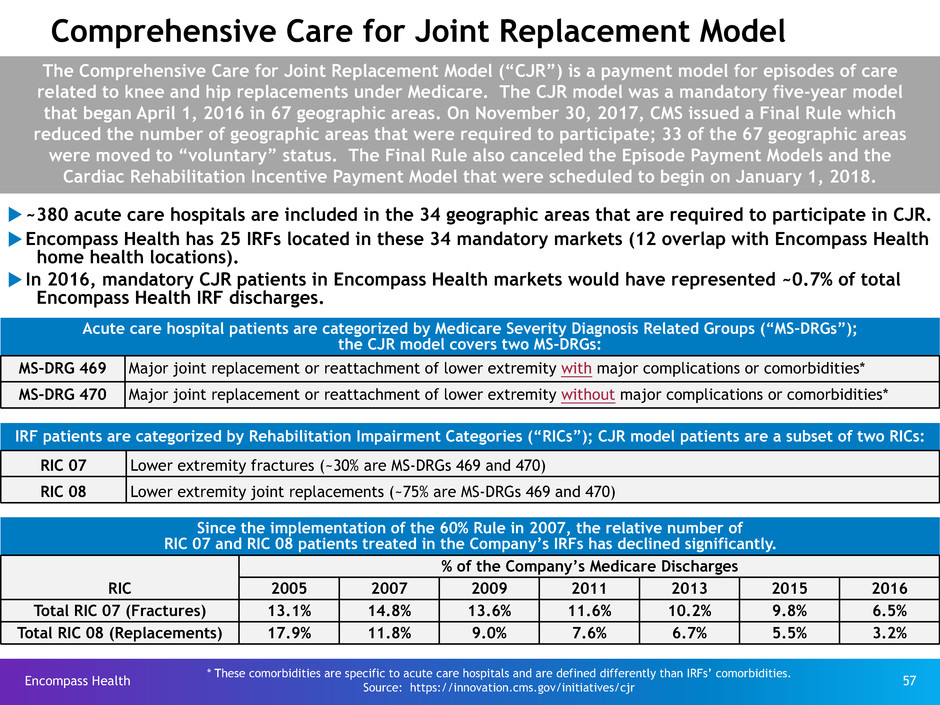
Acute care hospital patients are categorized by Medicare Severity Diagnosis Related Groups (“MS-DRGs”);
the CJR model covers two MS-DRGs:
MS-DRG 469 Major joint replacement or reattachment of lower extremity with major complications or comorbidities*
MS-DRG 470 Major joint replacement or reattachment of lower extremity without major complications or comorbidities*
IRF patients are categorized by Rehabilitation Impairment Categories (“RICs”); CJR model patients are a subset of two RICs:
RIC 07 Lower extremity fractures (~30% are MS-DRGs 469 and 470)
RIC 08 Lower extremity joint replacements (~75% are MS-DRGs 469 and 470)
Since the implementation of the 60% Rule in 2007, the relative number of
RIC 07 and RIC 08 patients treated in the Company’s IRFs has declined significantly.
RIC
% of the Company’s Medicare Discharges
2005 2007 2009 2011 2013 2015 2016
Total RIC 07 (Fractures) 13.1% 14.8% 13.6% 11.6% 10.2% 9.8% 6.5%
Total RIC 08 (Replacements) 17.9% 11.8% 9.0% 7.6% 6.7% 5.5% 3.2%
Comprehensive Care for Joint Replacement Model
The Comprehensive Care for Joint Replacement Model (“CJR”) is a payment model for episodes of care
related to knee and hip replacements under Medicare. The CJR model was a mandatory five-year model
that began April 1, 2016 in 67 geographic areas. On November 30, 2017, CMS issued a Final Rule which
reduced the number of geographic areas that were required to participate; 33 of the 67 geographic areas
were moved to “voluntary” status. The Final Rule also canceled the Episode Payment Models and the
Cardiac Rehabilitation Incentive Payment Model that were scheduled to begin on January 1, 2018.
u~380 acute care hospitals are included in the 34 geographic areas that are required to participate in CJR.
uEncompass Health has 25 IRFs located in these 34 mandatory markets (12 overlap with Encompass Health
home health locations).
uIn 2016, mandatory CJR patients in Encompass Health markets would have represented ~0.7% of total
Encompass Health IRF discharges.
Encompass Health 58
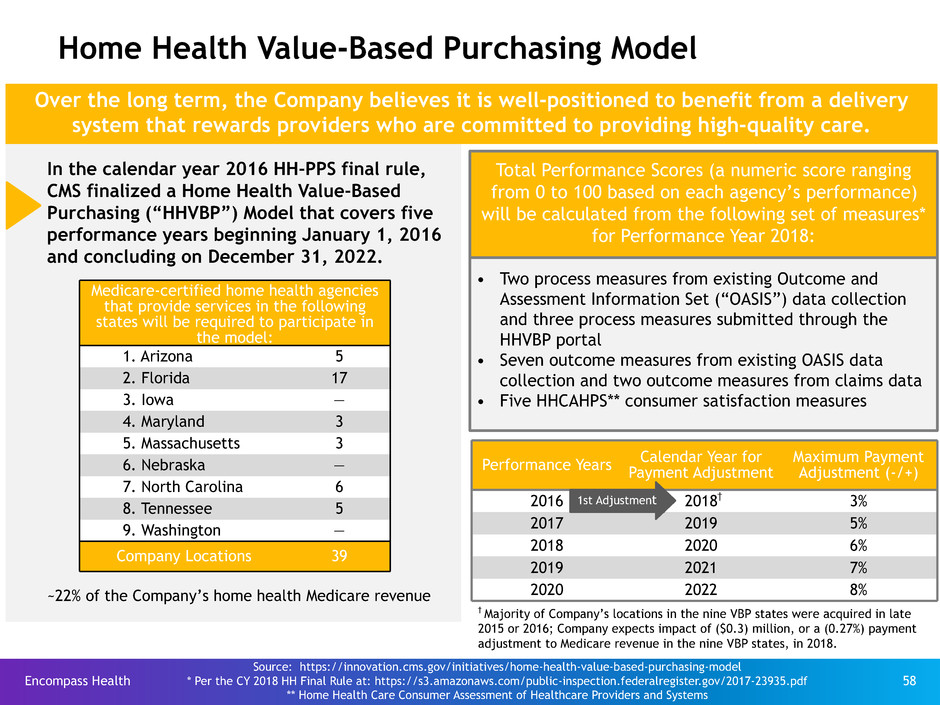
Medicare-certified home health agencies
that provide services in the following
states will be required to participate in
the model:
1. Arizona 5
2. Florida 17
3. Iowa —
4. Maryland 3
5. Massachusetts 3
6. Nebraska —
7. North Carolina 6
8. Tennessee 5
9. Washington —
Company Locations 39
In the calendar year 2016 HH-PPS final rule,
CMS finalized a Home Health Value-Based
Purchasing (“HHVBP”) Model that covers five
performance years beginning January 1, 2016
and concluding on December 31, 2022.
Home Health Value-Based Purchasing Model
Over the long term, the Company believes it is well-positioned to benefit from a delivery
system that rewards providers who are committed to providing high-quality care.
• Two process measures from existing Outcome and
Assessment Information Set (“OASIS”) data collection
and three process measures submitted through the
HHVBP portal
• Seven outcome measures from existing OASIS data
collection and two outcome measures from claims data
• Five HHCAHPS** consumer satisfaction measures
Total Performance Scores (a numeric score ranging
from 0 to 100 based on each agency’s performance)
will be calculated from the following set of measures*
for Performance Year 2018:
Performance Years Calendar Year forPayment Adjustment
Maximum Payment
Adjustment (-/+)
2016 2018† 3%
2017 2019 5%
2018 2020 6%
2019 2021 7%
2020 2022 8%
Source: https://innovation.cms.gov/initiatives/home-health-value-based-purchasing-model
* Per the CY 2018 HH Final Rule at: https://s3.amazonaws.com/public-inspection.federalregister.gov/2017-23935.pdf
** Home Health Care Consumer Assessment of Healthcare Providers and Systems
~22% of the Company’s home health Medicare revenue
1st Adjustment
† Majority of Company’s locations in the nine VBP states were acquired in late
2015 or 2016; Company expects impact of ($0.3) million, or a (0.27%) payment
adjustment to Medicare revenue in the nine VBP states, in 2018.

Encompass Health 59
Capital Structure
Encompass Health is positioned with a
cost-efficient, flexible capital structure.
Encompass Health 60
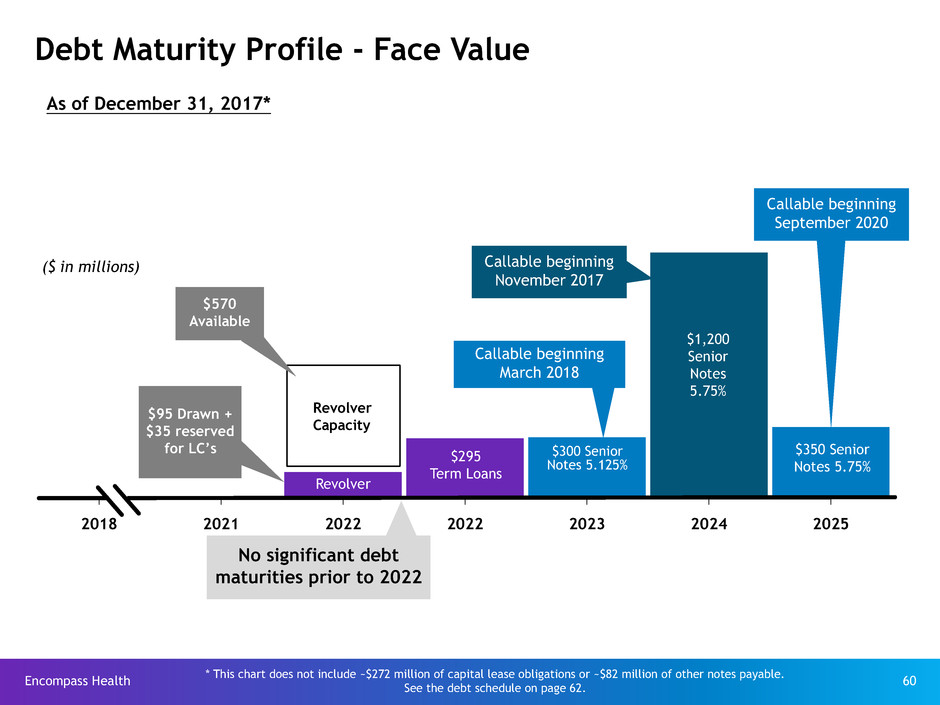
Debt Maturity Profile - Face Value
2018 2021 2022 2022 2023 2024 2025
$350 Senior
Notes 5.75%
$1,200
Senior
Notes
5.75%
$300 Senior
Notes 5.125%
$95 Drawn +
$35 reserved
for LC’s
As of December 31, 2017*
($ in millions)
$570
Available
Callable beginning
November 2017
Revolver
Revolver
Capacity
$295
Term Loans
Callable beginning
September 2020
No significant debt
maturities prior to 2022
Callable beginning
March 2018
* This chart does not include ~$272 million of capital lease obligations or ~$82 million of other notes payable.
See the debt schedule on page 62.
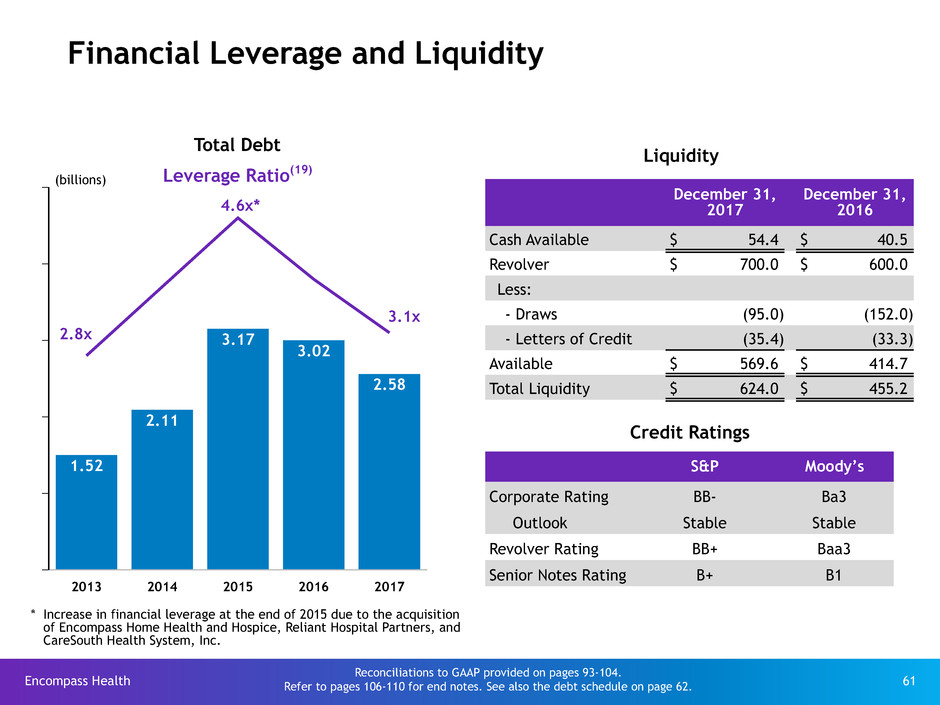
Encompass Health 61
2013 2014 2015 2016 2017
1.52
2.11
3.17 3.02
2.58
S&P Moody’s
Corporate Rating BB- Ba3
Outlook Stable Stable
Revolver Rating BB+ Baa3
Senior Notes Rating B+ B1
Financial Leverage and Liquidity
(1)
Liquidity
Credit Ratings
(billions) Leverage Ratio(19)
Total Debt
3.1x
December 31,
2017
December 31,
2016
Cash Available $ 54.4 $ 40.5
Revolver $ 700.0 $ 600.0
Less:
- Draws (95.0) (152.0)
- Letters of Credit (35.4) (33.3)
Available $ 569.6 $ 414.7
Total Liquidity $ 624.0 $ 455.2
2.8x
Reconciliations to GAAP provided on pages 93-104.
Refer to pages 106-110 for end notes. See also the debt schedule on page 62.
4.6x*
* Increase in financial leverage at the end of 2015 due to the acquisition
of Encompass Home Health and Hospice, Reliant Hospital Partners, and
CareSouth Health System, Inc.
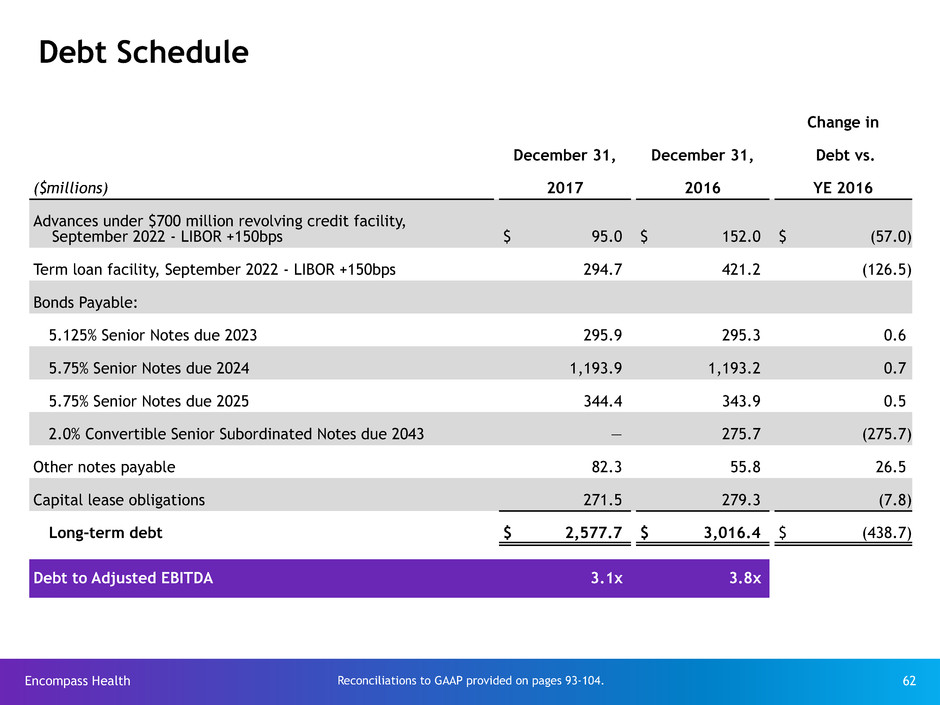
Encompass Health 62Reconciliations to GAAP provided on pages 93-104.
Debt Schedule
Change in
December 31, December 31, Debt vs.
($millions) 2017 2016 YE 2016
Advances under $700 million revolving credit facility,
September 2022 - LIBOR +150bps $ 95.0 $ 152.0 $ (57.0)
Term loan facility, September 2022 - LIBOR +150bps 294.7 421.2 (126.5)
Bonds Payable:
5.125% Senior Notes due 2023 295.9 295.3 0.6
5.75% Senior Notes due 2024 1,193.9 1,193.2 0.7
5.75% Senior Notes due 2025 344.4 343.9 0.5
2.0% Convertible Senior Subordinated Notes due 2043 — 275.7 (275.7)
Other notes payable 82.3 55.8 26.5
Capital lease obligations 271.5 279.3 (7.8)
Long-term debt $ 2,577.7 $ 3,016.4 $ (438.7)
Debt to Adjusted EBITDA 3.1x 3.8x
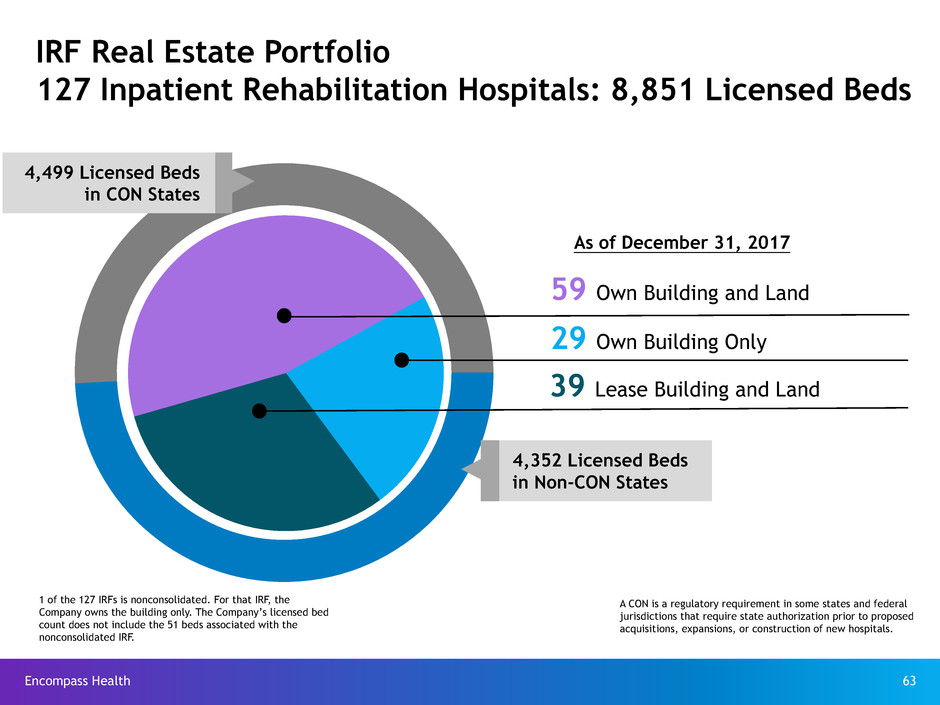
Encompass Health 63
39 Lease Building and Land
A CON is a regulatory requirement in some states and federal
jurisdictions that require state authorization prior to proposed
acquisitions, expansions, or construction of new hospitals.
59 Own Building and Land
29 Own Building Only
IRF Real Estate Portfolio
127 Inpatient Rehabilitation Hospitals: 8,851 Licensed Beds
4,499 Licensed Beds
in CON States
4,352 Licensed Beds
in Non-CON States
1 of the 127 IRFs is nonconsolidated. For that IRF, the
Company owns the building only. The Company’s licensed bed
count does not include the 51 beds associated with the
nonconsolidated IRF.
As of December 31, 2017
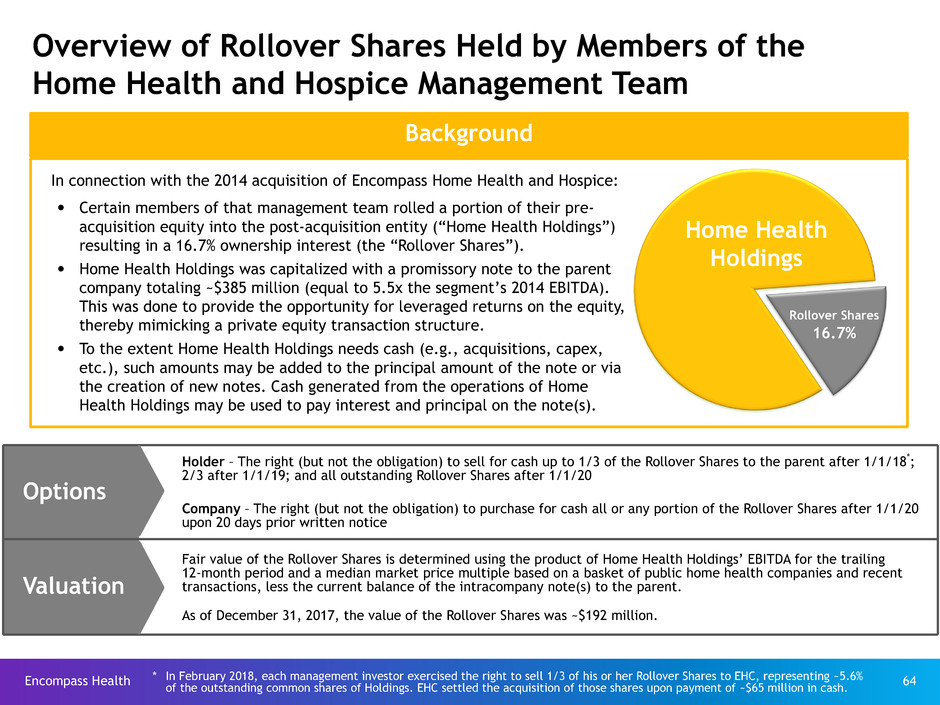
Encompass Health 64
Options
Holder – The right (but not the obligation) to sell for cash up to 1/3 of the Rollover Shares to the parent after 1/1/18*;
2/3 after 1/1/19; and all outstanding Rollover Shares after 1/1/20
Company – The right (but not the obligation) to purchase for cash all or any portion of the Rollover Shares after 1/1/20
upon 20 days prior written notice
Valuation
Fair value of the Rollover Shares is determined using the product of Home Health Holdings’ EBITDA for the trailing
12-month period and a median market price multiple based on a basket of public home health companies and recent
transactions, less the current balance of the intracompany note(s) to the parent.
As of December 31, 2017, the value of the Rollover Shares was ~$192 million.
In connection with the 2014 acquisition of Encompass Home Health and Hospice:
• Certain members of that management team rolled a portion of their pre-
acquisition equity into the post-acquisition entity (“Home Health Holdings”)
resulting in a 16.7% ownership interest (the “Rollover Shares”).
• Home Health Holdings was capitalized with a promissory note to the parent
company totaling ~$385 million (equal to 5.5x the segment’s 2014 EBITDA).
This was done to provide the opportunity for leveraged returns on the equity,
thereby mimicking a private equity transaction structure.
• To the extent Home Health Holdings needs cash (e.g., acquisitions, capex,
etc.), such amounts may be added to the principal amount of the note or via
the creation of new notes. Cash generated from the operations of Home
Health Holdings may be used to pay interest and principal on the note(s).
Overview of Rollover Shares Held by Members of the
Home Health and Hospice Management Team
Background
Home Health
Holdings
Rollover Shares
16.7%
* In February 2018, each management investor exercised the right to sell 1/3 of his or her Rollover Shares to EHC, representing ~5.6%
of the outstanding common shares of Holdings. EHC settled the acquisition of those shares upon payment of ~$65 million in cash.

Encompass Health 65
Information Technology
Encompass Health utilizes information technology to
improve patient care and generate operating efficiencies.
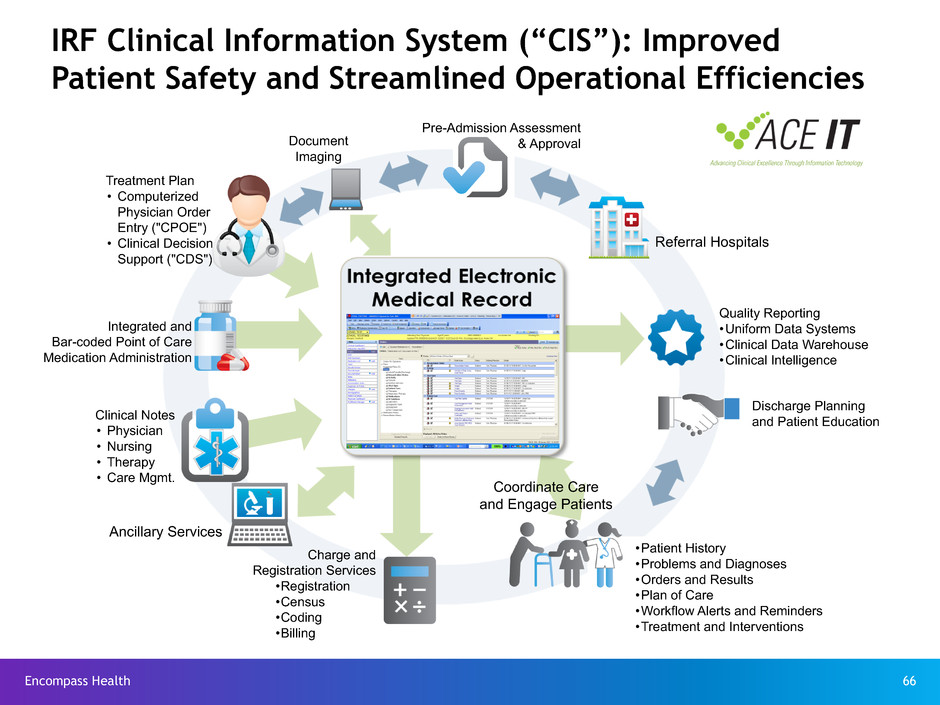
Encompass Health 66
IRF Clinical Information System (“CIS”): Improved
Patient Safety and Streamlined Operational Efficiencies
Pre-Admission Assessment
& Approval
Discharge Planning
and Patient Education
•Patient History
•Problems and Diagnoses
•Orders and Results
•Plan of Care
•Workflow Alerts and Reminders
•Treatment and Interventions
Document
Imaging
Charge and
Registration Services
•Registration
•Census
•Coding
•Billing
Quality Reporting
•Uniform Data Systems
•Clinical Data Warehouse
•Clinical Intelligence
Referral Hospitals
Ancillary Services
Clinical Notes
• Physician
• Nursing
• Therapy
• Care Mgmt.
Integrated and
Bar-coded Point of Care
Medication Administration
Treatment Plan
• Computerized
Physician Order
Entry ("CPOE")
• Clinical Decision
Support ("CDS")
Coordinate Care
and Engage Patients

Encompass Health 67
IRF Proprietary Management System: Beacon
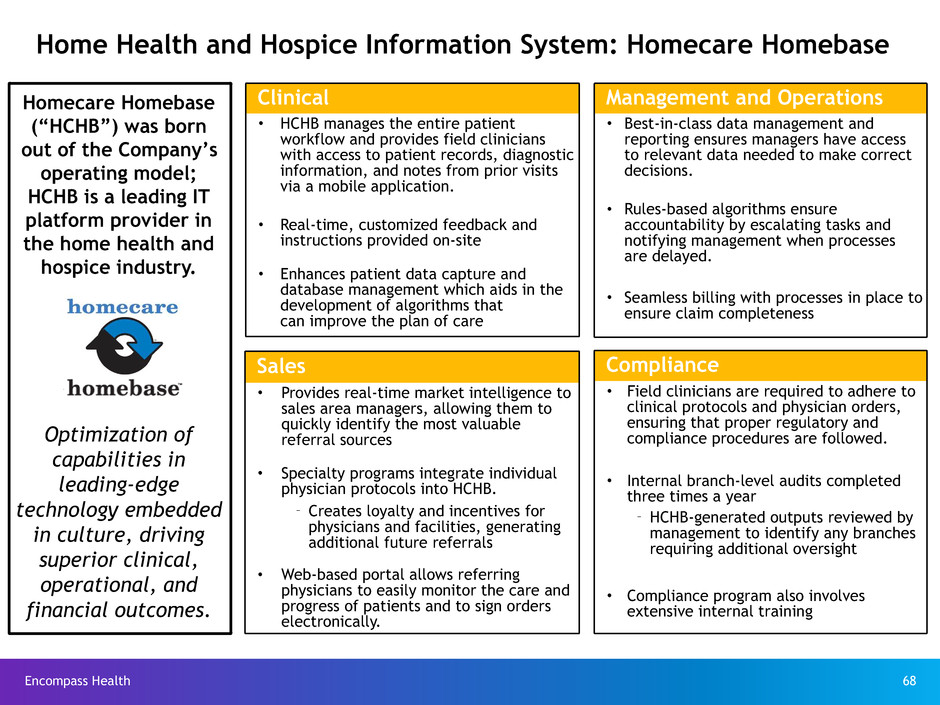
Encompass Health 68
Homecare Homebase
(“HCHB”) was born
out of the Company’s
operating model;
HCHB is a leading IT
platform provider in
the home health and
hospice industry.
Optimization of
capabilities in
leading-edge
technology embedded
in culture, driving
superior clinical,
operational, and
financial outcomes.
Home Health and Hospice Information System: Homecare Homebase
Clinical
• HCHB manages the entire patient
workflow and provides field clinicians
with access to patient records, diagnostic
information, and notes from prior visits
via a mobile application.
• Real-time, customized feedback and
instructions provided on-site
• Enhances patient data capture and
database management which aids in the
development of algorithms that
can improve the plan of care
Sales
• Provides real-time market intelligence to
sales area managers, allowing them to
quickly identify the most valuable
referral sources
• Specialty programs integrate individual
physician protocols into HCHB.
– Creates loyalty and incentives for
physicians and facilities, generating
additional future referrals
• Web-based portal allows referring
physicians to easily monitor the care and
progress of patients and to sign orders
electronically.
Compliance
• Field clinicians are required to adhere to
clinical protocols and physician orders,
ensuring that proper regulatory and
compliance procedures are followed.
• Internal branch-level audits completed
three times a year
– HCHB-generated outputs reviewed by
management to identify any branches
requiring additional oversight
• Compliance program also involves
extensive internal training
Management and Operations
• Best-in-class data management and
reporting ensures managers have access
to relevant data needed to make correct
decisions.
• Rules-based algorithms ensure
accountability by escalating tasks and
notifying management when processes
are delayed.
• Seamless billing with processes in place to
ensure claim completeness

Encompass Health 69
Operational Metrics
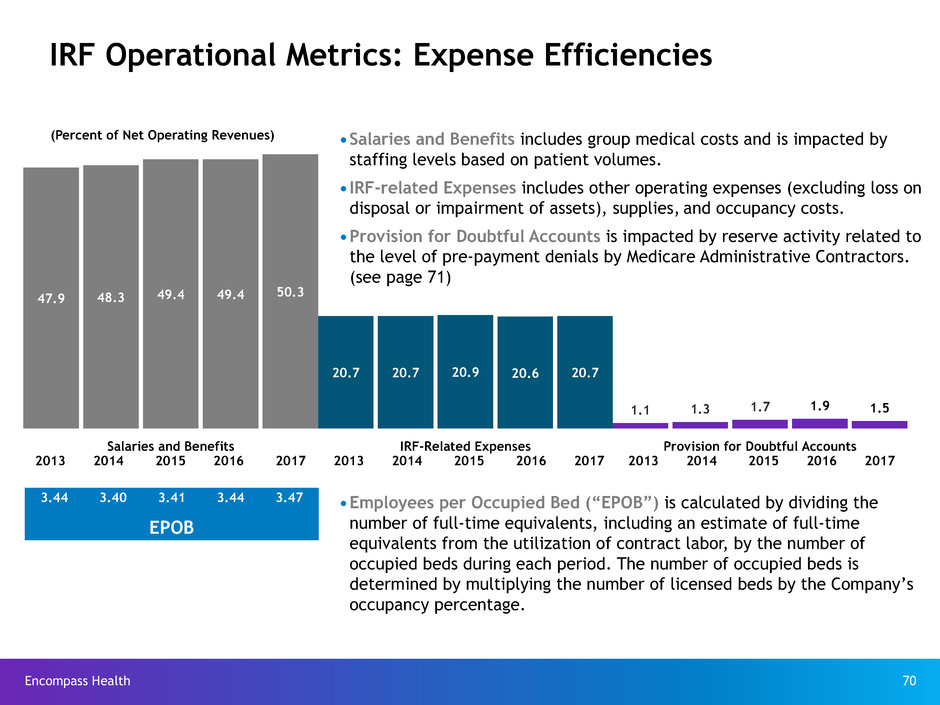
Encompass Health 70
•Salaries and Benefits includes group medical costs and is impacted by
staffing levels based on patient volumes.
•IRF-related Expenses includes other operating expenses (excluding loss on
disposal or impairment of assets), supplies, and occupancy costs.
•Provision for Doubtful Accounts is impacted by reserve activity related to
the level of pre-payment denials by Medicare Administrative Contractors.
(see page 71)
•Employees per Occupied Bed (“EPOB”) is calculated by dividing the
number of full-time equivalents, including an estimate of full-time
equivalents from the utilization of contract labor, by the number of
occupied beds during each period. The number of occupied beds is
determined by multiplying the number of licensed beds by the Company’s
occupancy percentage.
Salaries and Benefits IRF-Related Expenses Provision for Doubtful Accounts
47.9
20.7
1.1
48.3
20.7
1.3
49.4
20.9
1.7
49.4
20.6
1.9
50.3
20.7
1.5
IRF Operational Metrics: Expense Efficiencies
3.44 3.40 3.41 3.44 3.47
EPOB
(Percent of Net Operating Revenues)
2013 2014 2015 2016 2017 2013 2014 2015 2016 2017 2013 2014 2015 2016 2017
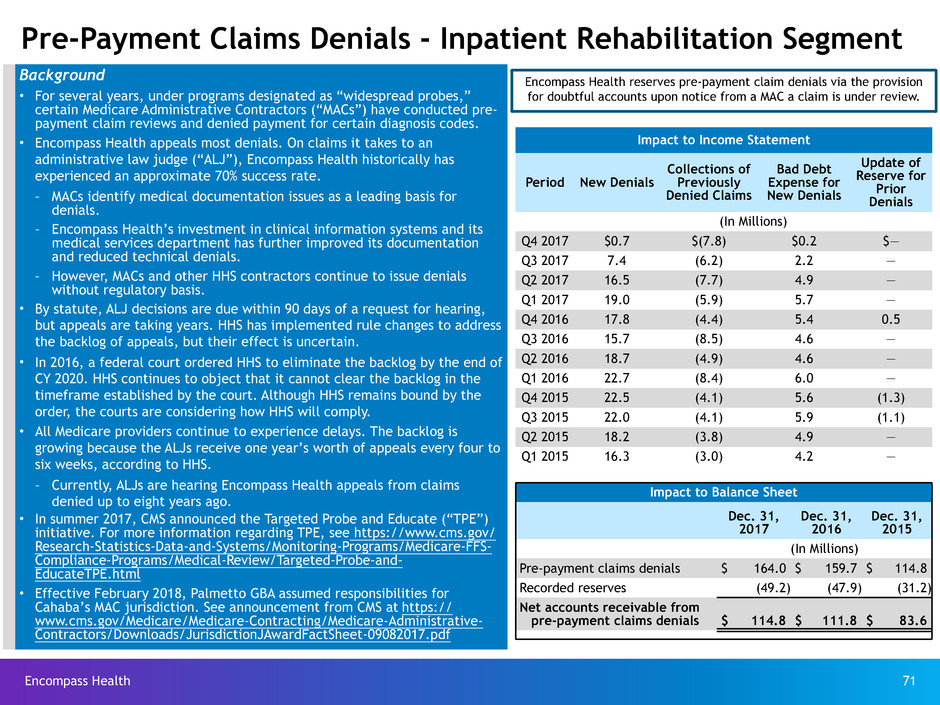
Encompass Health 71
Pre-Payment Claims Denials - Inpatient Rehabilitation Segment
Impact to Income Statement
Period New Denials
Collections of
Previously
Denied Claims
Bad Debt
Expense for
New Denials
Update of
Reserve for
Prior
Denials
(In Millions)
Q4 2017 $0.7 $(7.8) $0.2 $—
Q3 2017 7.4 (6.2) 2.2 —
Q2 2017 16.5 (7.7) 4.9 —
Q1 2017 19.0 (5.9) 5.7 —
Q4 2016 17.8 (4.4) 5.4 0.5
Q3 2016 15.7 (8.5) 4.6 —
Q2 2016 18.7 (4.9) 4.6 —
Q1 2016 22.7 (8.4) 6.0 —
Q4 2015 22.5 (4.1) 5.6 (1.3)
Q3 2015 22.0 (4.1) 5.9 (1.1)
Q2 2015 18.2 (3.8) 4.9 —
Q1 2015 16.3 (3.0) 4.2 —
Impact to Balance Sheet
Dec. 31,
2017
Dec. 31,
2016
Dec. 31,
2015
(In Millions)
Pre-payment claims denials $ 164.0 $ 159.7 $ 114.8
Recorded reserves (49.2) (47.9) (31.2)
Net accounts receivable from
pre-payment claims denials $ 114.8 $ 111.8 $ 83.6
Background
• For several years, under programs designated as “widespread probes,”
certain Medicare Administrative Contractors (“MACs”) have conducted pre-
payment claim reviews and denied payment for certain diagnosis codes.
• Encompass Health appeals most denials. On claims it takes to an
administrative law judge (“ALJ”), Encompass Health historically has
experienced an approximate 70% success rate.
– MACs identify medical documentation issues as a leading basis for
denials.
– Encompass Health’s investment in clinical information systems and its
medical services department has further improved its documentation
and reduced technical denials.
– However, MACs and other HHS contractors continue to issue denials
without regulatory basis.
• By statute, ALJ decisions are due within 90 days of a request for hearing,
but appeals are taking years. HHS has implemented rule changes to address
the backlog of appeals, but their effect is uncertain.
• In 2016, a federal court ordered HHS to eliminate the backlog by the end of
CY 2020. HHS continues to object that it cannot clear the backlog in the
timeframe established by the court. Although HHS remains bound by the
order, the courts are considering how HHS will comply.
• All Medicare providers continue to experience delays. The backlog is
growing because the ALJs receive one year’s worth of appeals every four to
six weeks, according to HHS.
– Currently, ALJs are hearing Encompass Health appeals from claims
denied up to eight years ago.
• In summer 2017, CMS announced the Targeted Probe and Educate (“TPE”)
initiative. For more information regarding TPE, see https://www.cms.gov/
Research-Statistics-Data-and-Systems/Monitoring-Programs/Medicare-FFS-
Compliance-Programs/Medical-Review/Targeted-Probe-and-
EducateTPE.html
• Effective February 2018, Palmetto GBA assumed responsibilities for
Cahaba’s MAC jurisdiction. See announcement from CMS at https://
www.cms.gov/Medicare/Medicare-Contracting/Medicare-Administrative-
Contractors/Downloads/JurisdictionJAwardFactSheet-09082017.pdf
Encompass Health reserves pre-payment claim denials via the provision
for doubtful accounts upon notice from a MAC a claim is under review.
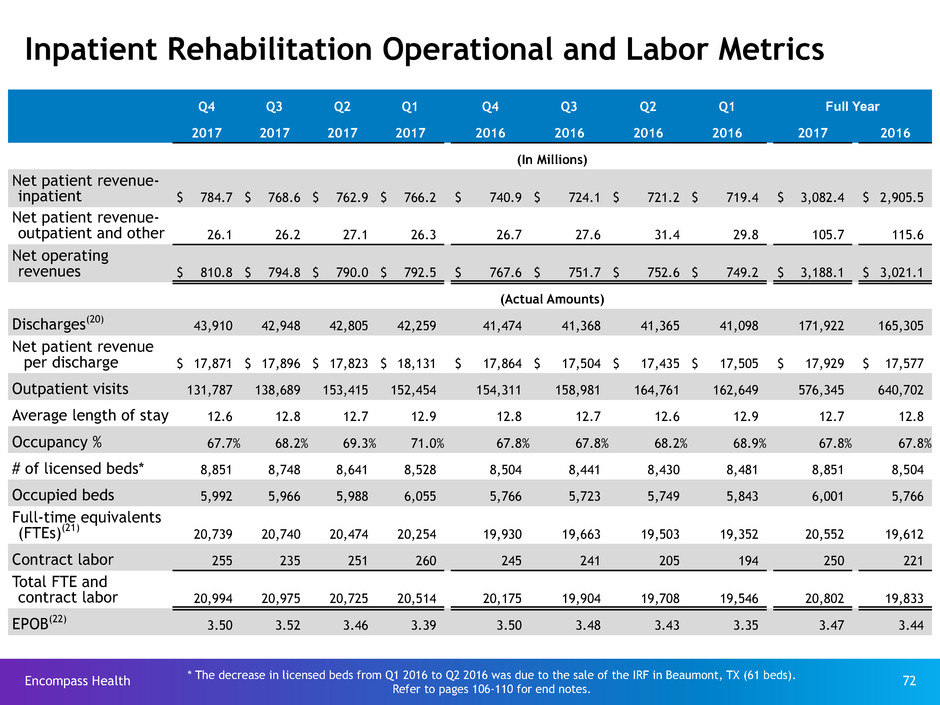
Encompass Health 72
Inpatient Rehabilitation Operational and Labor Metrics
Q4 Q3 Q2 Q1 Q4 Q3 Q2 Q1 Full Year
2017 2017 2017 2017 2016 2016 2016 2016 2017 2016
(In Millions)
Net patient revenue-
inpatient $ 784.7 $ 768.6 $ 762.9 $ 766.2 $ 740.9 $ 724.1 $ 721.2 $ 719.4 $ 3,082.4 $ 2,905.5
Net patient revenue-
outpatient and other
revenues
26.1 26.2 27.1 26.3 26.7 27.6 31.4 29.8 105.7 115.6
Net operating
revenues $ 810.8 $ 794.8 $ 790.0 $ 792.5 $ 767.6 $ 751.7 $ 752.6 $ 749.2 $ 3,188.1 $ 3,021.1
(Actual Amounts)
Discharges(20) 43,910 42,948 42,805 42,259 41,474 41,368 41,365 41,098 171,922 165,305
Net patient revenue
per discharge $ 17,871 $ 17,896 $ 17,823 $ 18,131 $ 17,864 $ 17,504 $ 17,435 $ 17,505 $ 17,929 $ 17,577
Outpatient visits 131,787 138,689 153,415 152,454 154,311 158,981 164,761 162,649 576,345 640,702
Average length of stay 12.6 12.8 12.7 12.9 12.8 12.7 12.6 12.9 12.7 12.8
Occupancy % 67.7% 68.2% 69.3% 71.0% 67.8% 67.8% 68.2% 68.9% 67.8% 67.8%
# of licensed beds* 8,851 8,748 8,641 8,528 8,504 8,441 8,430 8,481 8,851 8,504
Occupied beds 5,992 5,966 5,988 6,055 5,766 5,723 5,749 5,843 6,001 5,766
Full-time equivalents
(FTEs)(21) 20,739 20,740 20,474 20,254 19,930 19,663 19,503 19,352 20,552 19,612
Contract labor 255 235 251 260 245 241 205 194 250 221
Total FTE and
contract labor 20,994 20,975 20,725 20,514 20,175 19,904 19,708 19,546 20,802 19,833
EPOB(22) 3.50 3.52 3.46 3.39 3.50 3.48 3.43 3.35 3.47 3.44
* The decrease in licensed beds from Q1 2016 to Q2 2016 was due to the sale of the IRF in Beaumont, TX (61 beds).
Refer to pages 106-110 for end notes.
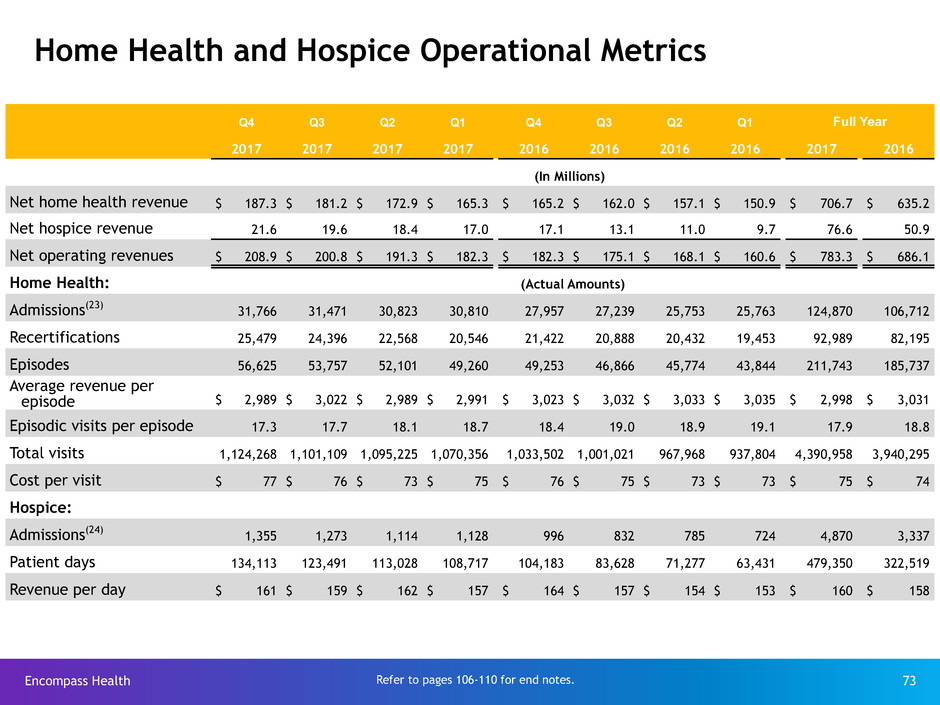
Encompass Health 73Refer to pages 106-110 for end notes.
Home Health and Hospice Operational Metrics
Q4 Q3 Q2 Q1 Q4 Q3 Q2 Q1 Full Year
2017 2017 2017 2017 2016 2016 2016 2016 2017 2016
(In Millions)
Net home health revenue $ 187.3 $ 181.2 $ 172.9 $ 165.3 $ 165.2 $ 162.0 $ 157.1 $ 150.9 $ 706.7 $ 635.2
Net hospice revenue 21.6 19.6 18.4 17.0 17.1 13.1 11.0 9.7 76.6 50.9
Net operating revenues $ 208.9 $ 200.8 $ 191.3 $ 182.3 $ 182.3 $ 175.1 $ 168.1 $ 160.6 $ 783.3 $ 686.1
Home Health: (Actual Amounts)
Admissions(23) 31,766 31,471 30,823 30,810 27,957 27,239 25,753 25,763 124,870 106,712
Recertifications 25,479 24,396 22,568 20,546 21,422 20,888 20,432 19,453 92,989 82,195
Episodes 56,625 53,757 52,101 49,260 49,253 46,866 45,774 43,844 211,743 185,737
Average revenue per
episode $ 2,989 $ 3,022 $ 2,989 $ 2,991 $ 3,023 $ 3,032 $ 3,033 $ 3,035 $ 2,998 $ 3,031
Episodic visits per episode 17.3 17.7 18.1 18.7 18.4 19.0 18.9 19.1 17.9 18.8
Total visits 1,124,268 1,101,109 1,095,225 1,070,356 1,033,502 1,001,021 967,968 937,804 4,390,958 3,940,295
Cost per visit $ 77 $ 76 $ 73 $ 75 $ 76 $ 75 $ 73 $ 73 $ 75 $ 74
Hospice:
Admissions(24) 1,355 1,273 1,114 1,128 996 832 785 724 4,870 3,337
Patient days 134,113 123,491 113,028 108,717 104,183 83,628 71,277 63,431 479,350 322,519
Revenue per day $ 161 $ 159 $ 162 $ 157 $ 164 $ 157 $ 154 $ 153 $ 160 $ 158
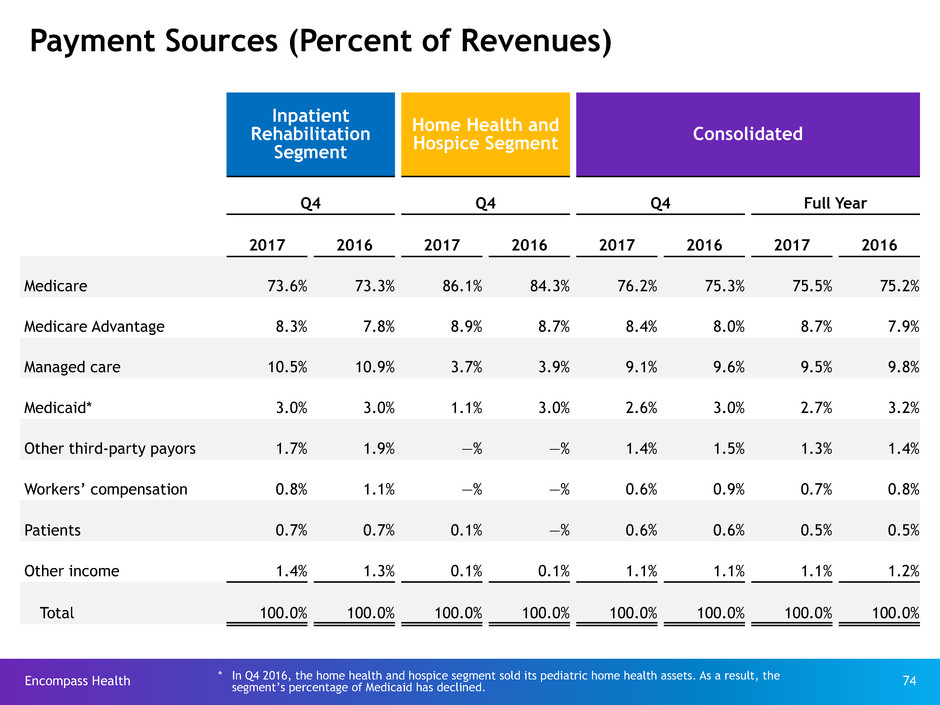
Encompass Health 74
Payment Sources (Percent of Revenues)
Inpatient
Rehabilitation
Segment
Home Health and
Hospice Segment Consolidated
Q4 Q4 Q4 Full Year
2017 2016 2017 2016 2017 2016 2017 2016
Medicare 73.6% 73.3% 86.1% 84.3% 76.2% 75.3% 75.5% 75.2%
Medicare Advantage 8.3% 7.8% 8.9% 8.7% 8.4% 8.0% 8.7% 7.9%
Managed care 10.5% 10.9% 3.7% 3.9% 9.1% 9.6% 9.5% 9.8%
Medicaid* 3.0% 3.0% 1.1% 3.0% 2.6% 3.0% 2.7% 3.2%
Other third-party payors 1.7% 1.9% —% —% 1.4% 1.5% 1.3% 1.4%
Workers’ compensation 0.8% 1.1% —% —% 0.6% 0.9% 0.7% 0.8%
Patients 0.7% 0.7% 0.1% —% 0.6% 0.6% 0.5% 0.5%
Other income 1.4% 1.3% 0.1% 0.1% 1.1% 1.1% 1.1% 1.2%
Total 100.0% 100.0% 100.0% 100.0% 100.0% 100.0% 100.0% 100.0%
* In Q4 2016, the home health and hospice segment sold its pediatric home health assets. As a result, the
segment’s percentage of Medicaid has declined.

Encompass Health 75
Industry Structure
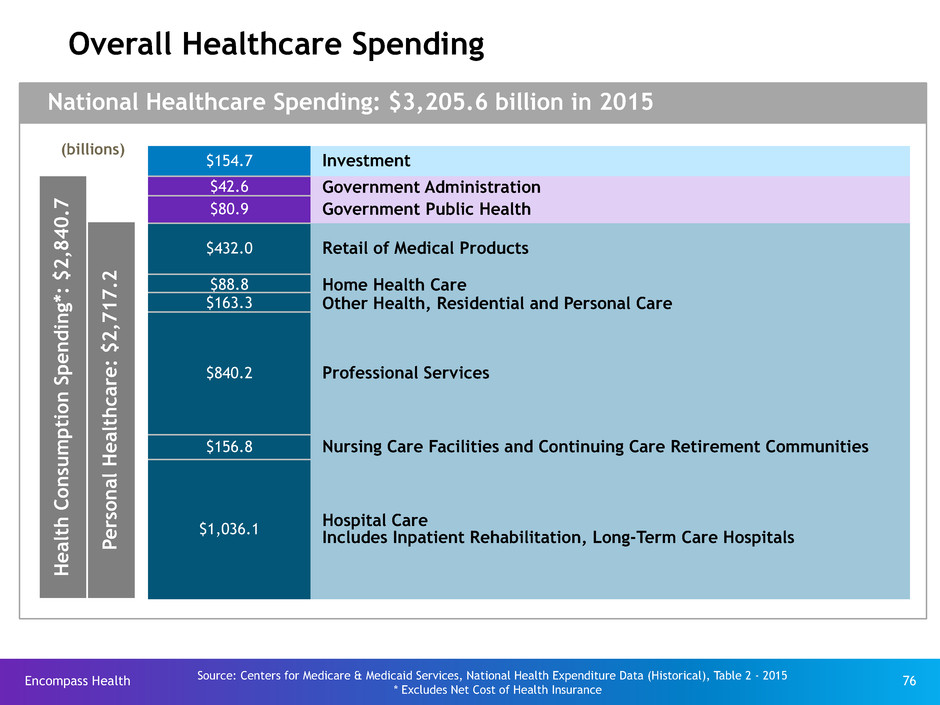
Encompass Health 76
Health Consumption Spending*: $2,840.
7
Overall Healthcare Spending
(billions)
Source: Centers for Medicare & Medicaid Services, National Health Expenditure Data (Historical), Table 2 - 2015
* Excludes Net Cost of Health Insurance
National Healthcare Spending: $3,205.6 billion in 2015
Personal Healthcare: $2,717.
2
$154.7 Investment
$42.6 Government Administration
$80.9 Government Public Health
$432.0 Retail of Medical Products
$88.8 Home Health Care
$163.3 Other Health, Residential and Personal Care
$840.2 Professional Services
$156.8 Nursing Care Facilities and Continuing Care Retirement Communities
$1,036.1 Hospital CareIncludes Inpatient Rehabilitation, Long-Term Care Hospitals
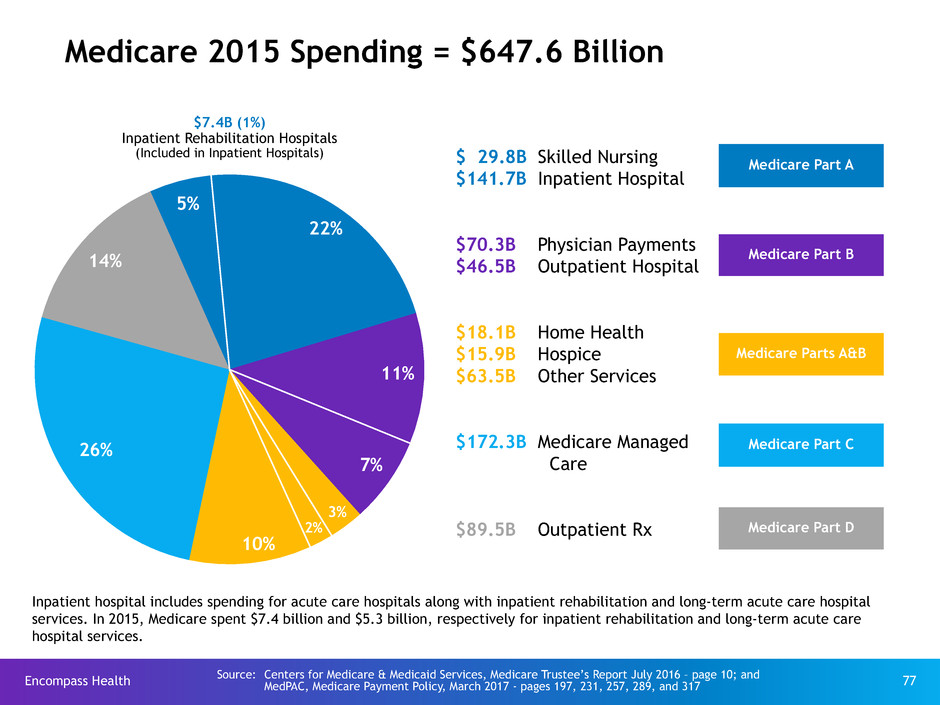
Encompass Health 77Source: Centers for Medicare & Medicaid Services, Medicare Trustee’s Report July 2016 – page 10; and MedPAC, Medicare Payment Policy, March 2017 - pages 197, 231, 257, 289, and 317
Medicare 2015 Spending = $647.6 Billion
$ 29.8B Skilled Nursing
$141.7B Inpatient Hospital
$70.3B Physician Payments
$46.5B Outpatient Hospital
$18.1B Home Health
$15.9B Hospice
$63.5B Other Services
$172.3B Medicare Managed
Care
$89.5B Outpatient Rx
$7.4B (1%)
Inpatient Rehabilitation Hospitals
(Included in Inpatient Hospitals)
14%
3%
7%
10%
11%
26%
22%
Medicare Part A
Medicare Part B
Medicare Parts A&B
Medicare Part C
Medicare Part D
5%
Inpatient hospital includes spending for acute care hospitals along with inpatient rehabilitation and long-term acute care hospital
services. In 2015, Medicare spent $7.4 billion and $5.3 billion, respectively for inpatient rehabilitation and long-term acute care
hospital services.
2%
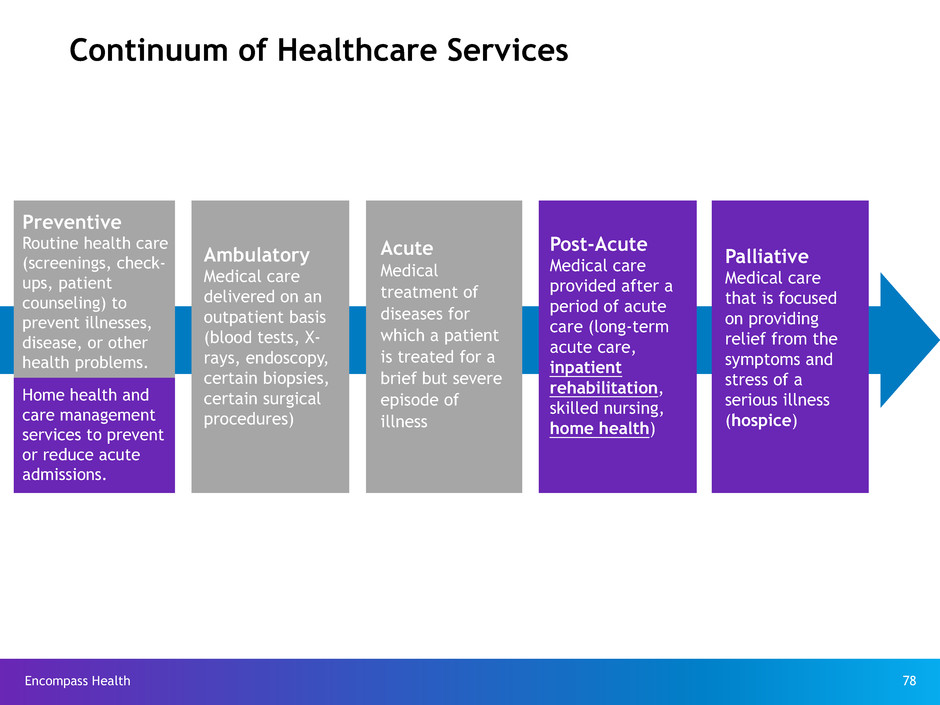
Encompass Health 78
Preventive
Routine health care
(screenings, check-
ups, patient
counseling) to
prevent illnesses,
disease, or other
health problems.
Home health and
care management
services to prevent
or reduce acute
admissions.
Continuum of Healthcare Services
Acute
Medical
treatment of
diseases for
which a patient
is treated for a
brief but severe
episode of
illness
Ambulatory
Medical care
delivered on an
outpatient basis
(blood tests, X-
rays, endoscopy,
certain biopsies,
certain surgical
procedures)
Post-Acute
Medical care
provided after a
period of acute
care (long-term
acute care,
inpatient
rehabilitation,
skilled nursing,
home health)
Palliative
Medical care
that is focused
on providing
relief from the
symptoms and
stress of a
serious illness
(hospice)
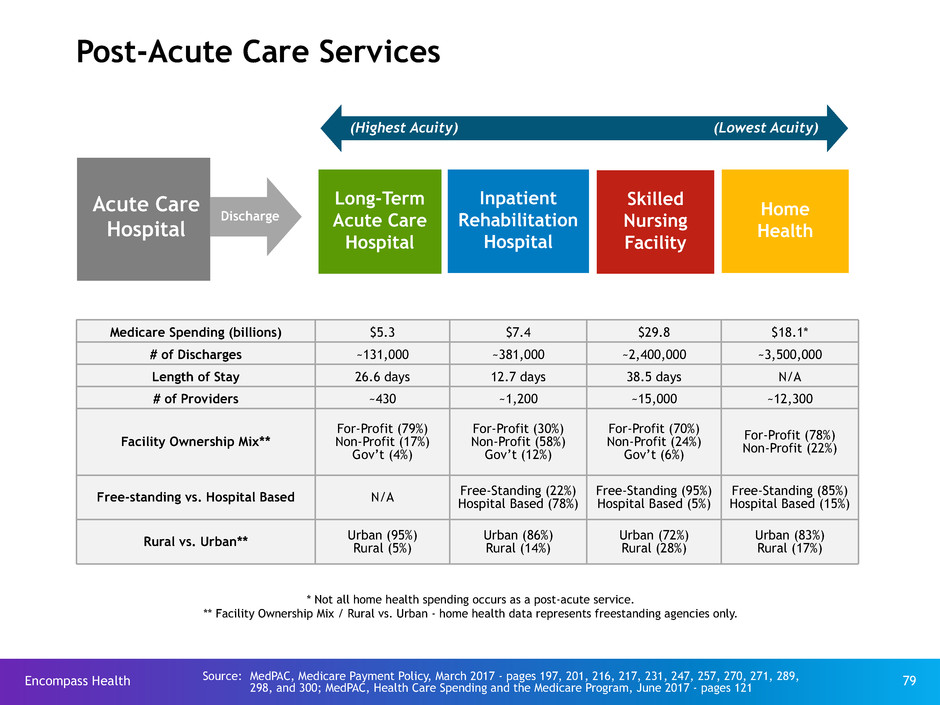
Encompass Health 79
Post-Acute Care Services
Acute Care
Hospital
Home
Health
Long-Term
Acute Care
Hospital
Inpatient
Rehabilitation
Hospital
Skilled
Nursing
Facility
Discharge
Medicare Spending (billions) $5.3 $7.4 $29.8 $18.1*
# of Discharges ~131,000 ~381,000 ~2,400,000 ~3,500,000
Length of Stay 26.6 days 12.7 days 38.5 days N/A
# of Providers ~430 ~1,200 ~15,000 ~12,300
Facility Ownership Mix**
For-Profit (79%)
Non-Profit (17%)
Gov’t (4%)
For-Profit (30%)
Non-Profit (58%)
Gov’t (12%)
For-Profit (70%)
Non-Profit (24%)
Gov’t (6%)
For-Profit (78%)
Non-Profit (22%)
Free-standing vs. Hospital Based N/A Free-Standing (22%)Hospital Based (78%)
Free-Standing (95%)
Hospital Based (5%)
Free-Standing (85%)
Hospital Based (15%)
Rural vs. Urban** Urban (95%)Rural (5%)
Urban (86%)
Rural (14%)
Urban (72%)
Rural (28%)
Urban (83%)
Rural (17%)
(Lowest Acuity)(Highest Acuity)
Source: MedPAC, Medicare Payment Policy, March 2017 - pages 197, 201, 216, 217, 231, 247, 257, 270, 271, 289,
298, and 300; MedPAC, Health Care Spending and the Medicare Program, June 2017 - pages 121
* Not all home health spending occurs as a post-acute service.
** Facility Ownership Mix / Rural vs. Urban - home health data represents freestanding agencies only.
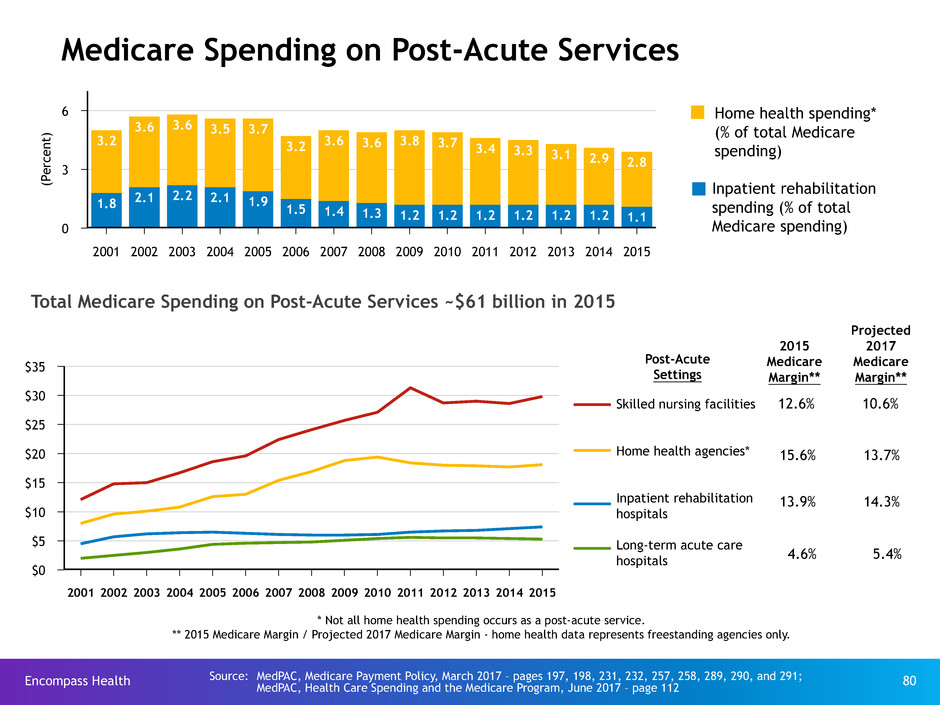
Encompass Health 80
$35
$30
$25
$20
$15
$10
$5
$0
2001 2002 2003 2004 2005 2006 2007 2008 2009 2010 2011 2012 2013 2014 2015
Medicare Spending on Post-Acute Services
Post-Acute
Settings
2015
Medicare
Margin**
Projected
2017
Medicare
Margin**
12.6% 10.6%
15.6% 13.7%
13.9% 14.3%
4.6% 5.4%
Skilled nursing facilities
Home health agencies*
Inpatient rehabilitation
hospitals
Long-term acute care
hospitals
Inpatient rehabilitation
spending (% of total
Medicare spending)
6
3
0
(P
er
ce
nt
)
2001 2002 2003 2004 2005 2006 2007 2008 2009 2010 2011 2012 2013 2014 2015
1.8 2.1 2.2 2.1 1.9 1.5 1.4 1.3 1.2 1.2 1.2 1.2 1.2 1.2 1.1
3.2
3.6 3.6 3.5 3.7
3.2 3.6 3.6 3.8 3.7 3.4 3.3 3.1 2.9 2.8
Home health spending*
(% of total Medicare
spending)
Total Medicare Spending on Post-Acute Services ~$61 billion in 2015
Source: MedPAC, Medicare Payment Policy, March 2017 – pages 197, 198, 231, 232, 257, 258, 289, 290, and 291;
MedPAC, Health Care Spending and the Medicare Program, June 2017 – page 112
* Not all home health spending occurs as a post-acute service.
** 2015 Medicare Margin / Projected 2017 Medicare Margin - home health data represents freestanding agencies only.
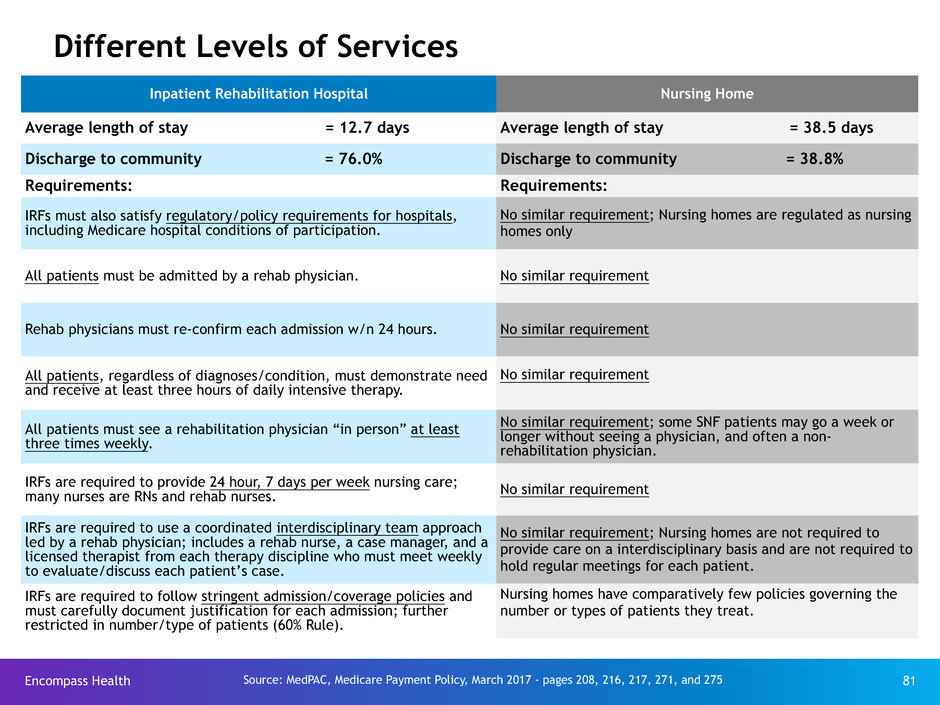
Encompass Health 81
Different Levels of Services
Inpatient Rehabilitation Hospital Nursing Home
Average length of stay = 12.7 days Average length of stay = 38.5 days
Discharge to community = 76.0% Discharge to community = 38.8%
Requirements: Requirements:
IRFs must also satisfy regulatory/policy requirements for hospitals,
including Medicare hospital conditions of participation.
No similar requirement; Nursing homes are regulated as nursing
homes only
All patients must be admitted by a rehab physician. No similar requirement
Rehab physicians must re-confirm each admission w/n 24 hours. No similar requirement
All patients, regardless of diagnoses/condition, must demonstrate need
and receive at least three hours of daily intensive therapy.
No similar requirement
All patients must see a rehabilitation physician “in person” at least
three times weekly.
No similar requirement; some SNF patients may go a week or
longer without seeing a physician, and often a non-
rehabilitation physician.
IRFs are required to provide 24 hour, 7 days per week nursing care;
many nurses are RNs and rehab nurses. No similar requirement
IRFs are required to use a coordinated interdisciplinary team approach
led by a rehab physician; includes a rehab nurse, a case manager, and a
licensed therapist from each therapy discipline who must meet weekly
to evaluate/discuss each patient’s case.
No similar requirement; Nursing homes are not required to
provide care on a interdisciplinary basis and are not required to
hold regular meetings for each patient.
IRFs are required to follow stringent admission/coverage policies and
must carefully document justification for each admission; further
restricted in number/type of patients (60% Rule).
Nursing homes have comparatively few policies governing the
number or types of patients they treat.
Source: MedPAC, Medicare Payment Policy, March 2017 - pages 208, 216, 217, 271, and 275
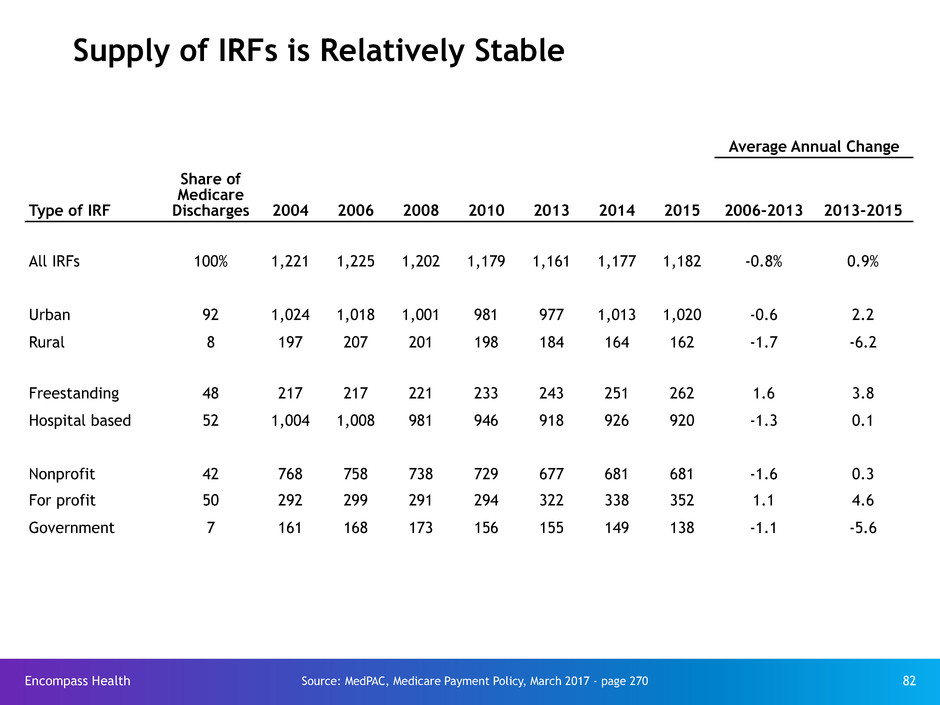
Encompass Health 82
Supply of IRFs is Relatively Stable
Average Annual Change
Share of
Medicare
DischargesType of IRF 2004 2006 2008 2010 2013 2014 2015 2006-2013 2013-2015
All IRFs 100% 1,221 1,225 1,202 1,179 1,161 1,177 1,182 -0.8% 0.9%
Urban 92 1,024 1,018 1,001 981 977 1,013 1,020 -0.6 2.2
Rural 8 197 207 201 198 184 164 162 -1.7 -6.2
Freestanding 48 217 217 221 233 243 251 262 1.6 3.8
Hospital based 52 1,004 1,008 981 946 918 926 920 -1.3 0.1
Nonprofit 42 768 758 738 729 677 681 681 -1.6 0.3
For profit 50 292 299 291 294 322 338 352 1.1 4.6
Government 7 161 168 173 156 155 149 138 -1.1 -5.6
Source: MedPAC, Medicare Payment Policy, March 2017 - page 270
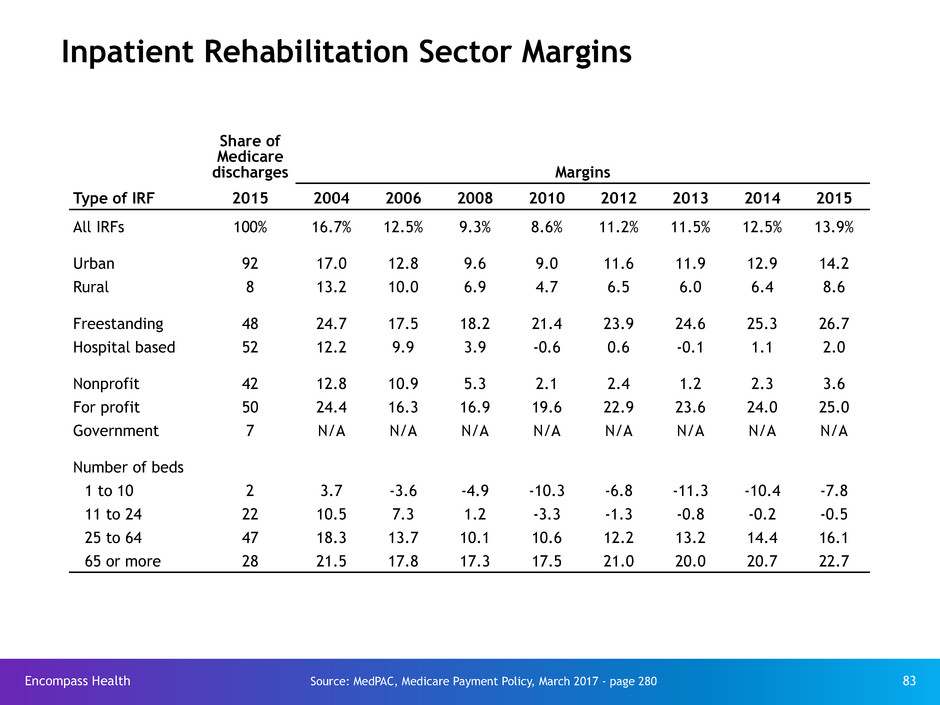
Encompass Health 83
Inpatient Rehabilitation Sector Margins
Share of
Medicare
discharges Margins
Type of IRF 2015 2004 2006 2008 2010 2012 2013 2014 2015
All IRFs 100% 16.7% 12.5% 9.3% 8.6% 11.2% 11.5% 12.5% 13.9%
Urban 92 17.0 12.8 9.6 9.0 11.6 11.9 12.9 14.2
Rural 8 13.2 10.0 6.9 4.7 6.5 6.0 6.4 8.6
Freestanding 48 24.7 17.5 18.2 21.4 23.9 24.6 25.3 26.7
Hospital based 52 12.2 9.9 3.9 -0.6 0.6 -0.1 1.1 2.0
Nonprofit 42 12.8 10.9 5.3 2.1 2.4 1.2 2.3 3.6
For profit 50 24.4 16.3 16.9 19.6 22.9 23.6 24.0 25.0
Government 7 N/A N/A N/A N/A N/A N/A N/A N/A
Number of beds
1 to 10 2 3.7 -3.6 -4.9 -10.3 -6.8 -11.3 -10.4 -7.8
11 to 24 22 10.5 7.3 1.2 -3.3 -1.3 -0.8 -0.2 -0.5
25 to 64 47 18.3 13.7 10.1 10.6 12.2 13.2 14.4 16.1
65 or more 28 21.5 17.8 17.3 17.5 21.0 20.0 20.7 22.7
Source: MedPAC, Medicare Payment Policy, March 2017 - page 280
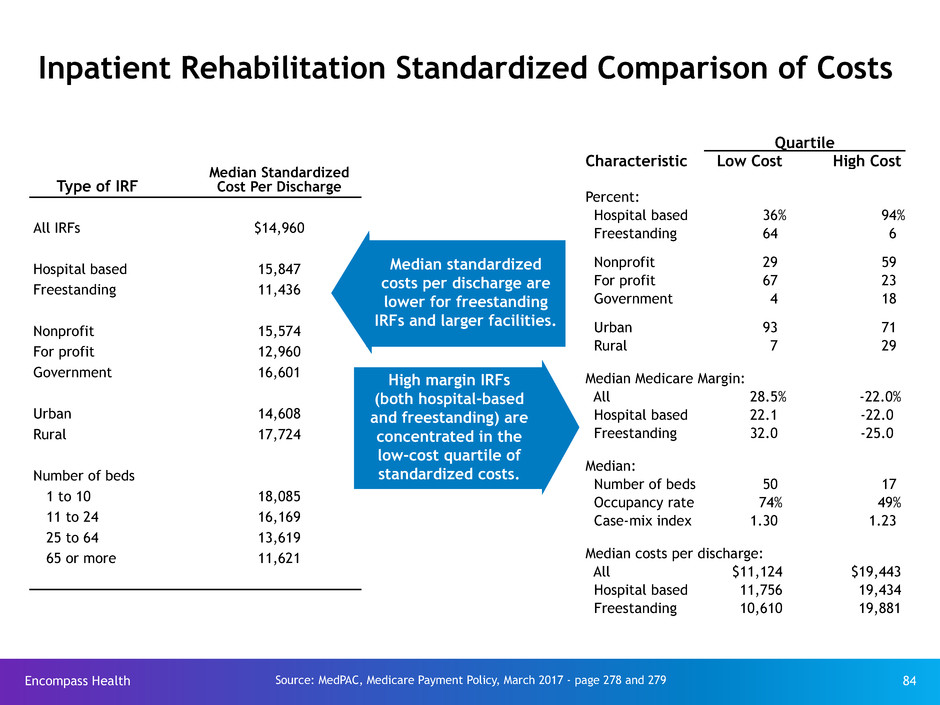
Encompass Health 84
Inpatient Rehabilitation Standardized Comparison of Costs
Type of IRF
Median Standardized
Cost Per Discharge
All IRFs $14,960
Hospital based 15,847
Freestanding 11,436
Nonprofit 15,574
For profit 12,960
Government 16,601
Urban 14,608
Rural 17,724
Number of beds
1 to 10 18,085
11 to 24 16,169
25 to 64 13,619
65 or more 11,621
Quartile
Characteristic Low Cost High Cost
Percent:
Hospital based 36% 94%
Freestanding 64 6
Nonprofit 29 59
For profit 67 23
Government 4 18
Urban 93 71
Rural 7 29
Median Medicare Margin:
All 28.5% -22.0%
Hospital based 22.1 -22.0
Freestanding 32.0 -25.0
Median:
Number of beds 50 17
Occupancy rate 74% 49%
Case-mix index 1.30 1.23
Median costs per discharge:
All $11,124 $19,443
Hospital based 11,756 19,434
Freestanding 10,610 19,881
Median standardized
costs per discharge are
lower for freestanding
IRFs and larger facilities.
High margin IRFs
(both hospital-based
and freestanding) are
concentrated in the
low-cost quartile of
standardized costs.
Source: MedPAC, Medicare Payment Policy, March 2017 - page 278 and 279
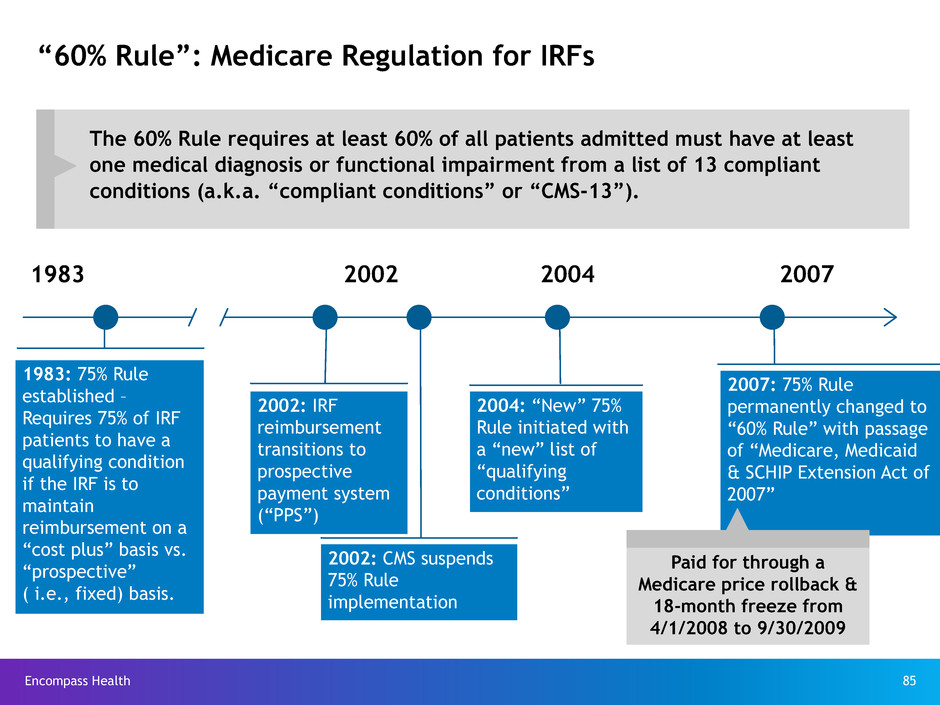
Encompass Health 85
“60% Rule”: Medicare Regulation for IRFs
1983
1983: 75% Rule
established –
Requires 75% of IRF
patients to have a
qualifying condition
if the IRF is to
maintain
reimbursement on a
“cost plus” basis vs.
“prospective”
( i.e., fixed) basis.
2002 2004 2007
2002: IRF
reimbursement
transitions to
prospective
payment system
(“PPS”)
2002: CMS suspends
75% Rule
implementation
2004: “New” 75%
Rule initiated with
a “new” list of
“qualifying
conditions”
2007: 75% Rule
permanently changed to
“60% Rule” with passage
of “Medicare, Medicaid
& SCHIP Extension Act of
2007”
Paid for through a
Medicare price rollback &
18-month freeze from
4/1/2008 to 9/30/2009
The 60% Rule requires at least 60% of all patients admitted must have at least
one medical diagnosis or functional impairment from a list of 13 compliant
conditions (a.k.a. “compliant conditions” or “CMS-13”).
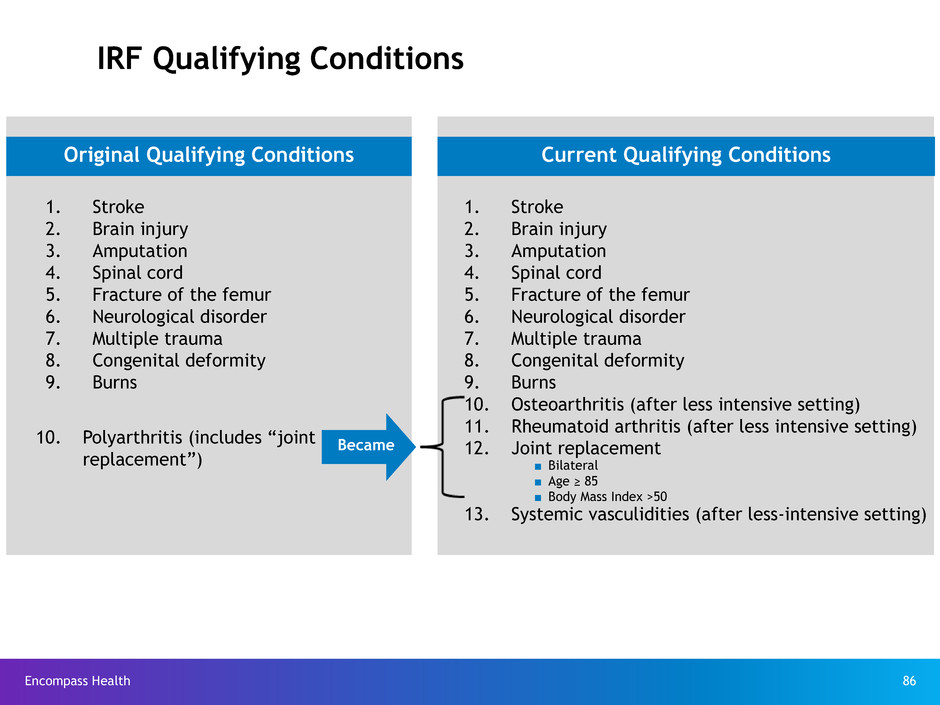

Encompass Health 86
1. Stroke
2. Brain injury
3. Amputation
4. Spinal cord
5. Fracture of the femur
6. Neurological disorder
7. Multiple trauma
8. Congenital deformity
9. Burns
IRF Qualifying Conditions
1. Stroke
2. Brain injury
3. Amputation
4. Spinal cord
5. Fracture of the femur
6. Neurological disorder
7. Multiple trauma
8. Congenital deformity
9. Burns
10. Osteoarthritis (after less intensive setting)
11. Rheumatoid arthritis (after less intensive setting)
12. Joint replacement
13. Systemic vasculidities (after less-intensive setting)
Original Qualifying Conditions Current Qualifying Conditions
■ Bilateral
■ Age ≥ 85
■ Body Mass Index >50
10. Polyarthritis (includes “joint
replacement”)
Became
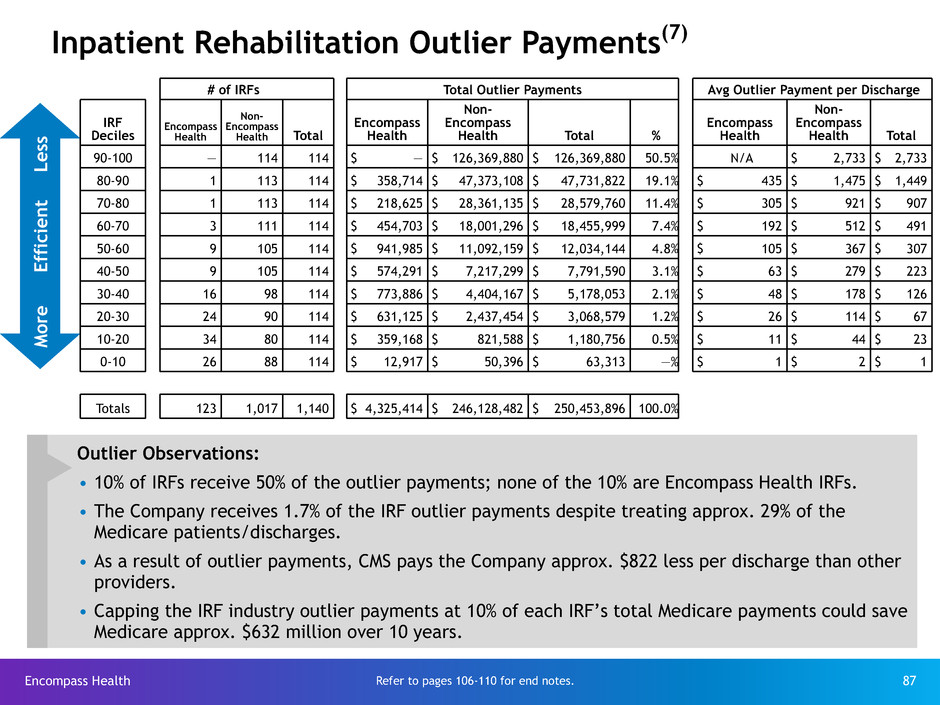

Encompass Health 87
Inpatient Rehabilitation Outlier Payments(7)
Refer to pages 106-110 for end notes.
More Efficient Less
Outlier Observations:
• 10% of IRFs receive 50% of the outlier payments; none of the 10% are Encompass Health IRFs.
• The Company receives 1.7% of the IRF outlier payments despite treating approx. 29% of the
Medicare patients/discharges.
• As a result of outlier payments, CMS pays the Company approx. $822 less per discharge than other
providers.
• Capping the IRF industry outlier payments at 10% of each IRF’s total Medicare payments could save
Medicare approx. $632 million over 10 years.
# of IRFs Total Outlier Payments Avg Outlier Payment per Discharge
IRF
Deciles
Encompass
Health
Non-
Encompass
Health Total
Encompass
Health
Non-
Encompass
Health Total %
Encompass
Health
Non-
Encompass
Health Total
90-100 — 114 114 $ — $ 126,369,880 $ 126,369,880 50.5% N/A $ 2,733 $ 2,733
80-90 1 113 114 $ 358,714 $ 47,373,108 $ 47,731,822 19.1% $ 435 $ 1,475 $ 1,449
70-80 1 113 114 $ 218,625 $ 28,361,135 $ 28,579,760 11.4% $ 305 $ 921 $ 907
60-70 3 111 114 $ 454,703 $ 18,001,296 $ 18,455,999 7.4% $ 192 $ 512 $ 491
50-60 9 105 114 $ 941,985 $ 11,092,159 $ 12,034,144 4.8% $ 105 $ 367 $ 307
40-50 9 105 114 $ 574,291 $ 7,217,299 $ 7,791,590 3.1% $ 63 $ 279 $ 223
30-40 16 98 114 $ 773,886 $ 4,404,167 $ 5,178,053 2.1% $ 48 $ 178 $ 126
20-30 24 90 114 $ 631,125 $ 2,437,454 $ 3,068,579 1.2% $ 26 $ 114 $ 67
10-20 34 80 114 $ 359,168 $ 821,588 $ 1,180,756 0.5% $ 11 $ 44 $ 23
0-10 26 88 114 $ 12,917 $ 50,396 $ 63,313 —% $ 1 $ 2 $ 1
Totals 123 1,017 1,140 $ 4,325,414 $ 246,128,482 $ 250,453,896 100.0%

Encompass Health 88
Segment Operating Results
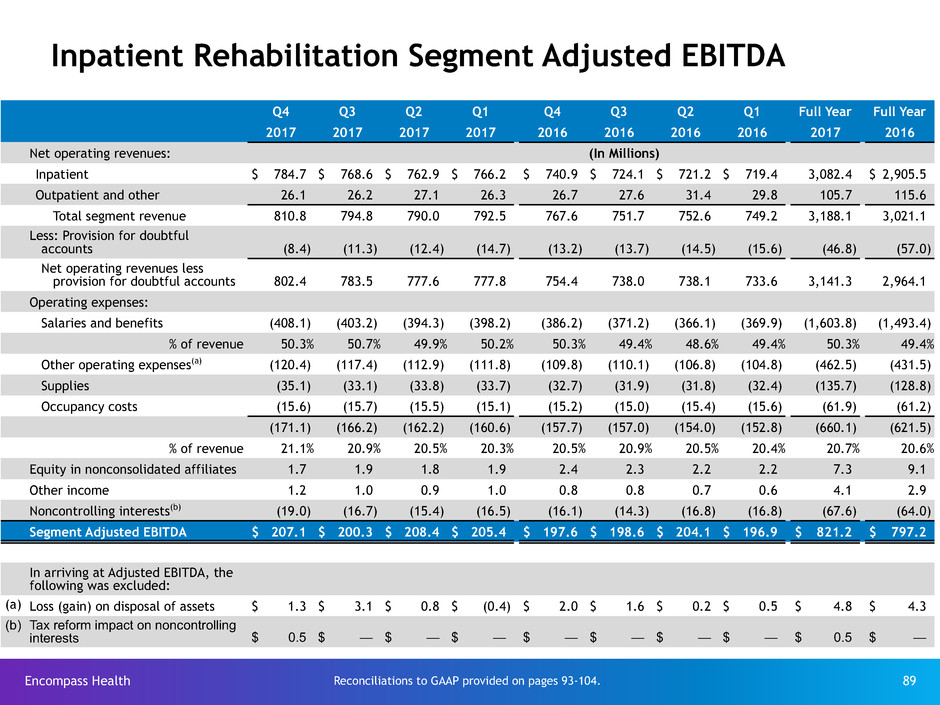
Encompass Health 89
Inpatient Rehabilitation Segment Adjusted EBITDA
Q4 Q3 Q2 Q1 Q4 Q3 Q2 Q1 Full Year Full Year
2017 2017 2017 2017 2016 2016 2016 2016 2017 2016
Net operating revenues: (In Millions)
Inpatient $ 784.7 $ 768.6 $ 762.9 $ 766.2 $ 740.9 $ 724.1 $ 721.2 $ 719.4 3,082.4 $ 2,905.5
Outpatient and other 26.1 26.2 27.1 26.3 26.7 27.6 31.4 29.8 105.7 115.6
Total segment revenue 810.8 794.8 790.0 792.5 767.6 751.7 752.6 749.2 3,188.1 3,021.1
Less: Provision for doubtful
accounts (8.4) (11.3) (12.4) (14.7) (13.2) (13.7) (14.5) (15.6) (46.8) (57.0)
Net operating revenues less
provision for doubtful accounts 802.4 783.5 777.6 777.8 754.4 738.0 738.1 733.6 3,141.3 2,964.1
Operating expenses:
Salaries and benefits (408.1) (403.2) (394.3) (398.2) (386.2) (371.2) (366.1) (369.9) (1,603.8) (1,493.4)
% of revenue 50.3% 50.7% 49.9% 50.2% 50.3% 49.4% 48.6% 49.4% 50.3% 49.4%
Other operating expenses(a) (120.4) (117.4) (112.9) (111.8) (109.8) (110.1) (106.8) (104.8) (462.5) (431.5)
Supplies (35.1) (33.1) (33.8) (33.7) (32.7) (31.9) (31.8) (32.4) (135.7) (128.8)
Occupancy costs (15.6) (15.7) (15.5) (15.1) (15.2) (15.0) (15.4) (15.6) (61.9) (61.2)
(171.1) (166.2) (162.2) (160.6) (157.7) (157.0) (154.0) (152.8) (660.1) (621.5)
% of revenue 21.1% 20.9% 20.5% 20.3% 20.5% 20.9% 20.5% 20.4% 20.7% 20.6%
Equity in nonconsolidated affiliates 1.7 1.9 1.8 1.9 2.4 2.3 2.2 2.2 7.3 9.1
Other income 1.2 1.0 0.9 1.0 0.8 0.8 0.7 0.6 4.1 2.9
Noncontrolling interests(b) (19.0) (16.7) (15.4) (16.5) (16.1) (14.3) (16.8) (16.8) (67.6) (64.0)
Segment Adjusted EBITDA $ 207.1 $ 200.3 $ 208.4 $ 205.4 $ 197.6 $ 198.6 $ 204.1 $ 196.9 $ 821.2 $ 797.2
In arriving at Adjusted EBITDA, the
following was excluded:
(a) Loss (gain) on disposal of assets $ 1.3 $ 3.1 $ 0.8 $ (0.4) $ 2.0 $ 1.6 $ 0.2 $ 0.5 $ 4.8 $ 4.3
(b) Tax reform impact on noncontrolling
interests $ 0.5 $ — $ — $ — $ — $ — $ — $ — $ 0.5 $ —
Reconciliations to GAAP provided on pages 93-104.
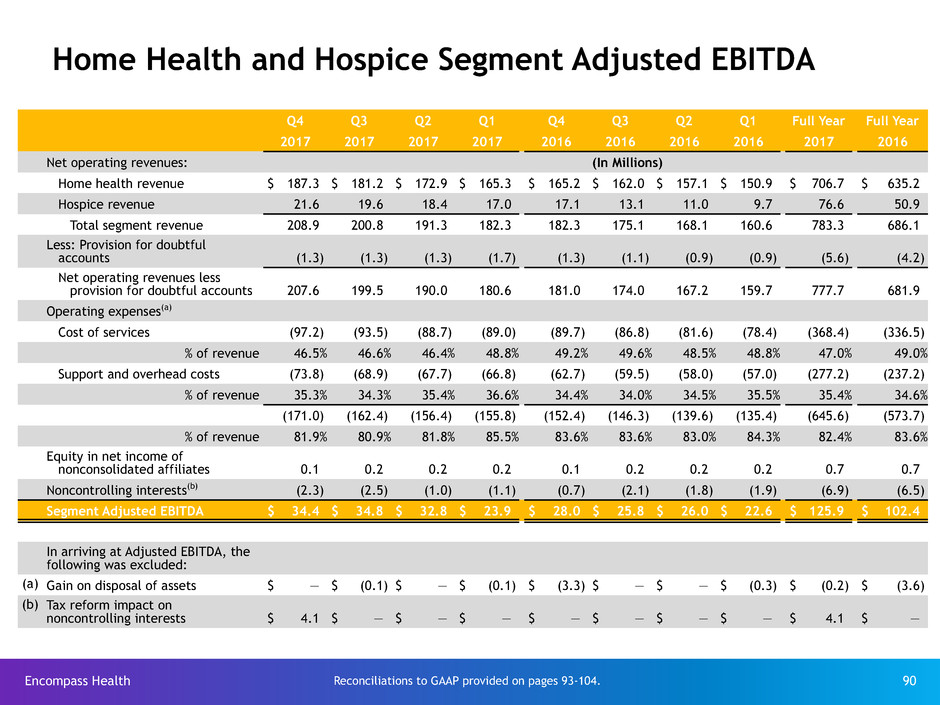
Encompass Health 90
Home Health and Hospice Segment Adjusted EBITDA
Q4 Q3 Q2 Q1 Q4 Q3 Q2 Q1 Full Year Full Year
2017 2017 2017 2017 2016 2016 2016 2016 2017 2016
Net operating revenues: (In Millions)
Home health revenue $ 187.3 $ 181.2 $ 172.9 $ 165.3 $ 165.2 $ 162.0 $ 157.1 $ 150.9 $ 706.7 $ 635.2
Hospice revenue 21.6 19.6 18.4 17.0 17.1 13.1 11.0 9.7 76.6 50.9
Total segment revenue 208.9 200.8 191.3 182.3 182.3 175.1 168.1 160.6 783.3 686.1
Less: Provision for doubtful
accounts (1.3) (1.3) (1.3) (1.7) (1.3) (1.1) (0.9) (0.9) (5.6) (4.2)
Net operating revenues less
provision for doubtful accounts 207.6 199.5 190.0 180.6 181.0 174.0 167.2 159.7 777.7 681.9
Operating expenses(a)
Cost of services (97.2) (93.5) (88.7) (89.0) (89.7) (86.8) (81.6) (78.4) (368.4) (336.5)
% of revenue 46.5% 46.6% 46.4% 48.8% 49.2% 49.6% 48.5% 48.8% 47.0% 49.0%
Support and overhead costs (73.8) (68.9) (67.7) (66.8) (62.7) (59.5) (58.0) (57.0) (277.2) (237.2)
% of revenue 35.3% 34.3% 35.4% 36.6% 34.4% 34.0% 34.5% 35.5% 35.4% 34.6%
(171.0) (162.4) (156.4) (155.8) (152.4) (146.3) (139.6) (135.4) (645.6) (573.7)
% of revenue 81.9% 80.9% 81.8% 85.5% 83.6% 83.6% 83.0% 84.3% 82.4% 83.6%
Equity in net income of
nonconsolidated affiliates 0.1 0.2 0.2 0.2 0.1 0.2 0.2 0.2 0.7 0.7
Noncontrolling interests(b) (2.3) (2.5) (1.0) (1.1) (0.7) (2.1) (1.8) (1.9) (6.9) (6.5)
Segment Adjusted EBITDA $ 34.4 $ 34.8 $ 32.8 $ 23.9 $ 28.0 $ 25.8 $ 26.0 $ 22.6 $ 125.9 $ 102.4
In arriving at Adjusted EBITDA, the
following was excluded:
(a) Gain on disposal of assets $ — $ (0.1) $ — $ (0.1) $ (3.3) $ — $ — $ (0.3) $ (0.2) $ (3.6)
(b) Tax reform impact on
noncontrolling interests $ 4.1 $ — $ — $ — $ — $ — $ — $ — $ 4.1 $ —
Reconciliations to GAAP provided on pages 93-104.
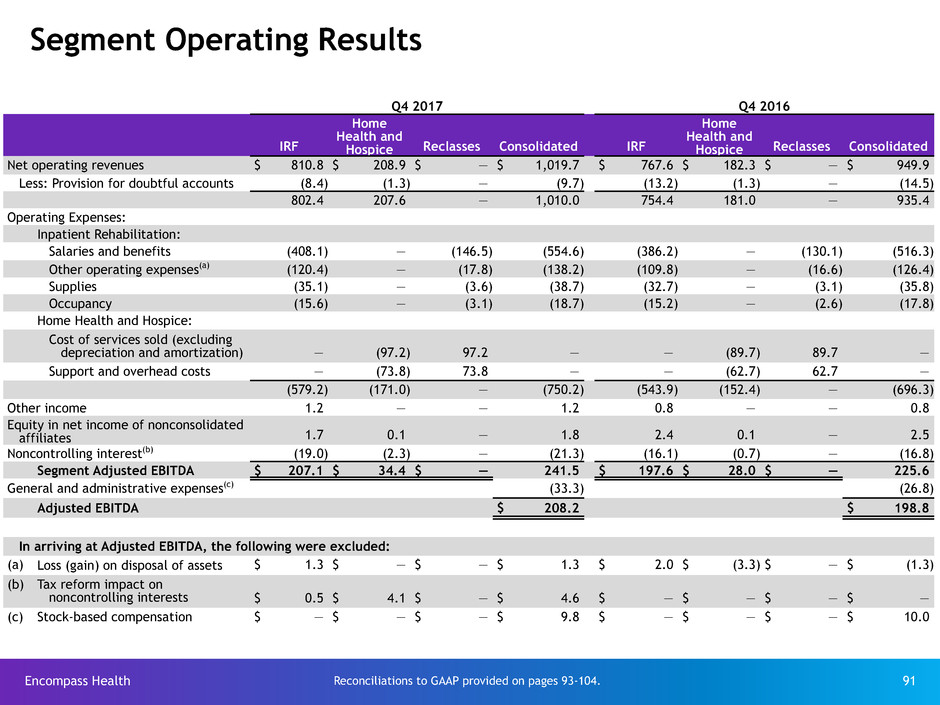
Encompass Health 91Reconciliations to GAAP provided on pages 93-104.
Segment Operating Results
Q4 2017 Q4 2016
IRF
Home
Health and
Hospice Reclasses Consolidated IRF
Home
Health and
Hospice Reclasses Consolidated
Net operating revenues $ 810.8 $ 208.9 $ — $ 1,019.7 $ 767.6 $ 182.3 $ — $ 949.9
Less: Provision for doubtful accounts (8.4) (1.3) — (9.7) (13.2) (1.3) — (14.5)
802.4 207.6 — 1,010.0 754.4 181.0 — 935.4
Operating Expenses:
Inpatient Rehabilitation:
Salaries and benefits (408.1) — (146.5) (554.6) (386.2) — (130.1) (516.3)
Other operating expenses(a) (120.4) — (17.8) (138.2) (109.8) — (16.6) (126.4)
Supplies (35.1) — (3.6) (38.7) (32.7) — (3.1) (35.8)
Occupancy (15.6) — (3.1) (18.7) (15.2) — (2.6) (17.8)
Home Health and Hospice:
Cost of services sold (excluding
depreciation and amortization) — (97.2) 97.2 — — (89.7) 89.7 —
Support and overhead costs — (73.8) 73.8 — — (62.7) 62.7 —
(579.2) (171.0) — (750.2) (543.9) (152.4) — (696.3)
Other income 1.2 — — 1.2 0.8 — — 0.8
Equity in net income of nonconsolidated
affiliates 1.7 0.1 — 1.8 2.4 0.1 — 2.5
Noncontrolling interest(b) (19.0) (2.3) — (21.3) (16.1) (0.7) — (16.8)
Segment Adjusted EBITDA $ 207.1 $ 34.4 $ — 241.5 $ 197.6 $ 28.0 $ — 225.6
General and administrative expenses(c) (33.3) (26.8)
Adjusted EBITDA $ 208.2 $ 198.8
In arriving at Adjusted EBITDA, the following were excluded:
(a) Loss (gain) on disposal of assets $ 1.3 $ — $ — $ 1.3 $ 2.0 $ (3.3) $ — $ (1.3)
(b) Tax reform impact on
noncontrolling interests $ 0.5 $ 4.1 $ — $ 4.6 $ — $ — $ — $ —
(c) Stock-based compensation $ — $ — $ — $ 9.8 $ — $ — $ — $ 10.0
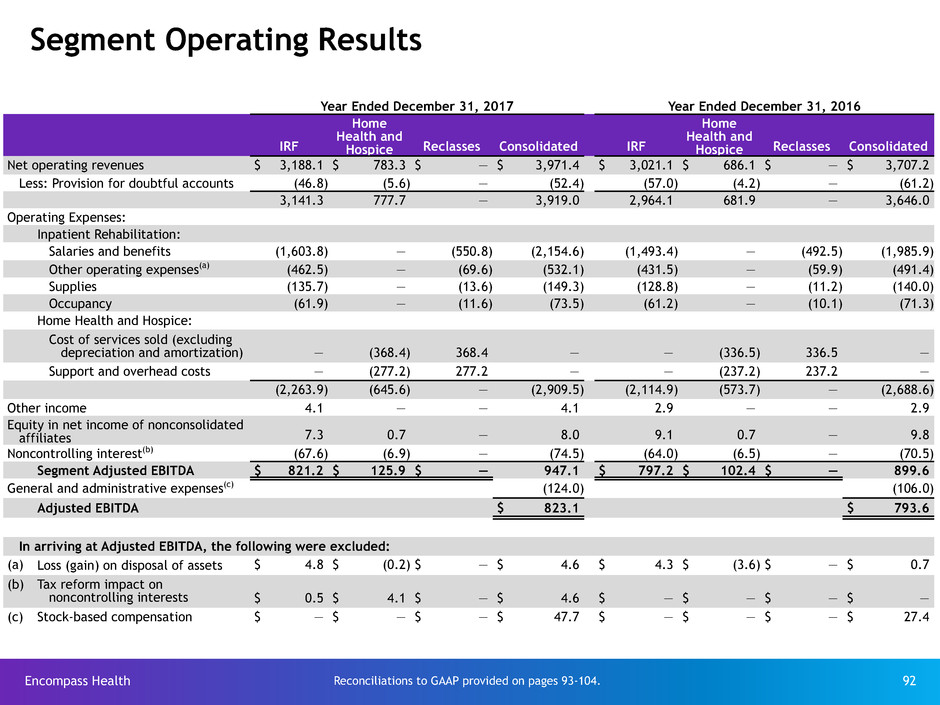
Encompass Health 92Reconciliations to GAAP provided on pages 93-104.
Year Ended December 31, 2017 Year Ended December 31, 2016
IRF
Home
Health and
Hospice Reclasses Consolidated IRF
Home
Health and
Hospice Reclasses Consolidated
Net operating revenues $ 3,188.1 $ 783.3 $ — $ 3,971.4 $ 3,021.1 $ 686.1 $ — $ 3,707.2
Less: Provision for doubtful accounts (46.8) (5.6) — (52.4) (57.0) (4.2) — (61.2)
3,141.3 777.7 — 3,919.0 2,964.1 681.9 — 3,646.0
Operating Expenses:
Inpatient Rehabilitation:
Salaries and benefits (1,603.8) — (550.8) (2,154.6) (1,493.4) — (492.5) (1,985.9)
Other operating expenses(a) (462.5) — (69.6) (532.1) (431.5) — (59.9) (491.4)
Supplies (135.7) — (13.6) (149.3) (128.8) — (11.2) (140.0)
Occupancy (61.9) — (11.6) (73.5) (61.2) — (10.1) (71.3)
Home Health and Hospice:
Cost of services sold (excluding
depreciation and amortization) — (368.4) 368.4 — — (336.5) 336.5 —
Support and overhead costs — (277.2) 277.2 — — (237.2) 237.2 —
(2,263.9) (645.6) — (2,909.5) (2,114.9) (573.7) — (2,688.6)
Other income 4.1 — — 4.1 2.9 — — 2.9
Equity in net income of nonconsolidated
affiliates 7.3 0.7 — 8.0 9.1 0.7 — 9.8
Noncontrolling interest(b) (67.6) (6.9) — (74.5) (64.0) (6.5) — (70.5)
Segment Adjusted EBITDA $ 821.2 $ 125.9 $ — 947.1 $ 797.2 $ 102.4 $ — 899.6
General and administrative expenses(c) (124.0) (106.0)
Adjusted EBITDA $ 823.1 $ 793.6
In arriving at Adjusted EBITDA, the following were excluded:
(a) Loss (gain) on disposal of assets $ 4.8 $ (0.2) $ — $ 4.6 $ 4.3 $ (3.6) $ — $ 0.7
(b) Tax reform impact on
noncontrolling interests $ 0.5 $ 4.1 $ — $ 4.6 $ — $ — $ — $ —
(c) Stock-based compensation $ — $ — $ — $ 47.7 $ — $ — $ — $ 27.4
Segment Operating Results

Encompass Health 93
Reconciliations to GAAP
and Share Information
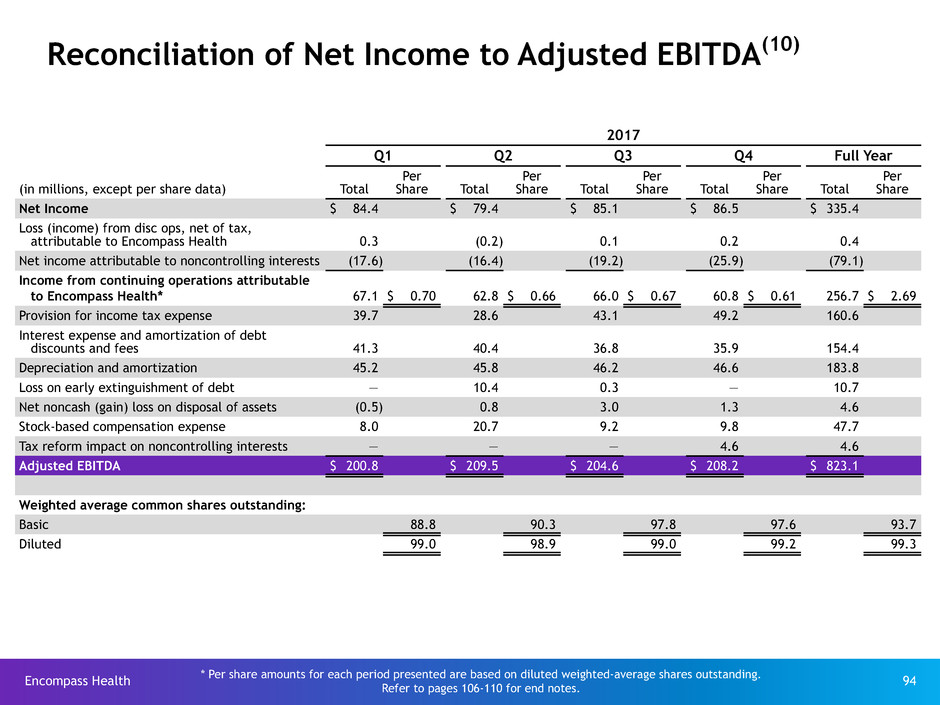
Encompass Health 94
Reconciliation of Net Income to Adjusted EBITDA(10)
* Per share amounts for each period presented are based on diluted weighted-average shares outstanding.
Refer to pages 106-110 for end notes.
2017
Q1 Q2 Q3 Q4 Full Year
(in millions, except per share data) Total
Per
Share Total
Per
Share Total
Per
Share Total
Per
Share Total
Per
Share
Net Income $ 84.4 $ 79.4 $ 85.1 $ 86.5 $ 335.4
Loss (income) from disc ops, net of tax,
attributable to Encompass Health 0.3 (0.2) 0.1 0.2 0.4
Net income attributable to noncontrolling interests (17.6) (16.4) (19.2) (25.9) (79.1)
Income from continuing operations attributable
to Encompass Health* 67.1 $ 0.70 62.8 $ 0.66 66.0 $ 0.67 60.8 $ 0.61 256.7 $ 2.69
Provision for income tax expense 39.7 28.6 43.1 49.2 160.6
Interest expense and amortization of debt
discounts and fees 41.3 40.4 36.8 35.9 154.4
Depreciation and amortization 45.2 45.8 46.2 46.6 183.8
Loss on early extinguishment of debt — 10.4 0.3 — 10.7
Net noncash (gain) loss on disposal of assets (0.5) 0.8 3.0 1.3 4.6
Stock-based compensation expense 8.0 20.7 9.2 9.8 47.7
Tax reform impact on noncontrolling interests — — — 4.6 4.6
Adjusted EBITDA $ 200.8 $ 209.5 $ 204.6 $ 208.2 $ 823.1
Weighted average common shares outstanding:
Basic 88.8 90.3 97.8 97.6 93.7
Diluted 99.0 98.9 99.0 99.2 99.3
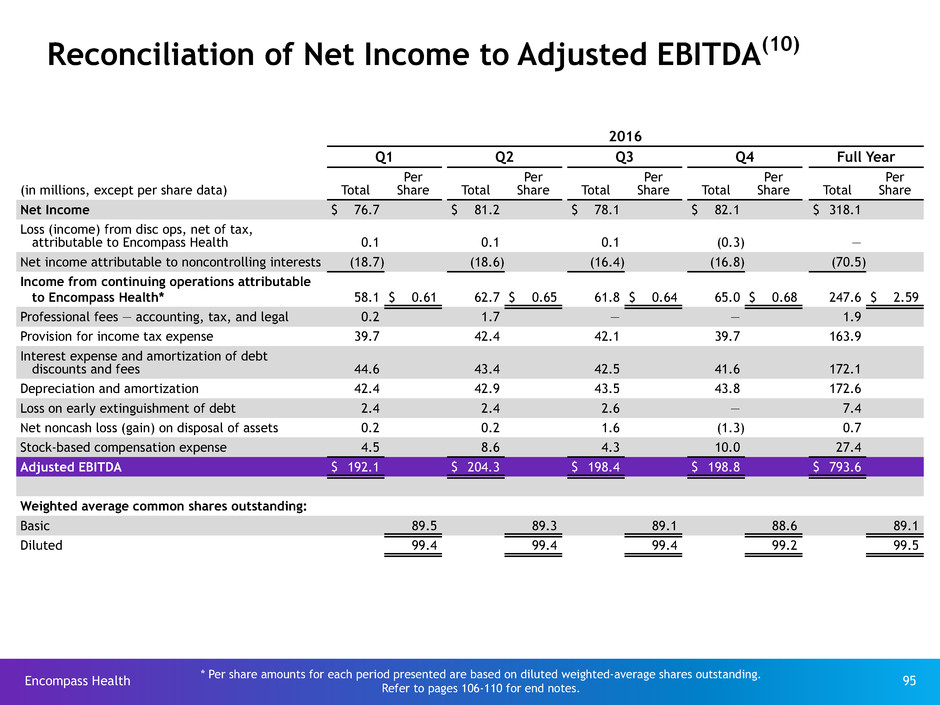
Encompass Health 95
2016
Q1 Q2 Q3 Q4 Full Year
(in millions, except per share data) Total
Per
Share Total
Per
Share Total
Per
Share Total
Per
Share Total
Per
Share
Net Income $ 76.7 $ 81.2 $ 78.1 $ 82.1 $ 318.1
Loss (income) from disc ops, net of tax,
attributable to Encompass Health 0.1 0.1 0.1 (0.3) —
Net income attributable to noncontrolling interests (18.7) (18.6) (16.4) (16.8) (70.5)
Income from continuing operations attributable
to Encompass Health* 58.1 $ 0.61 62.7 $ 0.65 61.8 $ 0.64 65.0 $ 0.68 247.6 $ 2.59
Professional fees — accounting, tax, and legal 0.2 1.7 — — 1.9
Provision for income tax expense 39.7 42.4 42.1 39.7 163.9
Interest expense and amortization of debt
discounts and fees 44.6 43.4 42.5 41.6 172.1
Depreciation and amortization 42.4 42.9 43.5 43.8 172.6
Loss on early extinguishment of debt 2.4 2.4 2.6 — 7.4
Net noncash loss (gain) on disposal of assets 0.2 0.2 1.6 (1.3) 0.7
Stock-based compensation expense 4.5 8.6 4.3 10.0 27.4
Adjusted EBITDA $ 192.1 $ 204.3 $ 198.4 $ 198.8 $ 793.6
Weighted average common shares outstanding:
Basic 89.5 89.3 89.1 88.6 89.1
Diluted 99.4 99.4 99.4 99.2 99.5
Reconciliation of Net Income to Adjusted EBITDA(10)
* Per share amounts for each period presented are based on diluted weighted-average shares outstanding.
Refer to pages 106-110 for end notes.
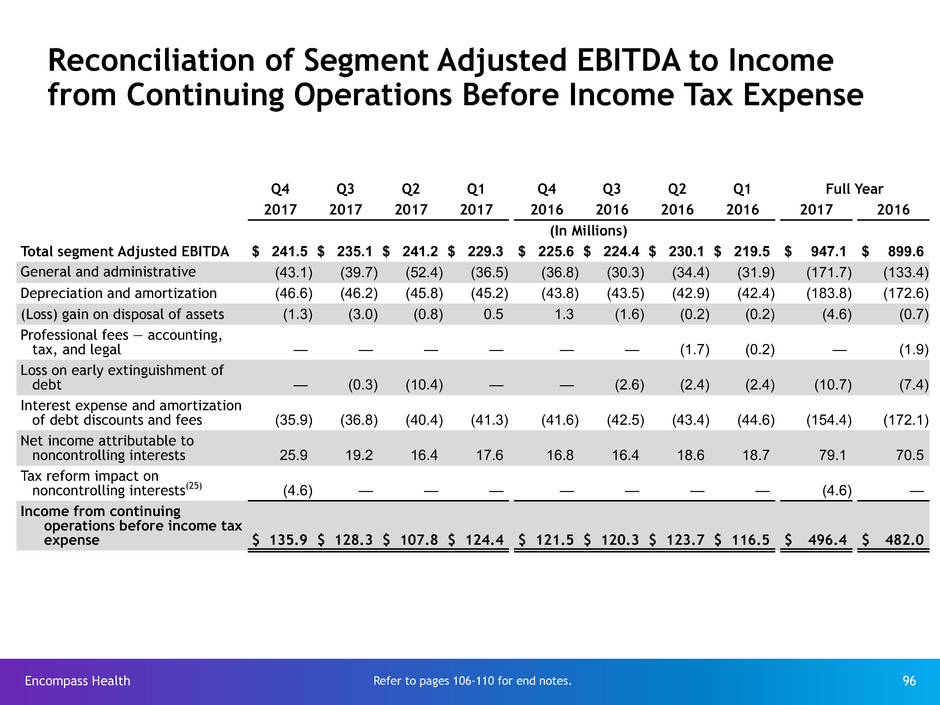
Encompass Health 96
Reconciliation of Segment Adjusted EBITDA to Income
from Continuing Operations Before Income Tax Expense
Q4 Q3 Q2 Q1 Q4 Q3 Q2 Q1 Full Year
2017 2017 2017 2017 2016 2016 2016 2016 2017 2016
(In Millions)
Total segment Adjusted EBITDA $ 241.5 $ 235.1 $ 241.2 $ 229.3 $ 225.6 $ 224.4 $ 230.1 $ 219.5 $ 947.1 $ 899.6
General and administrative
expenses
(43.1) (39.7) (52.4) (36.5) (36.8) (30.3) (34.4) (31.9) (171.7) (133.4)
Depreciation and amortization (46.6) (46.2) (45.8) (45.2) (43.8) (43.5) (42.9) (42.4) (183.8) (172.6)
(Loss) gain on disposal of assets (1.3) (3.0) (0.8) 0.5 1.3 (1.6) (0.2) (0.2) (4.6) (0.7)
Professional fees — accounting,
tax, and legal — — — — — — (1.7) (0.2) — (1.9)
Loss on early extinguishment of
debt — (0.3) (10.4) — — (2.6) (2.4) (2.4) (10.7) (7.4)
Interest expense and amortization
of debt discounts and fees (35.9) (36.8) (40.4) (41.3) (41.6) (42.5) (43.4) (44.6) (154.4) (172.1)
Net income attributable to
noncontrolling interests 25.9 19.2 16.4 17.6 16.8 16.4 18.6 18.7 79.1 70.5
Tax reform impact on
noncontrolling interests(25) (4.6) — — — — — — — (4.6) —
Income from continuing
operations before income tax
expense $ 135.9 $ 128.3 $ 107.8 $ 124.4 $ 121.5 $ 120.3 $ 123.7 $ 116.5 $ 496.4 $ 482.0
Refer to pages 106-110 for end notes.
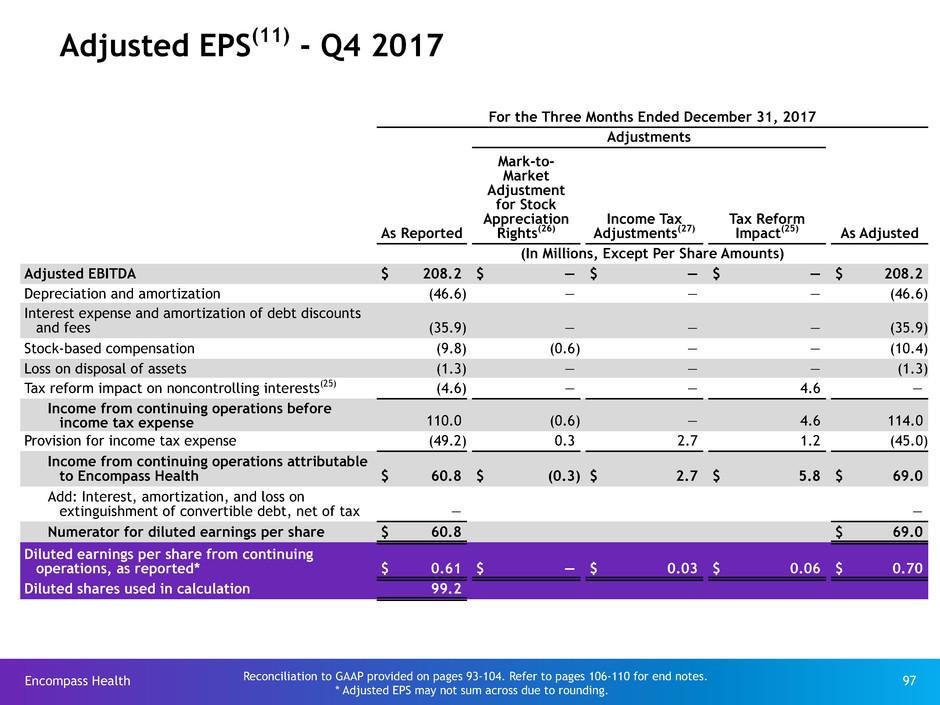
Encompass Health 97
Adjusted EPS(11) - Q4 2017
Reconciliation to GAAP provided on pages 93-104. Refer to pages 106-110 for end notes.
* Adjusted EPS may not sum across due to rounding.
For the Three Months Ended December 31, 2017
Adjustments
As Reported
Mark-to-
Market
Adjustment
for Stock
Appreciation
Rights(26)
Income Tax
Adjustments(27)
Tax Reform
Impact(25) As Adjusted
(In Millions, Except Per Share Amounts)
Adjusted EBITDA $ 208.2 $ — $ — $ — $ 208.2
Depreciation and amortization (46.6) — — — (46.6)
Interest expense and amortization of debt discounts
and fees (35.9) — — — (35.9)
Stock-based compensation (9.8) (0.6) — — (10.4)
Loss on disposal of assets (1.3) — — — (1.3)
Tax reform impact on noncontrolling interests(25) (4.6) — — 4.6 —
Income from continuing operations before
income tax expense 110.0 (0.6) — 4.6 114.0
Provision for income tax expense (49.2) 0.3 2.7 1.2 (45.0)
Income from continuing operations attributable
to Encompass Health $ 60.8 $ (0.3) $ 2.7 $ 5.8 $ 69.0
Add: Interest, amortization, and loss on
extinguishment of convertible debt, net of tax — —
Numerator for diluted earnings per share $ 60.8 $ 69.0
Diluted earnings per share from continuing
operations, as reported* $ 0.61 $ — $ 0.03 $ 0.06 $ 0.70
Diluted shares used in calculation 99.2
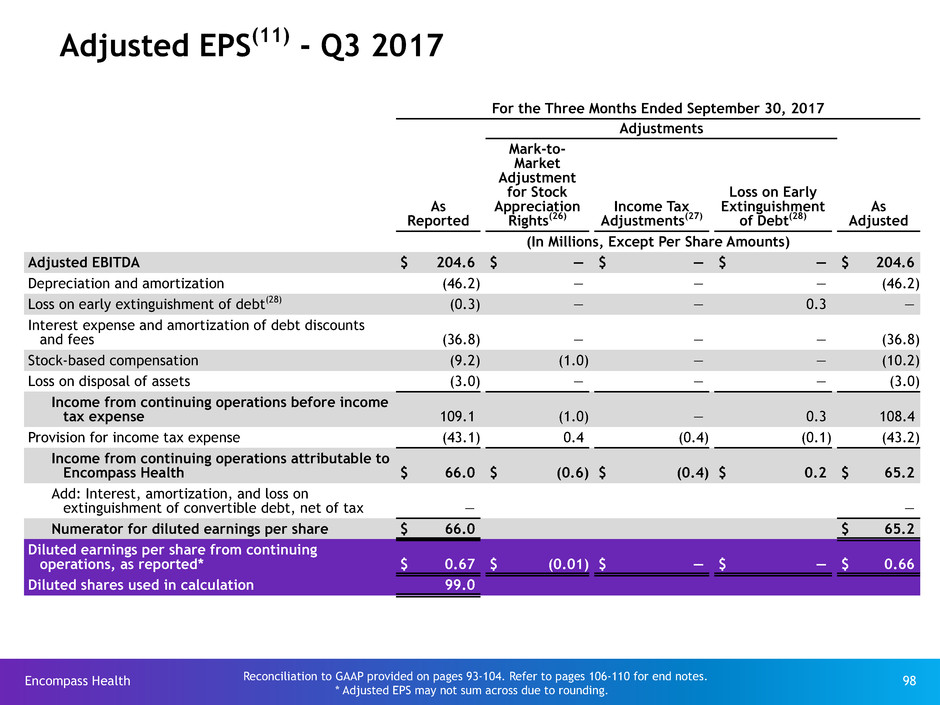
Encompass Health 98
For the Three Months Ended September 30, 2017
Adjustments
As
Reported
Mark-to-
Market
Adjustment
for Stock
Appreciation
Rights(26)
Income Tax
Adjustments(27)
Loss on Early
Extinguishment
of Debt(28)
As
Adjusted
(In Millions, Except Per Share Amounts)
Adjusted EBITDA $ 204.6 $ — $ — $ — $ 204.6
Depreciation and amortization (46.2) — — — (46.2)
Loss on early extinguishment of debt(28) (0.3) — — 0.3 —
Interest expense and amortization of debt discounts
and fees (36.8) — — — (36.8)
Stock-based compensation (9.2) (1.0) — — (10.2)
Loss on disposal of assets (3.0) — — — (3.0)
Income from continuing operations before income
tax expense 109.1 (1.0) — 0.3 108.4
Provision for income tax expense (43.1) 0.4 (0.4) (0.1) (43.2)
Income from continuing operations attributable to
Encompass Health $ 66.0 $ (0.6) $ (0.4) $ 0.2 $ 65.2
Add: Interest, amortization, and loss on
extinguishment of convertible debt, net of tax — —
Numerator for diluted earnings per share $ 66.0 $ 65.2
Diluted earnings per share from continuing
operations, as reported* $ 0.67 $ (0.01) $ — $ — $ 0.66
Diluted shares used in calculation 99.0
Adjusted EPS(11) - Q3 2017
Reconciliation to GAAP provided on pages 93-104. Refer to pages 106-110 for end notes.
* Adjusted EPS may not sum across due to rounding.
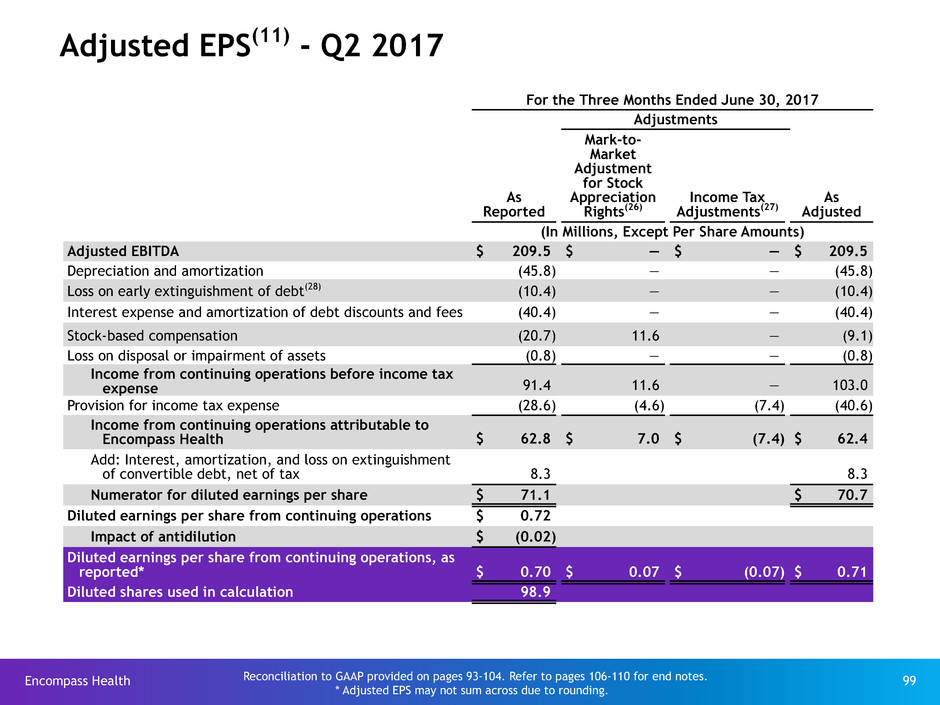
Encompass Health 99
Adjusted EPS(11) - Q2 2017
For the Three Months Ended June 30, 2017
Adjustments
As
Reported
Mark-to-
Market
Adjustment
for Stock
Appreciation
Rights(26)
Income Tax
Adjustments(27)
As
Adjusted
(In Millions, Except Per Share Amounts)
Adjusted EBITDA $ 209.5 $ — $ — $ 209.5
Depreciation and amortization (45.8) — — (45.8)
Loss on early extinguishment of debt(28) (10.4) — — (10.4)
Interest expense and amortization of debt discounts and fees (40.4) — — (40.4)
Stock-based compensation (20.7) 11.6 — (9.1)
Loss on disposal or impairment of assets (0.8) — — (0.8)
Income from continuing operations before income tax
expense 91.4 11.6 — 103.0
Provision for income tax expense (28.6) (4.6) (7.4) (40.6)
Income from continuing operations attributable to
Encompass Health $ 62.8 $ 7.0 $ (7.4) $ 62.4
Add: Interest, amortization, and loss on extinguishment
of convertible debt, net of tax 8.3 8.3
Numerator for diluted earnings per share $ 71.1 $ 70.7
Diluted earnings per share from continuing operations $ 0.72
Impact of antidilution $ (0.02)
Diluted earnings per share from continuing operations, as
reported* $ 0.70 $ 0.07 $ (0.07) $ 0.71
Diluted shares used in calculation 98.9
Reconciliation to GAAP provided on pages 93-104. Refer to pages 106-110 for end notes.
* Adjusted EPS may not sum across due to rounding.
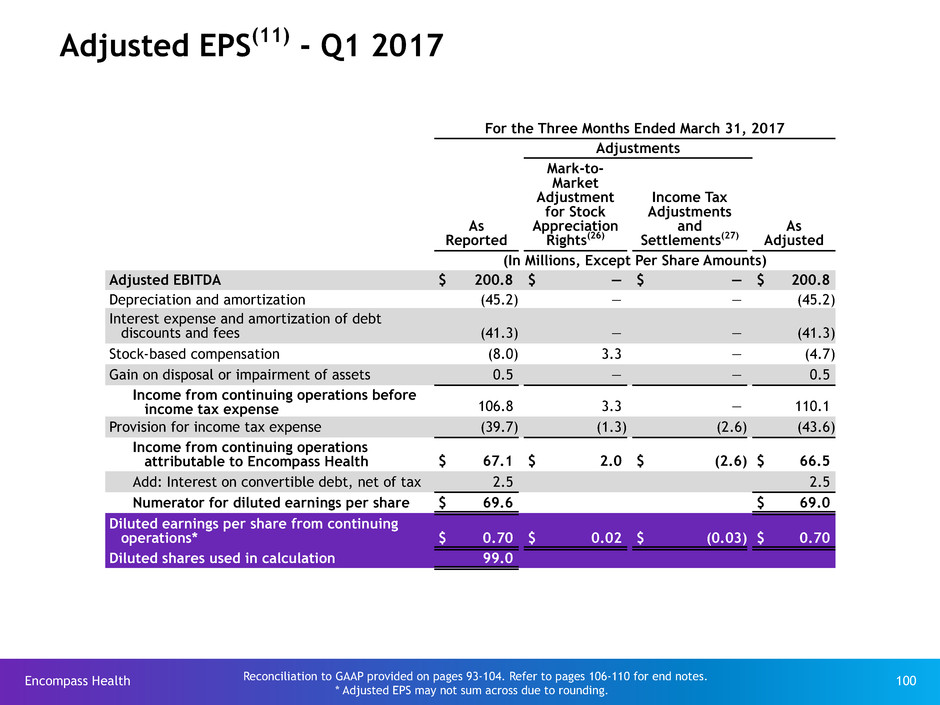
Encompass Health 100
Adjusted EPS(11) - Q1 2017
For the Three Months Ended March 31, 2017
Adjustments
As
Reported
Mark-to-
Market
Adjustment
for Stock
Appreciation
Rights(26)
Income Tax
Adjustments
and
Settlements(27)
As
Adjusted
(In Millions, Except Per Share Amounts)
Adjusted EBITDA $ 200.8 $ — $ — $ 200.8
Depreciation and amortization (45.2) — — (45.2)
Interest expense and amortization of debt
discounts and fees (41.3) — — (41.3)
Stock-based compensation (8.0) 3.3 — (4.7)
Gain on disposal or impairment of assets 0.5 — — 0.5
Income from continuing operations before
income tax expense 106.8 3.3 — 110.1
Provision for income tax expense (39.7) (1.3) (2.6) (43.6)
Income from continuing operations
attributable to Encompass Health $ 67.1 $ 2.0 $ (2.6) $ 66.5
Add: Interest on convertible debt, net of tax 2.5 2.5
Numerator for diluted earnings per share $ 69.6 $ 69.0
Diluted earnings per share from continuing
operations* $ 0.70 $ 0.02 $ (0.03) $ 0.70
Diluted shares used in calculation 99.0
Reconciliation to GAAP provided on pages 93-104. Refer to pages 106-110 for end notes.
* Adjusted EPS may not sum across due to rounding.
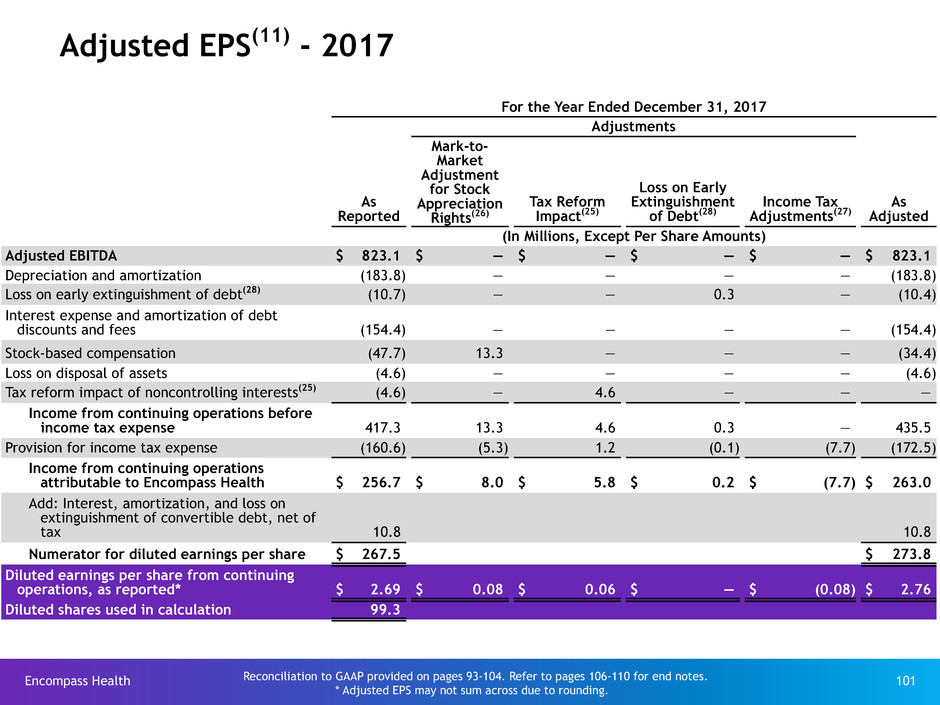
Encompass Health 101
Adjusted EPS(11) - 2017
For the Year Ended December 31, 2017
Adjustments
As
Reported
Mark-to-
Market
Adjustment
for Stock
Appreciation
Rights(26)
Tax Reform
Impact(25)
Loss on Early
Extinguishment
of Debt(28)
Income Tax
Adjustments(27)
As
Adjusted
(In Millions, Except Per Share Amounts)
Adjusted EBITDA $ 823.1 $ — $ — $ — $ — $ 823.1
Depreciation and amortization (183.8) — — — — (183.8)
Loss on early extinguishment of debt(28) (10.7) — — 0.3 — (10.4)
Interest expense and amortization of debt
discounts and fees (154.4) — — — — (154.4)
Stock-based compensation (47.7) 13.3 — — — (34.4)
Loss on disposal of assets (4.6) — — — — (4.6)
Tax reform impact of noncontrolling interests(25) (4.6) — 4.6 — — —
Income from continuing operations before
income tax expense 417.3 13.3 4.6 0.3 — 435.5
Provision for income tax expense (160.6) (5.3) 1.2 (0.1) (7.7) (172.5)
Income from continuing operations
attributable to Encompass Health $ 256.7 $ 8.0 $ 5.8 $ 0.2 $ (7.7) $ 263.0
Add: Interest, amortization, and loss on
extinguishment of convertible debt, net of
tax 10.8 10.8
Numerator for diluted earnings per share $ 267.5 $ 273.8
Diluted earnings per share from continuing
operations, as reported* $ 2.69 $ 0.08 $ 0.06 $ — $ (0.08) $ 2.76
Diluted shares used in calculation 99.3
Reconciliation to GAAP provided on pages 93-104. Refer to pages 106-110 for end notes.
* Adjusted EPS may not sum across due to rounding.
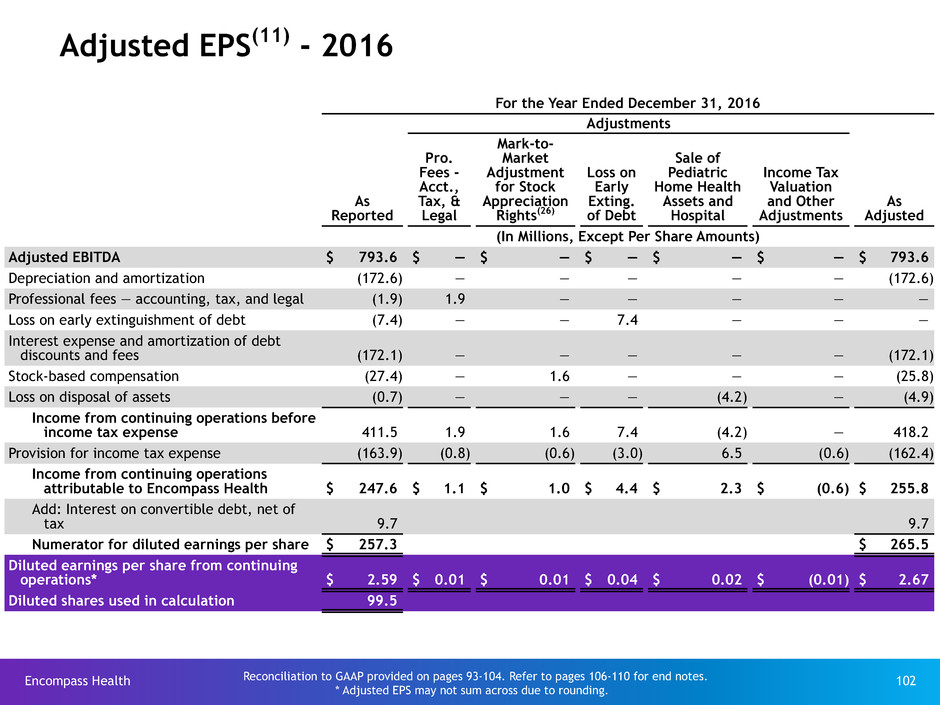
Encompass Health 102
For the Year Ended December 31, 2016
Adjustments
As
Reported
Pro.
Fees -
Acct.,
Tax, &
Legal
Mark-to-
Market
Adjustment
for Stock
Appreciation
Rights(26)
Loss on
Early
Exting.
of Debt
Sale of
Pediatric
Home Health
Assets and
Hospital
Income Tax
Valuation
and Other
Adjustments
As
Adjusted
(In Millions, Except Per Share Amounts)
Adjusted EBITDA $ 793.6 $ — $ — $ — $ — $ — $ 793.6
Depreciation and amortization (172.6) — — — — — (172.6)
Professional fees — accounting, tax, and legal (1.9) 1.9 — — — — —
Loss on early extinguishment of debt (7.4) — — 7.4 — — —
Interest expense and amortization of debt
discounts and fees (172.1) — — — — — (172.1)
Stock-based compensation (27.4) — 1.6 — — — (25.8)
Loss on disposal of assets (0.7) — — — (4.2) — (4.9)
Income from continuing operations before
income tax expense 411.5 1.9 1.6 7.4 (4.2) — 418.2
Provision for income tax expense (163.9) (0.8) (0.6) (3.0) 6.5 (0.6) (162.4)
Income from continuing operations
attributable to Encompass Health $ 247.6 $ 1.1 $ 1.0 $ 4.4 $ 2.3 $ (0.6) $ 255.8
Add: Interest on convertible debt, net of
tax 9.7 9.7
Numerator for diluted earnings per share $ 257.3 $ 265.5
Diluted earnings per share from continuing
operations* $ 2.59 $ 0.01 $ 0.01 $ 0.04 $ 0.02 $ (0.01) $ 2.67
Diluted shares used in calculation 99.5
Adjusted EPS(11) - 2016
Reconciliation to GAAP provided on pages 93-104. Refer to pages 106-110 for end notes.
* Adjusted EPS may not sum across due to rounding.
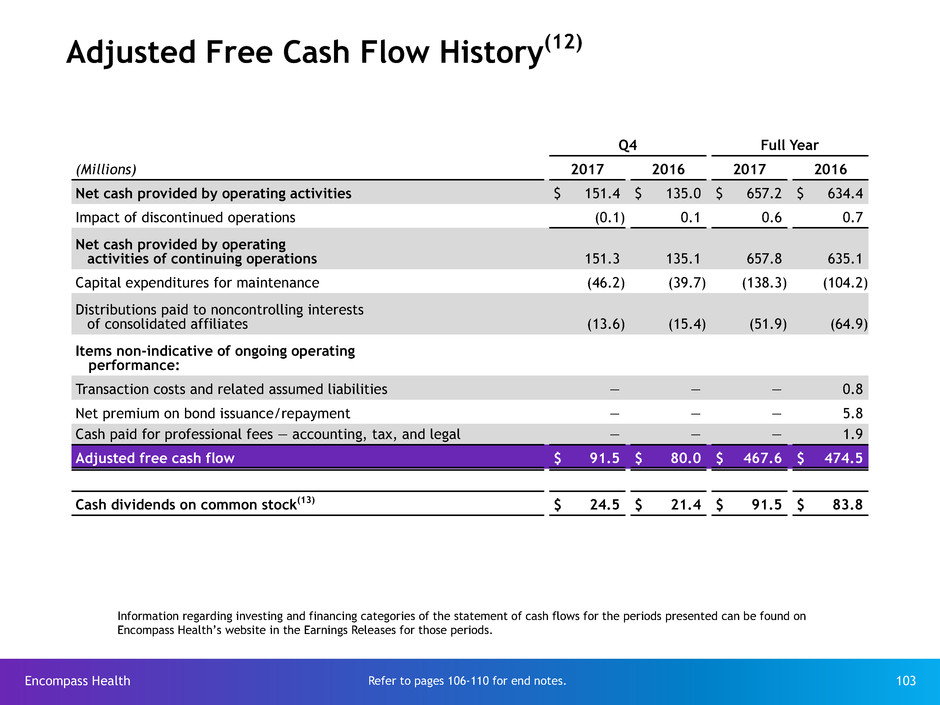
Encompass Health 103
Adjusted Free Cash Flow History(12)
Q4 Full Year
(Millions) 2017 2016 2017 2016
Net cash provided by operating activities $ 151.4 $ 135.0 $ 657.2 $ 634.4
Impact of discontinued operations (0.1) 0.1 0.6 0.7
Net cash provided by operating
activities of continuing operations 151.3 135.1 657.8 635.1
Capital expenditures for maintenance (46.2) (39.7) (138.3) (104.2)
Distributions paid to noncontrolling interests
of consolidated affiliates (13.6) (15.4) (51.9) (64.9)
Items non-indicative of ongoing operating
performance:
Transaction costs and related assumed liabilities — — — 0.8
Net premium on bond issuance/repayment — — — 5.8
Cash paid for professional fees — accounting, tax, and legal — — — 1.9
Adjusted free cash flow $ 91.5 $ 80.0 $ 467.6 $ 474.5
Cash dividends on common stock(13) $ 24.5 $ 21.4 $ 91.5 $ 83.8
Refer to pages 106-110 for end notes.
Information regarding investing and financing categories of the statement of cash flows for the periods presented can be found on
Encompass Health’s website in the Earnings Releases for those periods.
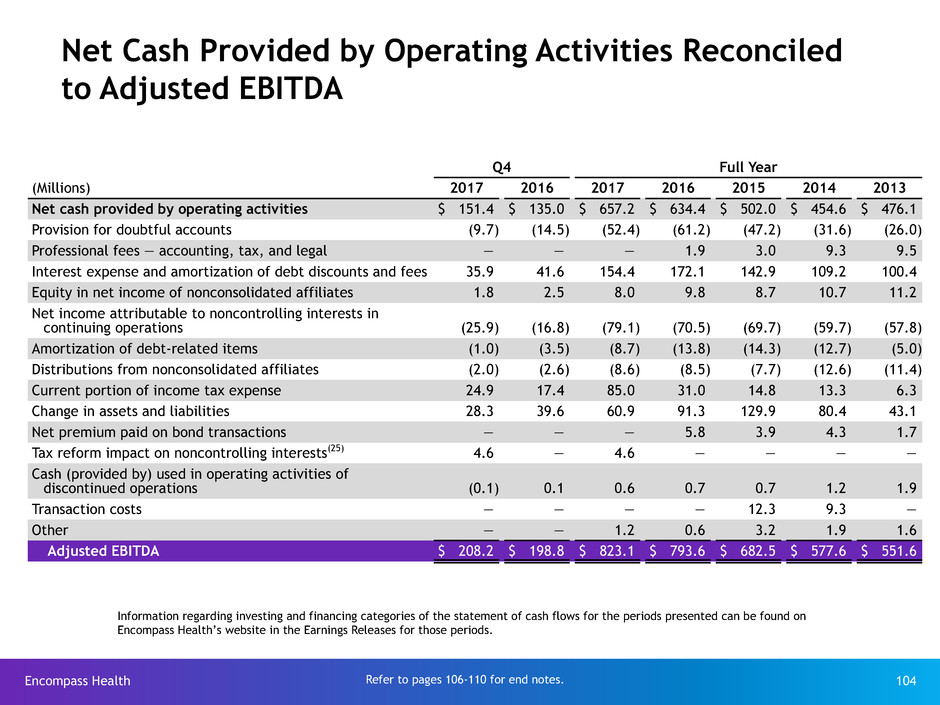
Encompass Health 104
Net Cash Provided by Operating Activities Reconciled
to Adjusted EBITDA
Information regarding investing and financing categories of the statement of cash flows for the periods presented can be found on
Encompass Health’s website in the Earnings Releases for those periods.
Q4 Full Year
(Millions) 2017 2016 2017 2016 2015 2014 2013
Net cash provided by operating activities $ 151.4 $ 135.0 $ 657.2 $ 634.4 $ 502.0 $ 454.6 $ 476.1
Provision for doubtful accounts (9.7) (14.5) (52.4) (61.2) (47.2) (31.6) (26.0)
Professional fees — accounting, tax, and legal — — — 1.9 3.0 9.3 9.5
Interest expense and amortization of debt discounts and fees 35.9 41.6 154.4 172.1 142.9 109.2 100.4
Equity in net income of nonconsolidated affiliates 1.8 2.5 8.0 9.8 8.7 10.7 11.2
Net income attributable to noncontrolling interests in
continuing operations (25.9) (16.8) (79.1) (70.5) (69.7) (59.7) (57.8)
Amortization of debt-related items (1.0) (3.5) (8.7) (13.8) (14.3) (12.7) (5.0)
Distributions from nonconsolidated affiliates (2.0) (2.6) (8.6) (8.5) (7.7) (12.6) (11.4)
Current portion of income tax expense 24.9 17.4 85.0 31.0 14.8 13.3 6.3
Change in assets and liabilities 28.3 39.6 60.9 91.3 129.9 80.4 43.1
Net premium paid on bond transactions — — — 5.8 3.9 4.3 1.7
Tax reform impact on noncontrolling interests(25) 4.6 — 4.6 — — — —
Cash (provided by) used in operating activities of
discontinued operations (0.1) 0.1 0.6 0.7 0.7 1.2 1.9
Transaction costs — — — — 12.3 9.3 —
Other — — 1.2 0.6 3.2 1.9 1.6
Adjusted EBITDA $ 208.2 $ 198.8 $ 823.1 $ 793.6 $ 682.5 $ 577.6 $ 551.6
Refer to pages 106-110 for end notes.
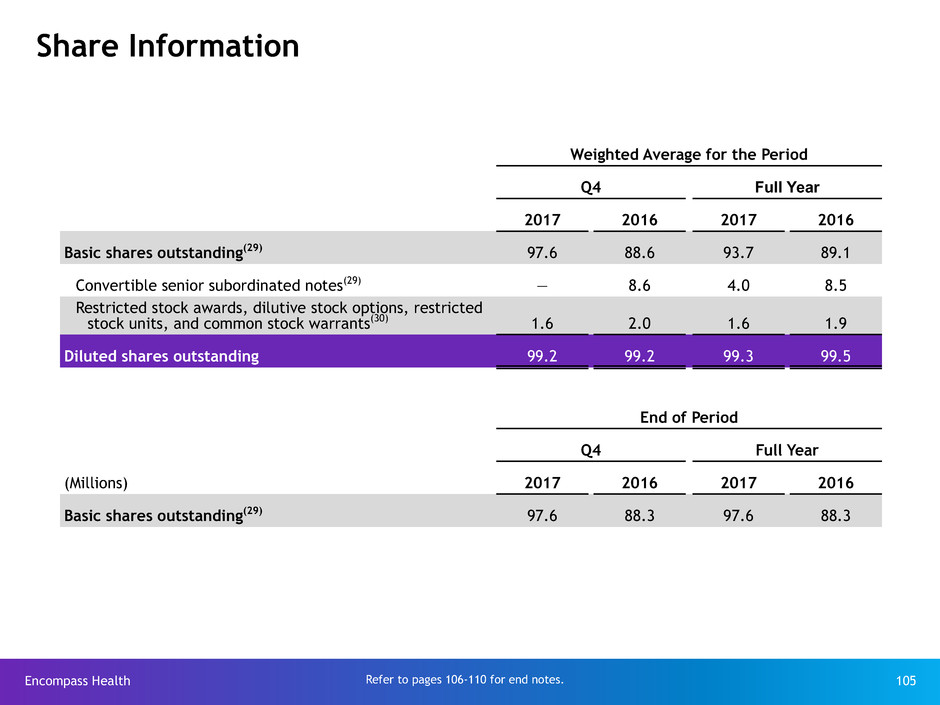
Encompass Health 105Refer to pages 106-110 for end notes.
Share Information
Weighted Average for the Period
Q4 Full Year
2017 2016 2017 2016
Basic shares outstanding(29) 97.6 88.6 93.7 89.1
Convertible senior subordinated notes(29) — 8.6 4.0 8.5
Restricted stock awards, dilutive stock options, restricted
stock units, and common stock warrants(30) 1.6 2.0 1.6 1.9
Diluted shares outstanding 99.2 99.2 99.3 99.5
End of Period
Q4 Full Year
(Millions) 2017 2016 2017 2016
Basic shares outstanding(29) 97.6 88.3 97.6 88.3

Encompass Health 106
End Notes

Encompass Health 107
(1) Under this program, Joint Commission accredited organizations, like the Company’s IRFs, may seek certification for chronic diseases or conditions such
as brain injury or stroke rehabilitation by complying with Joint Commission standards, effectively using evidence-based clinical practice guidelines to
manage and optimize patient care, and using an organized approach to performance measurement and evaluation of clinical outcomes. Obtaining such
certifications demonstrates the Company’s commitment to excellence in providing disease-specific care.
(2) Data compares Encompass Health IRFs to IRFs comprising the Uniform Data System for Medical Rehabilitation (“UDSMR”), a division of UB Foundation
Activities, Inc., a data gathering and analysis organization for the rehabilitation industry which represents approximately 70% of the industry, including
Encompass Health sites. Data is adjusted by applying Encompass Health IRF case-mix to non-Encompass Health UDS IRFs.
(3) Source: https://data.medicare.gov/data/home-health-compare. Data on this page was published in January 2018 and reflects OASIS and HHCAHPS
Survey data collected from July 2016 through June 2017 and claims-based data collected from April 2016 through March 2017.
(4) The 123 for Encompass Health excludes the inpatient rehabilitation hospitals at HealthSouth Rehabilitation Hospital of Modesto (opened October 2016);
HealthSouth Rehabilitation Hospital of Gulfport (opened April 2017); Mount Carmel Rehabilitation Hospital, in partnership with HealthSouth (opened
April 2017); Spire Rehabilitation Hospital, in partnership with HealthSouth (opened July 2017); HealthSouth Rehabilitation Hospital of Pearland (opened
October 2017); and HealthSouth Rehabilitation Hospital of Beaumont (sold June 2016). The 123 does include HealthSouth Rehabilitation Hospital of
Austin, which was closed August 2016.
(5) In 2016, the Company averaged 1,386 total Medicare and non-Medicare discharges per IRF in its then 118 consolidated IRFs that were open the full
year.
(6) Case Mix Index (CMI) from the rate-setting file is adjusted for short-stay transfer cases. The Company’s unadjusted CMI for 2016 was 1.36 versus 1.33
for the industry as measured by UDSMR.
(7) Source: FY 2018 CMS Final Rule Rate Setting File and the last publicly available Medicare cost reports (FYE 2015/2016) or in the case of new IRFs, the
June 2017 CMS Provider of Service File.
a.All data provided was filtered and compiled from the Centers for Medicare and Medicaid Services (CMS) Fiscal Year 2018 IRF Final Rule Rate Setting
File found at https://www.cms.gov/Medicare/Medicare-Fee-for-Service-Payment/InpatientRehabFacPPS/Downloads/FY2018_datafiles_final.zip.
The data presented was developed entirely by CMS and is based on its definitions which are different in form and substance from the criteria
Encompass Health uses for external reporting purposes. Because CMS does not provide its detailed methodology, Encompass Health is not able to
reconstruct the CMS projections or the calculation.
b.The CMS file contains data for each of the 1,140 inpatient rehabilitation facilities used to estimate the policy updates for the FY 2018 IRF-PPS Final
Rule. Most of the data represents historical information from the CMS fiscal year 2016 period and may or may not reflect the same Encompass
Health IRFs in operation today. The data presented was separated into three categories: Freestanding, Units, and Encompass Health. Encompass
Health is a subset of Freestanding and the Total.
(8) The Budget Control Act of 2011 included a reduction of up to 2% to Medicare payments for all providers that began on April 1, 2013 (as modified by
H.R. 8). The reduction was made from whatever level of payment would otherwise have been provided under Medicare law and regulation.
(9) The Company acquired an additional 30% equity interest in Fairlawn Rehabilitation Hospital in Worcester, MA from its joint venture partner. This
transaction increased the Company’s ownership interest from 50% to 80% and resulted in a change in accounting for the hospital from the equity
method to a consolidated entity effective June 1, 2014.
(10) Adjusted EBITDA is a non-GAAP financial measure. The Company’s leverage ratio (total consolidated debt to Adjusted EBITDA for the trailing four
quarters) is, likewise, a non-GAAP measure. Management and some members of the investment community utilize Adjusted EBITDA as a financial
measure and the leverage ratio as a liquidity measure on an ongoing basis. These measures are not recognized in accordance with GAAP and should not
be viewed as an alternative to GAAP measures of performance or liquidity. In evaluating Adjusted EBITDA, the reader should be aware that in the
future the Company may incur expenses similar to the adjustments set forth. Further explanation and disclosure relating to Adjusted EBITDA are
included in the Company’s Form 8-K, dated March 13, 2018, to which this Investor Reference Book is attached as Exhibit 99.1.
End Notes
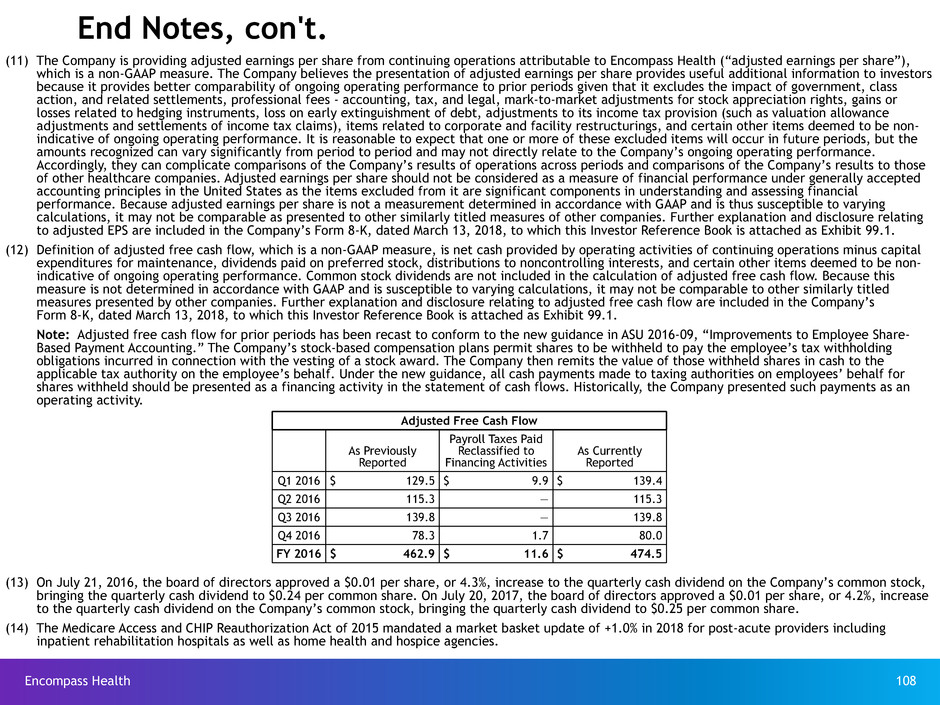
Encompass Health 108
(11) The Company is providing adjusted earnings per share from continuing operations attributable to Encompass Health (“adjusted earnings per share”),
which is a non-GAAP measure. The Company believes the presentation of adjusted earnings per share provides useful additional information to investors
because it provides better comparability of ongoing operating performance to prior periods given that it excludes the impact of government, class
action, and related settlements, professional fees - accounting, tax, and legal, mark-to-market adjustments for stock appreciation rights, gains or
losses related to hedging instruments, loss on early extinguishment of debt, adjustments to its income tax provision (such as valuation allowance
adjustments and settlements of income tax claims), items related to corporate and facility restructurings, and certain other items deemed to be non-
indicative of ongoing operating performance. It is reasonable to expect that one or more of these excluded items will occur in future periods, but the
amounts recognized can vary significantly from period to period and may not directly relate to the Company’s ongoing operating performance.
Accordingly, they can complicate comparisons of the Company’s results of operations across periods and comparisons of the Company’s results to those
of other healthcare companies. Adjusted earnings per share should not be considered as a measure of financial performance under generally accepted
accounting principles in the United States as the items excluded from it are significant components in understanding and assessing financial
performance. Because adjusted earnings per share is not a measurement determined in accordance with GAAP and is thus susceptible to varying
calculations, it may not be comparable as presented to other similarly titled measures of other companies. Further explanation and disclosure relating
to adjusted EPS are included in the Company’s Form 8-K, dated March 13, 2018, to which this Investor Reference Book is attached as Exhibit 99.1.
(12) Definition of adjusted free cash flow, which is a non-GAAP measure, is net cash provided by operating activities of continuing operations minus capital
expenditures for maintenance, dividends paid on preferred stock, distributions to noncontrolling interests, and certain other items deemed to be non-
indicative of ongoing operating performance. Common stock dividends are not included in the calculation of adjusted free cash flow. Because this
measure is not determined in accordance with GAAP and is susceptible to varying calculations, it may not be comparable to other similarly titled
measures presented by other companies. Further explanation and disclosure relating to adjusted free cash flow are included in the Company’s
Form 8-K, dated March 13, 2018, to which this Investor Reference Book is attached as Exhibit 99.1.
Note: Adjusted free cash flow for prior periods has been recast to conform to the new guidance in ASU 2016-09, “Improvements to Employee Share-
Based Payment Accounting.” The Company’s stock-based compensation plans permit shares to be withheld to pay the employee’s tax withholding
obligations incurred in connection with the vesting of a stock award. The Company then remits the value of those withheld shares in cash to the
applicable tax authority on the employee’s behalf. Under the new guidance, all cash payments made to taxing authorities on employees’ behalf for
shares withheld should be presented as a financing activity in the statement of cash flows. Historically, the Company presented such payments as an
operating activity.
Adjusted Free Cash Flow
As Previously
Reported
Payroll Taxes Paid
Reclassified to
Financing Activities
As Currently
Reported
Q1 2016 $ 129.5 $ 9.9 $ 139.4
Q2 2016 115.3 — 115.3
Q3 2016 139.8 — 139.8
Q4 2016 78.3 1.7 80.0
FY 2016 $ 462.9 $ 11.6 $ 474.5
(13) On July 21, 2016, the board of directors approved a $0.01 per share, or 4.3%, increase to the quarterly cash dividend on the Company’s common stock,
bringing the quarterly cash dividend to $0.24 per common share. On July 20, 2017, the board of directors approved a $0.01 per share, or 4.2%, increase
to the quarterly cash dividend on the Company’s common stock, bringing the quarterly cash dividend to $0.25 per common share.
(14) The Medicare Access and CHIP Reauthorization Act of 2015 mandated a market basket update of +1.0% in 2018 for post-acute providers including
inpatient rehabilitation hospitals as well as home health and hospice agencies.
End Notes, con't.

Encompass Health 109
(15) The Bipartisan Budget Act of 2018, signed into law on February 9, 2018, provides for a home health market basket update of 1.5% for CY 2020 and the
elimination of any productivity adjustment to the market basket for that year. It also provides for the extension of the rural add-on adjustment through
2022, albeit declining in amount along the way. Additionally, it requires that a new case mix payment model be introduced in 2020 that would be based
on a 30-day unit of service, not include therapy thresholds as a component of the system, and be implemented in a budget neutral manner.
(16) The Company estimates the expected impact of each rule utilizing, among other things, the acuity of its patients over the 8-month (home health
segment) to 12-month (inpatient rehabilitation segment) period prior to each rule’s release and incorporates other adjustments included in each rule.
These estimates are prior to the impact of sequestration.
(17) Quality reporting requirements and potential penalties were enabled for IRFs as part of the Healthcare Reform Bill (PPACA). The IMPACT Act of 2014
requires additional quality and clinical data reporting for IRFs to be subject to the original 2% penalty.
(18) Pre-opening expenses include expenses for training new employees on the clinical information system, which vary based on the timing of the first
admission.
(19) The leverage ratio is based on trailing four quarters of Adjusted EBITDA of $823.1 million from Q1 2017 to Q4 2017.
(20) Represents discharges from 126 consolidated IRFs in Q4 2017; 125 consolidated IRFs in Q3 2017; 124 consolidated IRFs in Q2 2017; 122 consolidated IRFs
in Q1 2017 and Q4 2016; 121 consolidated IRFs in Q3 2016; 120 consolidated IRFs in Q2 2016; and 121 consolidated IRFs in Q1 2016.
(21) Full-time equivalents included in the table represent Encompass Health employees who participate in or support the operations of our hospitals and
include an estimate of full-time equivalents related to contract labor.
(22) Employees per occupied bed, or “EPOB,” is calculated by dividing the number of full-time equivalents, including an estimate of full-time equivalents
from the utilization of contract labor, by the number of occupied beds during each period. The number of occupied beds is determined by multiplying
the number of licensed beds by the Company’s occupancy percentage.
(23) Represents home health admissions from 198 consolidated locations in Q4 2017; 196 consolidated locations in Q3 2017; 191 consolidated locations in Q2
2017 and Q1 2017; 186 consolidated locations in Q4 2016; 188 consolidated locations in Q3 2016; 187 consolidated locations in Q2 2016; and 184
consolidated locations in Q1 2016
(24) Represents hospice admissions from 37 locations in Q4 2017, Q3 2017 and Q2 2017; 35 locations in Q1 2017 and Q4 2016; 33 locations in Q3 2016; 29
locations in Q2 2016; and 27 locations in Q1 2016
(25) The application of the lower income tax rate that resulted from the Tax Cuts and Jobs Act to the Company’s net deferred tax assets resulted in a net
$1.2 million increase in tax expense in Q4 2017. Application of the new tax rate to the Company’s joint venture entities’ deferred tax liabilities
resulted in a net reduction in tax expense in Q4 2017. The Company’s joint venture partners’ share of this net tax benefit was $4.6 million, which
resulted in an increase in noncontrolling interest expense in Q4 2017.
(26) In connection with the acquisition of Encompass Home Health & Hospice, the Company granted stock appreciation rights based on the fair value of the
common stock of HealthSouth Home Health Holdings, Inc. to certain members of Encompass Home Health & Hospice management. The fair value of
Holdings’ common stock is the amount by which the product of the trailing 12-month adjusted EBITDA for Holdings and the median market EBITDA
multiple based on a basket of public home health companies and certain public home health acquisition transactions exceeds the initial fair value
assigned to the Holdings’ stock. The fair value also takes into consideration the balance of the intercompany note in place and the net debt of
Holdings. The fair value of these SARs will vary from period to period primarily based on the performance of the Company’s home health and hospice
segment and the change in the median market multiple. Half of the SARs vest of January 1, 2019, and the other half vest on January 1, 2020. Once
vested, they are exercisable until they expire on December 31, 2024 or in connection with termination of employment.
(27) New guidance in ASU 2016-09, “Improvements to Employee Share-Based Payment Accounting,” requires entities to record all of the tax effects related
to share-based payment at settlement (or expiration) through the income statement. Historically, the Company recorded such tax effects to equity.
End Notes, con't.

Encompass Health 110
(28) The interest and amortization and the loss on early extinguishment of debt related to the convertible senior subordinated notes must be added to
income from continuing operations when calculating diluted earnings per share because the debt was assumed to have been converted at the beginning
of the period, and the applicable shares were included in the diluted share count.
(29) In November 2013, the Company closed separate, privately negotiated exchanges in which it issued $320 million of 2.0% Convertible Senior
Subordinated Notes due 2043 in exchange for 257,110 shares of its 6.5% Series A Convertible Perpetual Preferred Stock. The Company recorded ~$249
million as debt and ~$71 million as equity. In May 2017, the Company provided notice of its intent to redeem all $320 million of outstanding convertible
notes. In lieu of receiving the redemption price, the holders had the right to convert their notes into shares of the Company’s common stock at a
conversion rate of 27.2221 shares per $1,000 principal amount of Notes, which rate was increased by a make-whole premium. In the aggregate, holders
of $319.4 million in principal elected to convert, which resulted in the Company issuing 8,895,483 shares of common stock (approximately 8.6 million
shares were previously included in the diluted share count). The remaining $0.6 million of principal was redeemed by cash payment.
(30) The agreement to settle the Company’s class action securities litigation received final court approval in January 2007. The 5.0 million shares of
common stock and warrants to purchase ~8.2 million shares of common stock at a strike price of $41.40 (expired January 17, 2017) related to this
settlement were issued on September 30, 2009. The 5.0 million common shares are included in the basic outstanding shares. The warrants were not
included in the diluted share count prior to 2015 because the strike price had historically been above the market price. In full-year 2016, zero shares
related to the warrants were included in the diluted share count due to antidilution based on the stock price.
End Notes, con't.



























































































































































































































